Introduction
Effective management of medical waste is essential for healthcare facilities. Improper handling can lead to significant risks for public health and the environment. This article explores best practices for safe disposal, compliance with regulations, and the protection of healthcare workers and patients. With evolving guidelines and the complexity of waste categories, facilities must navigate this intricate landscape to achieve optimal safety and efficiency.
Define Medical Waste and Its Categories
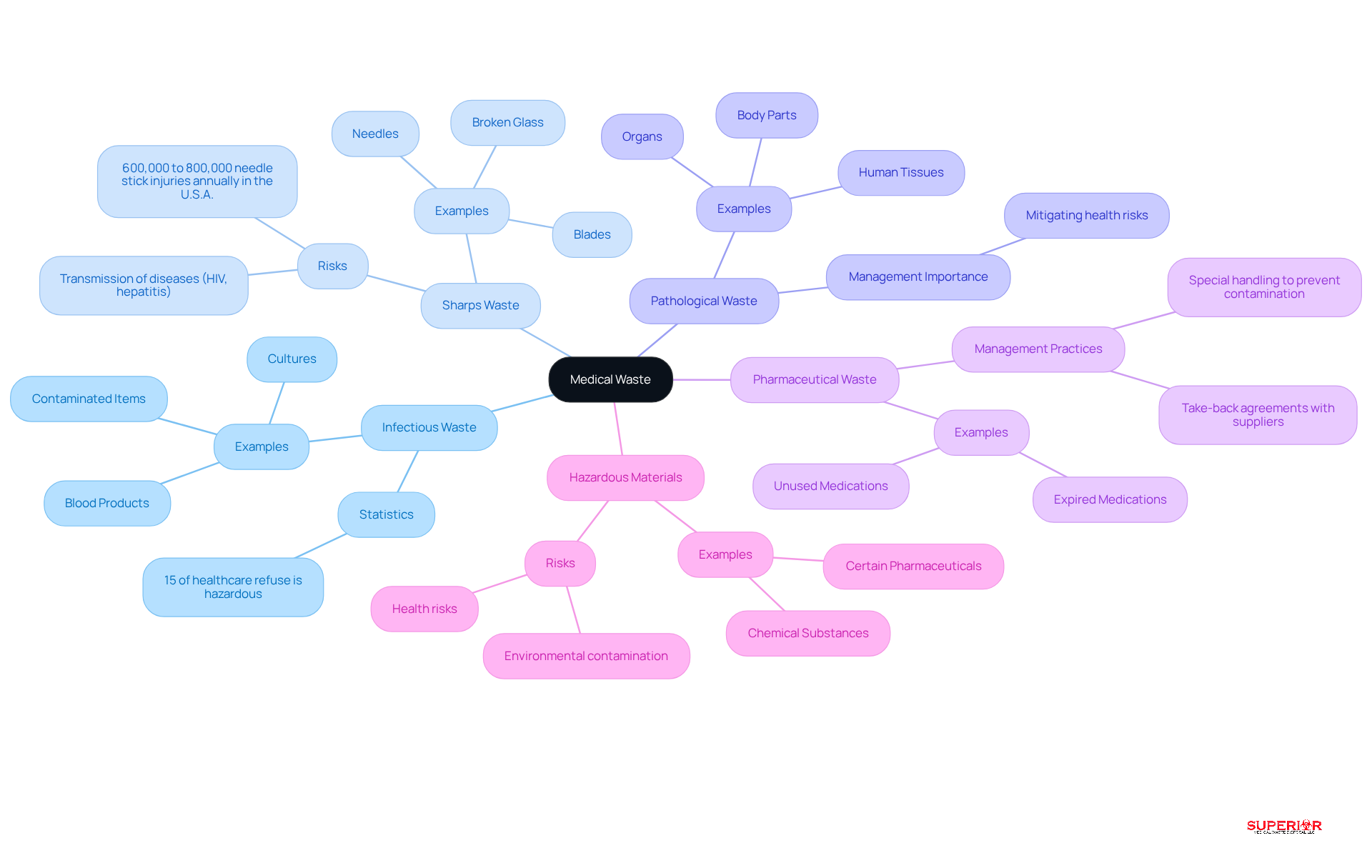
Medical refuse encompasses any byproduct generated in healthcare settings that may be contaminated by blood, bodily fluids, or other potentially infectious materials. Accurately categorizing this material is essential for ensuring safe and compliant disposal practices. The primary categories of medical waste include:
- Infectious Waste: This category includes materials that pose a risk of infection, such as cultures, blood products, and contaminated items. Approximately 15% of healthcare refuse is classified as hazardous, which can be infectious, toxic, or radioactive.
- Sharps Waste: Items that can puncture or cut skin, including needles, blades, and broken glass, fall under this category. Sharps injuries can lead to the transmission of serious diseases, including HIV and hepatitis. It is estimated that 600,000 to 800,000 needle stick injuries and other percutaneous injuries are reported annually in the U.S.A. This underscores the necessity for stringent to ensure the protection of healthcare workers and patients.
- Pathological Waste: This category consists of human tissues, organs, and body parts discarded after surgical procedures or autopsies. Proper management of medical waste and disposal are crucial to mitigate health risks associated with this type of refuse.
- [Pharmaceutical Waste](https://global.noharm.org/focus/waste/health-care-waste-treatment-and-disposal-by-type): Expired or unused medications require special handling and disposal to prevent environmental contamination and public health risks. Superior Medical Disposal offers pharmaceutical material handling and removal services, along with efficient stock management and take-back agreements with suppliers to minimize pharmaceutical byproducts. Additionally, OSHA compliance training for staff is provided to ensure legal adherence in managing such materials.
- Hazardous Materials: This includes materials that pose risks to human health or the environment, such as chemical substances and certain pharmaceuticals. Proper handling of hazardous materials is essential, as improper disposal can lead to significant environmental contamination and health risks.
Defining and classifying healthcare refuse precisely are fundamental steps in the management of medical waste, which ensures adherence to regulatory standards and safeguards public health.
Understand Medical Waste Regulations and Compliance Requirements
Healthcare facilities must comply with a complex framework of federal, state, and local regulations governing the management of medical waste. This framework includes several key components:
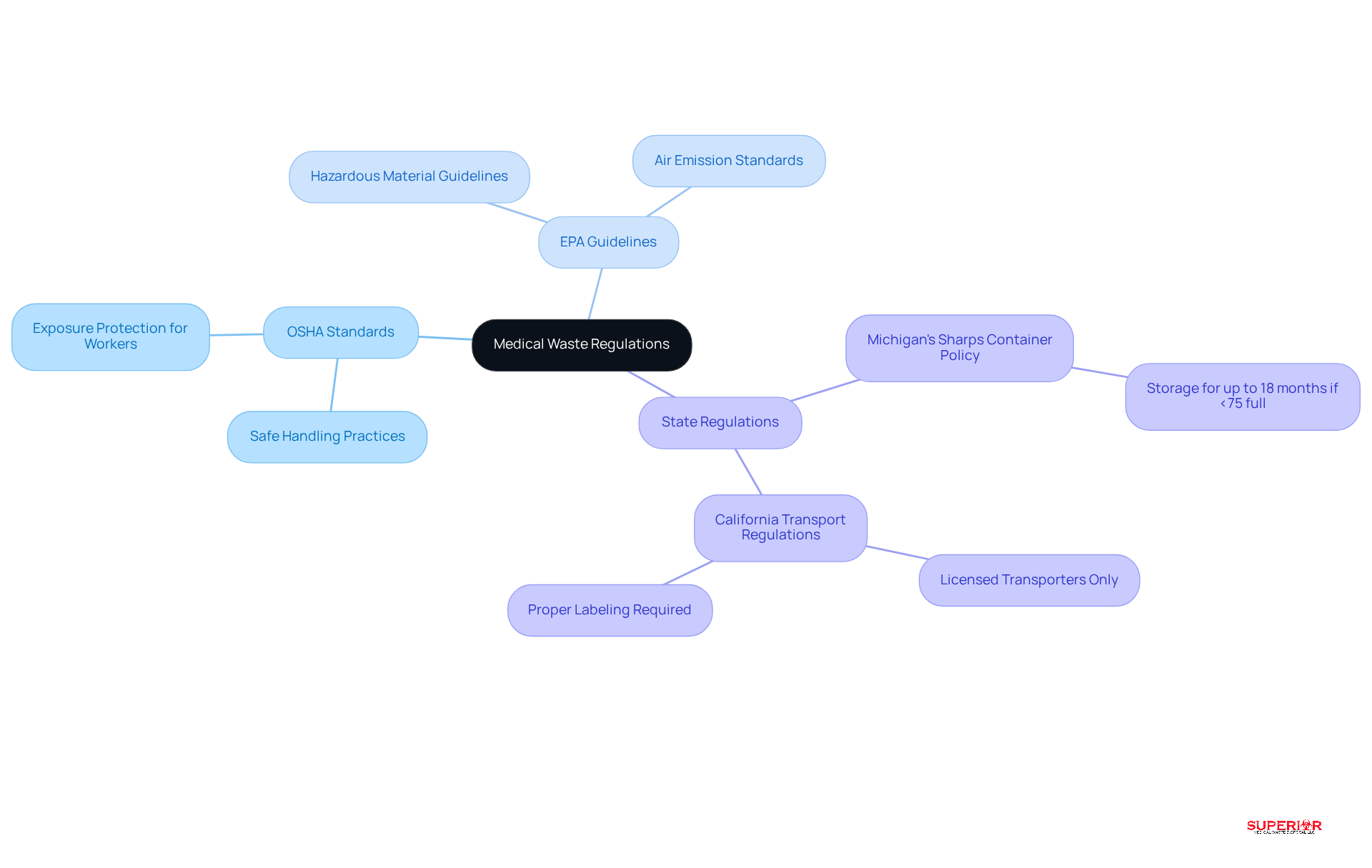
- OSHA Standards: The Occupational Safety and Health Administration enforces regulations that require safe handling and disposal practices to protect healthcare workers from exposure to hazardous materials. Compliance with these standards is essential for the management of medical waste and for maintaining a safe workplace.
- EPA Guidelines: The Environmental Protection Agency oversees the handling of hazardous materials, which encompasses specific types of healthcare refuse. Facilities must adhere to these guidelines for the management of medical waste to ensure environmental protection and compliance with federal standards.
- State Regulations: Each state establishes its own rules regarding medical refuse handling, which may include specific requirements for the storage, transportation, and disposal of medical materials. For instance, recent changes in Michigan law now allow sharps containers to be stored for up to 18 months if they are less than 75% full, reflecting a shift towards more flexible practices.
To ensure compliance, facilities should for the management of medical waste, aligning them with evolving regulations. This proactive approach not only protects the health of staff and patients but also reduces the risk of penalties associated with non-compliance.
Implement Effective Waste Segregation Strategies
Effective material segregation is crucial for the safe and efficient management of medical waste. To implement effective segregation strategies, consider the following best practices:
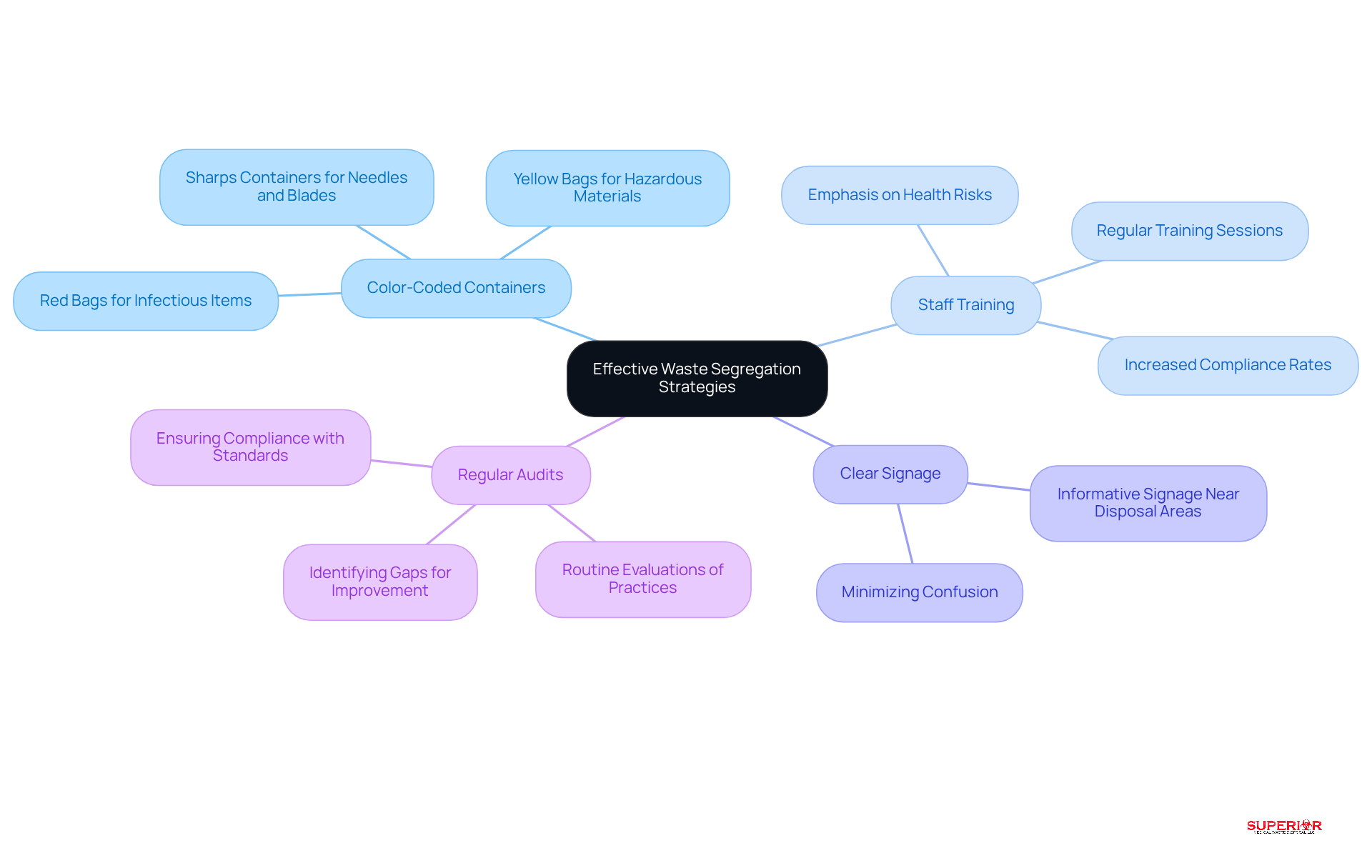
- Color-Coded Containers: Establish a color-coded system to distinctly identify various types of refuse. For instance, use red bags for infectious items, yellow for hazardous materials, and designated sharps containers for needles and blades. This visual cue aids in quick recognition and proper disposal.
- Staff Training: Conduct regular training sessions to educate staff on proper trash segregation techniques. Training should emphasize the significance of and the potential health risks associated with the management of medical waste. Studies indicate that healthcare professionals who receive training are significantly more likely to practice effective disposal separation, thereby enhancing compliance rates.
- Clear Signage: Place clear and informative signage near disposal areas to direct staff on the appropriate disposal methods for different types of refuse. This can minimize confusion and encourage adherence to segregation protocols.
- Regular Audits: Perform routine evaluations of refuse segregation practices to pinpoint gaps and areas needing improvement. These audits are essential for ensuring compliance with regulatory standards and can demonstrate the effectiveness of training programs.
By adopting these strategies, healthcare facilities can mitigate the risks associated with handling health-related refuse and enhance overall safety and compliance.
Establish Safe Collection, Storage, and Disposal Procedures
To ensure the management of medical waste is safe, healthcare facilities must implement comprehensive procedures for collection, storage, and disposal.
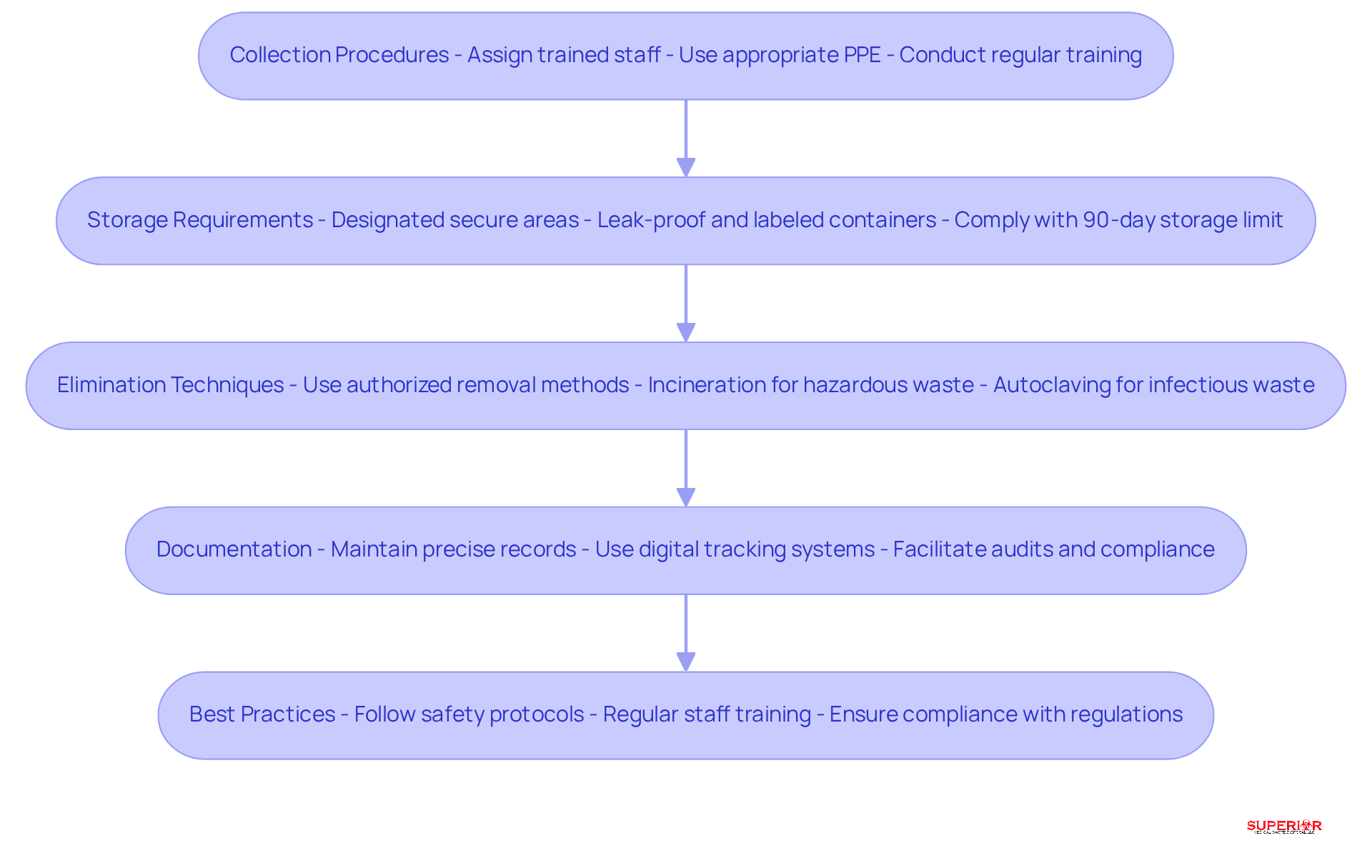
Collection Procedures: Specific staff members should be assigned to gather medical materials. These individuals must be trained in safe handling practices and equipped with appropriate personal protective equipment (PPE). Regular training sessions are essential to maintain compliance and reduce risks associated with mishandling.
Storage Requirements: Medical refuse must be stored in designated, secure areas that are leak-proof and clearly labeled. Facilities must comply with revised regulations, including the 90-day storage limit for biohazard materials in Michigan. It is crucial to maintain items at suitable temperatures and conditions to prevent degradation or contamination.
[Elimination Techniques](https://www.superiorwastedisposal.com/?p=1025): Authorized removal techniques should be utilized based on the category of medical refuse. For instance, incineration is appropriate for hazardous materials, while autoclaving is effective for infectious substances. At [Superior Medical Refuse Management](https://superiorwastedisposal.com), we autoclave and shred biohazard materials to reduce their volume by 70% before placement in a sanitary landfill, ensuring compliance with local regulations.
Documentation: Precise records of refuse generation, storage, and disposal must be maintained to demonstrate compliance with regulations and facilitate audits. Utilizing can enhance accountability and streamline the documentation process, reducing human error and ensuring adherence to safety protocols.
By following these best practices, healthcare facilities can effectively ensure the management of medical waste, safeguarding the health of staff and patients while meeting regulatory requirements.
Conclusion
Effective management of medical waste is essential for ensuring safety and compliance in healthcare settings. By accurately categorizing medical waste, adhering to regulatory frameworks, and implementing best practices for waste segregation, collection, storage, and disposal, healthcare facilities can significantly reduce the risks associated with hazardous refuse. This comprehensive approach not only safeguards healthcare workers and patients but also promotes environmental sustainability.
Key insights emphasize the necessity of precise categorization of medical waste to facilitate safe disposal practices. Effective waste segregation strategies, including color-coded containers and thorough staff training, are crucial for enhancing compliance and safety. Additionally, establishing robust procedures for collection, storage, and disposal is vital for demonstrating adherence to regulations and protecting public health.
The importance of effective medical waste management cannot be overstated. As healthcare facilities strive to enhance their practices, adopting these best practices will foster safer environments and more responsible waste handling. It is imperative for all stakeholders in the healthcare sector to prioritize these strategies, ensuring that medical waste management is both effective and compliant with evolving regulations.
Frequently Asked Questions
What is medical waste?
Medical waste refers to any byproduct generated in healthcare settings that may be contaminated by blood, bodily fluids, or other potentially infectious materials.
Why is categorizing medical waste important?
Accurately categorizing medical waste is essential for ensuring safe and compliant disposal practices.
What are the primary categories of medical waste?
The primary categories of medical waste include Infectious Waste, Sharps Waste, Pathological Waste, Pharmaceutical Waste, and Hazardous Materials.
What is Infectious Waste?
Infectious Waste includes materials that pose a risk of infection, such as cultures, blood products, and contaminated items. Approximately 15% of healthcare refuse is classified as hazardous, which can be infectious, toxic, or radioactive.
What constitutes Sharps Waste?
Sharps Waste consists of items that can puncture or cut skin, including needles, blades, and broken glass. These items can lead to serious diseases, such as HIV and hepatitis, highlighting the need for stringent management practices.
What is Pathological Waste?
Pathological Waste includes human tissues, organs, and body parts discarded after surgical procedures or autopsies. Proper management and disposal are crucial to mitigate health risks associated with this waste.
How should Pharmaceutical Waste be handled?
Expired or unused medications require special handling and disposal to prevent environmental contamination and public health risks. Services such as stock management and take-back agreements with suppliers help minimize pharmaceutical byproducts.
What are Hazardous Materials in medical waste?
Hazardous Materials include substances that pose risks to human health or the environment, such as chemical substances and certain pharmaceuticals. Proper handling is essential to prevent environmental contamination and health risks.
What role does proper classification of healthcare refuse play in public health?
Proper classification and management of medical waste ensure adherence to regulatory standards and safeguard public health.
