Introduction
Effective management of clinical waste is crucial for healthcare facilities, where the stakes are high and the consequences of mismanagement can be severe. This article presents five essential steps that enhance the safety and compliance of waste disposal practices, ultimately protecting the health of both patients and staff. With evolving regulations and increasing scrutiny, healthcare providers must consider how to meet the latest standards while effectively managing the diverse types of clinical waste they generate.
Identify Types of Clinical Waste
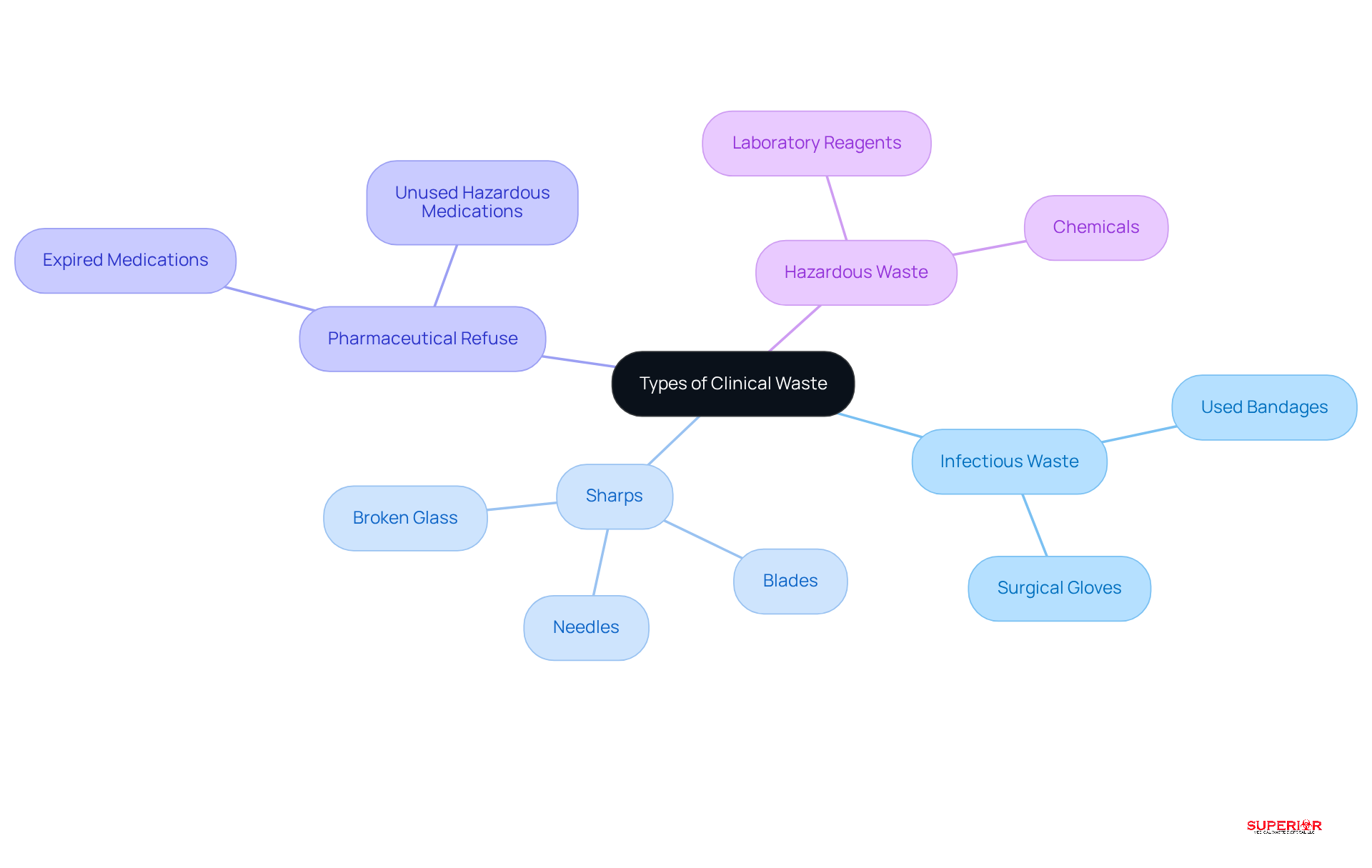
Effective clinical waste management starts with the accurate identification of the various types of waste generated within your facility. The primary categories include:
- Infectious Waste: This category encompasses materials contaminated with blood or other bodily fluids, such as used bandages and surgical gloves, which pose a risk of infection.
- Sharps: Items capable of puncturing or cutting skin, including needles, blades, and broken glass, require careful handling to prevent injuries.
- Pharmaceutical Refuse: Expired or unused medications, particularly those classified as hazardous, must be disposed of properly to mitigate environmental and health risks.
- Hazardous Waste: This includes chemicals or materials that pose significant risks to health or the environment, such as certain laboratory reagents.
To ensure comprehensive identification of refuse types specific to your facility’s operations, utilize resources such as the guidelines provided by the CDC and WHO. These organizations emphasize the critical importance of accurate refuse identification, noting that approximately 15% of materials produced by healthcare activities are deemed hazardous or biohazardous. Implementing effective refuse identification strategies not only enhances safety but also ensures regulatory compliance, ultimately supporting the operational efficiency of healthcare facilities.
Implement Waste Segregation Practices
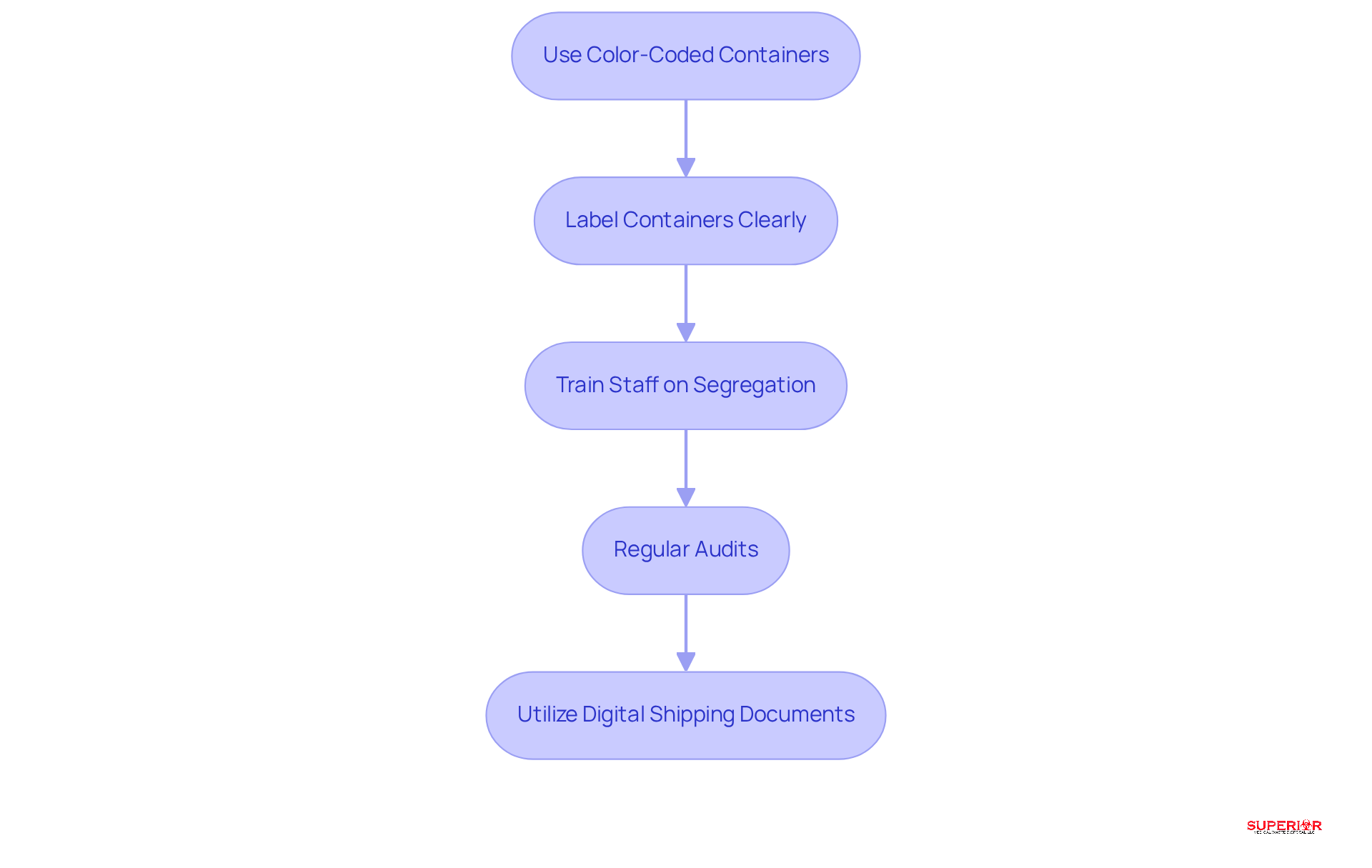
To ensure the safe handling of clinical refuse, effective segregation practices are essential for the proper disposal of clinical waste. Here are key steps to follow:
-
Use Color-Coded Containers: Designate specific colors for different types of refuse – red for infectious materials, yellow for sharps, and white for general items. This system simplifies identification and promotes compliance with regulations. Given that hospital patients in the United States produce approximately 33.8 pounds of refuse daily, proper segregation is vital for managing this volume effectively.
-
Label Containers Clearly: Clearly identify each container with its designated refuse type to prevent cross-contamination and ensure proper disposal. This practice aligns with OSHA and EPA guidelines, which emphasize the importance of precise material segregation in the disposal of clinical waste. Notably, 15% of refuse produced by healthcare activities is classified as hazardous or biohazardous, underscoring the necessity for strict adherence to the disposal of clinical waste.
-
Train Staff on Segregation: Conduct comprehensive training sessions to educate staff on the significance of proper material segregation and the correct use of color-coded containers. Enhanced training has been shown to improve adherence and reduce instances of mishandling, particularly in the disposal of clinical waste, which can lead to the spread of infectious diseases. Superior Medical Waste Disposal offers online OSHA training services to equip your staff with essential knowledge and resources, ensuring they are prepared to manage refuse safely.
-
Regular Audits: Implement regular audits to assess compliance with segregation practices and identify areas for improvement. Monitoring processes related to the disposal of clinical waste helps uphold safety standards and ensures compliance with evolving regulations, which are becoming increasingly stringent by 2026. As Daniels Health notes, focusing on the disposal of clinical waste is crucial for reducing the environmental impact of healthcare and ensuring sustainable practices.
-
Utilize Digital Shipping Documents: Ensure that your facility maintains digital shipping documents for refuse removal, providing a clear record of transport and treatment. This documentation is essential for compliance and monitoring the waste management process.
By adopting these practices, healthcare facilities can significantly enhance their strategies for the disposal of clinical waste, reduce environmental impact, and ensure the safety of both staff and patients.
Choose Appropriate Disposal Methods
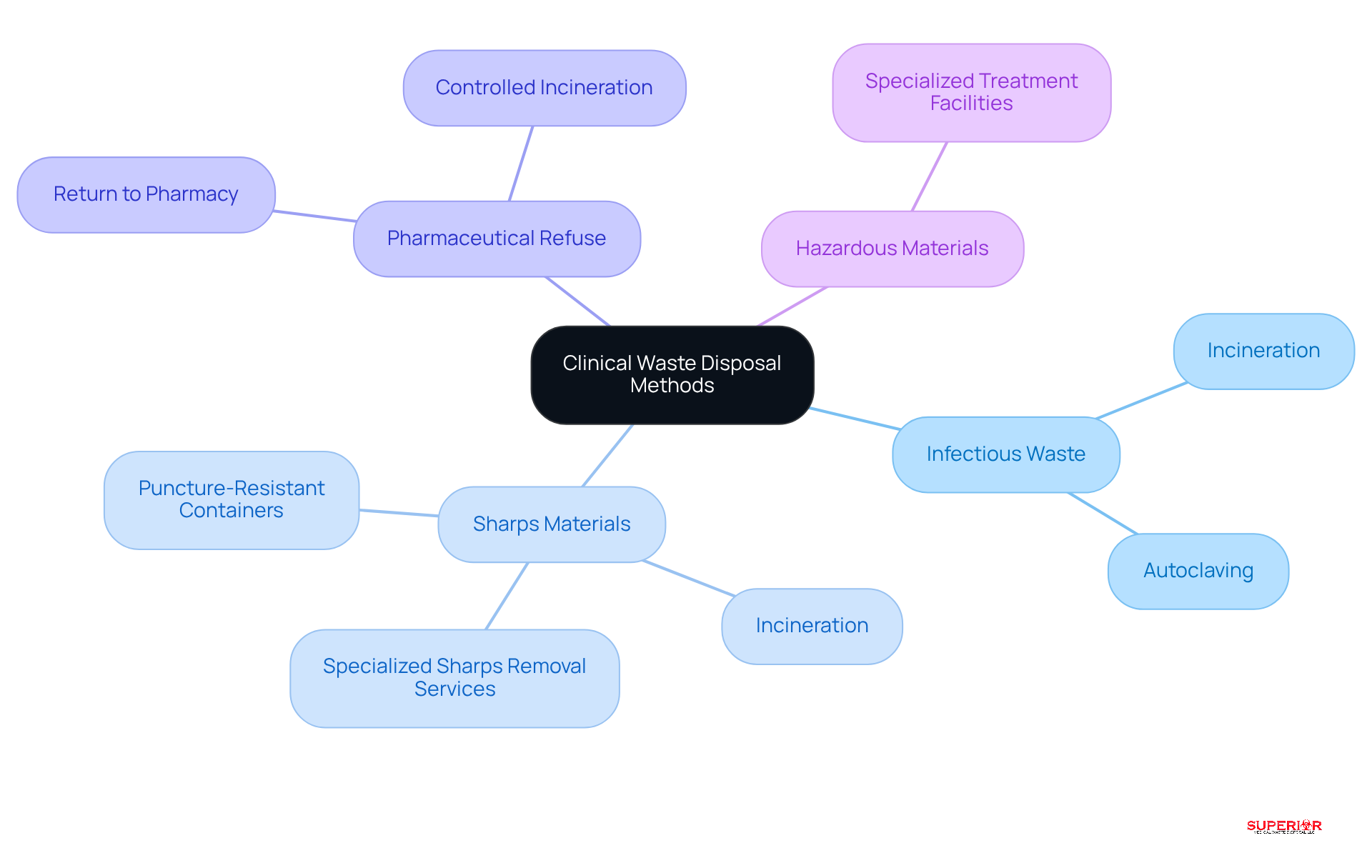
After proper segregation, determining the appropriate disposal methods for each type of clinical waste is crucial:
-
Infectious Waste: This waste is typically disposed of through incineration or autoclaving, both of which effectively eliminate pathogens. Incineration is favored for its ability to reduce waste volume and destroy harmful microorganisms. In contrast, autoclaving uses steam under pressure to sterilize waste, making it safe for landfill disposal. Superior Medical Refuse Disposal collaborates with a commercial autoclaving facility to ensure compliance with Ohio EPA regulations.
-
Sharps Materials: Sharps must be placed in puncture-resistant containers to prevent injuries and are eliminated through incineration or specialized sharps removal services. Statistics indicate that millions of healthcare workers are at risk of sharps injuries each year, underscoring the significance of proper waste management techniques.
-
Pharmaceutical Refuse: This category of refuse should be returned to a pharmacy for safe disposal or incinerated in a controlled environment to prevent environmental contamination. Superior Medical Disposal provides pharmaceutical refuse handling and removal services, along with OSHA compliance training for staff to ensure adherence to legal requirements and protect patient health information (PHI).
-
Hazardous Materials: These require treatment through specialized facilities that comply with environmental regulations. The EPA’s Hazardous Substance Pharmaceuticals Rule emphasizes the necessity for appropriate segregation and elimination to mitigate risks linked to hazardous materials. Superior Medical Waste Management offers professional hazardous material removal services to guarantee adherence and safety.
Consult local regulations and guidelines from the Ohio EPA and CDC to ensure compliance with disposal methods, as rules continue to evolve and adapt to new challenges in refuse management.
Ensure Regulatory Compliance
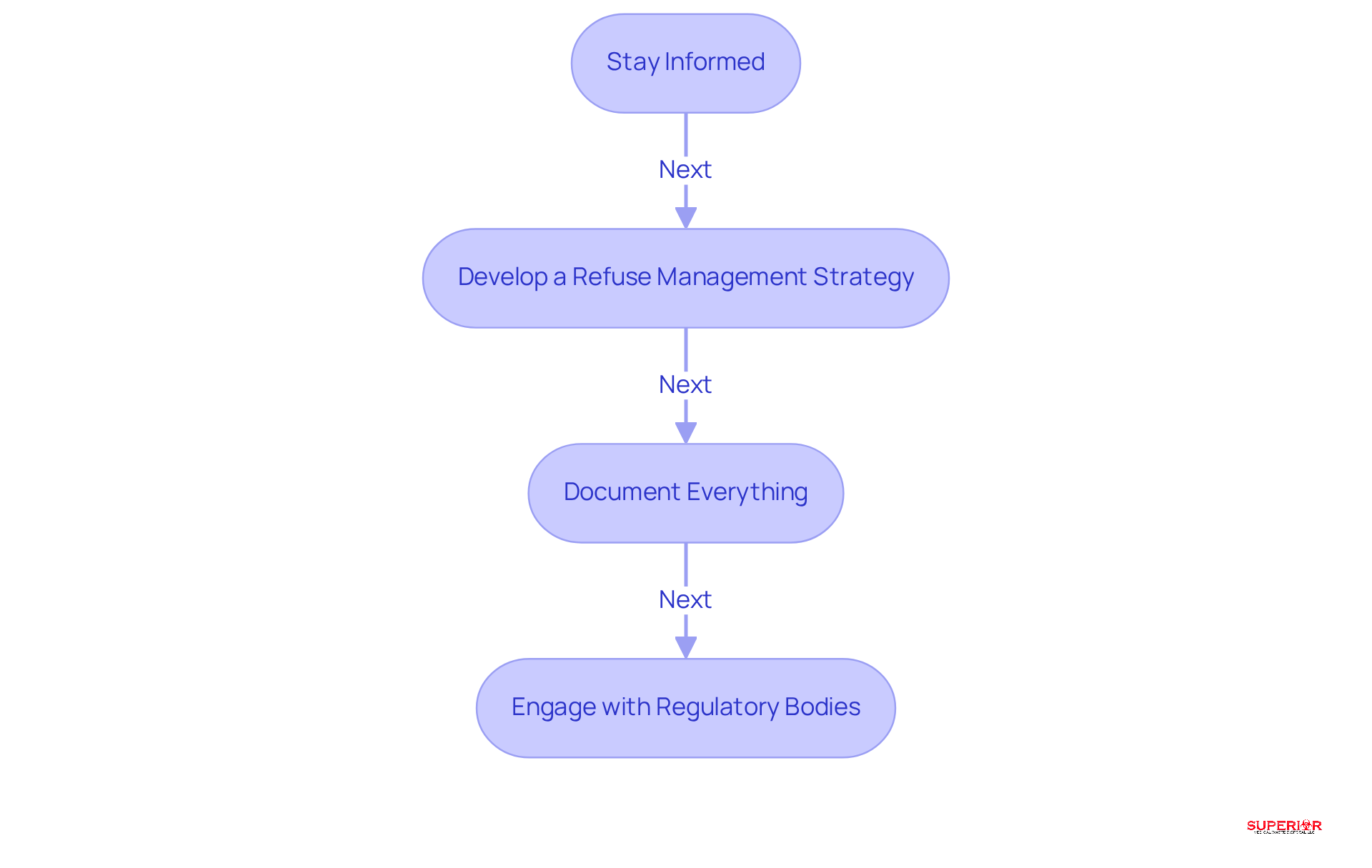
To ensure compliance with medical waste regulations, healthcare facilities must adhere to specific guidelines:
-
Stay Informed: Regularly review both state and federal regulations regarding medical refuse management, including OSHA and EPA standards. By 2026, healthcare organizations are expected to demonstrate clear responsibility and consistent procedures in their disposal management practices, reflecting the evolving regulatory landscape.
-
Develop a Refuse Management Strategy: Establish a comprehensive refuse management strategy that outlines procedures for handling, segregation, and removal. This plan should include protocols for managing protected health information (PHI) throughout its lifecycle, as improper disposal can lead to significant regulatory risks, including HIPAA violations.
-
Document Everything: Keep detailed records of refuse generation, disposal methods, and training sessions. Effective documentation is crucial for demonstrating compliance during inspections and audits, particularly as regulators increasingly scrutinize the disposal of clinical waste management practices.
-
Engage with Regulatory Bodies: Maintain ongoing communication with local health departments and regulatory agencies to stay informed about changes in regulations. Proactive engagement can help facilities navigate the complexities of regulations and adapt to new requirements, such as those introduced by the EPA’s Hazardous Waste Pharmaceuticals Rule, which several states adopted in 2025.
By implementing these strategies, healthcare facilities can enhance their operational efficiency while ensuring compliance with the stringent regulations governing medical refuse management.
Train Staff on Waste Disposal Procedures
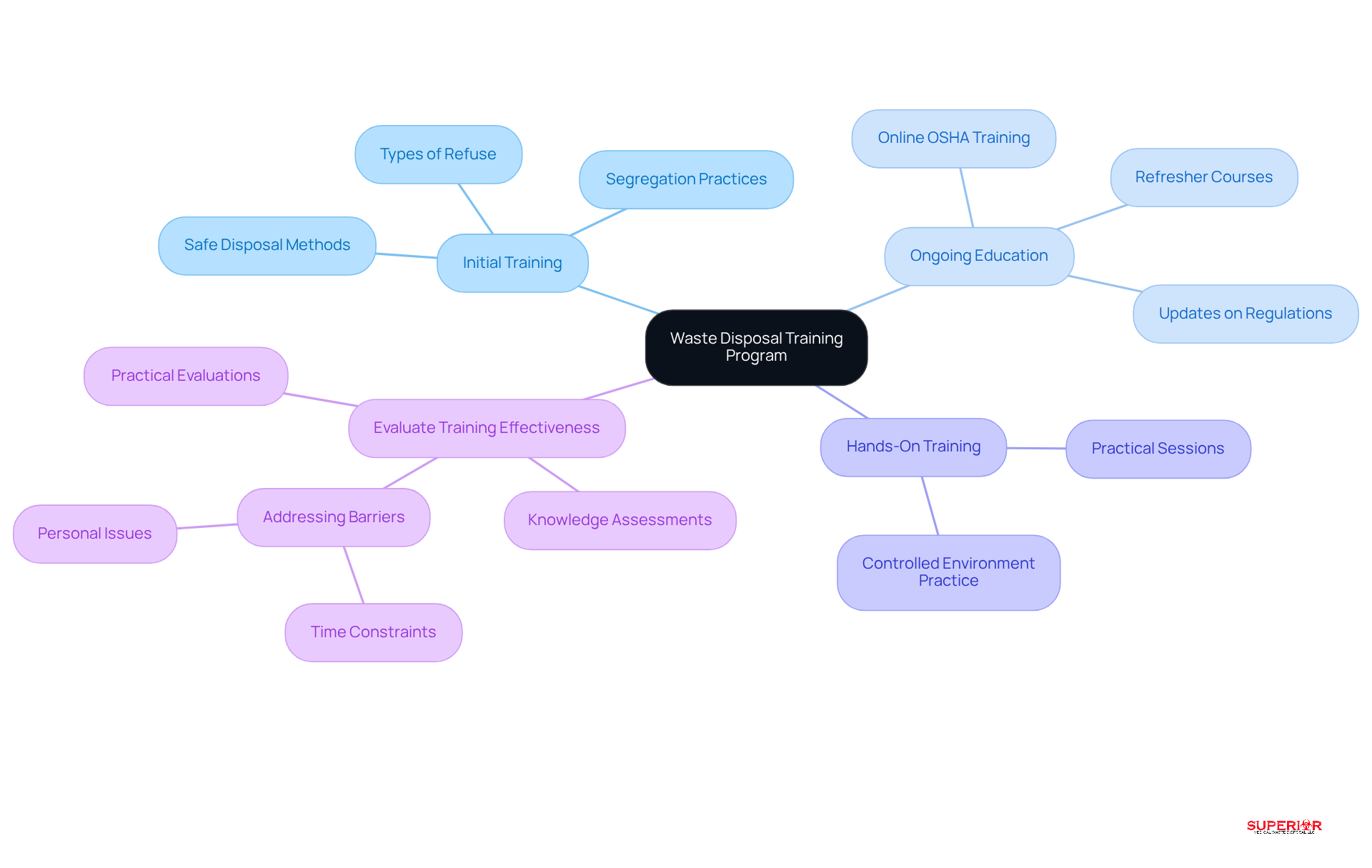
Establishing a thorough training program for all personnel engaged in refuse management is crucial for upholding high standards of safety and compliance. This program should include the following key components:
-
Initial training requires that new employees receive thorough instruction on the various types of refuse, proper segregation practices, and safe methods for the disposal of clinical waste. This essential knowledge is vital for the efficient disposal of clinical waste management and aids in reducing the environmental effect of healthcare refuse.
-
Ongoing Education: Regular refresher courses should be scheduled to keep staff informed about best practices and any changes in regulations. Ongoing education strengthens knowledge and adjusts to changing standards in resource management. Superior Medical Waste Disposal offers online OSHA training services that cover essential compliance-related topics, ensuring your entire staff is up to date with the latest safety protocols.
-
Hands-On Training: Practical sessions should be conducted, allowing staff to practice disposal of clinical waste handling techniques in a controlled environment. This experiential learning enhances confidence and competence in managing clinical materials.
-
Evaluate Training Effectiveness: Assessing staff knowledge through quizzes or practical evaluations is important. This guarantees that employees grasp the material and adhere to established protocols, ultimately resulting in enhanced resource management practices. Addressing obstacles to material segregation, such as time constraints and personal issues, is crucial for the success of these training initiatives.
By prioritizing these training elements, healthcare facilities can cultivate a culture of safety and environmental responsibility, significantly lowering the risks linked to the improper disposal of clinical waste. Incorporating statistics from case studies, such as the significant increase in recyclable waste post-training, can further demonstrate the effectiveness of these training programs.
Conclusion
Effective clinical waste management is crucial for ensuring safety and compliance in healthcare facilities. By adhering to essential steps – identifying waste types, implementing segregation practices, selecting appropriate disposal methods, ensuring regulatory compliance, and training staff – healthcare providers can significantly improve their waste disposal strategies. These practices not only safeguard staff and patients but also align with evolving regulations aimed at minimizing environmental impact.
Key insights throughout the article emphasize the importance of accurate waste identification, the necessity of proper segregation, and the critical role of training. The adoption of color-coded systems, regular audits, and comprehensive staff education are pivotal in fostering a culture of safety and responsibility. Additionally, engaging with regulatory bodies ensures that facilities remain informed and compliant with the latest guidelines.
Ultimately, effective clinical waste disposal is not merely a regulatory obligation; it is a fundamental aspect of healthcare operations that protects public health and the environment. By prioritizing these best practices, healthcare facilities can lead the way in responsible waste management, contributing to a safer and more sustainable future in healthcare.
Frequently Asked Questions
What are the main types of clinical waste identified in healthcare facilities?
The main types of clinical waste include Infectious Waste, Sharps, Pharmaceutical Refuse, and Hazardous Waste. Infectious Waste consists of materials contaminated with bodily fluids, Sharps includes items like needles and blades, Pharmaceutical Refuse pertains to expired or unused medications, and Hazardous Waste includes chemicals that pose health or environmental risks.
Why is accurate identification of clinical waste important?
Accurate identification of clinical waste is crucial for ensuring safety, regulatory compliance, and operational efficiency in healthcare facilities. Approximately 15% of materials produced by healthcare activities are classified as hazardous or biohazardous, making proper identification essential.
What practices can be implemented for effective waste segregation?
Effective waste segregation practices include using color-coded containers for different types of refuse, labeling containers clearly, training staff on proper segregation techniques, conducting regular audits for compliance, and maintaining digital shipping documents for waste removal.
What color codes are recommended for clinical waste containers?
Recommended color codes include red for infectious materials, yellow for sharps, and white for general items. This system simplifies identification and promotes compliance with regulations.
How can staff be trained on waste segregation?
Staff can be trained through comprehensive training sessions that educate them on the significance of proper material segregation and the correct use of color-coded containers. Enhanced training improves adherence and reduces mishandling of clinical waste.
What is the importance of regular audits in waste management?
Regular audits are important for assessing compliance with segregation practices, identifying areas for improvement, and ensuring adherence to safety standards and evolving regulations related to clinical waste disposal.
How do digital shipping documents contribute to waste management?
Digital shipping documents provide a clear record of the transport and treatment of clinical waste, which is essential for compliance and monitoring the waste management process.
