Introduction
Healthcare facilities play a crucial role in public health, yet they encounter significant challenges in managing the various types of clinical waste they produce. Effective waste management is essential, as it not only protects the health of staff and patients but also ensures adherence to stringent regulations governing the disposal of hazardous materials. As healthcare administrators navigate the complexities of waste classification and disposal methods, they face a critical question: how can they adopt best practices that reduce risks while fostering a culture of safety and compliance?
Identify and Classify Medical Waste Types
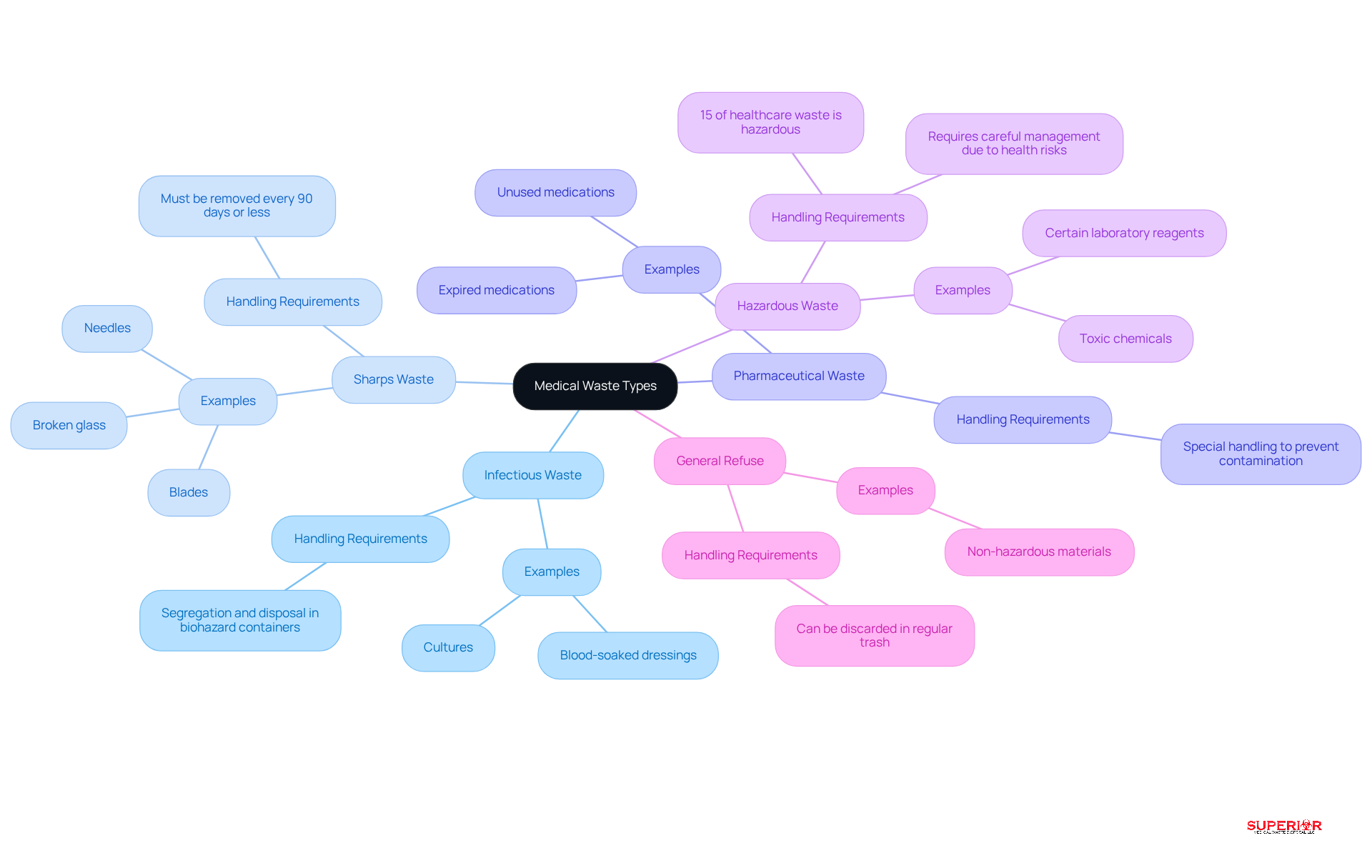
Healthcare facilities generate a diverse array of medical waste, categorized into several key groups:
- Infectious Waste: This category includes materials contaminated with pathogens, such as blood-soaked dressings and cultures, which pose significant health risks.
- Sharps Waste: Items like needles, blades, and broken glass fall under this classification, presenting dangers of injury and infection to staff and patients. All medical refuse-producing facilities are legally required to have their sharps waste removed from their premises every 90 days or less, regardless of the volume generated.
- Pharmaceutical Waste: This category includes medications and drugs to prevent environmental contamination and ensure safe disposal.
- Hazardous Waste: This includes chemicals and materials that pose risks to health or the environment, such as certain laboratory reagents and toxic substances. Notably, regulations govern hazardous waste, underscoring the need for careful management.
- General Refuse: Non-hazardous materials that can be discarded in regular trash, representing the bulk of refuse generated in healthcare settings.
Proper classification of medical refuse is crucial for compliance with stringent regulations, including obtaining a Certificate of Registration for facilities producing any volume of medical waste, which must be renewed every three years. The Centers for Disease Control and Prevention (CDC) states, “Safe HCW management practices reflect on HCF service quality and encompass all activities related to the generation, segregation, transportation, storage, treatment and disposal of refuse.” Additionally, the World Health Organization (WHO) suggests establishing a color-coding system for disposal containers. This system enables straightforward recognition and separation of material types, thereby improving waste management within healthcare facilities. At our organization, we implement waste management protocols by ensuring that infectious materials are autoclaved and shredded to decrease volume by 70% before disposal, adhering to best practices that significantly lower the risks associated with improper refuse disposal. By investing in a contemporary healthcare refuse management system, healthcare organizations can evade possible penalties and reputational harm, promoting a safer healthcare atmosphere while enabling staff to concentrate more on patient care.
Understand Regulatory Compliance and Standards
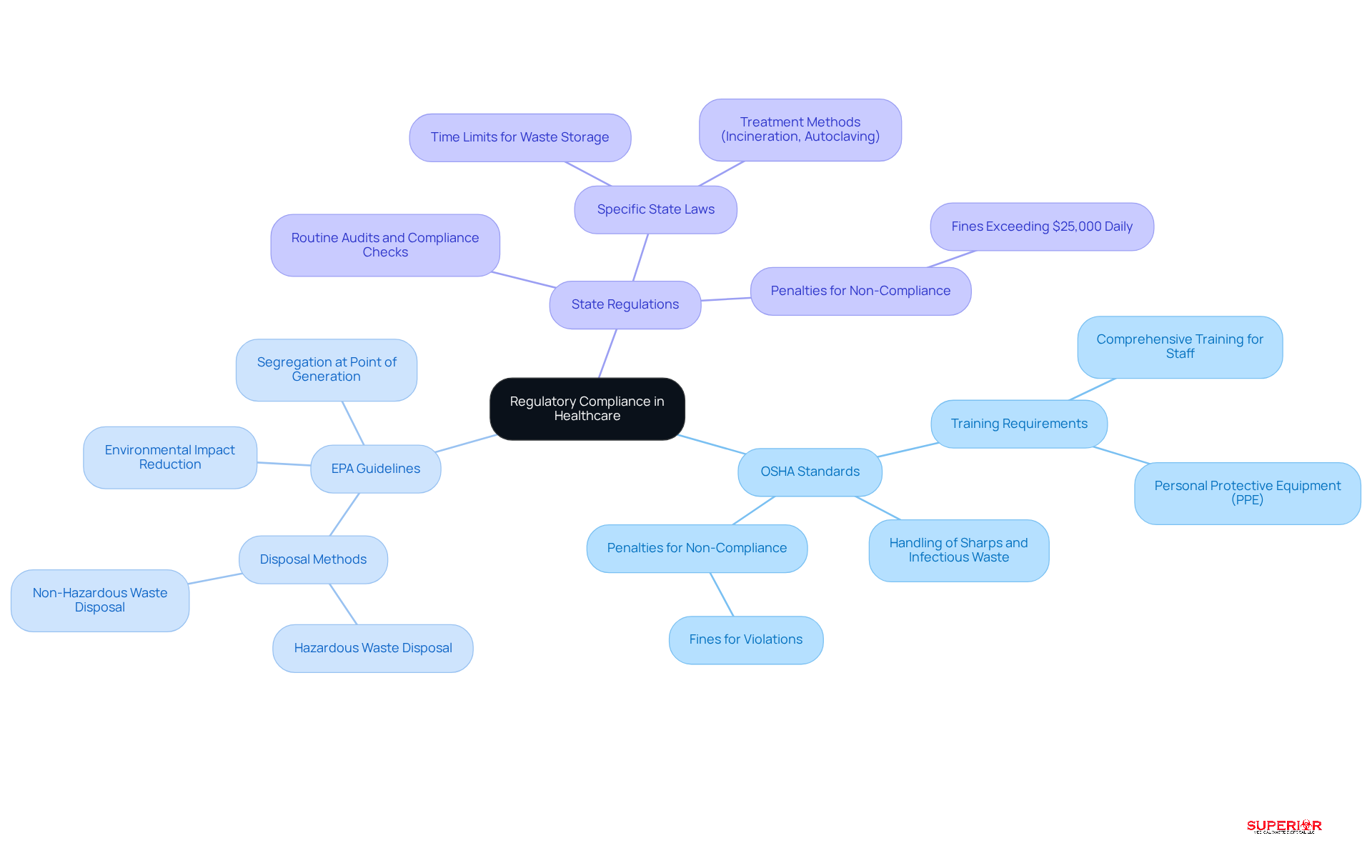
Healthcare managers must possess a thorough understanding of the regulations to ensure compliance and safety within their facilities. The key regulations include:
- OSHA regulations: These regulations are designed to protect healthcare workers handling medical waste. Facilities are required to provide training to minimize risks associated with exposure to hazardous materials.
- EPA guidelines: The Environmental Protection Agency outlines standards. These guidelines emphasize the importance of proper disposal and ensuring that refuse is treated and disposed of in a manner that protects public health. For instance, healthcare facilities must separate refuse at the point of generation, using clearly labeled, leak-proof containers to prevent contamination and ensure compliance with federal standards.
- State laws: Each state may impose specific laws regarding medical refuse disposal, which can vary significantly. For example, states like Washington have stringent time limits on how long untreated waste can be stored on-site, while others may mandate specific treatment methods such as incineration or autoclaving. Routine audits and adherence checks are essential for complying with these regulations and avoiding potential penalties, which can exceed $25,000 daily for non-compliance.
Staying informed about regulatory changes and conducting regular training sessions for staff are crucial strategies for mitigating risks and enhancing compliance. Facilities that implement effective waste management practices not only improve safety but also lower the risk of violations. By prioritizing adherence to OSHA, EPA, and state guidelines, healthcare administrators can create a safer environment for both staff and patients.
Implement Effective Waste Disposal Procedures
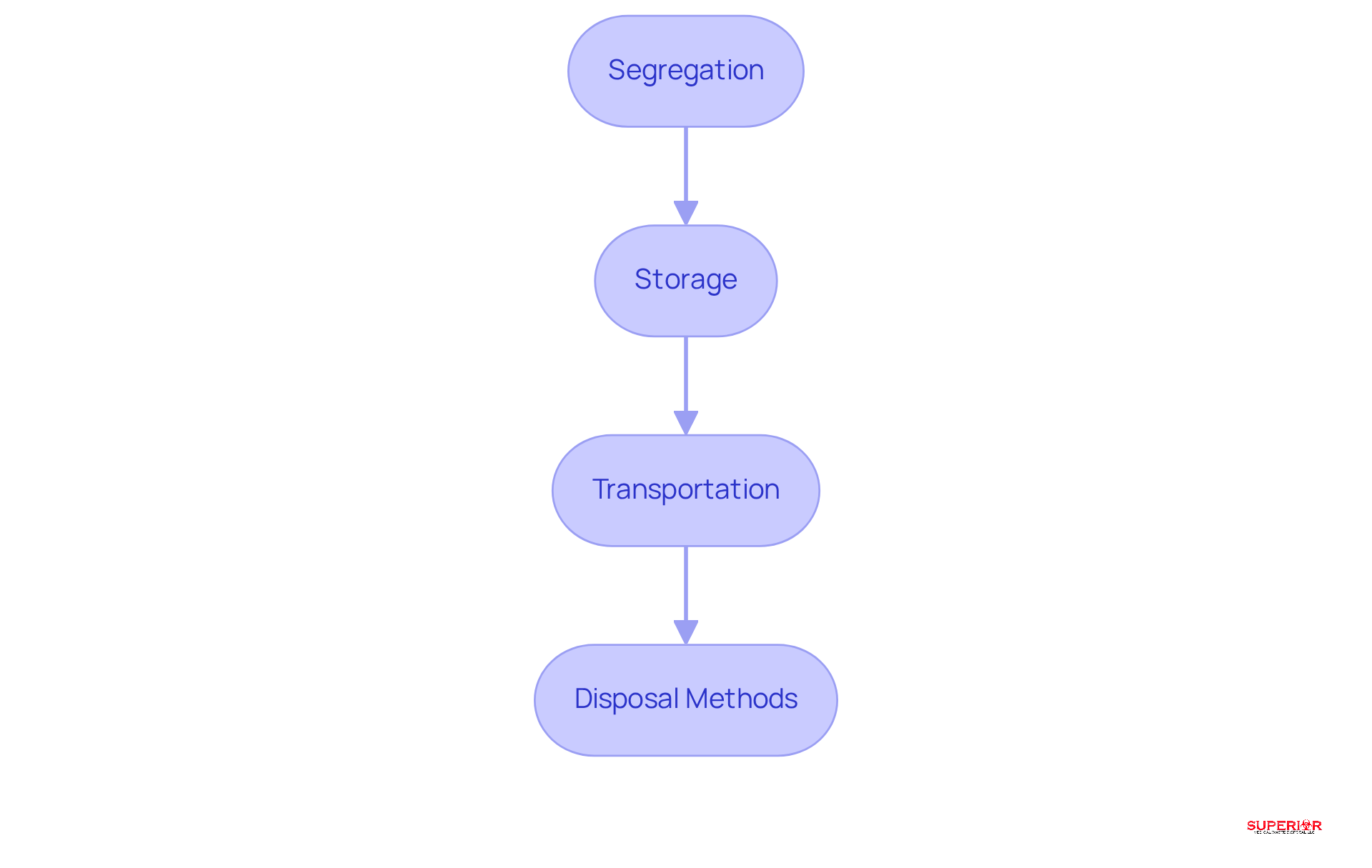
To implement effective waste disposal procedures, healthcare facilities should adhere to the following best practices:
- Segregation: Waste must be segregated at the point of generation. Clearly labeled containers for various refuse types should be utilized to prevent cross-contamination and ensure compliance with evolving regulations. This practice is crucial, as it reduces risks and operational inefficiencies.
- Storage: Waste should be stored in secure, leak-proof containers that are easily identifiable. Storage areas must comply with local regulations, and establishments should provide training on handling procedures. Regular monitoring of storage areas is essential to prevent unauthorized access and ensure safety. Facilities should consider implementing color-coded bins and instructive posters to enhance awareness and adherence to waste management protocols among staff.
- Transportation: Waste must be transported to disposal facilities. All personnel involved in transportation must receive training in handling hazardous materials, ensuring adherence to OSHA and DOT regulations. This training is vital for minimizing risks during transit and maintaining safety.
- Disposal methods are essential for proper waste management in healthcare settings. Facilities should choose suitable methods based on the type of refuse produced. Options include incineration, autoclaving, and chemical disinfection. At Superior Medical Disposal, we utilize autoclaving to steam treat biohazard materials, effectively disinfecting them before shredding to reduce volume by 70%, followed by disposal in a sanitary landfill. Regularly review and update disposal methods to align with best practices and regulatory changes. Furthermore, ensure adherence to pharmaceutical disposal procedures and provide training for staff to uphold legal standards.
Provide Staff Training and Education on Waste Management
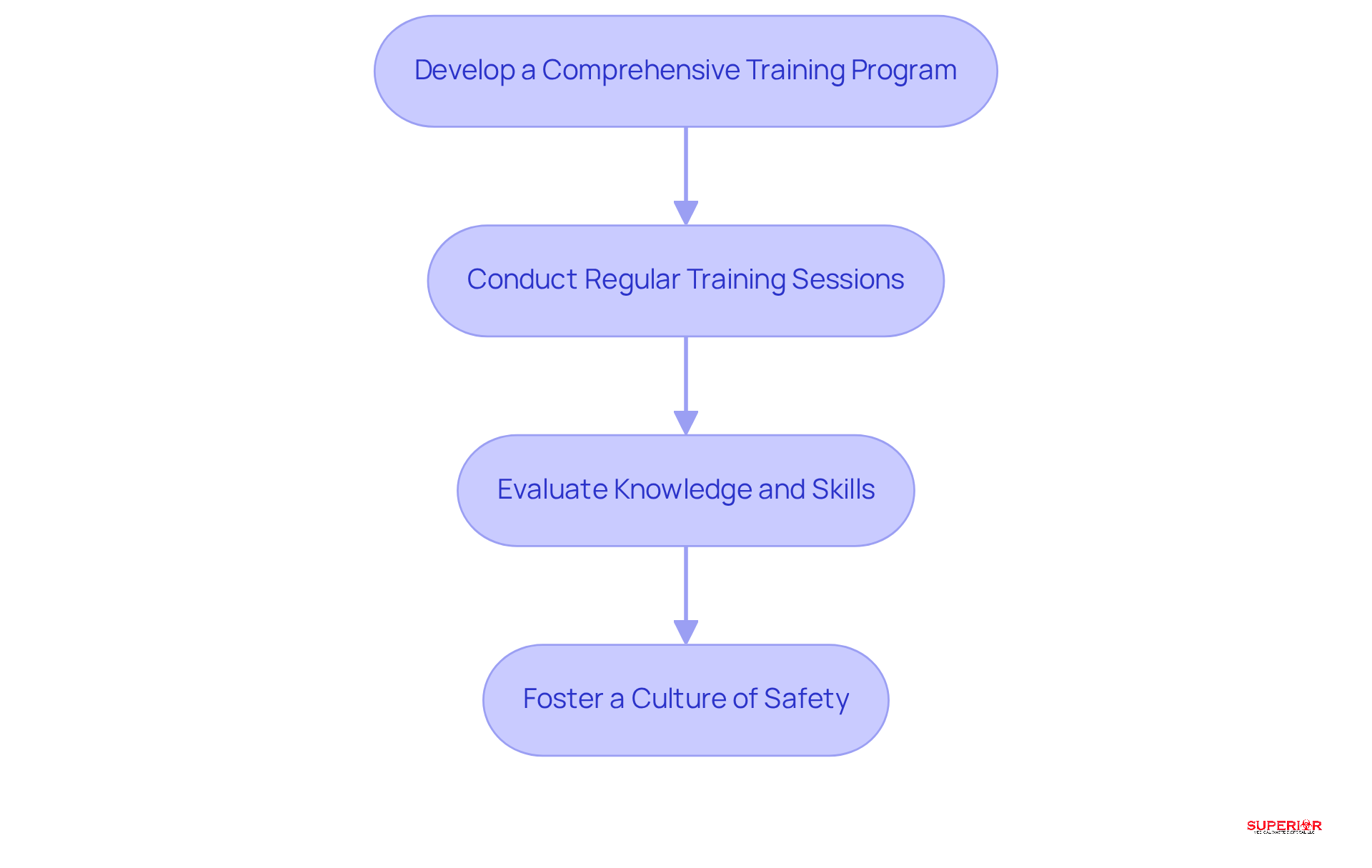
Training and education are essential components of an effective program within healthcare facilities. To ensure compliance and safety, organizations should take the following steps:
- Develop a Comprehensive Program: Establish a thorough program that covers all aspects of medical refuse management, including identification, segregation, handling, and disposal protocols. This program must be tailored to accommodate the diverse educational levels of staff, ensuring accessibility for everyone involved.
- Schedule Training Sessions: Schedule ongoing training sessions to keep staff updated on the latest regulations and best practices. Incorporating hands-on training and real-life scenarios not only enhances engagement but also reinforces learning, enabling staff to apply their knowledge effectively in practical situations.
- Implement Assessments: Implement assessments to measure staff understanding of resource management protocols. Regular evaluations help identify knowledge gaps and provide opportunities for feedback, facilitating continuous improvement of training materials and methods.
- Encourage Communication: Encourage staff to express any concerns or issues related to refuse management. By creating an environment that prioritizes communication, organizations enhance operational efficiency and empower employees to take ownership of their roles in waste management.
Conclusion
Effective management of clinical waste is crucial for healthcare administrators who seek to ensure safety and compliance within their facilities. By understanding the different types of medical waste and implementing best practices for classification, segregation, and disposal, healthcare organizations can significantly reduce the risks associated with improper waste handling. The emphasis on regulatory compliance highlights the necessity of adhering to guidelines established by OSHA, EPA, and state regulations, which are essential for maintaining a safe environment for both staff and patients.
This article explores key strategies, including the importance of comprehensive staff training and education on waste management protocols. By fostering a culture of safety and ensuring that employees are well-equipped with the knowledge to handle medical waste appropriately, healthcare facilities can enhance operational efficiency while minimizing the potential for costly penalties. Furthermore, implementing effective waste disposal procedures, such as utilizing specialized containers and transportation methods, is vital for maintaining compliance and reducing environmental impact.
Ultimately, prioritizing clinical waste solutions not only safeguards public health but also reinforces the integrity of healthcare organizations. As the healthcare landscape continues to evolve, staying informed about innovative waste disposal technologies and regulatory changes will be essential for administrators. By adopting these best practices, healthcare facilities can create a safer, more efficient environment that allows staff to concentrate on what truly matters – providing exceptional patient care.
Frequently Asked Questions
What are the main types of medical waste generated by healthcare facilities?
The main types of medical waste include Infectious Waste, Sharps Waste, Pharmaceutical Waste, Hazardous Waste, and General Refuse.
What constitutes Infectious Waste?
Infectious Waste includes materials contaminated with pathogens, such as blood-soaked dressings and cultures, which pose significant health risks.
What items are classified as Sharps Waste?
Sharps Waste includes items like needles, blades, and broken glass, which present dangers of injury and infection to staff and patients.
What regulations exist regarding the disposal of Sharps Waste?
All medical refuse-producing facilities are legally required to have their sharps and biohazard materials removed from their premises every 90 days or less, regardless of the volume generated.
How should Pharmaceutical Waste be handled?
Expired or unused medications require special handling to prevent environmental contamination and ensure safe disposal.
What is considered Hazardous Waste in healthcare?
Hazardous Waste includes chemicals and materials that pose risks to health or the environment, such as certain laboratory reagents and toxic substances.
What percentage of healthcare refuse is classified as hazardous?
Approximately 15% of healthcare refuse is classified as hazardous.
What is General Refuse in the context of medical waste?
General Refuse refers to non-hazardous materials that can be discarded in regular trash, representing the bulk of refuse generated in healthcare settings.
Why is proper classification of medical waste important?
Proper classification is crucial for compliance with regulations, including obtaining a Certificate of Registration for facilities producing clinical waste solutions, which must be renewed every three years.
What does the CDC say about healthcare waste management practices?
The CDC states that “Safe HCW management practices reflect on HCF service quality and encompass all activities related to the generation, segregation, transportation, storage, treatment, and disposal of refuse.”
How does the WHO suggest improving waste disposal in healthcare facilities?
The WHO suggests establishing a color-coding system for disposal containers to enable straightforward recognition and separation of material types.
What practices does Superior Medical Refuse Disposal implement for clinical waste solutions?
Superior Medical Refuse Disposal ensures that biohazard materials are autoclaved and shredded to decrease volume by 70% before disposal.
What are the benefits of investing in a contemporary healthcare refuse management system?
Investing in a contemporary system helps healthcare organizations evade possible penalties and reputational harm while promoting a safer atmosphere and allowing staff to focus more on patient care.
List of Sources
- Identify and Classify Medical Waste Types
- Managing 5.9 Million Tons Annually for a Sustainable Future – The Growing Challenge of Medical Waste Disposal (https://medprodisposal.com/managing-5-9-million-tons-annually-for-a-sustainable-future-the-growing-challenge-of-medical-waste-disposal)
- The Ins and Outs of Medical Waste Systems: Best Practices and Management – Routeware (https://routeware.com/blog/the-ins-and-outs-of-medical-waste-systems-best-practices-and-management)
- Expert Guide For Medical Waste Management In Healthcare 2026 (https://securewaste.net/professional-medical-waste-management-for-healthcare-facilities)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC9858835)
- wastetodaymagazine.com (https://wastetodaymagazine.com/tag/medical-waste)
- Understand Regulatory Compliance and Standards
- The Ins and Outs of Medical Waste Systems: Best Practices and Management – Routeware (https://routeware.com/blog/the-ins-and-outs-of-medical-waste-systems-best-practices-and-management)
- Washington Medical Waste Regulations: 2026 Compliance Guide (https://octopussaas.com/post/medical-waste-regulations-in-washington)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- Biomedical Waste Solutions For 2026 | MedSharps (https://medsharps.com/blog/biomedical-waste-solutions-for-2026)
- EPA’s Third Rule Is Now Fully Enforced – What Waste Generators Need to Know – Safety Partners, LLC (https://safetypartnersinc.com/epas-third-rule-is-now-fully-enforced-what-waste-generators-need-to-know)
- Implement Effective Waste Disposal Procedures
- Healthcare Waste Segregation Practice and Associated Factors among Healthcare Professionals Working in Public and Private Hospitals, Dire Dawa, Eastern Ethiopia – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9899136)
- The Future of Waste Management in Hospitals: Trends to Watch (https://danielshealth.com/knowledge-center/future-of-waste-management)
- Biomedical Waste Solutions For 2026 | MedSharps (https://medsharps.com/blog/biomedical-waste-solutions-for-2026)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- Provide Staff Training and Education on Waste Management
- Educating Hospital Staff on Waste Management | Waste Managed (https://wastemanaged.co.uk/our-news/hospital/educating-hospital-staff-on-waste-management)
- The Future of Waste Management in Hospitals: Trends to Watch (https://danielshealth.com/knowledge-center/future-of-waste-management)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC6040849)
- medsharps.com (https://medsharps.com/blog/the-importance-of-training-staff-on-regulated-medical-waste-a-professional-guide)
