Introduction
The healthcare sector is vital to public health, yet it generates an alarming amount of biomedical waste – over 5.9 million tons annually in the U.S. alone. Effective disposal of this waste is not merely a regulatory requirement; it is essential for safeguarding both the environment and community health. Given the various types of biomedical waste and the complex web of regulations, how can healthcare facilities ensure they manage this waste safely and effectively?
This article delves into best practices for biomedical waste disposal, providing insights into regulatory compliance and strategies for safe handling. By doing so, it empowers healthcare providers to minimize risks and uphold their commitment to public safety.
Identify Types of Biomedical Waste in Healthcare Facilities
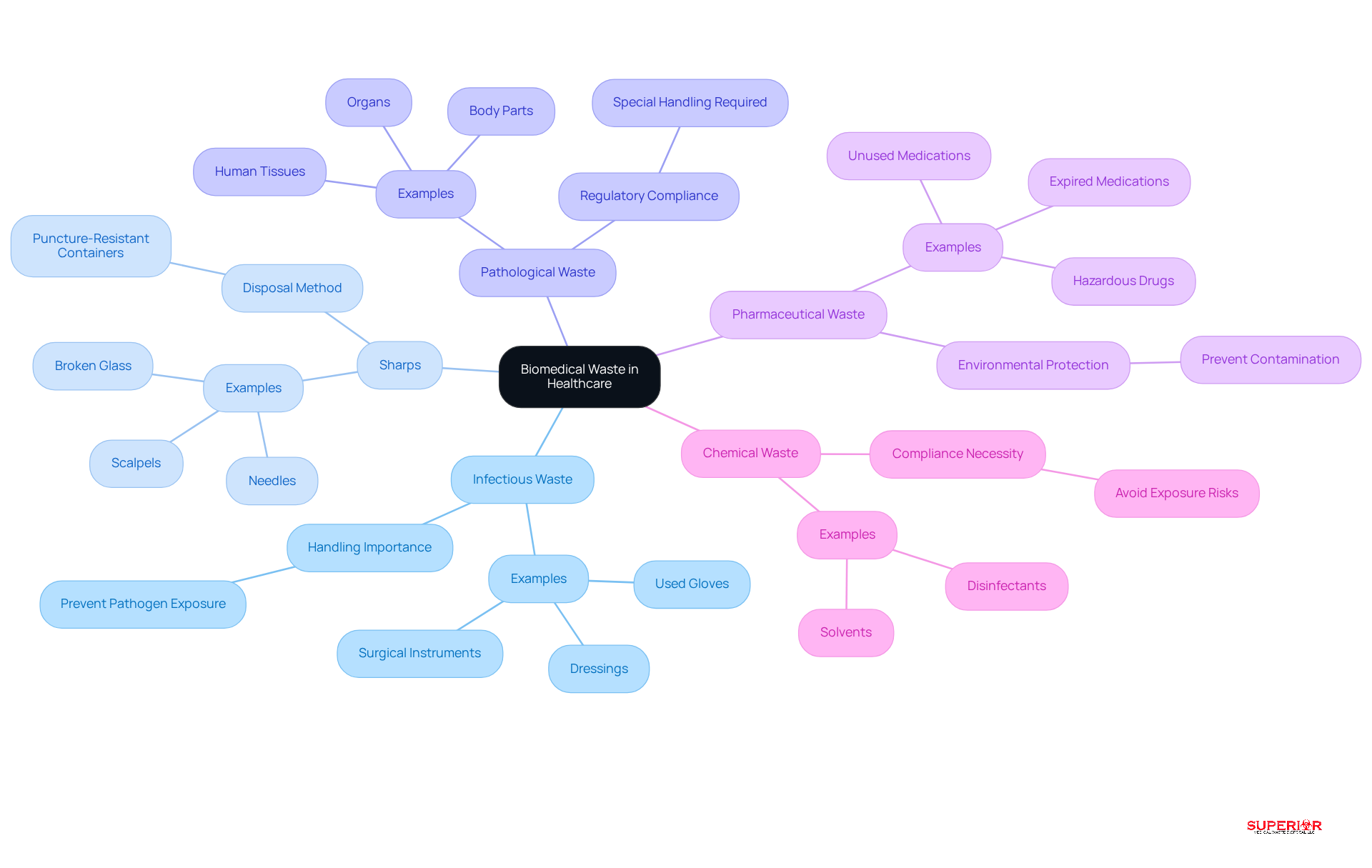
Healthcare facilities generate various types of biomedical waste, which can be categorized into several distinct groups:
- Infectious Waste: This category includes materials contaminated with blood, bodily fluids, or other potentially infectious materials (OPIM). Common examples are used gloves, dressings, and surgical instruments. Proper handling is crucial to prevent exposure to pathogens.
- Sharps: Items that can puncture or cut skin, such as needles, scalpels, and broken glass, are classified as sharps. It is essential to dispose of these items in puncture-resistant containers to mitigate injury risks and ensure safe disposal.
- Pathological Waste: This includes human tissues, organs, and body parts that require special handling and disposal methods due to their potential health risks. Facilities must adhere to strict regulations when managing this type of refuse.
- Pharmaceutical Waste: Expired or unused medications, including hazardous drugs, must be disposed of according to specific regulations to prevent environmental contamination and protect public health. This refuse type is critical in preventing the spread of drug-resistant pathogens.
- Chemical Waste: This encompasses hazardous chemicals used in healthcare settings, such as solvents and disinfectants. Careful oversight is necessary to avoid exposure risks and ensure compliance with environmental regulations.
Precise identification of these refuse types allows healthcare centers to apply customized disposal strategies that adhere to local and federal regulations. With over 5.9 million tons of medical refuse generated annually in the U.S., are essential for safeguarding public health and the environment.
Understand Regulatory Requirements for Biomedical Waste Disposal
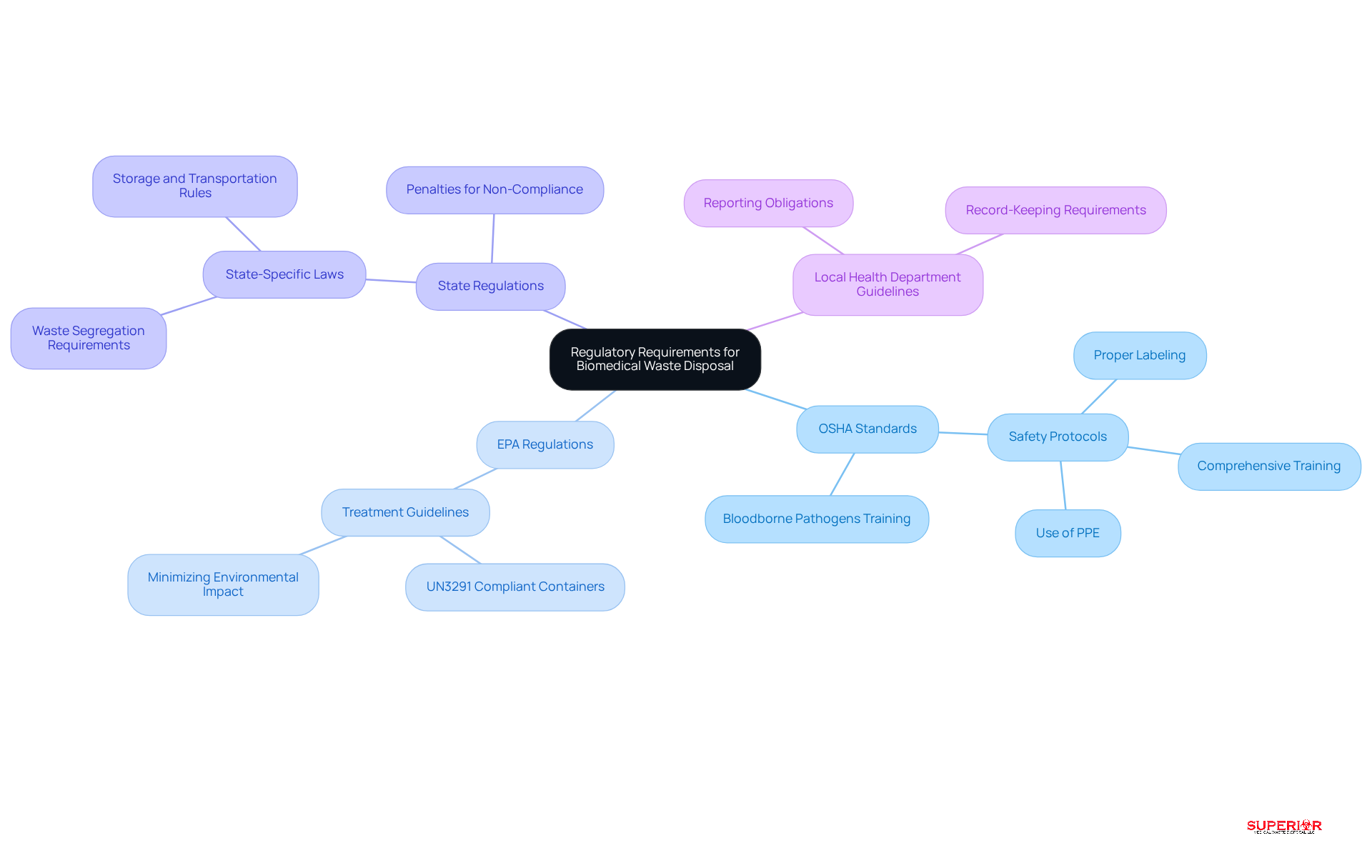
Healthcare establishments must navigate a complex landscape of federal, state, and local regulations concerning biomedical disposal. Understanding these key regulatory frameworks is essential:
- OSHA Standards: The Occupational Safety and Health Administration (OSHA) mandates that healthcare facilities implement safety protocols to protect workers from exposure to hazardous materials. This includes proper labeling, comprehensive training, and the use of personal protective equipment (PPE) to maintain a safe working environment. Superior Medical Disposal provides essential bloodborne pathogens training for all employees handling such materials, ensuring compliance with OSHA standards.
- EPA Regulations: The Environmental Protection Agency (EPA) oversees the disposal of hazardous materials, including biomedical waste. Facilities are required to adhere to EPA guidelines for treatment and disposal to minimize environmental impact, ensuring responsible management of materials throughout their lifecycle. Superior Medical Refuse Disposal employs UN3291 compliant containers for waste removal, guaranteeing safe and compliant disposal processes.
- State Regulations: Each state enforces specific laws governing biomedical waste management, often imposing stringent requirements for waste segregation, storage, and transportation. It is crucial for establishments to familiarize themselves with their respective state regulations to maintain compliance and avoid potential penalties. Superior Medical Waste Disposal offers tailored services that align with state-specific regulations, aiding organizations in effectively navigating these requirements.
- Local Health Department Guidelines: Local health departments may impose additional requirements for handling biomedical waste, including obligations for reporting and detailed record-keeping. By partnering with Superior Medical Disposal, healthcare establishments can ensure adherence to these local regulations through comprehensive management solutions and appropriate documentation.
Additionally, Superior Medical Disposal offers flexible scheduling to accommodate the specific needs of healthcare establishments, along with complimentary biohazard containers for the secure storage of sharps and medical waste prior to collection.
By thoroughly understanding and adhering to these regulatory requirements, healthcare organizations can significantly reduce the risks associated with improper waste disposal and enhance their compliance posture, ultimately safeguarding both public health and the environment.
Implement Safe Handling and Disposal Practices for Biomedical Waste
To ensure the safe handling and disposal of biomedical waste, healthcare facilities must adopt several best practices:
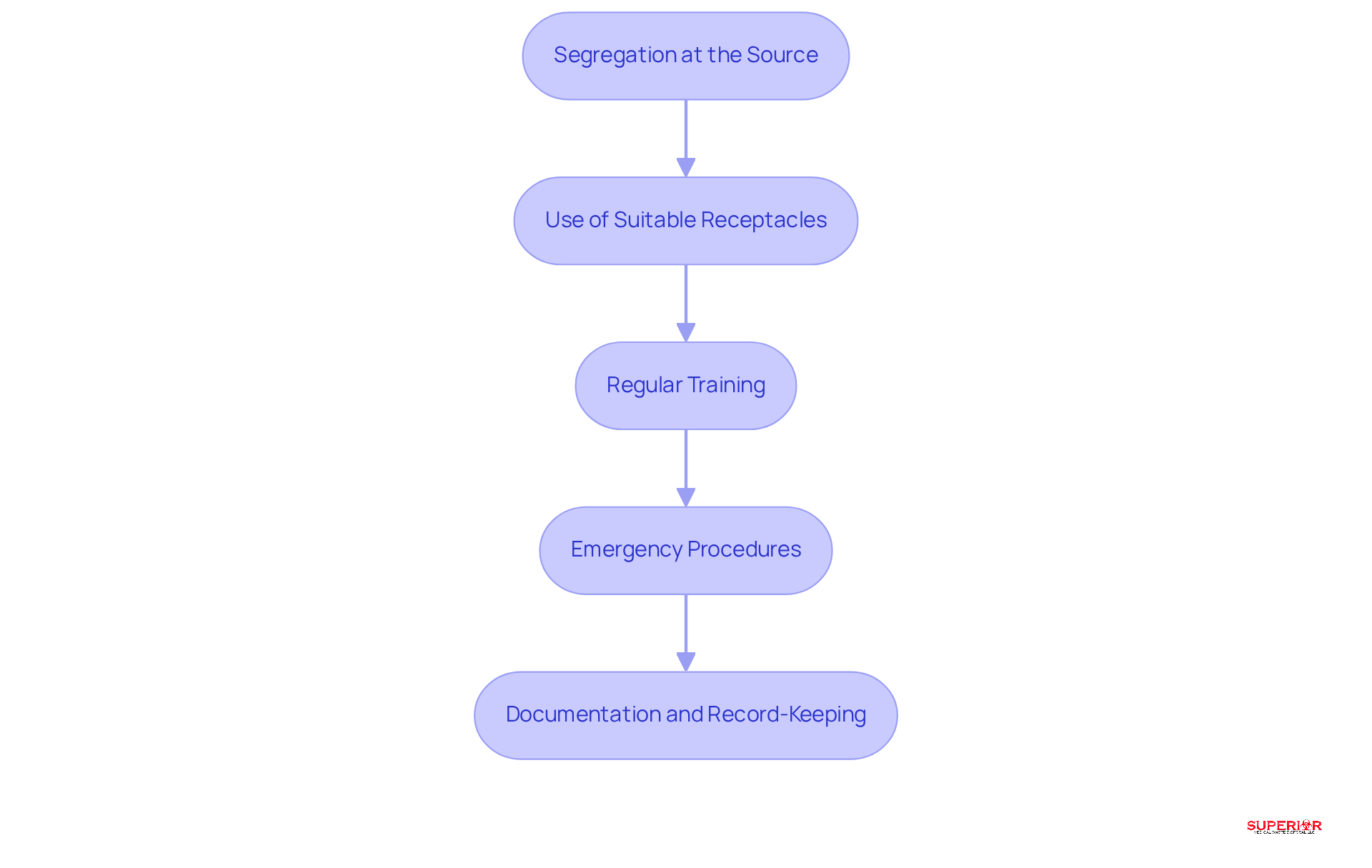
- Segregation at the Source: Waste should be separated at the point of generation to prevent contamination. Implementing color-coded bins for various types of refuse – red for infectious materials and yellow for sharps – facilitates proper disposal and minimizes risks associated with cross-contamination.
- Use of Suitable Receptacles: All medical refuse must be placed in leak-proof, clearly marked with the biohazard symbol. This includes specialized sharps containers for needles and other sharp objects, essential for preventing injuries and ensuring compliance with safety regulations.
- Regular Training: Ongoing training for staff on safe handling practices is crucial. This training should address the correct disposal of different kinds of medical refuse and be revised frequently to incorporate updates in regulations and best methods, ensuring that all staff are well-informed and compliant.
- Emergency Procedures: Facilities must establish clear protocols for addressing spills or accidents involving biomedical materials. This includes having spill kits readily available and ensuring staff are trained in their use, which is vital for maintaining safety and compliance during unexpected incidents.
- Documentation and Record-Keeping: Accurate records of refuse disposal are essential. Facilities should maintain detailed documentation of the type and quantity of refuse generated, treatment methods used, and disposal locations. This documentation is critical for compliance with regulatory requirements and for facilitating audits.
By adopting these practices, healthcare organizations can significantly reduce the risks linked to medical refuse handling, ensuring a safer environment for both personnel and patients.
Train Staff on Best Practices for Biomedical Waste Management
Training is essential for the effective in healthcare settings. To ensure that staff are adequately prepared, the following strategies should be implemented:
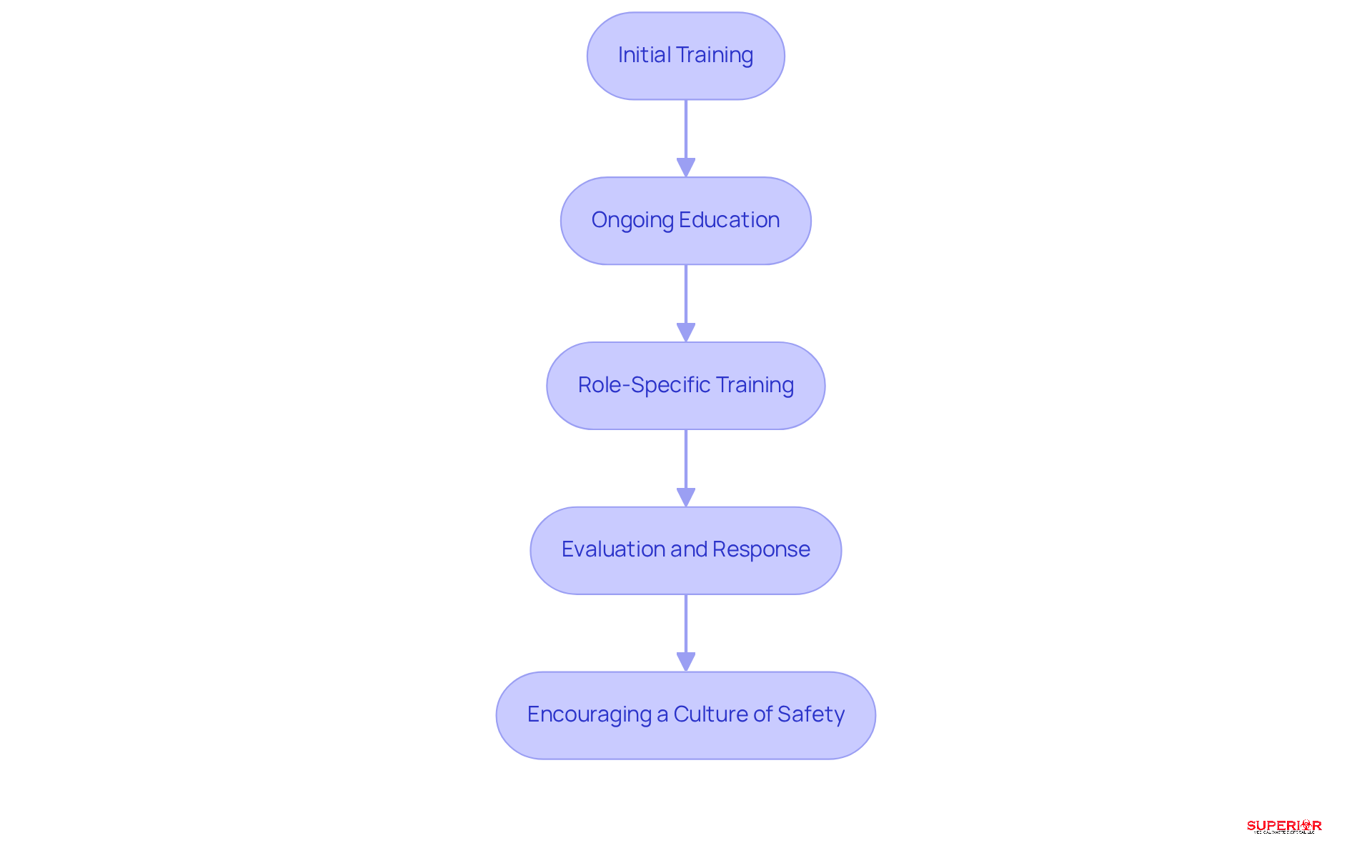
- Initial Training: Comprehensive instruction on biomedical refuse handling must be integrated into the onboarding process for all new employees. This training should encompass the various types of refuse, proper handling procedures, and pertinent regulatory requirements.
- Ongoing Education: Regular refresher courses are vital for keeping staff updated on the latest regulations and best practices. These can take the form of workshops, online courses, or in-person training sessions, facilitating continuous learning.
- Role-Specific Training: Training programs should be customized to the specific roles of staff members. For instance, clinical staff may require distinct training related to their disposal responsibilities compared to administrative personnel.
- Evaluation and Response: Conducting evaluations to assess personnel understanding of disposal practices is crucial. Providing constructive feedback and additional training as necessary addresses any knowledge gaps and reinforces learning.
- Encouraging a Culture of Safety: Fostering an environment where employees feel comfortable reporting concerns or asking questions about refuse handling is essential. This proactive approach can help identify potential issues before they escalate, thereby enhancing overall safety.
By prioritizing these training strategies, healthcare facilities can significantly enhance their waste management practices and ensure compliance with regulatory standards.
Conclusion
Effective biomedical waste disposal is essential for ensuring a safe and healthy environment within healthcare facilities. Understanding the various types of biomedical waste and implementing best practices for disposal allows healthcare organizations to significantly reduce the risks associated with improper waste management. Adhering to regulatory requirements and providing comprehensive staff training are critical components in ensuring compliance and protecting public health.
Key points highlighted throughout the article include:
- The identification of different categories of biomedical waste
- The necessity of understanding regulatory frameworks from OSHA, EPA, and local health departments
- The implementation of safe handling practices
Continuous staff training and education are emphasized to reinforce the importance of a knowledgeable workforce in managing biomedical waste effectively. By prioritizing these strategies, healthcare facilities can establish a robust waste management system that not only complies with regulations but also promotes safety and environmental responsibility.
In conclusion, managing biomedical waste transcends mere regulatory obligation; it is a fundamental aspect of healthcare practice that directly influences community health and safety. By adopting best practices for waste disposal and ensuring staff are well-trained, healthcare facilities contribute to a cleaner, safer environment. It is imperative for all healthcare organizations to take proactive steps in enhancing their waste management strategies, thereby safeguarding both their personnel and the communities they serve.
Frequently Asked Questions
What are the main types of biomedical waste generated in healthcare facilities?
The main types of biomedical waste include infectious waste, sharps, pathological waste, pharmaceutical waste, and chemical waste.
What is considered infectious waste?
Infectious waste includes materials contaminated with blood, bodily fluids, or other potentially infectious materials, such as used gloves, dressings, and surgical instruments.
What are sharps in the context of biomedical waste?
Sharps are items that can puncture or cut skin, such as needles, scalpels, and broken glass, which require disposal in puncture-resistant containers to ensure safety.
What constitutes pathological waste?
Pathological waste includes human tissues, organs, and body parts that necessitate special handling and disposal due to their potential health risks.
How should pharmaceutical waste be managed?
Pharmaceutical waste, including expired or unused medications and hazardous drugs, must be disposed of according to specific regulations to prevent environmental contamination and protect public health.
What is classified as chemical waste in healthcare facilities?
Chemical waste encompasses hazardous chemicals used in healthcare settings, such as solvents and disinfectants, which require careful oversight to avoid exposure risks.
Why is the identification of biomedical waste types important?
Precise identification of biomedical waste types allows healthcare centers to implement customized disposal strategies that comply with local and federal regulations, essential for safeguarding public health and the environment.
