Introduction
Healthcare facilities play a crucial role in public health, yet they encounter significant challenges in managing the various types of medical waste they produce. Effective waste disposal is vital not only for meeting stringent regulatory requirements but also for protecting the health of patients, staff, and the environment.
As hospitals grapple with the complexities of waste management, a pressing question emerges: how can they adopt best practices that ensure safety and regulatory compliance while also minimizing environmental impact?
This article explores essential strategies for waste disposal in hospitals, providing insights that can transform compliance into a proactive framework for health and safety.
Identify Types of Medical Waste in Healthcare Facilities
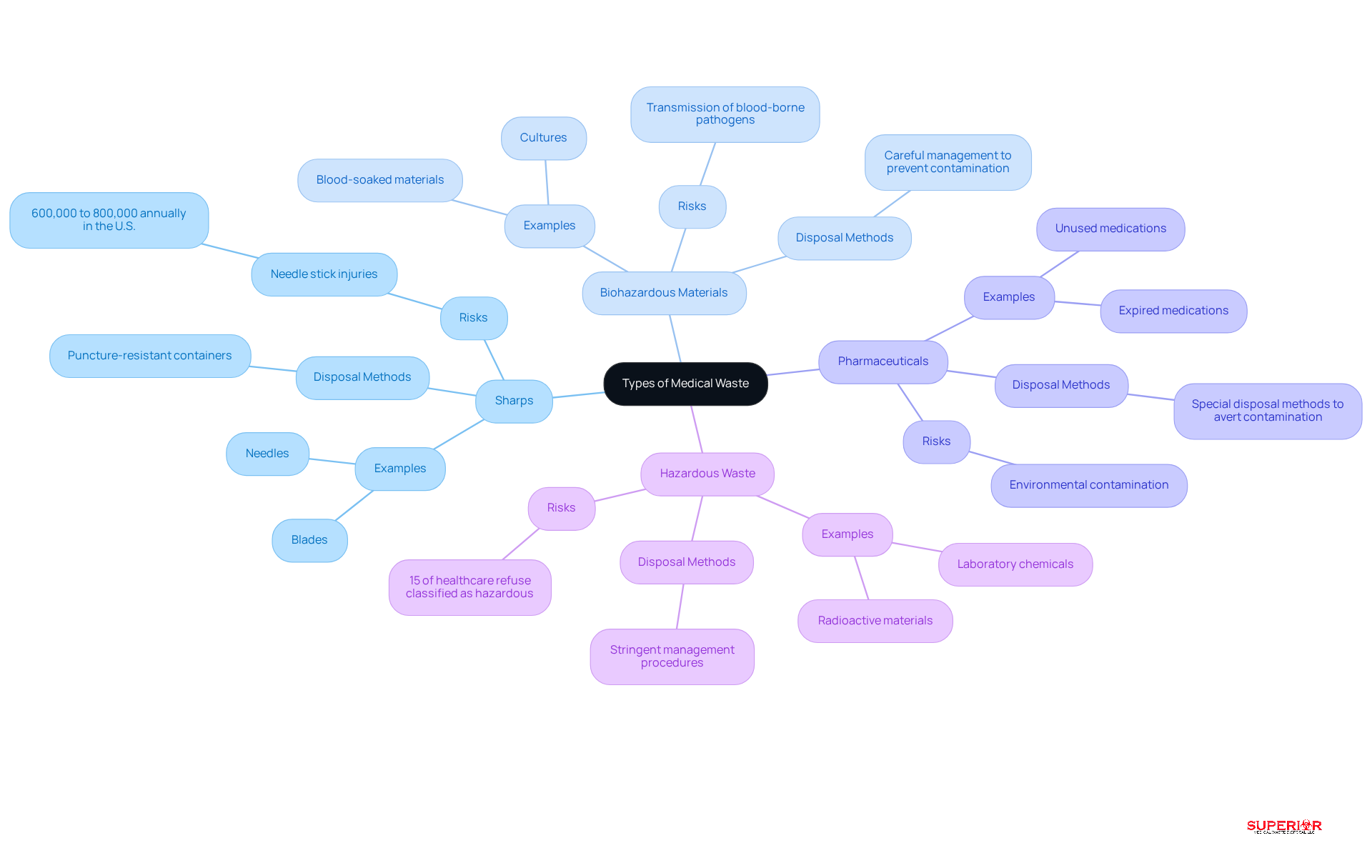
Healthcare facilities generate various types of , which can be categorized into four main types: sharps, , pharmaceuticals, and hazardous materials.
- Sharps: This category encompasses needles, blades, and other sharp objects that present a risk of injury. is essential to prevent accidents and minimize the occurrence of needle stick injuries, which range from 600,000 to 800,000 annually in the U.S.
- : Waste that may harbor , such as blood-soaked materials and cultures, must be managed carefully to prevent contamination. The World Health Organization highlights that inadequately managed waste can lead to long-term , including the transmission of blood-borne pathogens.
- Pharmaceuticals: necessitate special disposal methods to avert environmental contamination. Improper handling of pharmaceuticals can lead to their presence in groundwater and soil, posing risks to both human health and ecosystems.
- : This category includes chemicals and materials that pose a threat to health or the environment, such as certain laboratory chemicals and radioactive materials. Approximately 15% of healthcare refuse is classified as hazardous, necessitating stringent management procedures to mitigate risks.
By accurately identifying and classifying these refuse categories, healthcare establishments can implement appropriate disposal techniques, ensuring compliance with evolving state and federal regulations while enhancing overall safety.
Implement Effective Waste Segregation Strategies
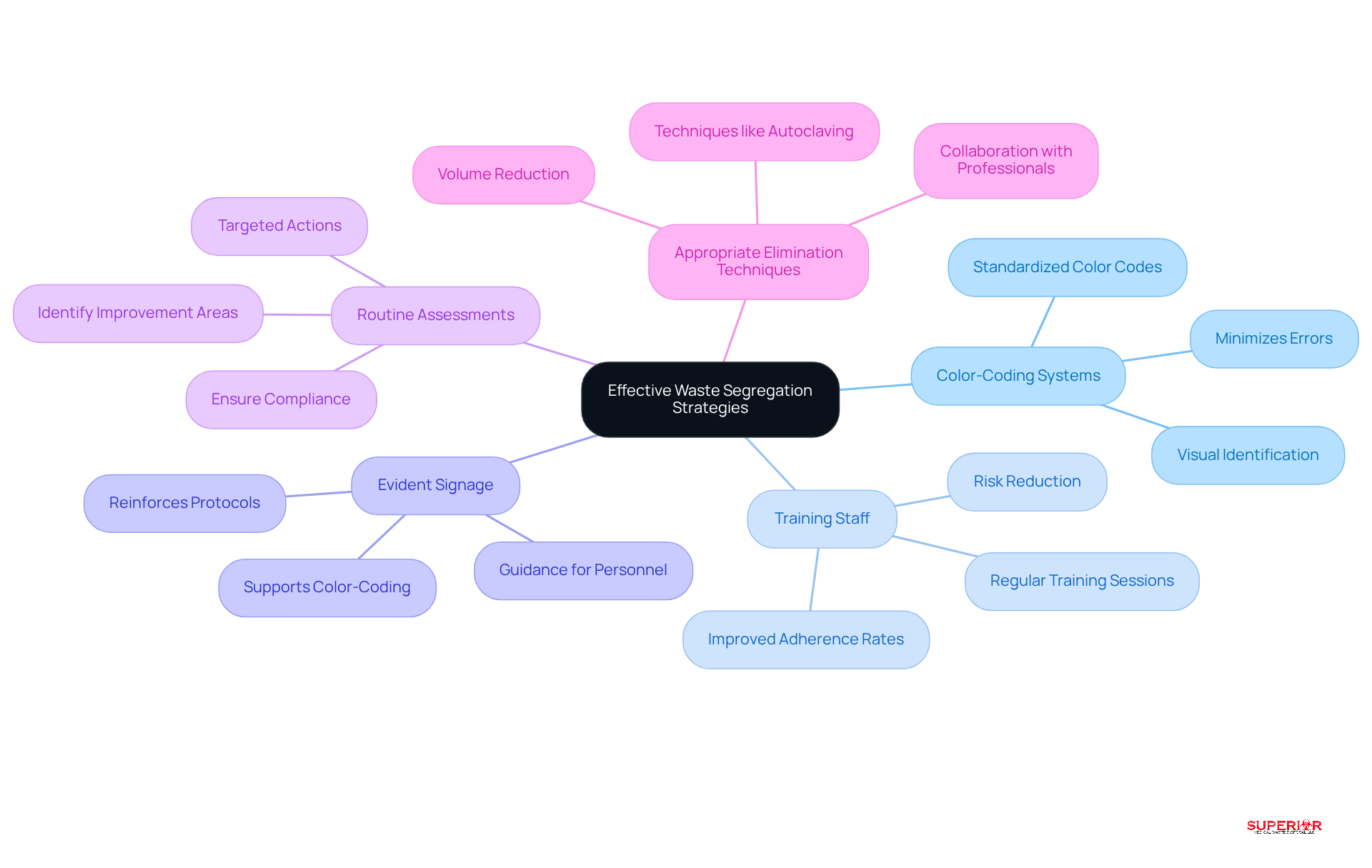
To ensure safe and compliant refuse disposal, healthcare establishments must implement effective segregation strategies. The following key practices are essential:
- Color-Coding Systems: A standardized – such as red for and yellow for sharps – facilitates easy identification and minimizes errors. This practice is crucial; research indicates that over 60% of healthcare establishments lack adequate segregation systems, underscoring the need for clear visual indicators.
- Training Staff: on and the importance of adherence, particularly in assisted living facilities. Successful training initiatives have shown significant improvements in segregation adherence rates, thereby reducing the risk of contamination and ensuring compliance with safety protocols.
- Evident Signage: Positioning clear signage near refuse collection zones guides personnel on the appropriate methods for different types of refuse. This visual reinforcement supports the color-coding system and helps maintain adherence to established protocols.
- Routine Assessments: Conducting allows facilities to identify areas for improvement and ensure compliance with . These audits can reveal inconsistencies in disposal management practices, enabling targeted actions to enhance compliance.
- : Collaborating with professional medical refuse management services, such as those offered by , ensures compliant handling, storage, and treatment of . Techniques like autoclaving and shredding can reduce refuse volume by 70%.
By implementing these strategies, healthcare institutions can significantly enhance their management processes, mitigate risks associated with improper handling, and comply with regulatory standards.
Evaluate Disposal Methods: Incineration vs. Autoclaving
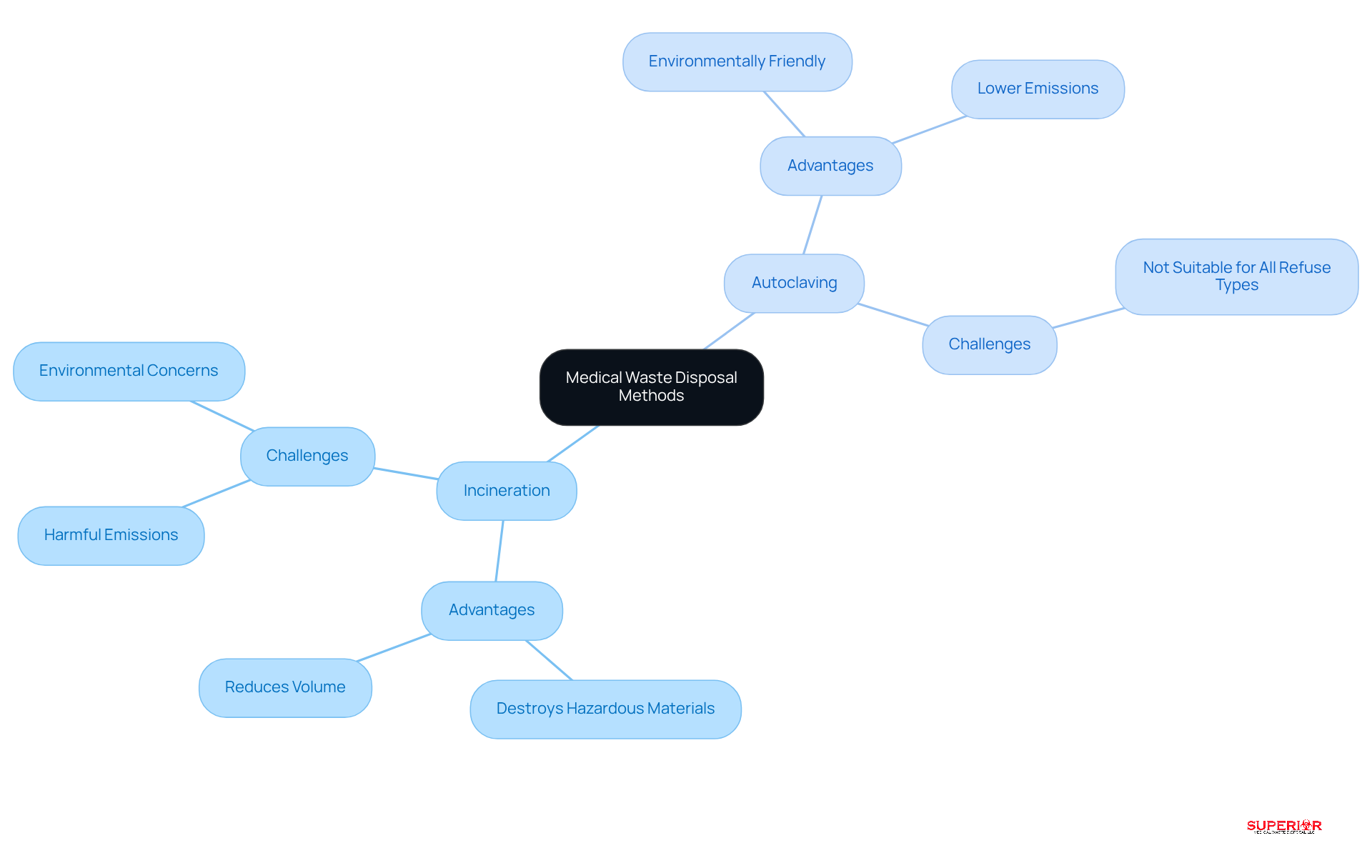
Healthcare facilities in Traverse City face a critical decision regarding : . Each method offers distinct advantages and challenges that must be carefully considered.
Incineration is a high-temperature treatment method that effectively destroys hazardous materials, significantly reducing their volume and eliminating pathogens. However, it is associated with harmful emissions, including dioxins and heavy metals, which can negatively impact air quality and public health. In the United States, over 70% of medical refuse is incinerated, raising concerns about its environmental effects. Notably, incineration generates approximately 3 kg of CO2 for every kg of clinical refuse burned. Healthcare institutions such as Munson and Byers Heather contribute significantly to the medical refuse produced in Traverse City, necessitating a thorough evaluation of .
Autoclaving, on the other hand, utilizes steam under pressure to sterilize medical refuse, making it safe for disposal in regular landfills. This method is generally regarded as more , as it produces significantly lower emissions and avoids combustion. Operating at temperatures between 250-270°F, autoclaving efficiently removes pathogens while minimizing the carbon footprint associated with disposal treatment. However, it may not be suitable for all types of refuse, particularly highly hazardous materials that require complete destruction.
To ensure compliance, all facilities generating medical refuse must obtain a , which is mandatory for any amount of medical refuse and must be renewed every three years. Facilities should conduct comprehensive assessments of their refuse streams to select the disposal method that aligns with their regulatory obligations and environmental goals. Regular evaluations of the effectiveness of the chosen approach are also essential to ensure ongoing . is dedicated to providing comprehensive medical refuse management solutions tailored to the needs of local healthcare establishments.
Understand Regulatory Compliance Requirements for Medical Waste
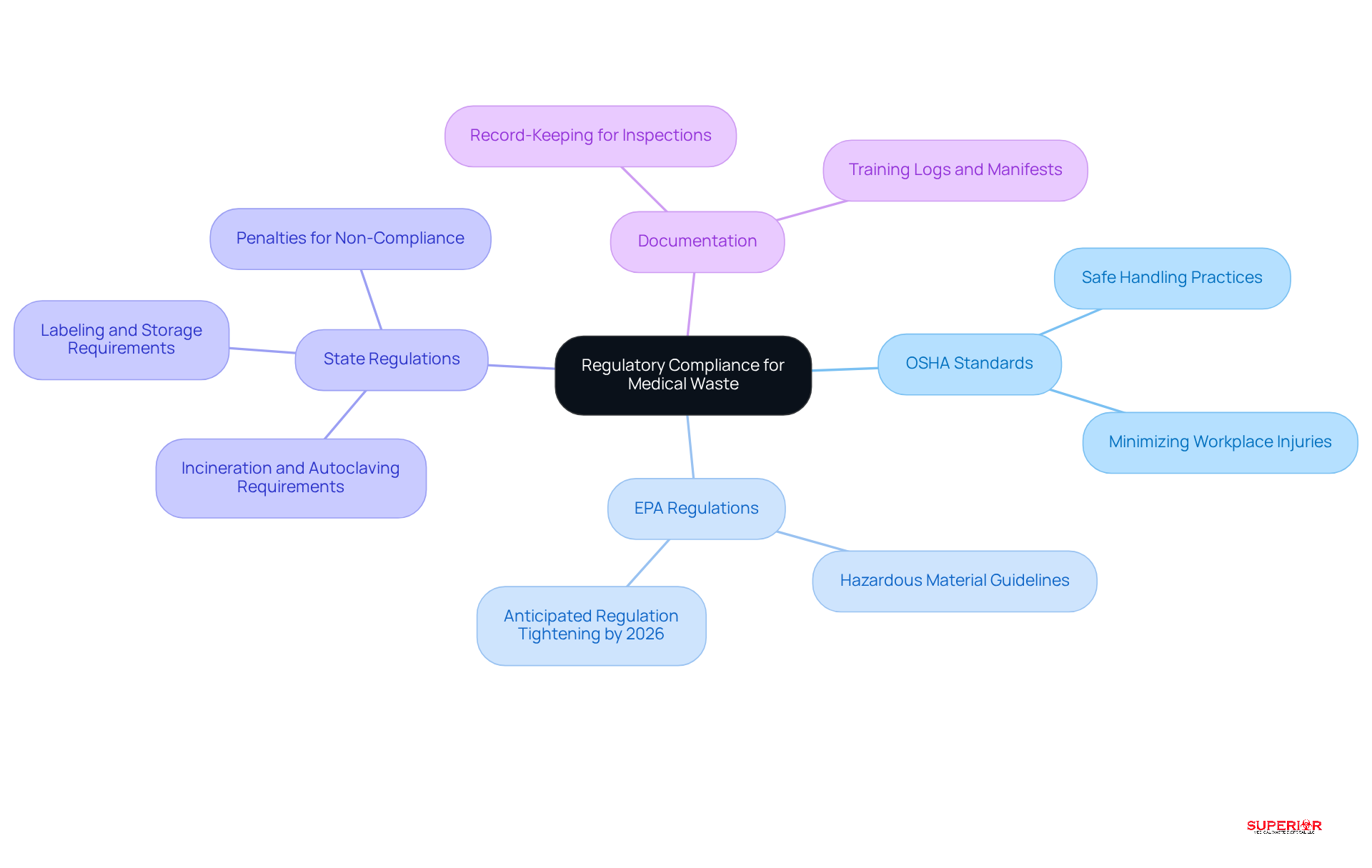
must navigate a complex landscape of obligations concerning waste disposal and medical . Understanding these regulations is essential for ensuring safe and compliant practices in s.
: The Occupational Safety and Health Administration (OSHA) mandates safe handling and disposal practices to protect healthcare workers from hazardous materials. Adhering to is vital for minimizing workplace injuries and safeguarding the well-being of staff at the .
: The Environmental Protection Agency (EPA) regulates the disposal of hazardous materials, requiring healthcare facilities to follow specific guidelines for treatment and disposal. With anticipated by 2026, it is imperative for to bolster their regarding practices.
: Each state enforces additional regulations governing medical , which can differ significantly. For example, some states mandate incineration or autoclaving of infectious waste, while others impose specific labeling and storage requirements. Staying informed about local laws is crucial for compliance and avoiding penalties, which can amount to $25,000 per day for violations.
Documentation: Accurate record-keeping is essential for demonstrating compliance during inspections. Facilities must maintain comprehensive records of , including manifests and training logs. This documentation not only supports regulatory adherence but also enhances operational transparency and accountability.
By thoroughly understanding and adhering to these guidelines, can mitigate risks associated with improper handling of practices and ensure safe, compliant management.
Provide Ongoing Training for Waste Management Staff
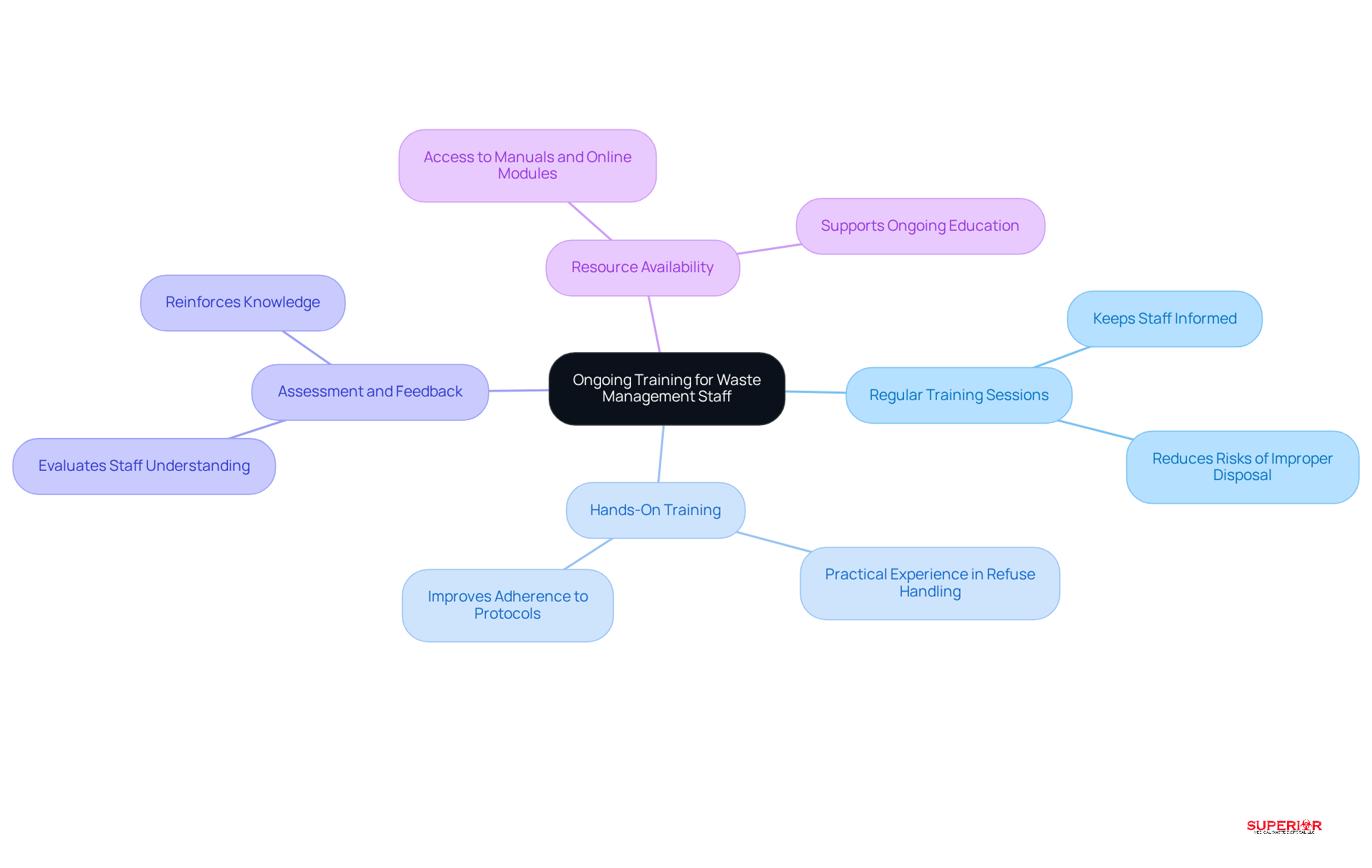
for staff at the is crucial for ensuring compliance and safety in healthcare facilities. This training not only enhances understanding but also . Here are :
- : Consistent training sessions should be scheduled to keep staff informed about the latest regulations, disposal methods, and safety protocols. This approach strengthens understanding and reduces risks linked to improper disposal.
- : Practical, is essential for staff to practice proper refuse handling and segregation techniques in a controlled environment. Case studies have shown that such training significantly improves staff understanding and adherence to disposal protocols, leading to fewer errors and enhanced safety.
- : Implementing assessments to evaluate staff understanding and providing constructive feedback is vital. Frequent assessments reinforce knowledge and ensure personnel are confident in their disposal management practices, fostering a culture of safety.
- Resource Availability: It is important to ensure that staff have access to , such as manuals and , to support their ongoing education. Providing these tools empowers staff to remain informed and compliant with evolving regulations.
By investing in , healthcare facilities can improve their practices related to , enhance staff retention, and maintain a robust culture of safety and compliance.
Conclusion
Implementing effective waste disposal practices in hospitals is crucial for ensuring compliance and safeguarding public health. By accurately identifying and categorizing medical waste, healthcare facilities can adopt disposal methods that meet regulatory standards. The focus on proper waste segregation, staff training, and understanding disposal techniques such as incineration and autoclaving underscores the comprehensive approach necessary for responsible medical waste management.
Key insights highlight the importance of a systematic strategy in waste management. Identifying waste types – sharps, biohazardous materials, pharmaceuticals, and hazardous waste – establishes a foundation for effective segregation practices. Additionally, the comparison of incineration and autoclaving illustrates the need for facilities to critically assess their disposal methods, weighing environmental impact against compliance with evolving regulations. Regular training and continuous education for staff are essential components in upholding high standards of safety and compliance.
Ultimately, the importance of adhering to waste management best practices cannot be overstated. As healthcare facilities navigate the complexities of regulatory compliance, prioritizing effective waste disposal strategies not only protects public health but also enhances operational efficiency. Engaging with these practices cultivates a culture of safety and responsibility, ensuring that healthcare environments remain safe for both patients and staff while positively contributing to the broader community and environment.
Frequently Asked Questions
What are the main types of medical waste generated in healthcare facilities?
The main types of medical waste are sharps, biohazardous materials, pharmaceuticals, and hazardous materials.
What are sharps, and why is their disposal important?
Sharps include needles, blades, and other sharp objects that pose a risk of injury. Proper disposal in puncture-resistant containers is essential to prevent accidents and minimize needle stick injuries, which occur between 600,000 to 800,000 times annually in the U.S.
What constitutes biohazardous materials, and what risks do they pose?
Biohazardous materials are waste that may harbor infectious agents, such as blood-soaked materials and cultures. Inadequately managed biohazardous waste can lead to long-term public health risks, including the transmission of blood-borne pathogens.
How should pharmaceuticals be disposed of?
Expired or unused medications require special disposal methods to prevent environmental contamination, as improper handling can result in pharmaceuticals entering groundwater and soil, posing risks to human health and ecosystems.
What is classified as hazardous waste in healthcare?
Hazardous waste includes chemicals and materials that pose a threat to health or the environment, such as certain laboratory chemicals and radioactive materials. Approximately 15% of healthcare refuse is classified as hazardous, requiring stringent management procedures.
What are effective strategies for waste segregation in healthcare facilities?
Effective strategies include implementing a color-coding system for disposal containers, training staff on proper segregation techniques, using evident signage near collection zones, conducting routine assessments of refuse management practices, and collaborating with professional medical refuse management services.
Why is a color-coding system important in waste segregation?
A color-coding system helps facilitate easy identification of disposal containers, minimizing errors and ensuring compliance. Research indicates that over 60% of healthcare establishments lack adequate segregation systems, highlighting the need for clear visual indicators.
How can staff training improve waste segregation practices?
Regular training sessions educate staff on proper segregation techniques and the importance of adherence, particularly in assisted living facilities. Successful training initiatives have shown significant improvements in segregation adherence rates, reducing the risk of contamination.
What role does signage play in waste management?
Clear signage near refuse collection zones guides personnel on appropriate disposal methods for different types of refuse, supporting the color-coding system and helping maintain adherence to established protocols.
How can healthcare facilities assess their waste management practices?
Conducting routine assessments allows facilities to identify areas for improvement and ensure compliance with segregation protocols. These audits can reveal inconsistencies in disposal management practices, enabling targeted actions to enhance compliance.
List of Sources
- Identify Types of Medical Waste in Healthcare Facilities
- Healthcare Waste—A Serious Problem for Global Health – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9858835)
- Medical waste management in the modern healthcare era: A comprehensive review of technologies, environmental impact, and sustainable practices (https://sciencedirect.com/science/article/pii/S2590123025032657)
- Medical Waste 101: Discussing the Types and the Categories (https://danielshealth.com/knowledge-center/types-of-medical-waste)
- How Much Medical Waste is Produced? | Medical Waste Pros (https://medicalwastepros.com/blog/how-much-medical-waste-is-produced)
- Health-care waste (https://who.int/news-room/fact-sheets/detail/health-care-waste)
- Implement Effective Waste Segregation Strategies
- New Normal – Hospital Waste Management | Daniels Health (https://danielshealth.com/new-normal-hospital-waste-management)
- Assessment of Medical Waste Segregation, Disposal Practices for Infectious and Sharps Waste in Healthcare Facilities in Somalia: Implications for Infection Prevention and Control – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12301244)
- Hospital Waste Disposal in 2026: Complete Compliance Guide for Healthcare Facilities (https://medprodisposal.com/hospital-waste-disposal-2026-compliance-guide)
- remedi Announces 2026 Landfill Diversion Target as Demand for Medical Waste Recycling Accelerates (https://prnewswire.com/news-releases/remedi-announces-2026-landfill-diversion-target-as-demand-for-medical-waste-recycling-accelerates-302670816.html)
- Healthcare Management Resolutions To Make Healthcare Safer (https://securewaste.net/healthcare-waste-management-resolutions-to-make-healthcare-safer-in-2026)
- Evaluate Disposal Methods: Incineration vs. Autoclaving
- A Review on Medical Waste Management: Treatment, Recycling, and Disposal Options (https://mdpi.com/2076-3298/9/11/146)
- Autoclave vs incineration: which is best for medical waste disposal? (https://celitron.com/en/blog/autoclave-vs-incineration-which-one-is-the-best-method-for-the-disposal-of-medical-waste)
- Medical waste management in the modern healthcare era: A comprehensive review of technologies, environmental impact, and sustainable practices (https://sciencedirect.com/science/article/pii/S2590123025032657)
- Environmental Impact: Incineration vs. Autoclaving | All Points Med Waste (https://allpointsmedicalwaste.com/comparing-the-environmental-impact-of-incineration-vs-autoclaving)
- Understand Regulatory Compliance Requirements for Medical Waste
- The Future of Waste Management in Hospitals: Trends to Watch (https://danielshealth.com/knowledge-center/future-of-waste-management)
- Commonly Used Statistics | Occupational Safety and Health Administration (https://osha.gov/data/commonstats)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- Hospital Waste Disposal in 2026: Complete Compliance Guide for Healthcare Facilities (https://medprodisposal.com/hospital-waste-disposal-2026-compliance-guide)
- stericycle.com (https://stericycle.com/en-us/about-us/our-stories/annual-safety-trend-report-unveiling-healthcare-challenges-medical-waste-insights)
- Provide Ongoing Training for Waste Management Staff
- Healthcare Management Resolutions To Make Healthcare Safer (https://securewaste.net/healthcare-waste-management-resolutions-to-make-healthcare-safer-in-2026)
- Hospital Waste Disposal in 2026: Complete Compliance Guide for Healthcare Facilities (https://medprodisposal.com/hospital-waste-disposal-2026-compliance-guide)
- Medical Waste Management Program (https://cdph.ca.gov/Programs/CEH/DRSEM/Pages/EMB/MedicalWaste/MedicalWaste.aspx)
- wastemedic.com (https://wastemedic.com/2026/01/08/medical-waste-segregation-refresher-starting-the-year-the-right-way)
