Introduction
Infectious waste disposal in healthcare facilities is not just a procedural necessity; it is a critical component of public health that protects both healthcare workers and the community. Given the alarming statistics surrounding infection transmission linked to improper waste management, the stakes have never been higher. This article explores essential best practices for managing infectious waste, emphasizing:
- Innovative methods
- Regulatory compliance
- The crucial role of staff training
How can healthcare facilities ensure their waste disposal practices not only meet regulatory standards but also safeguard the health of everyone involved?
Define Infectious Waste and Its Importance in Healthcare
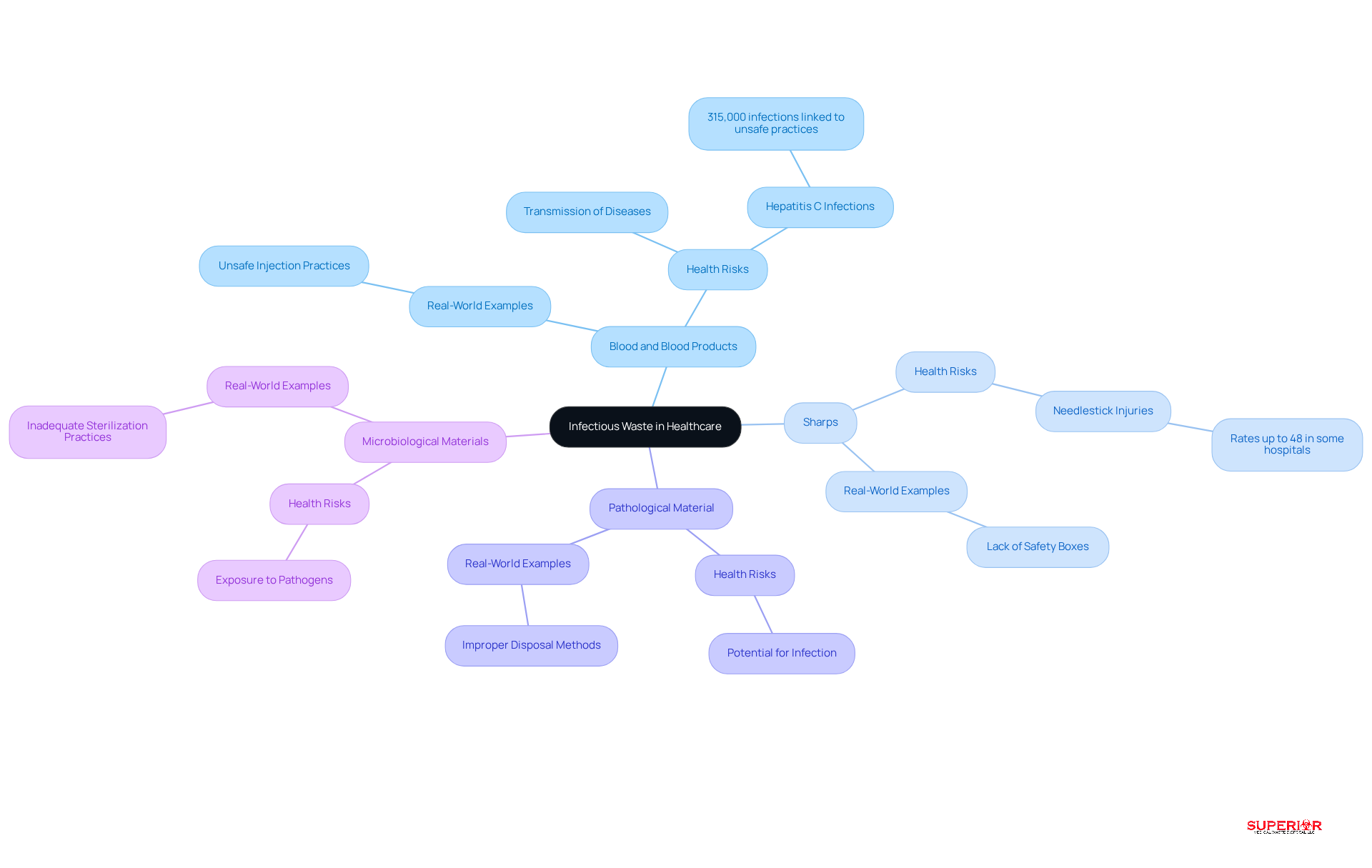
Infectious materials, often termed medical or biohazardous, consist of items contaminated with pathogens capable of causing illness in humans. This category encompasses:
- Blood and blood products: Any waste containing human blood or its components.
- : Needles, blades, and other items that can puncture the skin.
- Pathological material: Tissues, organs, and body parts removed during surgical procedures or autopsies.
- Microbiological materials: Cultures and stocks of infectious agents.
Defining and managing is essential due to its , posing significant , patients, and the broader community. For example, unsafe injection practices have been linked to over 315,000 hepatitis C infections in a single year, highlighting the severe consequences of inadequate waste management.
Real-world examples underscore the necessity of . In numerous healthcare facilities, the absence of has resulted in increased needlestick injuries among staff, with some hospitals reporting rates as high as 48%. Such incidents not only jeopardize healthcare personnel but also elevate the risk of disease transmission within the community.
Healthcare professionals stress the importance of stringent protocols for . One provider noted, “The key to effective management of is the .” This statement underscores the need for and awareness initiatives to ensure that all personnel understand the significance of appropriate refuse management.
The repercussions of improper infectious waste disposal extend beyond immediate health risks; they can lead to long-term public health challenges. , threatening water sources and soil quality, which can have extensive effects on community health. Therefore, implementing robust refuse management practices is not merely a regulatory requirement but a crucial element in safeguarding public health.
Implement Safe Disposal Methods for Infectious Waste
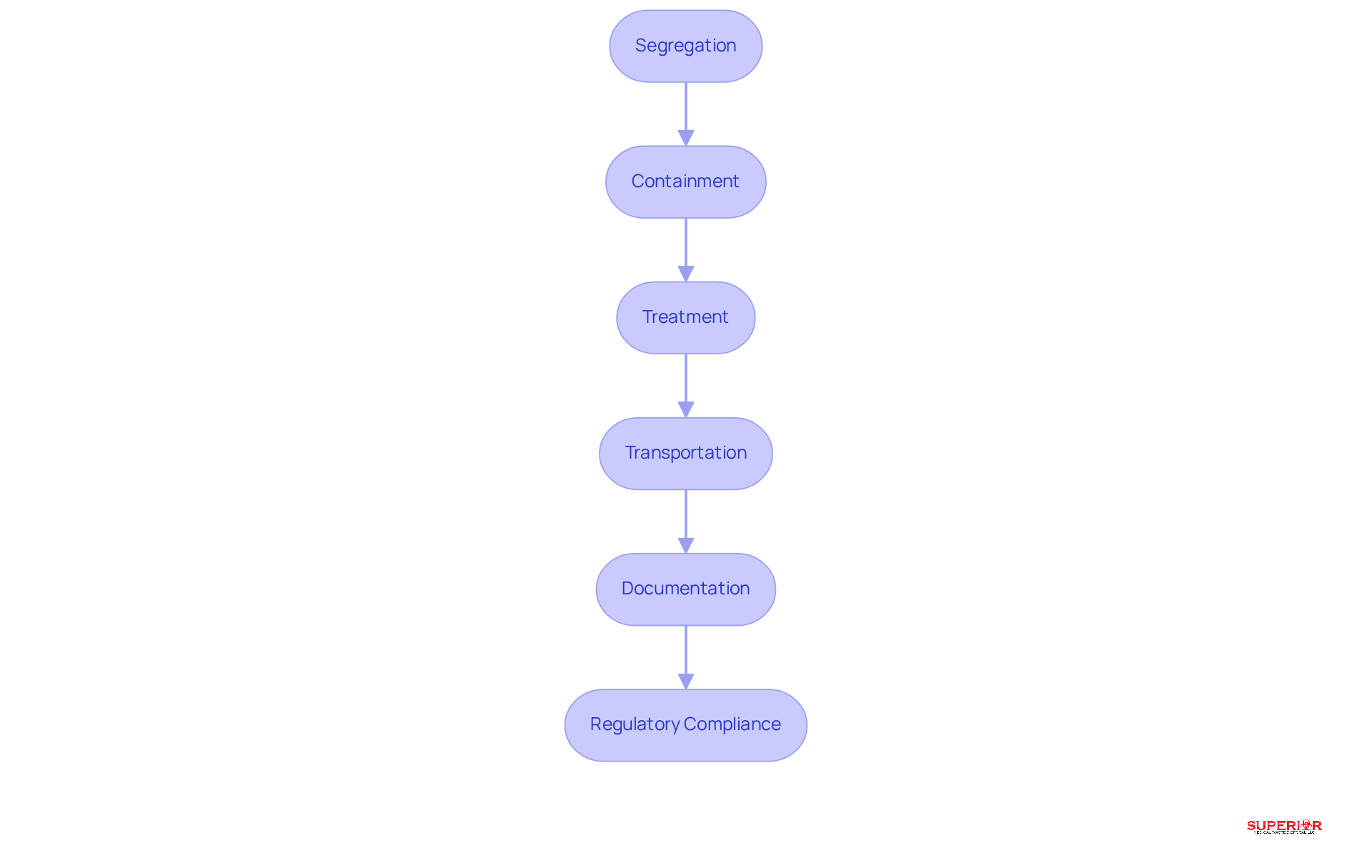
To ensure the safe disposal of infectious waste, healthcare facilities should adopt several key practices:
-
Segregation: Clearly separating infectious materials from general refuse at the point of generation is essential. Implementing facilitates proper sorting and enhances compliance with safety protocols for .
-
Containment: Utilize specifically designed for sharps and biohazardous materials. To ensure safe handling and prevent accidental exposure, all containers must be clearly labeled with biohazard symbols for .
-
Treatment: Employ to effectively neutralize infectious waste:
- Incineration: This method is highly effective for destroying pathogens and significantly reducing waste volume.
- Autoclaving: A steam sterilization method that ensures infectious waste disposal by decontaminating refuse prior to removal, thereby ensuring safety and adherence to health regulations. At , our biohazard material is autoclaved and shredded to reduce volume by 70% before going to the landfill, aligning with best practices for efficient disposal processes.
-
Transportation: Ensure that refuse is conveyed in to prevent leaks or spills during transit. This step is crucial for maintaining .
-
Documentation: Keep , treatment, and removal. This documentation is essential for adherence to regulatory requirements related to infectious waste disposal and facilitates audits, ensuring accountability in management practices.
-
Regulatory compliance: Always consult your local environmental authority for guidance on regulations and laws concerning infectious waste disposal and and removal. This step is vital for ensuring compliance with state-specific requirements.
Understand Regulatory Compliance for Infectious Waste Management
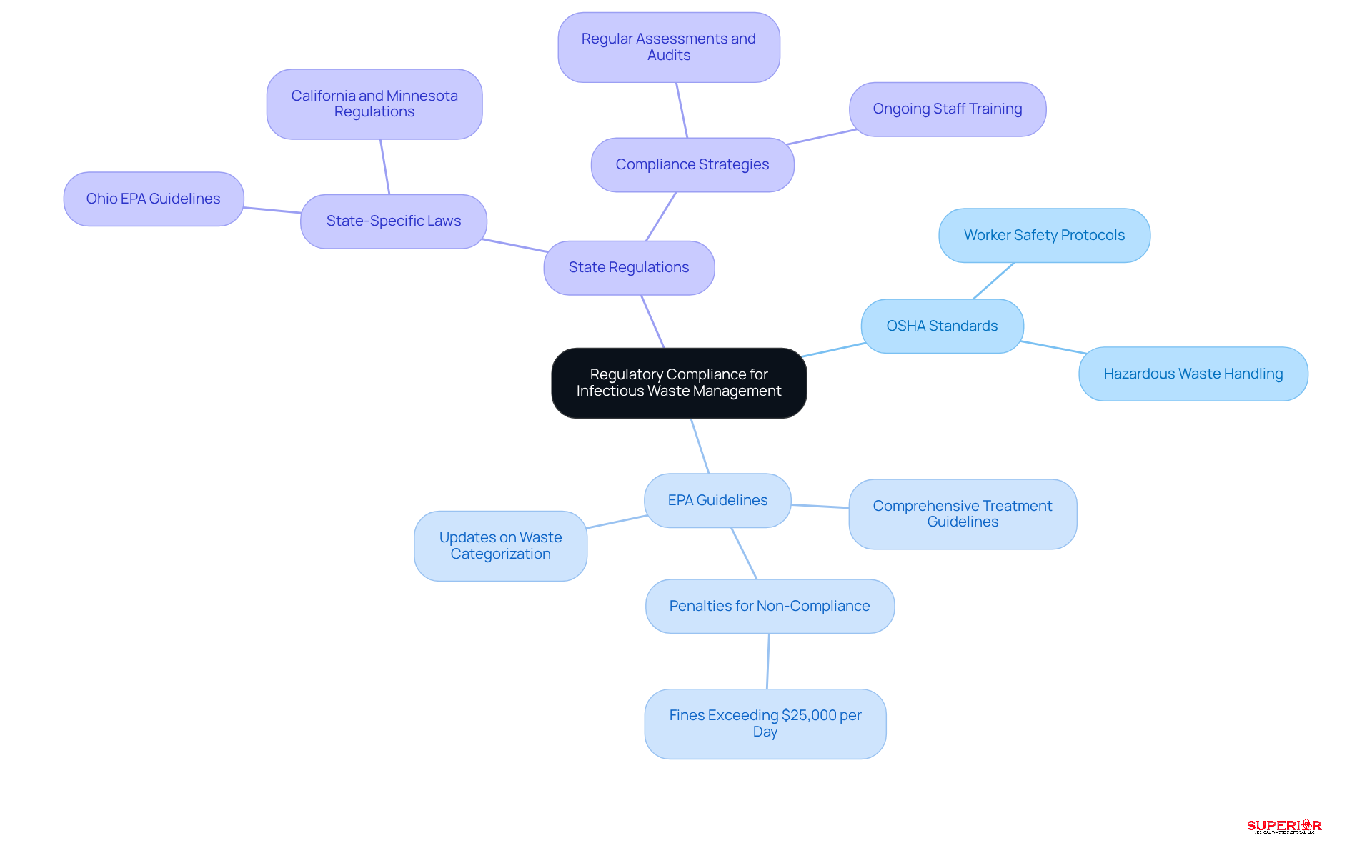
Healthcare facilities must adhere to a variety of regulations concerning the management of infectious waste. These regulations include:
- : The Occupational Safety and Health Administration enforces strict protocols for the safe handling and disposal of hazardous waste, ensuring that workers are protected from potential exposure.
- The outlines comprehensive guidelines for the treatment and of medical refuse. These guidelines underscore the critical need for , such as , to reduce environmental contamination risks. Recent updates to EPA regulations highlight the importance of proper categorization and treatment methods for infectious waste disposal, with penalties for non-compliance potentially exceeding $25,000 per day. is committed to adhering to these regulations for infectious waste disposal, ensuring that all refuse is managed according to state and federal guidelines.
- : Each state has specific laws regarding , which can vary significantly. For instance, in Ohio, the Ohio EPA oversees the production, storage, and treatment of medical refuse, advising that all infectious waste disposal should involve sending infectious materials to a commercial treatment center. Superior Medical Refuse Disposal collaborates with a commercial autoclaving site for infectious waste disposal to process all medical refuse in Ohio, ensuring . States like California and Minnesota impose stringent criteria for segregation and treatment techniques in infectious waste disposal, necessitating that organizations stay informed about local regulations to ensure adherence.
To maintain compliance, healthcare organizations should conduct , perform audits to identify potential compliance gaps, and provide ongoing training for personnel on current regulatory standards. This proactive approach not only protects public health but also enhances operational efficiency and environmental stewardship, backed by the expertise and extensive partnerships of .
Provide Training for Staff on Infectious Waste Handling
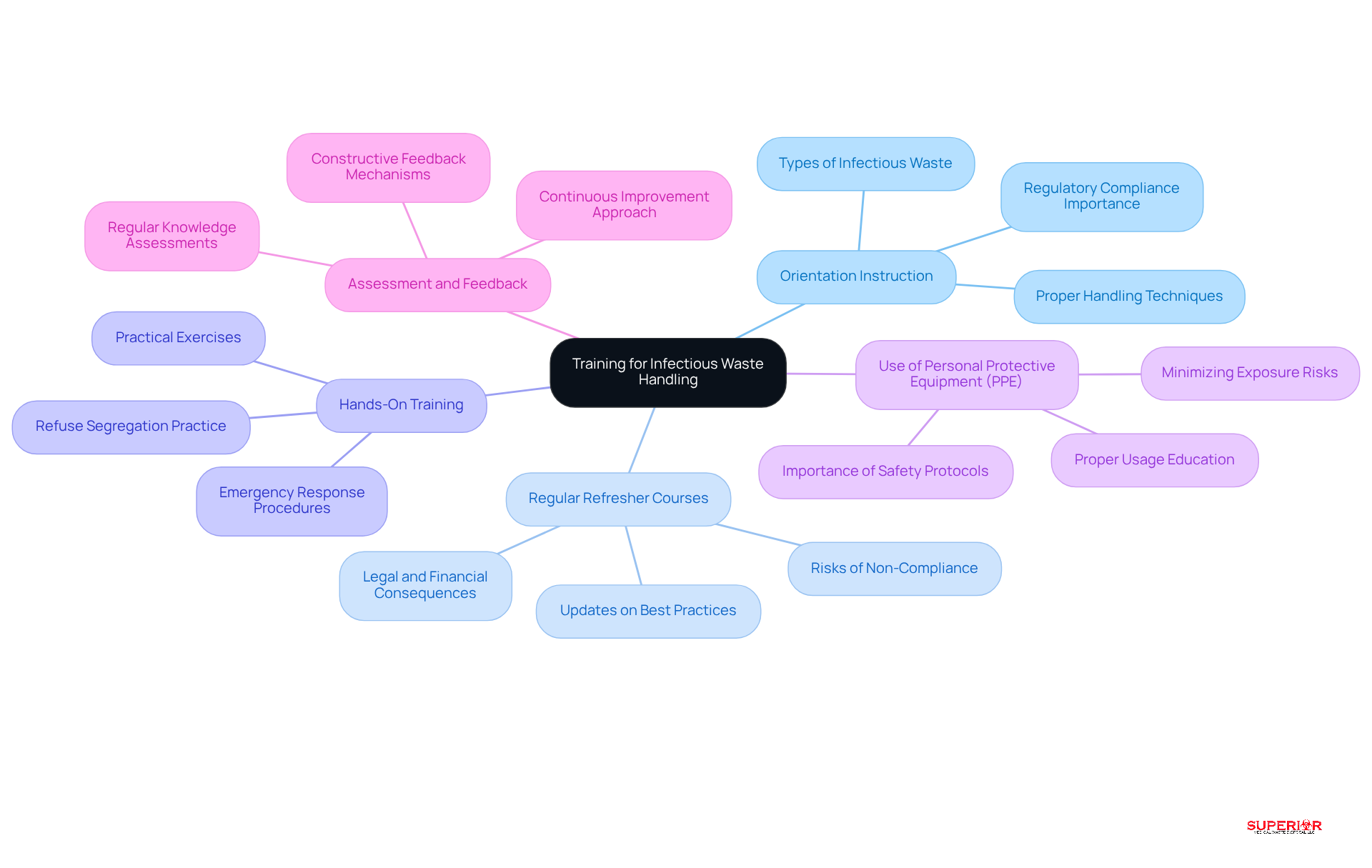
To ensure the safe handling of infectious waste, healthcare facilities must implement comprehensive training programs that encompass several key elements:
- Orientation Instruction: New employees should receive thorough education on the types of infectious waste, , and the , particularly the guidelines established by the Ohio EPA. This foundational knowledge is crucial for fostering a culture of safety from the outset.
- : Ongoing educational sessions are essential to keep staff updated on best practices and regulatory changes. Statistics indicate that a significant percentage of healthcare facilities do not provide , which can lead to outdated practices and increased risks of non-compliance. Insufficient preparation can result in legal, financial, and reputational harm for organizations.
- : Practical exercises are vital for enabling staff to practice refuse segregation, container usage, and emergency response procedures. Engaging in practical exercises enhances staff confidence and skills in handling infectious materials efficiently. Case studies have shown that facilities with robust practical instruction programs experience fewer occurrences of improper refuse disposal.
- Use of : Educating staff on the , including gloves, masks, and gowns, is critical to minimizing exposure risks. Adequate instruction on PPE not only protects employees but also underscores the importance of safety protocols in disposal. Insights from healthcare education professionals highlight that effective PPE instruction is essential for reducing workplace injuries.
- : Regular assessments of staff knowledge, coupled with constructive feedback, are necessary to reinforce learning and address any gaps in understanding. This continuous improvement approach ensures that staff remain vigilant and compliant with safety standards. Institutions that prioritize mechanisms report higher compliance rates and improved safety outcomes.
By emphasizing these training elements, healthcare organizations can significantly reduce the hazards associated with improper and enhance overall workplace safety. Additionally, partnering with a reliable service provider like ensures that facilities comply with for , including preferred treatment methods for regulated medical waste, such as autoclaving.
Conclusion
Effective management of infectious waste in healthcare facilities is essential for protecting public health and ensuring the safety of healthcare workers. Understanding the various types of infectious waste and implementing strict disposal protocols allows healthcare organizations to significantly mitigate the risks associated with improper waste handling. By integrating comprehensive training programs and adhering to regulatory compliance, these organizations not only foster a culture of safety but also enhance operational efficiency within healthcare settings.
Key practices include:
- The segregation of waste at the point of generation
- The use of appropriate containment methods
- The application of effective treatment techniques such as incineration and autoclaving
Additionally, maintaining meticulous documentation and ensuring compliance with local, state, and federal regulations are crucial steps in responsibly managing infectious waste. Regular staff training and practical exercises empower healthcare workers to handle infectious materials safely and effectively.
Ultimately, the responsibility of infectious waste disposal extends beyond mere regulatory compliance; it is a critical component of public health protection. Healthcare facilities are encouraged to adopt these best practices and prioritize ongoing education and training for their staff. By doing so, they not only mitigate health risks but also contribute to a safer and healthier community. Embracing innovative technologies and strategies in waste management will further enhance the effectiveness of these efforts, ensuring that healthcare providers can meet the challenges of waste disposal in an ever-evolving landscape.
Frequently Asked Questions
What is infectious waste?
Infectious waste, also known as medical or biohazardous waste, consists of items contaminated with pathogens that can cause illness in humans. This includes blood and blood products, sharps, pathological material, and microbiological materials.
Why is managing infectious waste important in healthcare?
Managing infectious waste is crucial because improper disposal can transmit infections, posing significant health risks to healthcare workers, patients, and the community. For instance, unsafe injection practices have led to over 315,000 hepatitis C infections in a single year.
What types of materials are classified as infectious waste?
Infectious waste includes blood and blood products, sharps (like needles and blades), pathological material (such as tissues and organs), and microbiological materials (cultures and stocks of infectious agents).
What are the consequences of inadequate infectious waste management?
Inadequate management can lead to increased needlestick injuries among healthcare staff and heightened risk of disease transmission in the community. Additionally, contaminated materials can harm the environment, affecting water sources and soil quality.
What do healthcare professionals recommend for infectious waste disposal?
Healthcare professionals emphasize the importance of stringent protocols for infectious waste disposal, particularly the segregation of waste at the point of generation. Comprehensive training and awareness initiatives are essential for ensuring proper waste management practices.
How does improper disposal of infectious waste affect public health?
Improper disposal can lead to immediate health risks and long-term public health challenges, as contaminated materials may leach into the environment, threatening community health by contaminating water and soil.
List of Sources
- Define Infectious Waste and Its Importance in Healthcare
- Managing 5.9 Million Tons Annually for a Sustainable Future – The Growing Challenge of Medical Waste Disposal (https://medprodisposal.com/managing-5-9-million-tons-annually-for-a-sustainable-future-the-growing-challenge-of-medical-waste-disposal)
- Health-care waste (https://who.int/news-room/fact-sheets/detail/health-care-waste)
- Healthcare Waste—A Serious Problem for Global Health – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9858835)
- mdpi.com (https://mdpi.com/2076-3298/5/8/89)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC12598056)
- Implement Safe Disposal Methods for Infectious Waste
- The Future of Waste Management in Hospitals: Trends to Watch (https://danielshealth.com/knowledge-center/future-of-waste-management)
- Best Practices for Containing and Disposing of Infectious Waste (https://oshaoutreachcourses.com/blog/infectious-waste-disposal-osha)
- What Healthcare Must Know About PHI Disposal & Medical Waste in 2026 (https://appliedinnovation.com/health-services/what-healthcare-must-know-about-phi-disposal-medical-waste-in-2026)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- How U.S. hospitals cleaned up their toxic trash (https://pbs.org/newshour/world/agents-for-change/how-u-s-hospitals-cleaned-up-their-toxic-trash)
- Understand Regulatory Compliance for Infectious Waste Management
- Regulatory Updates in Medical Waste Management | ASMAI (https://asiwaste.com/medical-waste/regulatory-updates-in-medical-waste-management)
- EPA Final Rule on Pharmaceutical Waste | Compliance Guide (https://securewaste.net/epa-final-rule-on-hazardous-waste-pharmaceuticals)
- Medical Waste | US EPA (https://epa.gov/rcra/medical-waste)
- Medical Waste Disposal Regulations (2026): A State-by-State Compliance Checklist (https://medprodisposal.com/medical-waste-disposal-regulations-2026-state-by-state-checklist)
- Provide Training for Staff on Infectious Waste Handling
- medprodisposal.com (https://medprodisposal.com/medical-waste-training-program-for-faculty)
- medsharps.com (https://medsharps.com/blog/the-importance-of-training-staff-on-regulated-medical-waste-a-professional-guide)
- Expert Guide For Medical Waste Management In Healthcare 2026 (https://securewaste.net/professional-medical-waste-management-for-healthcare-facilities)
- Best Practices for Containing and Disposing of Infectious Waste (https://oshaoutreachcourses.com/blog/infectious-waste-disposal-osha)
- Bio-MED Regulated Waste Solutions (https://getbiomed.com/hazardous-waste/the-importance-of-staff-training-in-hazardous-waste-management)
