Introduction
Biohazardous materials pose significant risks in healthcare settings, ranging from sharp objects to infectious waste that can jeopardize human health and the environment. Managing these materials effectively is not merely a regulatory obligation; it is a crucial practice that protects healthcare workers, patients, and the broader community. The challenge, however, lies in determining how healthcare facilities can adhere to best practices while navigating complex regulations and the constantly changing landscape of biohazard waste management. This article explores essential strategies and guidelines designed to empower healthcare providers in the safe and efficient management of biohazardous materials.
Define Biohazardous Materials and Their Risks
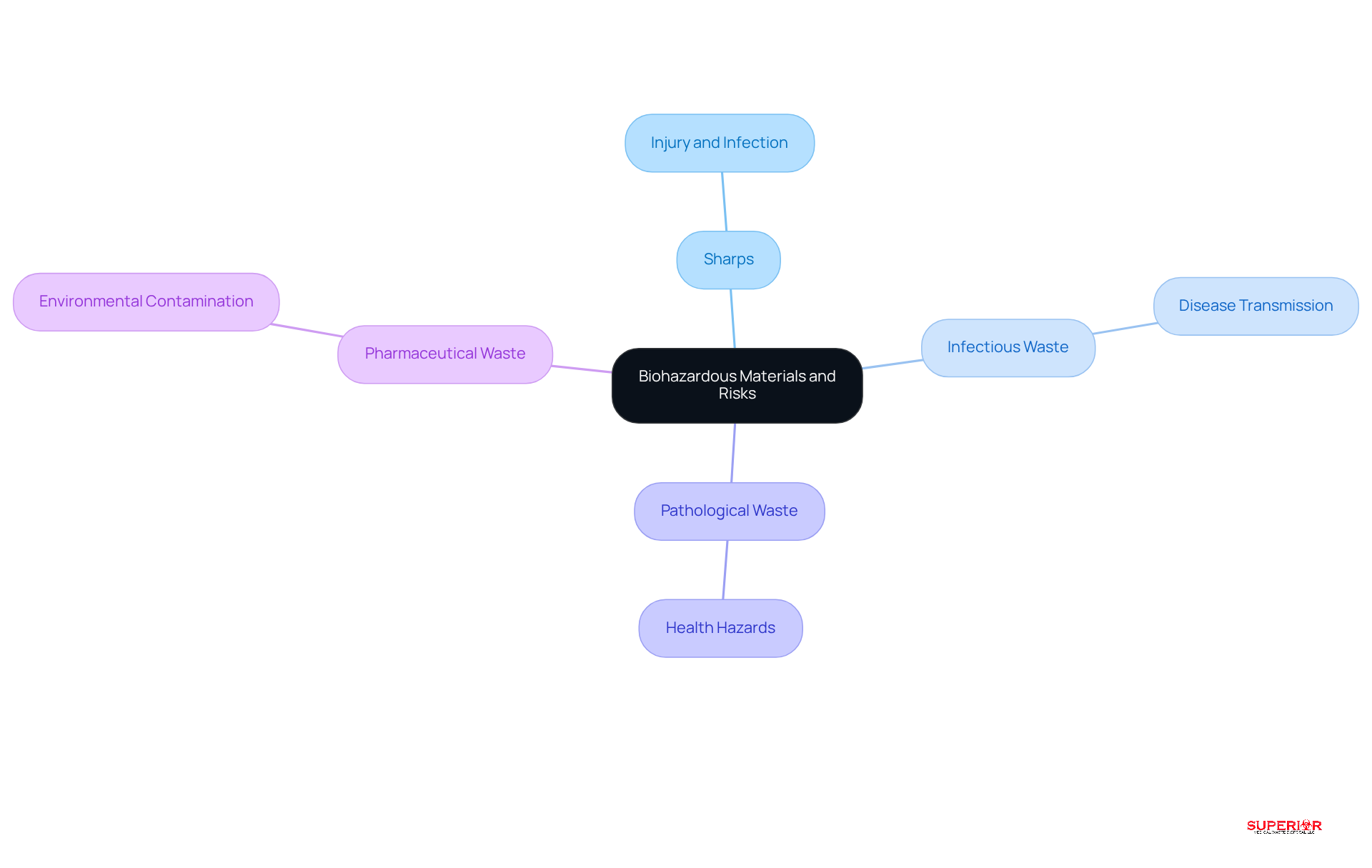
Biohazard materials encompass any waste that contains infectious agents or poses a threat to human health. The primary categories include:
- Sharps: Items such as needles, blades, and other sharp objects that can puncture skin, presenting a significant risk of injury and infection.
- Infectious Waste: Materials contaminated with blood, bodily fluids, or other potentially infectious materials (OPIM), which can transmit diseases if not handled properly.
- Pathological Waste: Human tissues, organs, and body parts that require careful disposal to prevent health hazards.
- Pharmaceutical Waste: Expired or unused medications that can be hazardous to both health and the environment if not disposed of correctly.
The dangers associated with biohazardous substances are considerable. Improper handling can lead to disease transmission, with statistics indicating that up to 30% of hepatitis B, 1-3% of hepatitis C, and 0.3% of HIV cases are linked to inadequate healthcare waste management. Furthermore, environmental contamination can occur, posing long-term risks to ecosystems and public health, such as the leaching of toxic substances into soil and water. Legal repercussions for failing to comply with regulations further underscore the necessity for stringent oversight practices.
To ensure compliance, all staff handling bloodborne pathogens must undergo training, which should be documented in accordance with the facility’s medical disposal plan and retained for review for a minimum of three years. Effective identification and management of biohazard materials are essential for the protection of healthcare workers, patients, and the environment. Additionally, ongoing training and public awareness initiatives are crucial to ensure that all personnel involved in waste disposal possess the knowledge and skills necessary to handle hazardous materials safely. At Superior Medical Disposal, we prioritize best practices in the handling of biohazard materials, including proper packaging, storage, treatment, and disposal methods, to ensure compliance with state regulations and safeguard public health. This includes adhering to specific regulations regarding hazardous material disposal, such as the requirement for the prompt removal of dangerous substances and the use of autoclaving to effectively disinfect waste prior to disposal.
Understand Regulatory Compliance for Biohazard Waste
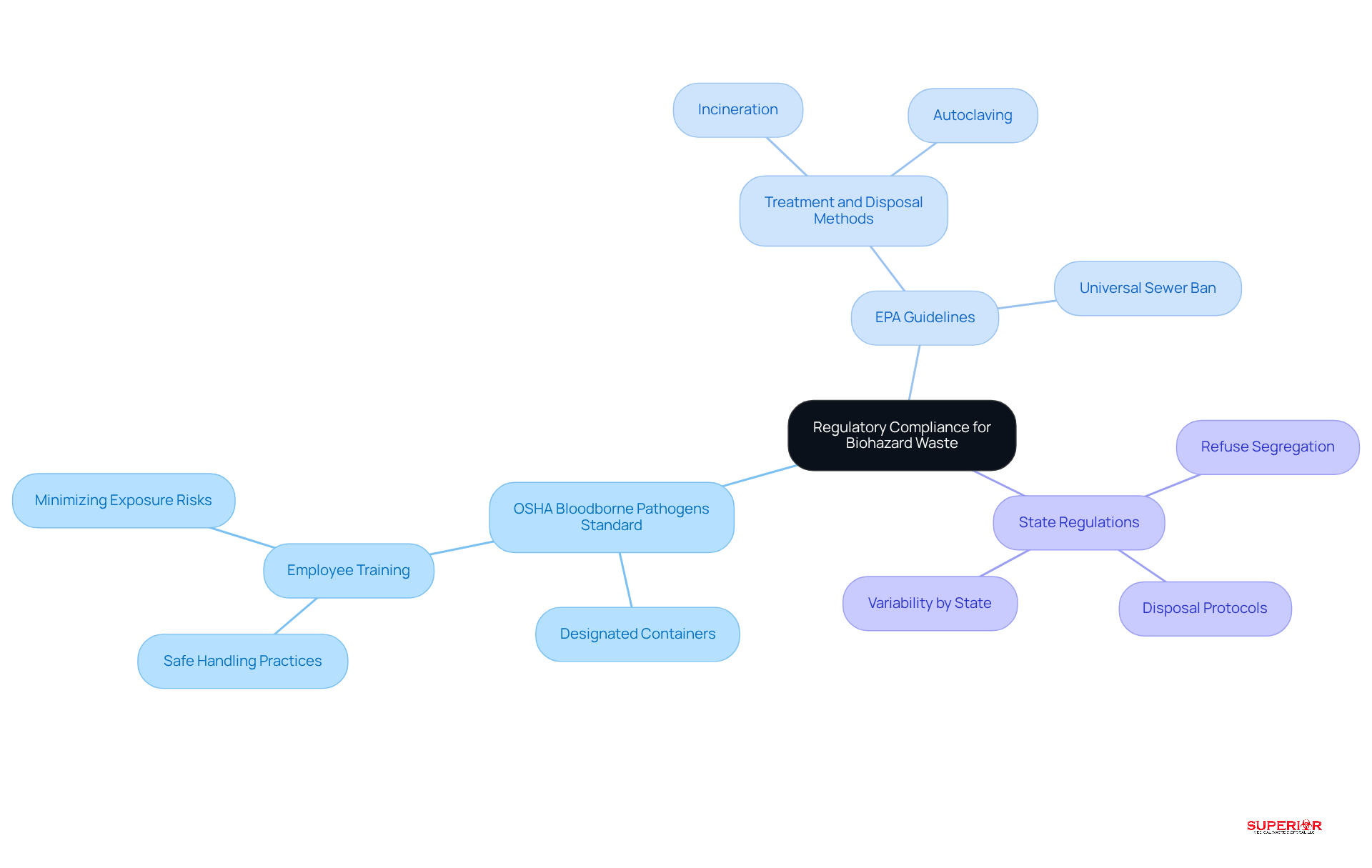
Healthcare facilities must comply with various regulations regarding biohazard materials management. These regulations include:
- OSHA Bloodborne Pathogens Standard: This standard requires the use of designated containers for sharps and infectious waste. It also mandates comprehensive employee training on safe handling practices to minimize exposure risks.
- The Environmental Protection Agency establishes strict guidelines for the treatment and disposal of biohazard materials. It emphasizes methods such as incineration or autoclaving to ensure safe and effective handling.
- State Regulations: These regulations can differ significantly from one state to another, often imposing additional requirements for refuse segregation and disposal protocols.
To ensure compliance, facilities should regularly review and update their management policies. This practice guarantees that all staff members are well-trained and fully aware of the latest compliance requirements. Such a proactive approach not only protects public health but also aligns with effective practices in environmental sustainability.
Implement Best Practices for Segregation and Disposal
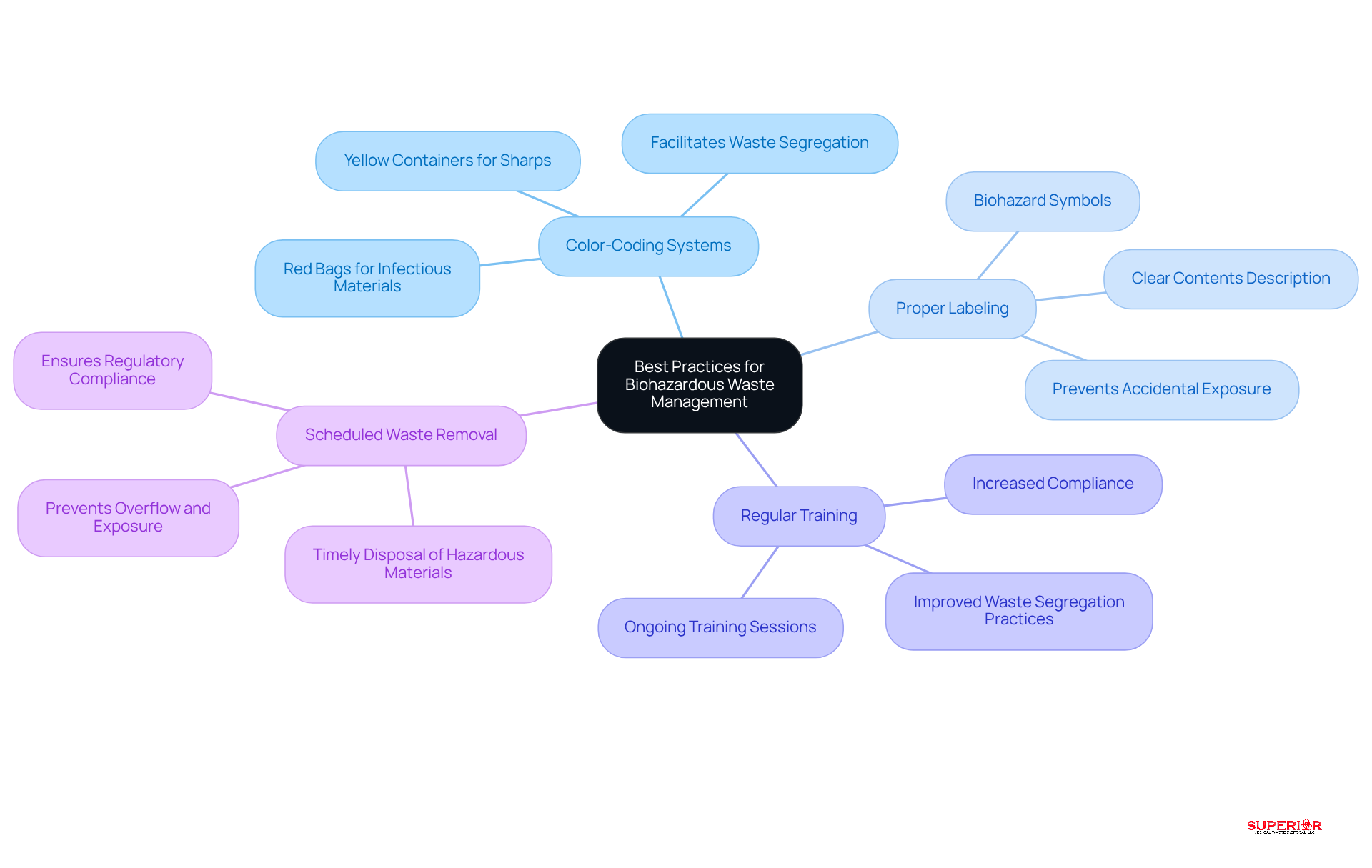
To effectively manage biohazardous waste, healthcare facilities should adopt several best practices:
-
Color-Coding Systems: Implementing color-coded containers is essential for clearly differentiating between types of waste. For example, red bags should be designated for infectious materials, while yellow containers are reserved for sharps. This system simplifies refuse segregation and minimizes the risk of cross-contamination.
-
Proper Labeling: All containers must be clearly labeled with biohazard symbols and specific contents. This practice is crucial in preventing accidental exposure and ensuring that all staff members are aware of the potential dangers associated with the materials they handle.
-
Regular Training: Ongoing training sessions for staff on proper material segregation techniques and disposal methods are vital. Research indicates that healthcare personnel who undergo training are significantly more inclined to implement efficient garbage separation, thereby minimizing the dangers linked to incorrect disposal.
-
Scheduled Waste Removal: Establishing a routine for the timely disposal of hazardous materials is critical to prevent overflow and potential exposure. Regular collection schedules help maintain a safe environment and ensure compliance with regulatory standards.
By adopting these practices, facilities can significantly reduce the dangers associated with biohazard materials and enhance their adherence to health and safety regulations.
Train Staff on Safe Handling and Compliance Procedures
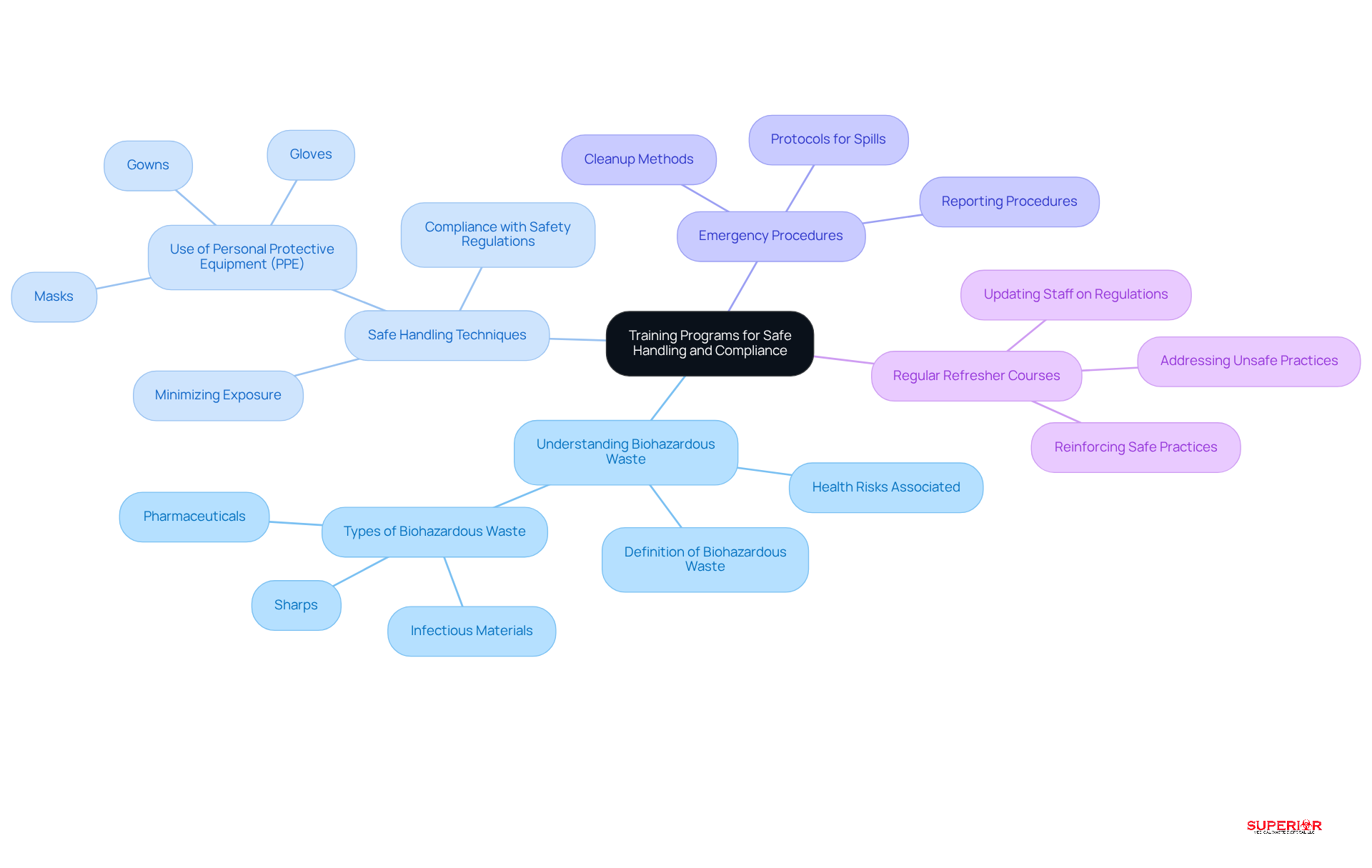
Training programs for healthcare staff are essential for the effective management of biohazard materials. These programs should encompass several critical components:
-
Understanding Biohazardous Waste: It is crucial for staff to be educated on what constitutes biohazardous waste, including sharps, infectious materials, and pharmaceuticals, as well as the associated health risks. This foundational knowledge is vital for safe practices.
-
Safe Handling Techniques: Training must focus on the proper use of personal protective equipment (PPE), such as gloves, masks, and gowns. This minimizes exposure during disposal handling. Emphasizing safe handling practices is essential to prevent accidents and ensure compliance with safety regulations.
-
Emergency Procedures: Clear protocols should be established for responding to spills or exposure incidents. Staff must be trained on immediate actions to take, including reporting procedures and cleanup methods, to effectively mitigate risks.
-
Regular Refresher Courses: To keep staff updated on evolving regulations and best practices, periodic training updates are crucial. These refresher courses reinforce essential concepts and rectify unsafe practices, ensuring that all personnel remain compliant and informed about hazardous waste management.
By prioritizing comprehensive training, healthcare facilities can cultivate a safer work environment, enhance staff confidence in handling biohazard materials, and ensure adherence to regulatory requirements.
Conclusion
Effective management of biohazard materials in healthcare is essential for protecting human health and the environment. Understanding the risks associated with biohazardous waste and adhering to regulatory compliance enables healthcare facilities to mitigate potential dangers and enhance safety protocols. Implementing best practices in waste segregation, disposal, and staff training is vital for achieving these objectives.
This article underscores the importance of recognizing the various types of biohazard materials, such as:
- sharps
- infectious waste
- pathological waste
- pharmaceutical waste
It highlights the necessity for proper handling, labeling, and disposal methods to prevent disease transmission and environmental contamination. Furthermore, ongoing training for healthcare personnel is crucial to ensure they possess the knowledge and skills required to manage these materials safely and effectively.
The significance of robust biohazard waste management practices cannot be overstated. As healthcare facilities work to improve their compliance with regulations and prioritize public health, adopting these best practices will not only protect individuals but also contribute to a safer and healthier environment for all. Embracing a proactive approach to biohazard management is imperative for the future of healthcare safety and sustainability.
Frequently Asked Questions
What are biohazardous materials?
Biohazardous materials are any waste that contains infectious agents or poses a threat to human health. They include sharps, infectious waste, pathological waste, and pharmaceutical waste.
What are examples of sharps?
Sharps include items such as needles, blades, and other sharp objects that can puncture skin, presenting a significant risk of injury and infection.
What constitutes infectious waste?
Infectious waste consists of materials contaminated with blood, bodily fluids, or other potentially infectious materials (OPIM) that can transmit diseases if not handled properly.
What is pathological waste?
Pathological waste refers to human tissues, organs, and body parts that require careful disposal to prevent health hazards.
Why is pharmaceutical waste considered hazardous?
Pharmaceutical waste includes expired or unused medications that can be hazardous to both health and the environment if not disposed of correctly.
What are the risks associated with improper handling of biohazardous materials?
Improper handling can lead to disease transmission, with statistics indicating that up to 30% of hepatitis B, 1-3% of hepatitis C, and 0.3% of HIV cases are linked to inadequate healthcare waste management. It can also result in environmental contamination and legal repercussions.
What training is required for staff handling biohazard materials?
All staff handling bloodborne pathogens must undergo training, which should be documented according to the facility’s medical disposal plan and retained for a minimum of three years.
What practices are essential for managing biohazard materials?
Effective identification and management of biohazard materials are essential, including proper packaging, storage, treatment, and disposal methods to ensure compliance with state regulations and safeguard public health.
How does Superior Medical Disposal ensure safety in handling biohazard materials?
Superior Medical Disposal prioritizes best practices, including adherence to regulations regarding hazardous material disposal, prompt removal of dangerous substances, and the use of autoclaving to effectively disinfect waste prior to disposal.
