Introduction
In the complex realm of healthcare, the secure disposal of medical records is not just a best practice; it is a critical obligation shaped by stringent regulatory requirements. Healthcare facilities must navigate the complexities of HIPAA and state-specific laws, ensuring that sensitive patient information is rendered irretrievable and unreadable. This article explores essential strategies for compliant medical record disposal, emphasizing the benefits of secure destruction methods and the importance of selecting reliable partners.
How can healthcare organizations effectively safeguard patient data while adapting to evolving regulations and best practices?
Understand Regulatory Requirements for Medical Record Disposal
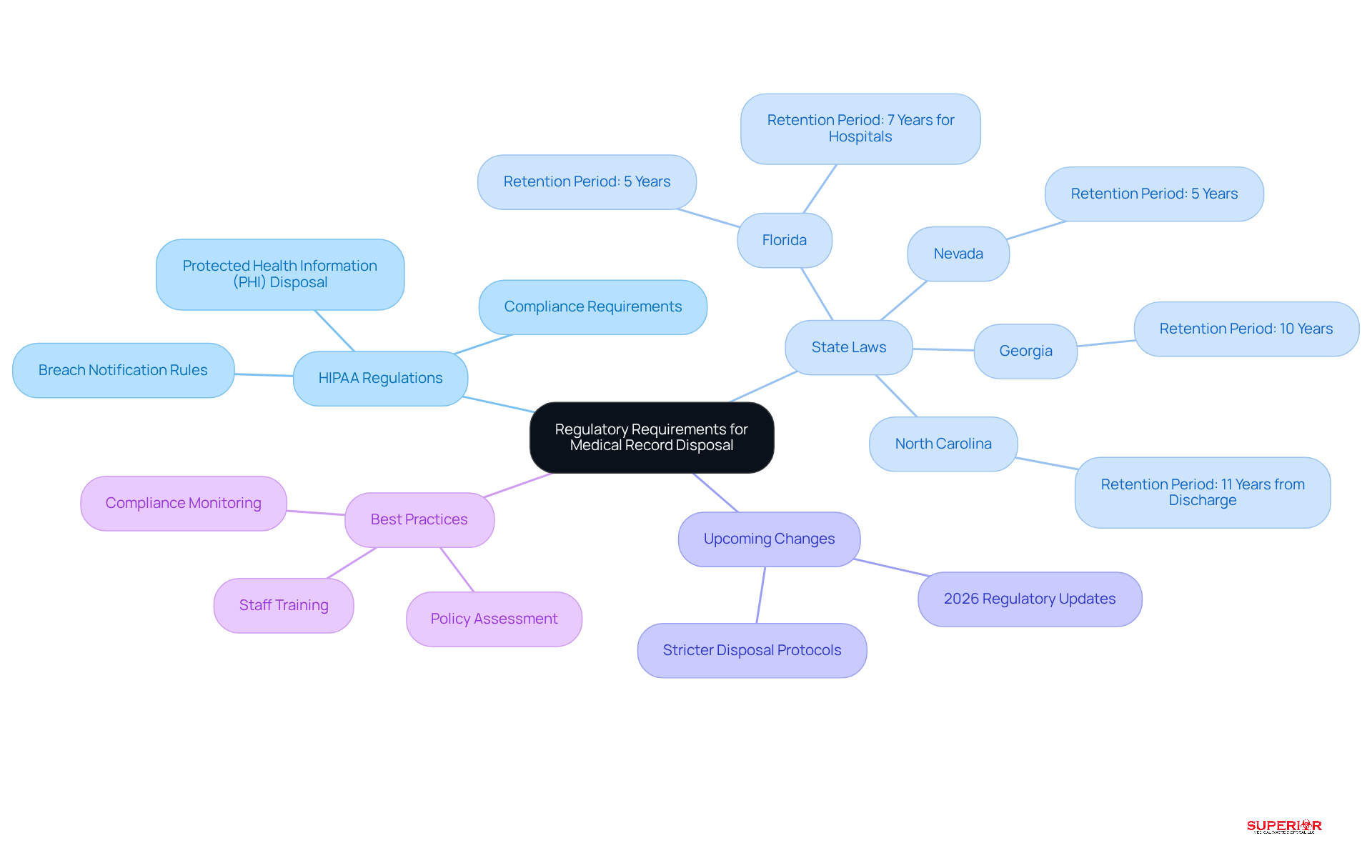
face a complex regulatory landscape regarding the . The Health Insurance Portability and Accountability Act (HIPAA) mandates that the , including , must ensure that it is rendered unreadable and irretrievable. Additionally, state laws may impose even . For instance:
- In Florida, for at least five years following the last patient contact.
- In North Carolina, there is an eleven-year retention period from discharge.
Starting in 2026, with that could introduce more stringent protocols for the .
It is essential for these establishments to consistently assess and revise their policies to align with evolving regulations. This practice not only ensures compliance but also . Furthermore, training staff on these requirements is vital to foster a culture of compliance within the organization. Facilities that proactively adapt their policies not only protect sensitive information but also enhance their operational integrity.
Implement Secure Destruction Methods for Compliance
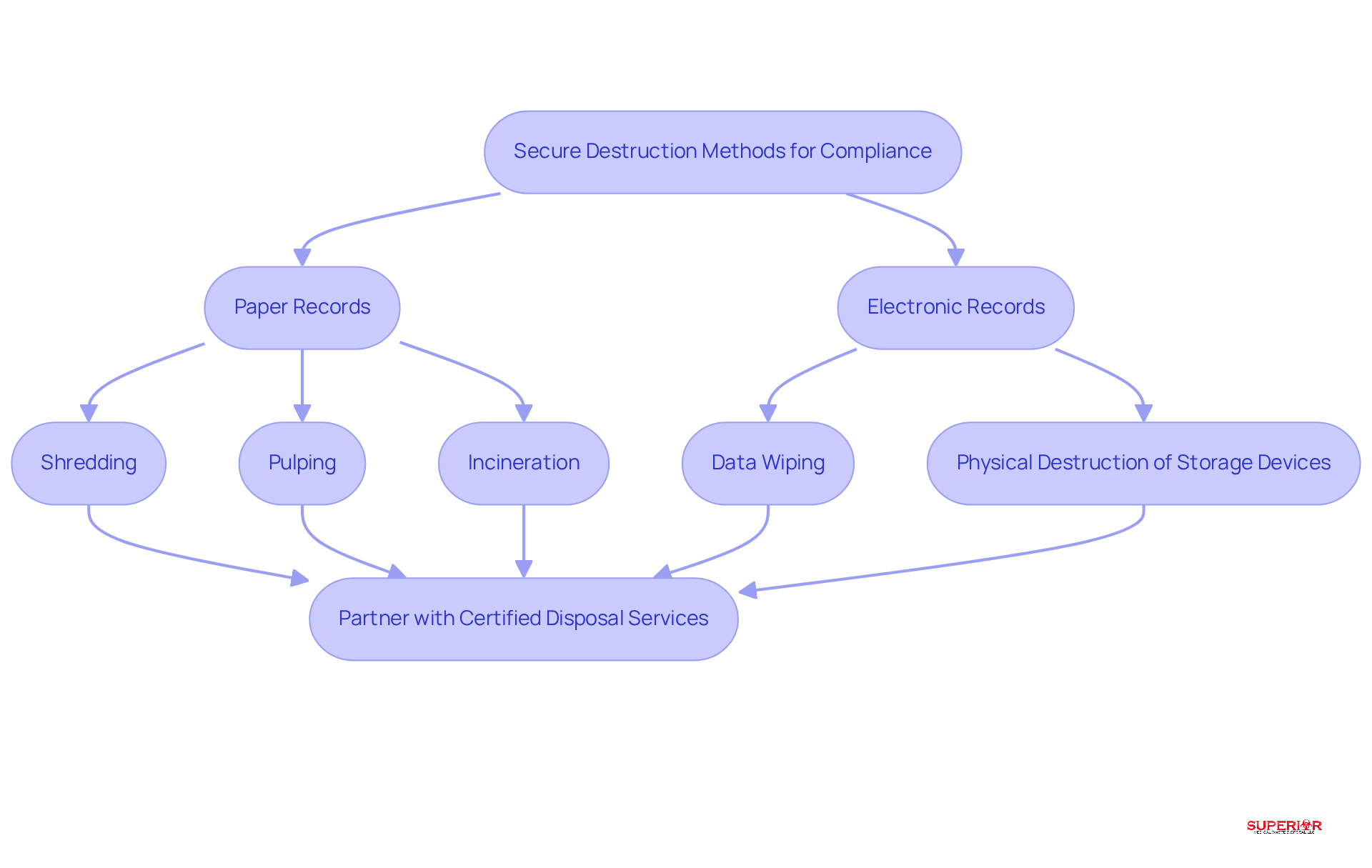
To comply with HIPAA and other regulations, healthcare facilities must implement . The most efficient methods include:
- Shredding
- Pulping
- Incineration for paper records
For electronic records, data wiping or the physical destruction of storage devices is essential. Investing in that produce confetti-sized particles is crucial, as this makes reconstruction virtually impossible.
Moreover, partnering with , such as those provided by , enhances security. These vendors are particularly skilled in managing sensitive information effectively. Utilizing not only ensures compliance but also saves time and reduces costs compared to in-house shredding.
It is vital to maintain comprehensive records of the disposal of medical records, including certificates of disposal, since from their creation or last effective date. As regulations tighten in 2026, . Therefore, it is essential for healthcare organizations to stay ahead of best practices.
Select Appropriate Disposal Methods and Partners
Selecting appropriate methods and partners for the is essential for healthcare facilities to ensure compliance and safeguard sensitive patient information. It is crucial to confirm that potential vendors for the adhere to and possess proven expertise in , commonly known as paper shredding. Key criteria for include in managing medical records, especially in relation to the containing individually identifiable health information such as patient medical records, social security numbers, and other sensitive identifiers like birth dates, geographic identifiers, and account numbers.
Conducting site visits allows organizations to assess the vendor’s operational security measures firsthand. Establishing a that clearly outlines responsibilities, regulatory obligations, and liability is vital for protecting the facility’s interests, particularly regarding the . Regular performance reviews of the partnership can help maintain high standards of security and compliance, particularly regarding the , ensuring that the vendor continues to meet the evolving needs of the healthcare environment. By 2026, organizations are increasingly prioritizing shredding providers that demonstrate a commitment to sustainability, with expectations that 100% of shredded paper will be recycled. This trend underscores the importance of aligning the with broader while maintaining strict data protection standards.
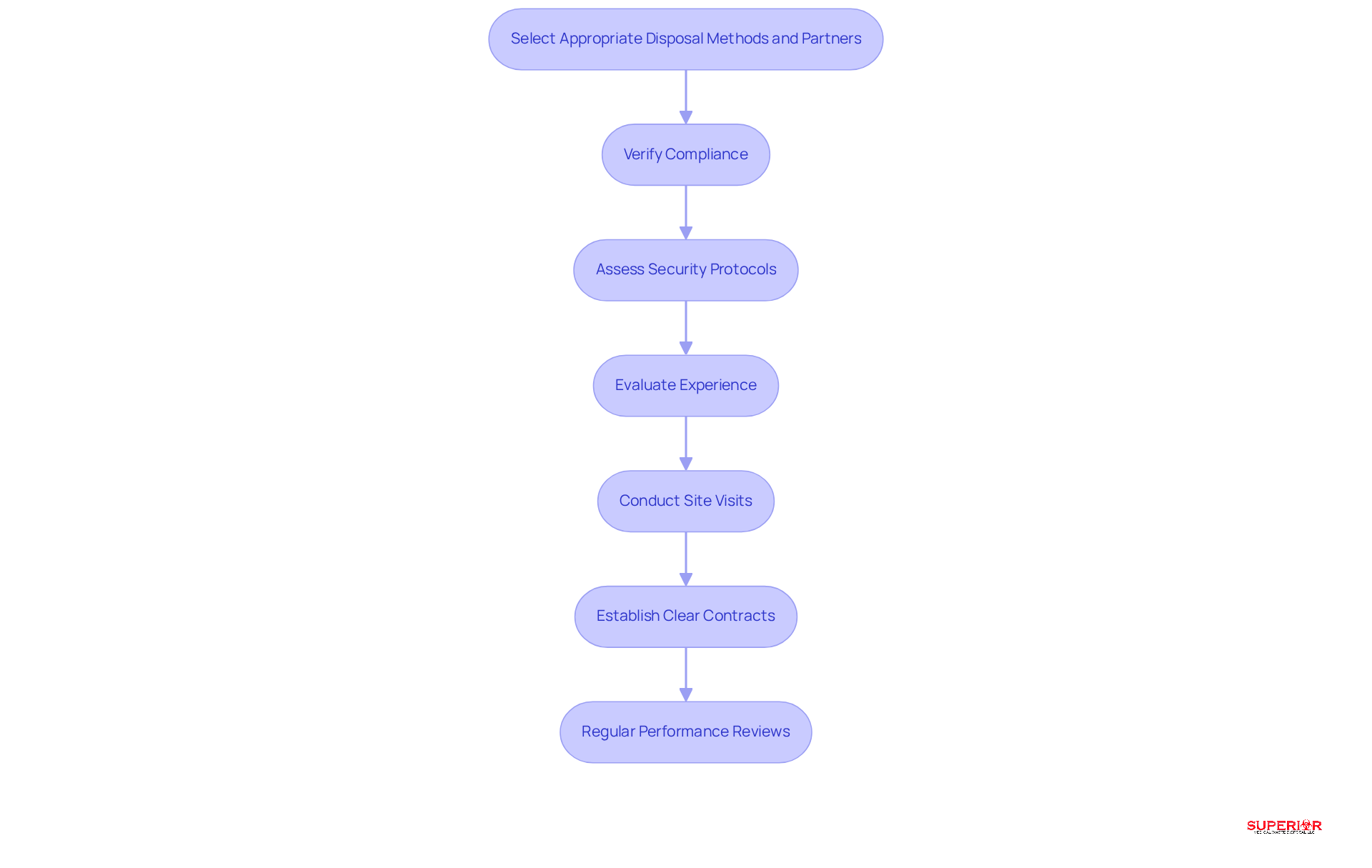
To enhance the selection process, healthcare facilities should consider the following steps:
- Verify Compliance: Ensure the vendor is HIPAA-compliant and holds relevant certifications.
- Assess Security Protocols: Review the vendor’s security measures and protocols for handling sensitive information, including the .
- Evaluate Experience: Seek vendors with extensive experience in the and .
- Conduct Site Visits: Visit the vendor’s facilities to observe their operations and security practices concerning the .
- Establish Clear Contracts: Create contracts that outline responsibilities, adherence requirements, and liability related to the .
- Regular Performance Reviews: Schedule regular reviews to ensure ongoing compliance and security standards regarding the .
Incorporating insights from industry leaders can further guide the selection process. For instance, Kent Cañas, a content strategist, emphasizes that “HIPAA violations often result from poor data security policies and procedures,” highlighting the critical need for . Additionally, successful partnerships between healthcare facilities and certified shredding providers exemplify best practices in the , reinforcing the importance of selecting reliable partners. Furthermore, it is noteworthy that stemmed from lost devices, underscoring the necessity of practices for the .
Conduct Regular Audits and Staff Training for Compliance
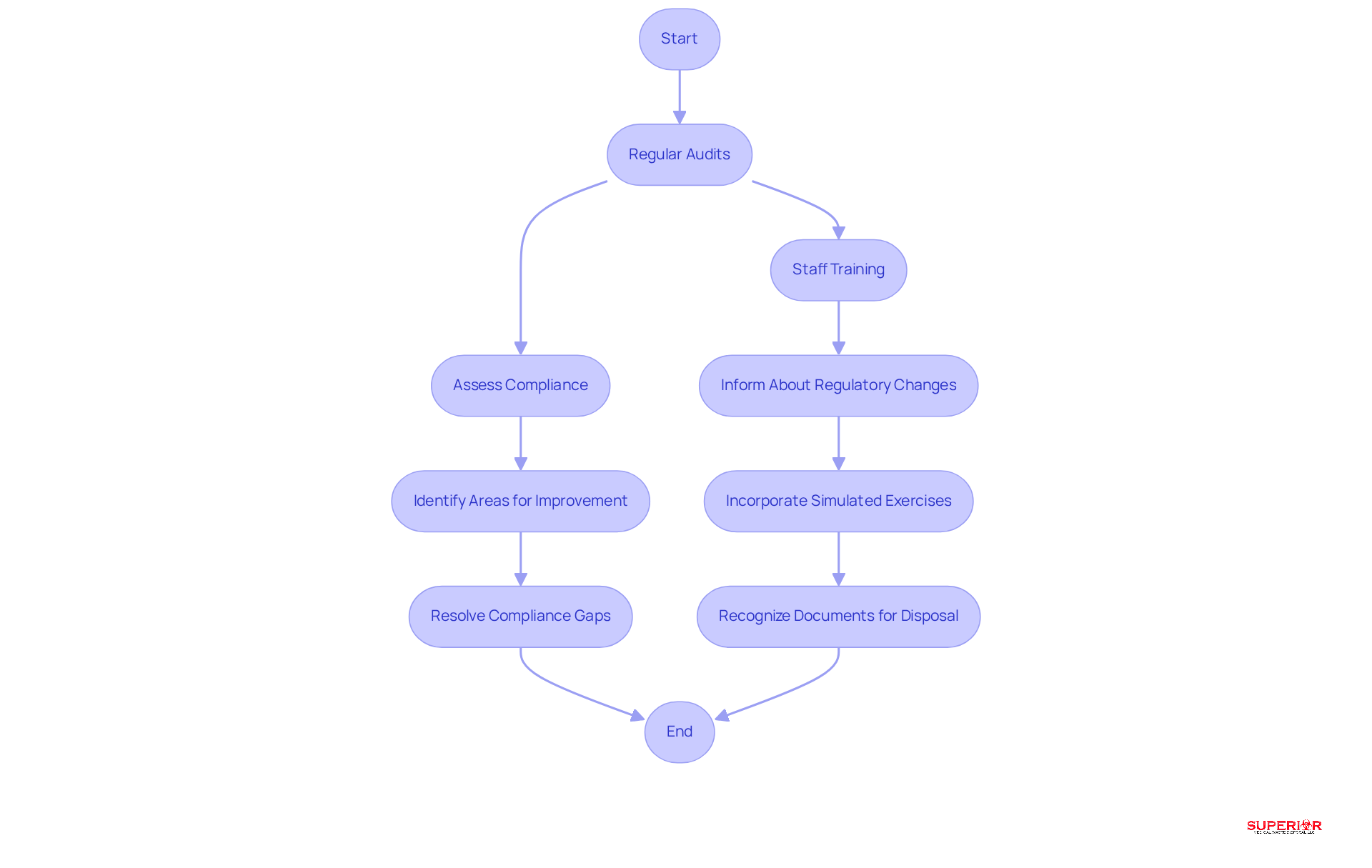
An effective program for the requires and thorough . Audits enable facilities to assess compliance with disposal policies and identify areas for improvement. These evaluations ensure that all staff members follow , allowing for prompt resolution of any .
Equally important is ongoing , which keeps employees informed about and securely. often incorporate simulated exercises, helping employees recognize documents that require disposal and understand the appropriate destruction methods.
Statistics show that organizations with strong training initiatives experience a notable decrease in compliance violations, underscoring the necessity of cultivating a and compliance. By prioritizing these practices, healthcare facilities can significantly enhance the and reduce risks associated with the improper .
Conclusion
The secure disposal of medical records is essential not only for regulatory compliance but also for maintaining patient trust and protecting sensitive information. Healthcare organizations must navigate a complex array of regulations, including HIPAA and state-specific laws, to ensure that medical records are disposed of in ways that make them unreadable and irretrievable. Adapting policies to meet these evolving standards is crucial for compliance and risk mitigation.
Key practices include:
- Implementing secure destruction methods, such as shredding and incineration
- Partnering with certified disposal services that follow stringent security protocols
- Conducting regular audits
- Providing comprehensive staff training
These practices are vital in reinforcing security measures, ensuring that all employees are equipped to handle sensitive information appropriately. By prioritizing these measures, healthcare facilities can significantly reduce the risk of data breaches and uphold the integrity of their operations.
Ultimately, the responsibility for secure medical record disposal extends beyond mere compliance with regulations; it involves fostering a culture of accountability and vigilance within healthcare organizations. As regulations tighten and the landscape of data security evolves, it is imperative for healthcare providers to remain informed and proactive. Investing in best practices for medical record disposal is crucial for protecting patient information and enhancing overall operational integrity.
Frequently Asked Questions
What are the regulatory requirements for medical record disposal?
Healthcare establishments must ensure that the disposal of medical records, including Protected Health Information (PHI), renders them unreadable and irretrievable, as mandated by the Health Insurance Portability and Accountability Act (HIPAA).
Are there state-specific regulations for medical record retention?
Yes, state laws may impose stricter retention and disposal requirements. For example, in Florida, medical records must be kept for at least five years following the last patient contact, while in North Carolina, there is an eleven-year retention period from discharge.
What changes are expected in regulations starting in 2026?
Starting in 2026, healthcare facilities will need to comply with updated regulations that could introduce more stringent protocols for the disposal of medical records.
Why is it important for healthcare establishments to assess and revise their policies regularly?
Regularly assessing and revising policies ensures compliance with evolving regulations and mitigates legal risks associated with improper disposal of medical records.
How can healthcare facilities promote compliance with medical record disposal regulations?
Training staff on regulatory requirements is vital to foster a culture of compliance within the organization, helping to protect sensitive information and enhance operational integrity.
List of Sources
- Understand Regulatory Requirements for Medical Record Disposal
- HIPAA Retention Requirements – 2026 Update (https://hipaajournal.com/hipaa-retention-requirements)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- hipaajournal.com (https://hipaajournal.com/hipaa-updates-hipaa-changes)
- Office for Civil Rights Announces Civil Enforcement Program for Confidentiality of Substance Use Disorder Patient Records (https://hhs.gov/press-room/hhs-announce-civil-enforcement-program-sud-patient-records.html)
- Implement Secure Destruction Methods for Compliance
- HIPAA Retention Requirements – 2026 Update (https://hipaajournal.com/hipaa-retention-requirements)
- Healthcare Data Breach Statistics (https://hipaajournal.com/healthcare-data-breach-statistics)
- HIPAA Compliance for Medical Document Shredding Companies (https://hipaajournal.com/hipaa-compliance-for-medical-document-shredding-companies)
- Secure Document Destruction Trends to Watch in 2026 | A1 Data Shred (https://secdocshredding.com/secure-document-destruction-trends-to-watch-in-2026)
- Select Appropriate Disposal Methods and Partners
- Bio-MED Regulated Waste Solutions (https://getbiomed.com/medical-waste/collaborative-efforts-in-medical-waste-management-a-multi-stakeholder-approach)
- Secure Document Destruction Trends to Watch in 2026 | A1 Data Shred (https://secdocshredding.com/secure-document-destruction-trends-to-watch-in-2026)
- HIPAA Violation Statistics: 2026 Recent Violation Cases, Trends (https://ifaxapp.com/hipaa/hipaa-violation-statistics)
- What Healthcare Must Know About PHI Disposal & Medical Waste in 2026 (https://appliedinnovation.com/health-services/what-healthcare-must-know-about-phi-disposal-medical-waste-in-2026)
- 51 HIPAA Statistics Every Healthcare Entity Needs to Know in 2026 | UpGuard (https://upguard.com/blog/hipaa-statistics)
- Conduct Regular Audits and Staff Training for Compliance
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- Conducting Regular Compliance Audits in Healthcare (https://shccares.com/blog/workforce-solutions/conducting-healthcare-compliance-audits)
- Respond Effectively to Healthcare Audits and Investigations | University of Miami School of Law (https://news.miami.edu/law/stories/2026/01/respond-effectively-to-healthcare-audits-and-investigations.html)
- 25 Inspiring Workplace Safety Quotes for Safer Workspaces (https://yodeck.com/use-cases/workplace-safety-quotes)
- Top 20 Safety Quotes To Improve Your Safety Culture (https://blog.safetyculture.com/industry-trends/top-20-safety-quotes-improve-safety-culture)
