Introduction
Healthcare facilities encounter a significant challenge in managing pathological waste, which includes potentially hazardous materials derived from human and animal bodies. With the volume of medical refuse on the rise – especially following recent global health crises – understanding and implementing effective waste disposal practices is more critical than ever. Healthcare providers must navigate complex regulations while ensuring the safety of their staff and patients. This article explores essential strategies for effective pathological waste management, emphasizing the importance of:
- Proper segregation
- Labeling
- Staff training
to cultivate a culture of safety and compliance.
Define Pathological Waste: Key Characteristics and Types
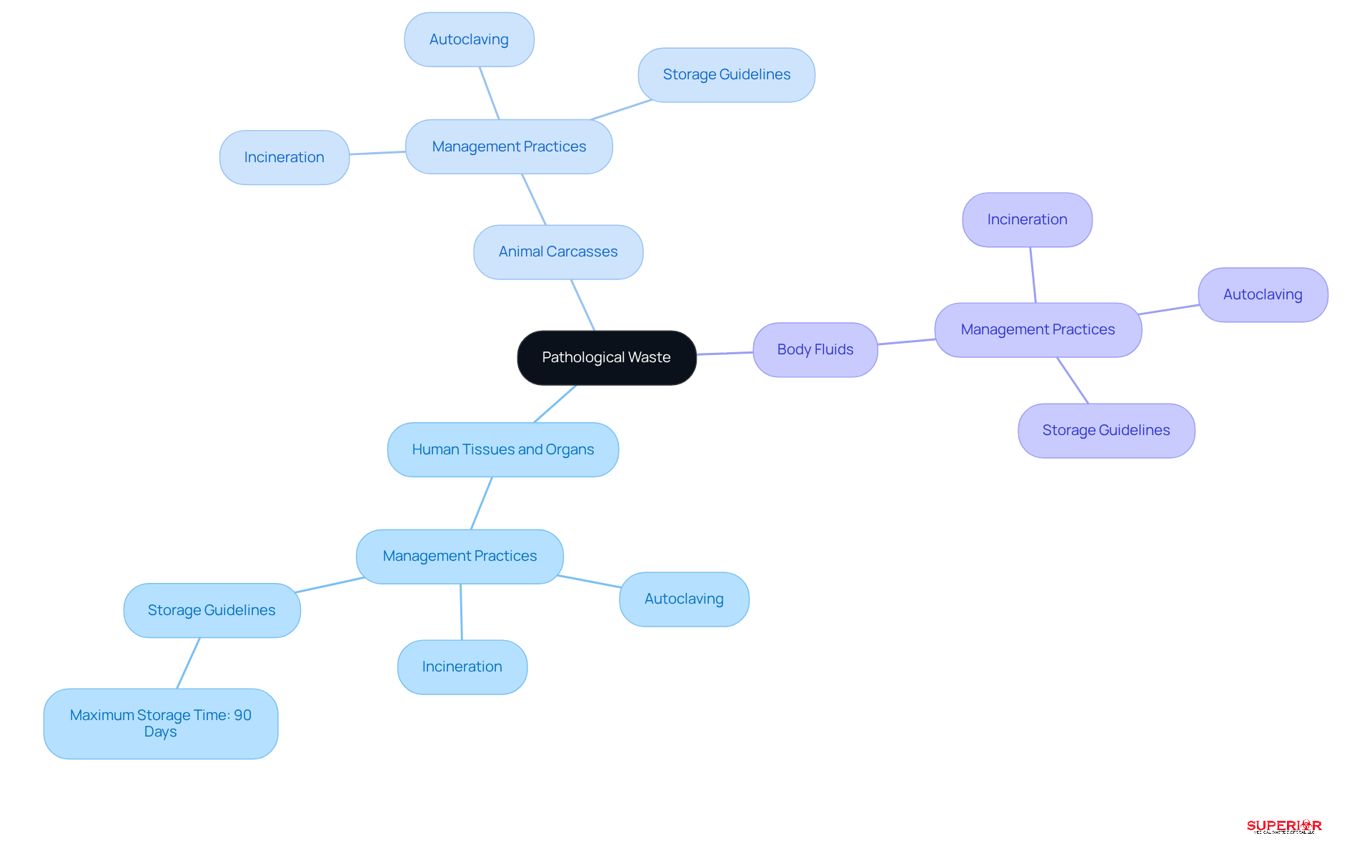
Pathological refuse encompasses any material derived from human or animal bodies that may pose a risk of infection or contamination. This category includes:
- Human tissues and organs: These are typically removed during surgeries, autopsies, or biopsies.
- Animal carcasses: Often utilized in research or veterinary practices.
- Body fluids: Such as blood, urine, and other bodily secretions that may harbor infectious agents.
Identifying these forms of refuse is essential for healthcare establishments to ensure appropriate management and pathological waste disposal techniques. Commonly, incineration is employed as a method of pathological waste disposal to mitigate health hazards. Furthermore, adherence to medical disposal regulations is critical, particularly in relation to pathological waste disposal; facilities must document their management plans and ensure that all staff handling bloodborne pathogens receive adequate training.
Moreover, it is vital to follow specific guidelines for the management of pathological waste disposal. This includes utilizing autoclaves for treating refuse and adhering to a maximum storage time of 90 days before proper removal by a licensed medical refuse hauler. Superior Medical Disposal underscores the importance of following these guidelines to uphold safety and regulatory compliance in the management of pathological materials.
Understand Regulatory Compliance: Federal and State Guidelines
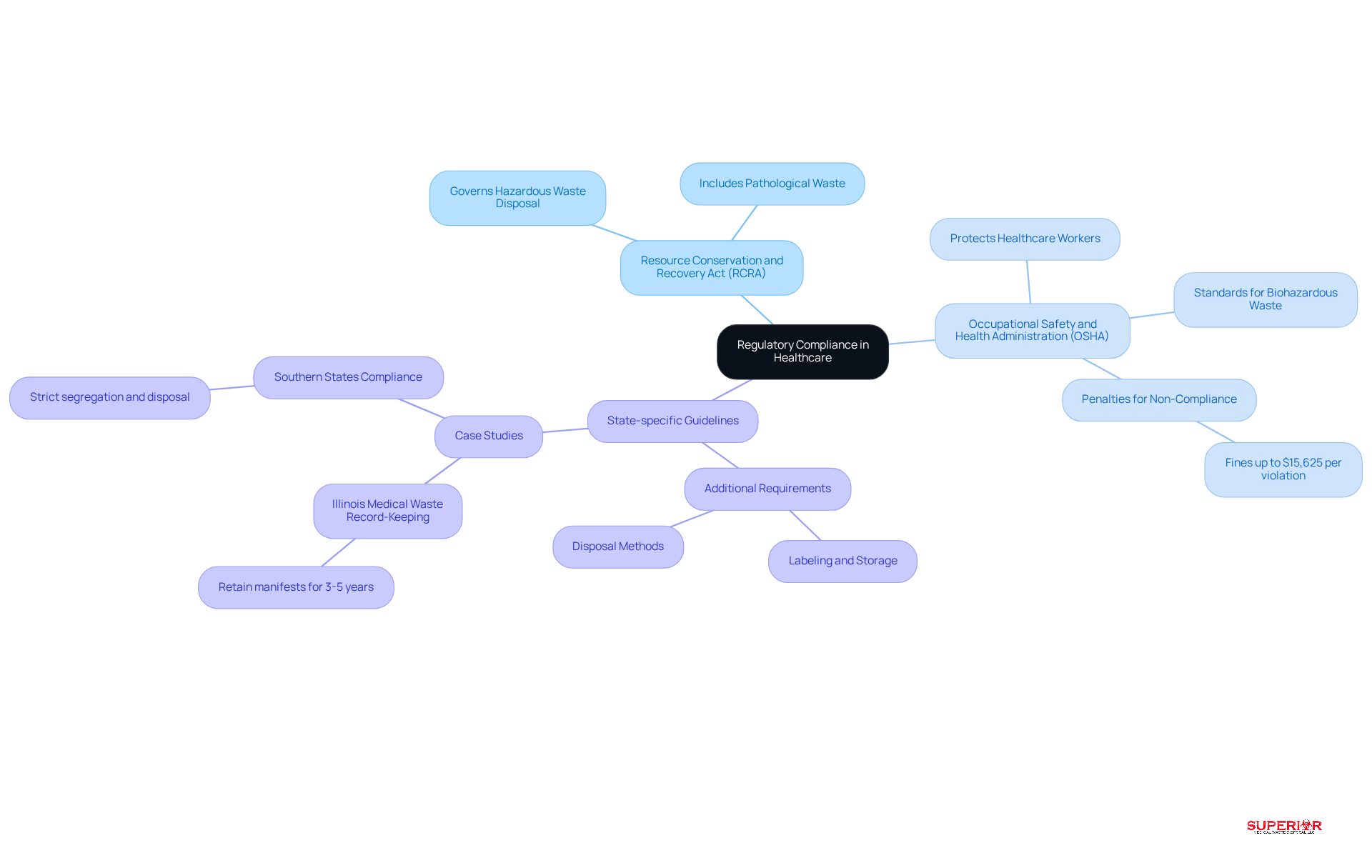
Healthcare facilities are required to comply with various federal and state guidelines regarding pathological waste disposal. The key regulations include:
- Resource Conservation and Recovery Act (RCRA): This act governs the disposal of hazardous waste, which encompasses certain types of pathological waste.
- Occupational Safety and Health Administration (OSHA): OSHA establishes standards for the handling and disposal of biohazardous waste, including guidelines for pathological waste disposal, aimed at protecting healthcare workers.
- State-specific guidelines: Each state may impose additional requirements that healthcare facilities must follow, including specific labeling, storage, and disposal methods.
At Superior Medical Waste Disposal, we leverage our extensive network of collaborations with leading organizations in the healthcare sector to ensure our clients fully comply with these regulations. Our expertise in regulatory adherence and environmental sustainability practices allows us to provide tailored solutions for the safe management and pathological waste disposal of medical materials. It is essential for facilities to regularly assess these regulations to ensure compliance and avoid potential penalties. We are committed to supporting them throughout this process.
Implement Best Practices: Segregation and Labeling of Pathological Waste
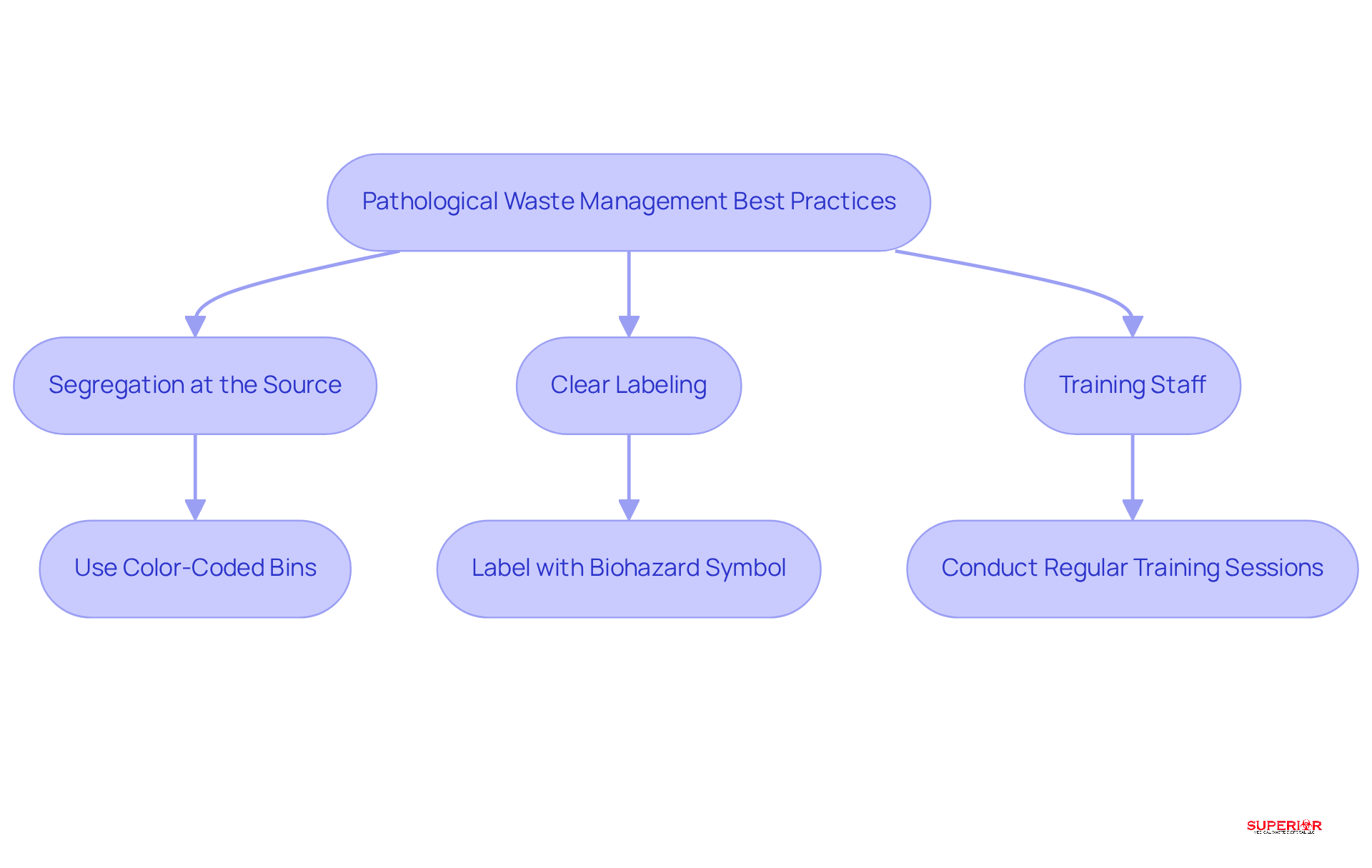
To effectively manage pathological waste, healthcare facilities should adopt several best practices:
-
Segregation at the source: Waste must be separated immediately after generation to prevent contamination. Utilizing standardized color-coded bins specifically designated for pathological waste disposal is essential for clear identification and compliance. This is particularly important given the increase in medical refuse production, which rose by an estimated 3.4 kg per bed per day during the COVID-19 pandemic.
-
Clear labeling is essential: Containers should be distinctly labeled with the words ‘Pathological Waste Disposal’ alongside the biohazard symbol. This practice ensures that all staff members recognize the potential dangers associated with the refuse, thereby enhancing safety protocols. Experts emphasize that appropriate labeling is crucial for compliance and minimizing hazards in the context of pathological waste disposal.
-
Training staff: Regular training sessions are vital for educating staff on proper segregation and labeling techniques. This underscores the importance of adherence and safety, ensuring that all personnel are informed of the latest guidelines and best practices. Addressing challenges such as a lack of knowledge among professionals and regulatory complexities is essential for effective waste management.
Additionally, healthcare facilities should consult local environmental authorities regarding regulations and handling procedures specific to pathological waste disposal in their state. For example, in Michigan, biohazard materials must be removed by a licensed medical waste hauler within 90 days of storage. At Superior Medical Waste Disposal, we ensure that our biohazard material is not only autoclaved to eliminate biological threats but also shredded to reduce volume by 70% before disposal in a sanitary landfill. By adopting these practices, establishments can significantly enhance their waste management procedures, ensuring compliance with regulatory standards while fostering a safer environment for both personnel and patients.
Prioritize Staff Training: Ensuring Compliance and Safety in Waste Disposal
To ensure compliance and safety in pathological waste disposal, healthcare facilities must prioritize staff training. This approach is essential for cultivating a culture of safety and compliance, effectively mitigating the risks associated with the disposal of pathological waste.
-
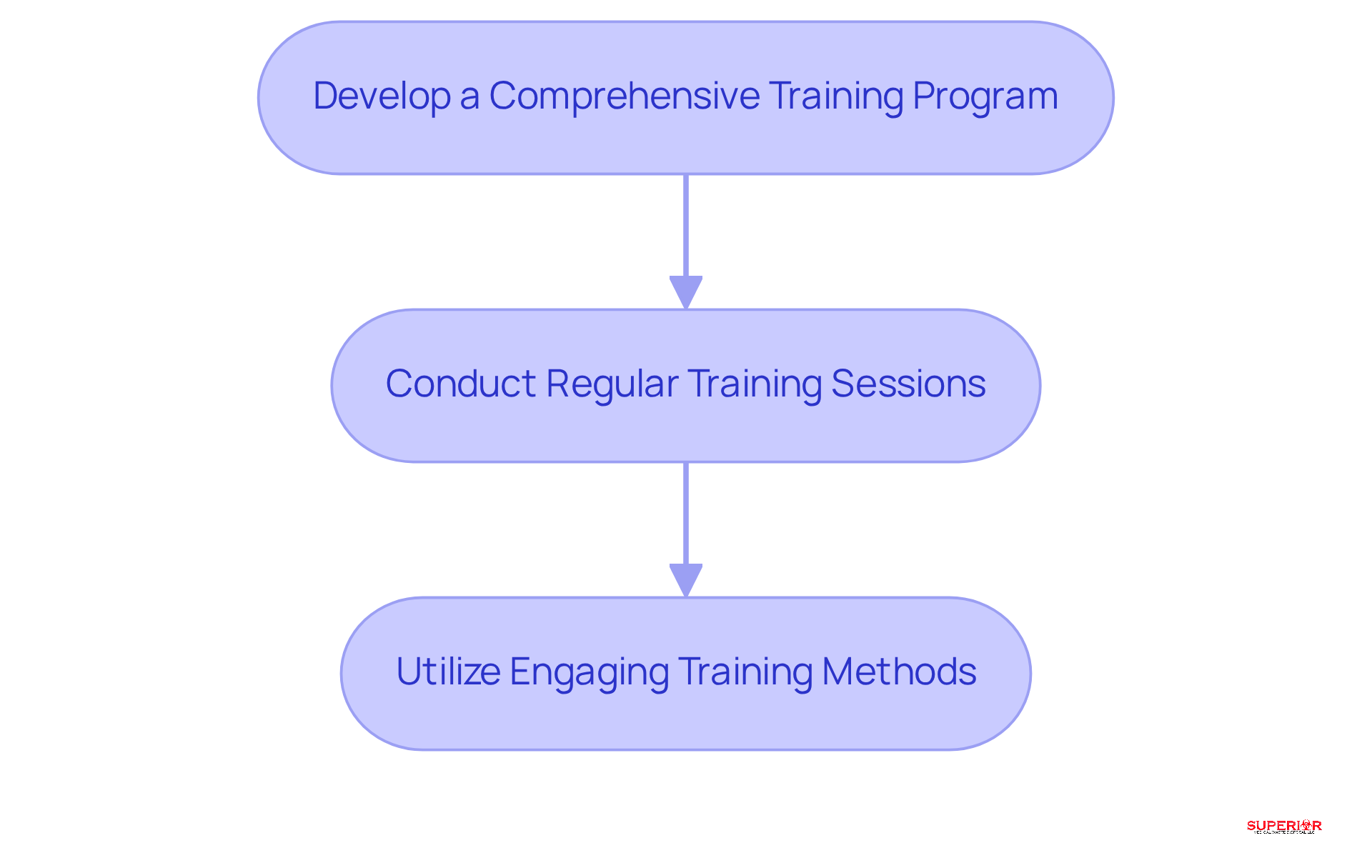
Develop a comprehensive training program: A robust training program should cover the various types of pathological waste, proper handling techniques, and the latest regulatory requirements. A well-structured curriculum equips staff with the necessary knowledge and skills to effectively manage pathological waste disposal.
-
Conduct regular training sessions: Ongoing training is vital to keep staff informed about changes in regulations and best practices. Frequent updates emphasize the importance of adherence and safety in pathological waste disposal, ensuring that staff remain vigilant and knowledgeable.
-
Utilize engaging training methods: Incorporating interactive elements such as quizzes, simulations, and hands-on demonstrations can significantly enhance learning and retention. These methods not only make training more enjoyable but also prepare staff for safe and effective pathological waste disposal.
Conclusion
Effective management of pathological waste is essential for healthcare facilities, ensuring safety and regulatory compliance. This article underscores the importance of understanding the characteristics and types of pathological waste, adhering to federal and state guidelines, and implementing best practices for waste segregation, labeling, and staff training. By prioritizing these aspects, healthcare establishments can mitigate risks and maintain a safe environment for both staff and patients.
Key insights include:
- The necessity of proper identification of pathological waste
- The significance of compliance with regulations such as the Resource Conservation and Recovery Act (RCRA) and OSHA standards
- The implementation of effective waste management practices
Furthermore, the article highlights the critical role of staff training in fostering a culture of safety and compliance, ensuring that personnel are well-equipped to handle pathological waste responsibly.
In conclusion, managing pathological waste is not merely a regulatory obligation; it is a fundamental component of healthcare safety. By adopting best practices, maintaining compliance, and committing to ongoing education, healthcare facilities can significantly enhance their waste disposal processes. This proactive approach not only safeguards the health of staff and patients but also contributes to a more sustainable healthcare system. Embracing these practices is vital for any facility striving to excel in waste management and uphold the highest standards of safety and compliance.
Frequently Asked Questions
What is pathological waste?
Pathological waste refers to any material derived from human or animal bodies that may pose a risk of infection or contamination.
What types of materials are considered pathological waste?
Pathological waste includes human tissues and organs removed during surgeries, autopsies, or biopsies; animal carcasses used in research or veterinary practices; and body fluids such as blood, urine, and other bodily secretions that may harbor infectious agents.
Why is it important to identify pathological waste?
Identifying pathological waste is essential for healthcare establishments to ensure appropriate management and disposal techniques, reducing the risk of infection and contamination.
What is a common method for disposing of pathological waste?
Incineration is commonly employed as a method of pathological waste disposal to mitigate health hazards.
What regulations must healthcare facilities follow regarding pathological waste disposal?
Healthcare facilities must adhere to medical disposal regulations, document their management plans, and ensure that all staff handling bloodborne pathogens receive adequate training.
What guidelines should be followed for managing pathological waste?
Guidelines include utilizing autoclaves for treating refuse and adhering to a maximum storage time of 90 days before proper removal by a licensed medical refuse hauler.
Why is compliance with disposal guidelines important?
Compliance with disposal guidelines is crucial to uphold safety and regulatory standards in the management of pathological materials.
