Introduction
In healthcare settings, the safe disposal of sharp instruments is a critical concern. Sharps containers serve as the frontline defense against needlestick injuries and the transmission of infections. Understanding when to change these containers is essential not only for maintaining safety but also for complying with regulatory standards.
However, many healthcare professionals may overlook key indicators that signal the need for replacement. Recognizing the telltale signs that a sharps container is no longer fit for use is vital. Proper procedures can ensure a safer environment for both staff and patients.
Understand the Purpose of Sharps Containers
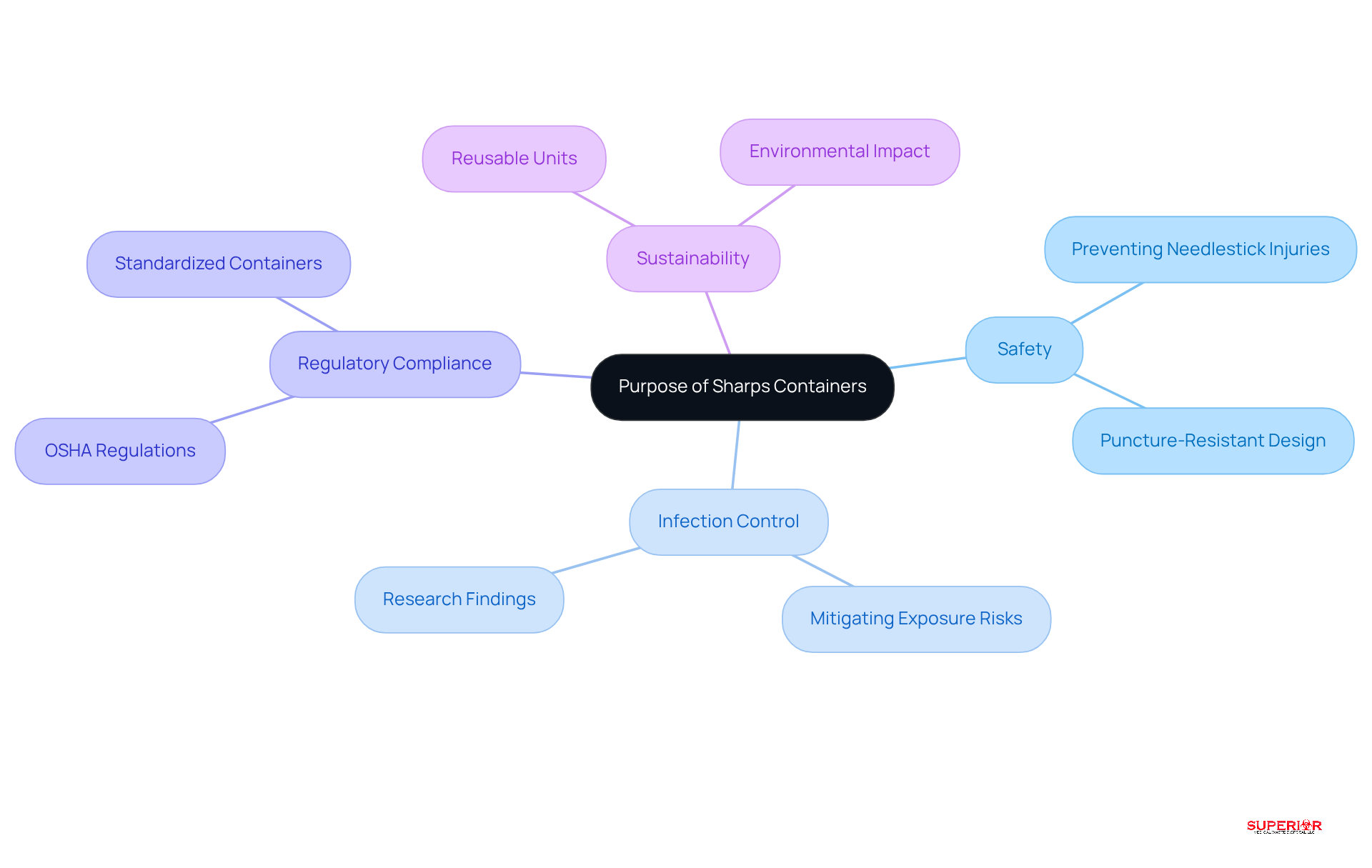
Sharps bins serve as essential receptacles for the secure disposal of pointed medical instruments, such as needles, blades, and other items that pose a risk of puncture or cut. Their primary purpose is to prevent infections and the transmission of infections, particularly bloodborne pathogens. These containers are designed to be puncture-resistant, leak-proof, and clearly marked to indicate their hazardous contents, ensuring that medical professionals can easily identify and utilize them correctly.
The significance of disposal units extends beyond immediate safety; they play a crucial role in infection control within healthcare environments. By containing potentially infectious materials, these vessels help mitigate the risk of exposure for both staff and patients. Research indicates that the use of sharps containers can significantly reduce the incidence of needlestick injuries, a common concern in healthcare settings.
Healthcare professionals emphasize the importance of proper disposal in fostering a secure work environment. Adhering to safety protocols is vital for protecting medical staff from preventable injuries and infections. Moreover, employing standardized, certified containers aligns with regulatory standards, thereby enhancing compliance and operational efficiency.
Practical examples illustrate the effectiveness of disposal units across various healthcare settings. Many hospitals have adopted reusable disposal units, which can be utilized up to 600 times, substantially reducing environmental impacts and costs associated with single-use alternatives. This transition not only promotes sustainability but also reinforces the importance of safe disposal practices, as evidenced by partnerships with commercial autoclaving facilities for the secure treatment of medical waste.
In summary, understanding the purpose and proper use of sharps containers is essential for medical practitioners. By prioritizing their utilization, facilities can enhance safety protocols, protect staff and patients, and contribute to a more sustainable healthcare system. As the healthcare sector prepares for new regulations in 2026, the importance of proper disposal of medical instruments will continue to grow.
Identify Key Indicators for Changing Sharps Containers
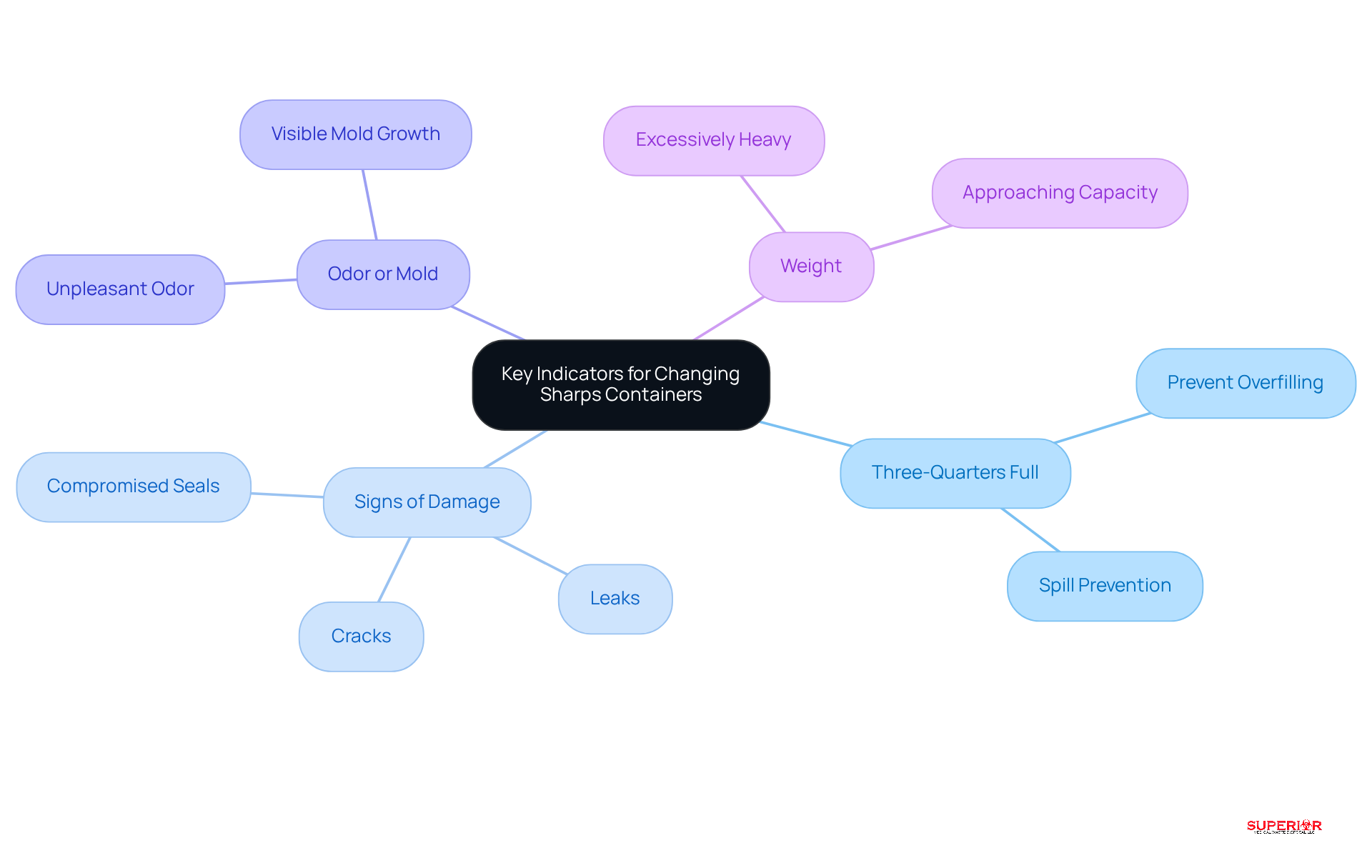
To ensure the safety of medical instruments, it is essential to frequently monitor the condition of disposal units. Key indicators for replacing a sharps container include:
- Most guidelines indicate that you should know when to change a sharps container when it is three-quarters full. This practice helps prevent overfilling, which can lead to spills and injuries.
- Signs of Damage: Regularly inspect the container for cracks, leaks, or compromised seals. Any visible damage can undermine the container’s integrity, making it unsafe for continued use.
- Odor or Mold: If there is any unpleasant odor or visible mold growth inside the container, it should be replaced immediately to mitigate health risks.
- Weight: If the container feels excessively heavy, it may be approaching its capacity and should be assessed for replacement.
By remaining vigilant about these indicators, healthcare professionals can enhance safety. Notably, injury rates increased from 49% in 2021 to 51% in 2022, highlighting ongoing challenges in injury prevention. The Massachusetts Department of Public Health advocates for best practices to enhance safety, which is vital for effective monitoring practices. Additionally, at our organization, we emphasize the importance of adhering to local regulations regarding sharps disposal, including the use of appropriate containers to ensure compliance. Clear documentation and adaptable service models are critical for compliance in waste management, enabling medical facilities to prepare for audits and maintain operational efficiency.
Follow Safe Procedures for Changing Sharps Containers
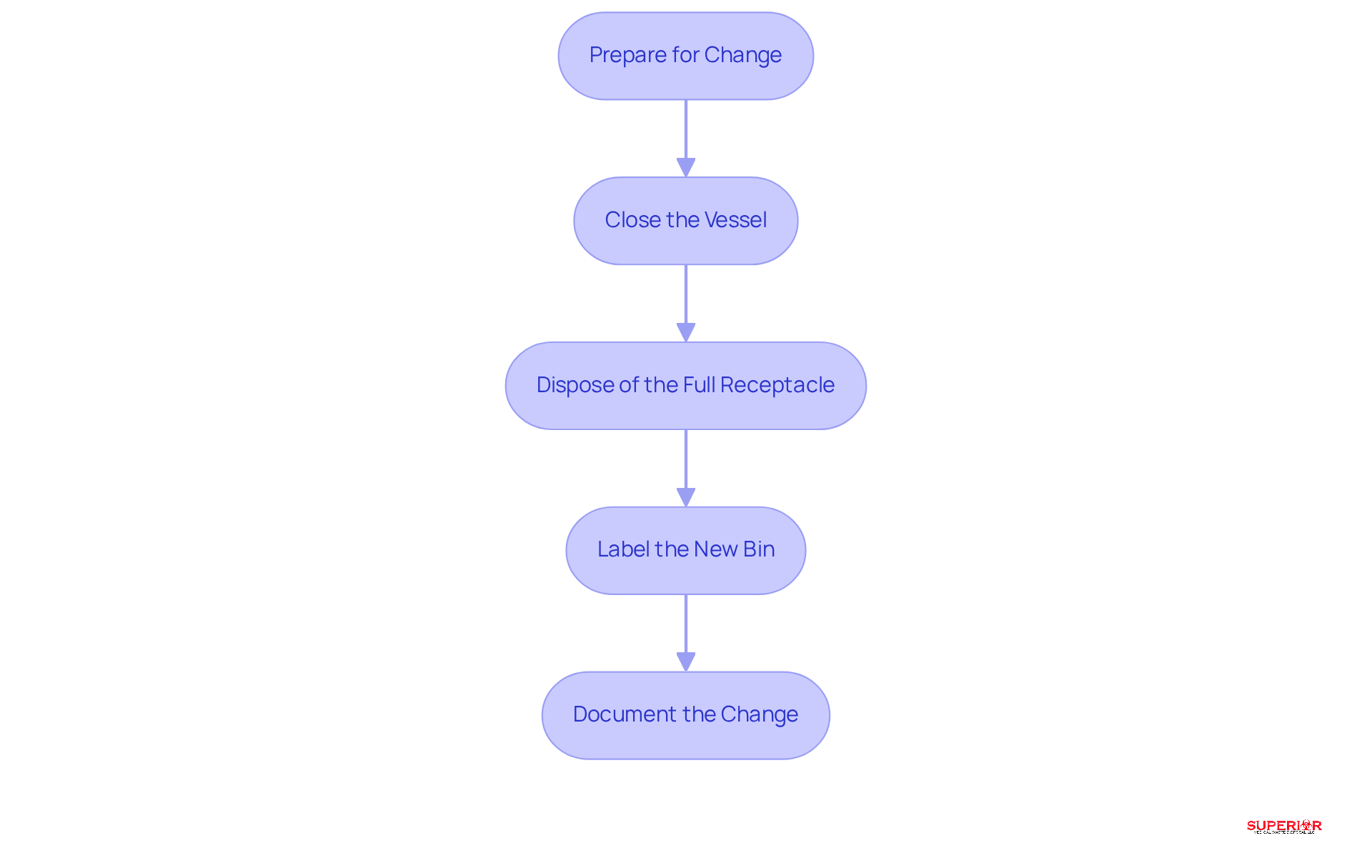
Replacing a waste container necessitates strict adherence to regulations to protect healthcare personnel and patients. This process can be effectively managed by following these essential steps:
- Prepare for Change: Gather essential personal protective equipment (PPE), such as gloves, goggles, and gowns, to wear during the process. Experts emphasize that proper PPE is vital in preventing injuries and ensuring safety during disposal.
- Close the Vessel: Prior to removal, confirm that the vessel is securely closed. Most vessels are equipped with a locking mechanism or a lid that must be sealed to prevent spillage, which is crucial for maintaining a safe environment.
- Disposal: Place the closed receptacle into a designated bag or bin for hazardous waste. It is imperative to avoid placing it in regular trash to comply with regulations and prevent contamination.
- Labeling: Clearly label the new waste bin with the date of use and any other pertinent information. This practice aids in tracking usage and ensures compliance with facility policies.
- Documentation: Keep a log of when containers are changed to ensure adherence to facility policies and regulatory requirements. Statistics indicate that facilities with robust documentation practices achieve better outcomes in disposal procedures for needles.
By following these protocols, medical professionals can significantly reduce the likelihood of injury and comply with regulations, ultimately fostering a safer work environment.
Implement Best Practices for Sharps Container Management
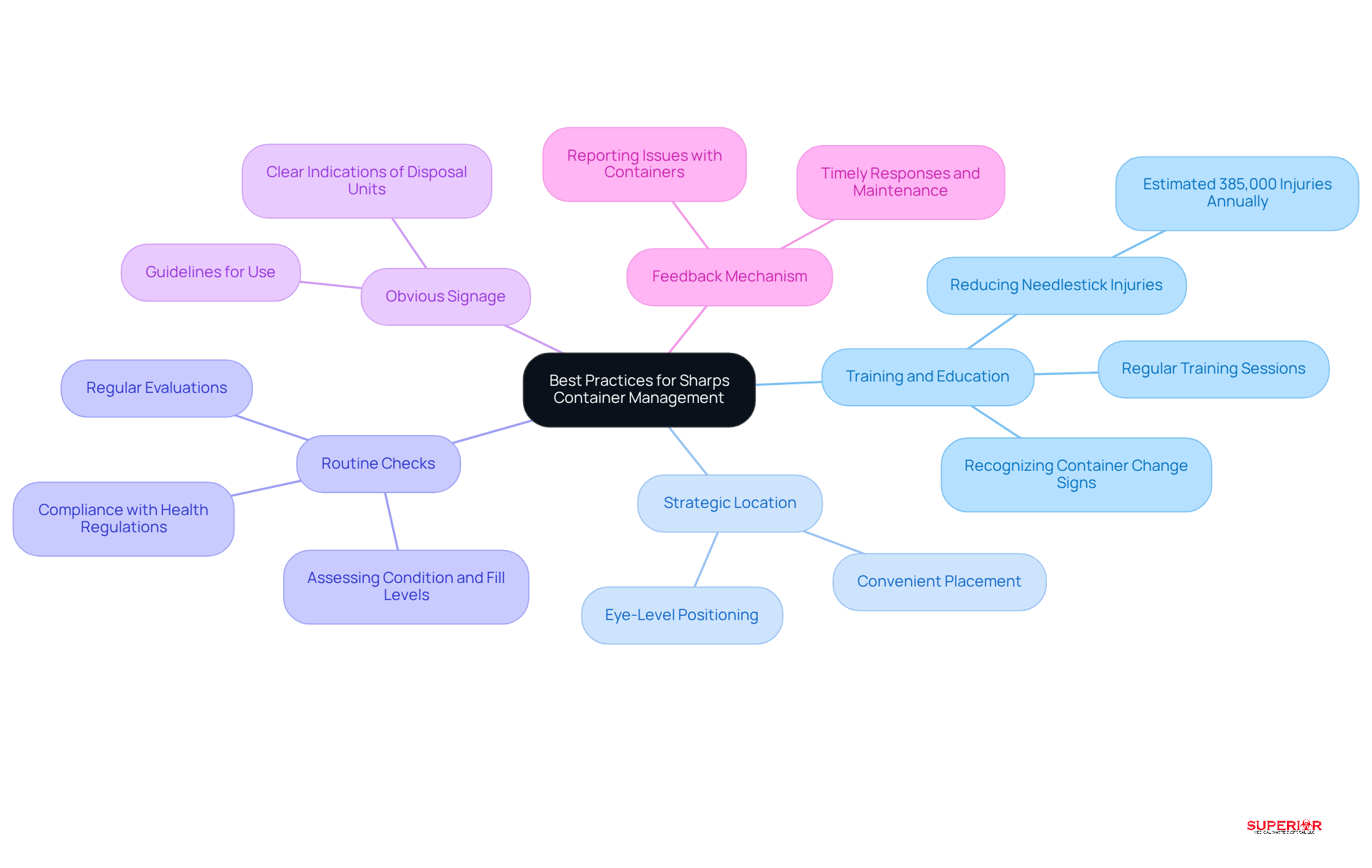
To enhance the safety and effectiveness of sharps disposal, healthcare facilities should implement several best practices:
- Training and Education: Regular training sessions are essential for staff to understand the importance of sharps containers. This includes recognizing signs that indicate a need for change. Comprehensive training can significantly reduce the risk of sharps injuries, which are estimated to occur at a rate of approximately 385,000 annually among U.S. healthcare workers.
- Strategic Location: Placing disposal units in conveniently reachable spots near areas where needles are frequently used promotes prompt disposal. For instance, positioning receptacles at eye level in examination rooms and nursing stations can enhance adherence and reduce the likelihood of improper disposal.
- Regular Inspections: Conduct regular evaluations of needle disposal units to assess their condition, fill levels, and compliance with safety standards. Routine inspections help identify containers that are damaged or nearing capacity, which is crucial for preventing spills and ensuring safety.
- Clear Signage: Implement clear signage to indicate the location of disposal units and provide straightforward guidelines for their use. Effective signage can raise awareness and encourage proper disposal practices among staff.
- Feedback Mechanism: Establish a system for staff to report issues with needle containers, such as damage or overfilling. This feedback loop ensures timely responses and maintenance, contributing to a safer working environment.
By adopting these best practices, healthcare facilities can significantly improve their sharps management, ensuring a safer environment for both staff and patients. The Massachusetts Department of Public Health emphasizes that despite advancements in safety measures, ongoing training and awareness remain vital to reducing sharps injuries, which have plateaued in recent years.
Conclusion
Understanding the critical role of sharps containers in healthcare is essential for maintaining a safe and compliant environment. These containers not only prevent needlestick injuries but also play a vital part in infection control, ensuring that both healthcare professionals and patients are protected from potential hazards. By recognizing when to change these containers and adhering to safe procedures, medical facilities can significantly enhance their operational efficiency and safety protocols.
Key indicators for replacing sharps containers include:
- Monitoring fill levels
- Checking for signs of damage
- Being vigilant about odors or excessive weight
Implementing best practices such as:
- Regular training
- Strategic placement
- Routine inspections
further strengthens the management of these containers. The emphasis on proper disposal methods and compliance with regulations is crucial, as they are pivotal in minimizing risks associated with sharps waste.
Ultimately, fostering a culture of safety through effective sharps container management is imperative in healthcare settings. By prioritizing education and adherence to guidelines, facilities can protect their staff and patients while contributing to a sustainable healthcare system. Continuous improvement in practices surrounding sharps disposal will ensure that safety remains at the forefront of healthcare operations, paving the way for a healthier future.
Frequently Asked Questions
What is the primary purpose of sharps containers?
Sharps containers are designed for the secure disposal of pointed medical instruments, such as needles and blades, to prevent needlestick injuries and the transmission of infections, particularly bloodborne pathogens.
How do sharps containers contribute to infection control in healthcare environments?
By containing potentially infectious materials, sharps containers help mitigate the risk of exposure for both healthcare staff and patients, thereby playing a crucial role in infection control.
Why is it important for healthcare professionals to use sharps containers?
Proper use of sharps containers significantly reduces the incidence of needlestick injuries, which are a common concern in healthcare settings, and helps protect medical staff from preventable injuries and infections.
What regulations must be adhered to regarding needle disposal?
Healthcare professionals must comply with OSHA regulations concerning needle disposal to ensure safety and protect staff from injuries and infections.
What are the benefits of using standardized, certified, puncture-resistant containers?
Using standardized, certified, puncture-resistant containers enhances compliance with regulatory standards and improves operational efficiency in healthcare facilities.
How do reusable disposal units impact environmental sustainability and costs?
Reusable disposal units can be utilized up to 600 times, which reduces environmental impacts and costs associated with single-use alternatives, promoting sustainability in waste management practices.
What role do partnerships with commercial autoclaving facilities play in medical waste disposal?
Partnerships with commercial autoclaving facilities ensure the secure treatment of medical waste, reinforcing safety and compliance in waste management practices.
Why is understanding the proper use of sharps containers important for medical practitioners?
Prioritizing the utilization of sharps containers enhances safety protocols, protects staff and patients, and contributes to a more sustainable healthcare system, especially as new regulations are anticipated in 2026.
List of Sources
- Understand the Purpose of Sharps Containers
- The Vital Role of Sharps Containers in Public Health (https://mycomedical.com/post/the-vital-role-of-sharps-containers-in-public-health)
- medcitynews.com (https://medcitynews.com/2025/04/advancing-patient-planet-health-through-proper-healthcare-waste-management)
- 2026 predictions: Managing the medical waste challenge in home care (https://mcknightshomecare.com/2026-predictions-managing-the-medical-waste-challenge-in-home-care)
- Biomedical Waste Solutions For 2026 | MedSharps (https://medsharps.com/blog/biomedical-waste-solutions-for-2026)
- vernacare.com (https://vernacare.com/the-importance-of-sharps-disposal-in-healthcare-facilities-an-insiders-view)
- Identify Key Indicators for Changing Sharps Containers
- Biomedical Waste Solutions For 2026 | MedSharps (https://medsharps.com/blog/biomedical-waste-solutions-for-2026)
- Sharps Injury Reductions | Journal of Infection Control (https://danielshealth.com/knowledge-center/sharps-injury-reductions-journal-infection-control)
- betsylehmancenterma.gov (https://betsylehmancenterma.gov/news/the-rate-of-sharps-injuries-to-hospital-workers-has-not-declined-in-more-than-10-years)
- Alarming surge in needlestick injuries tackled with essential guide to proper medical waste disposal (https://ems1.com/ems-products/Ambulance-Disposable-Supplies/alarming-surge-in-needlestick-injuries-tackled-with-essential-guide-to-proper-medical-waste-disposal)
- Follow Safe Procedures for Changing Sharps Containers
- medprodisposal.com (https://medprodisposal.com/sharps-disposal-practices-reduce-needle-stick-injuries)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- Awareness About Sharps Disposal Leads to Significant Improvement in Healthcare Safety: an Audit of Compliance in the National Health Service During the COVID-19 Pandemic – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7603408)
- 9 Medical Waste Safety Tips for New Healthcare Faculty (https://medprodisposal.com/medical-waste-safety-tips-new-healthcare-faculty)
- Alarming surge in needlestick injuries tackled with essential guide to proper medical waste disposal (https://ems1.com/ems-products/Ambulance-Disposable-Supplies/alarming-surge-in-needlestick-injuries-tackled-with-essential-guide-to-proper-medical-waste-disposal)
- Implement Best Practices for Sharps Container Management
- medprodisposal.com (https://medprodisposal.com/sharps-disposal-practices-reduce-needle-stick-injuries)
- betsylehmancenterma.gov (https://betsylehmancenterma.gov/news/the-rate-of-sharps-injuries-to-hospital-workers-has-not-declined-in-more-than-10-years)
- infectioncontroltoday.com (https://infectioncontroltoday.com/view/from-awareness-action-educating-staff-sharps-safety-standards)
- Healthcare Management Resolutions To Make Healthcare Safer (https://securewaste.net/healthcare-waste-management-resolutions-to-make-healthcare-safer-in-2026)
