Introduction
Effective medical waste management is crucial for healthcare facilities. Improper disposal can pose significant health risks and environmental hazards. This article explores ten essential examples of medical waste, emphasizing the importance of understanding and managing each type effectively. Readers will learn about best practices, regulatory compliance requirements, and innovative strategies that can enhance safety and efficiency in waste disposal.
How can healthcare facilities ensure compliance while proactively mitigating the risks associated with medical waste?
Sharps Waste: Understanding the Risks and Management Strategies
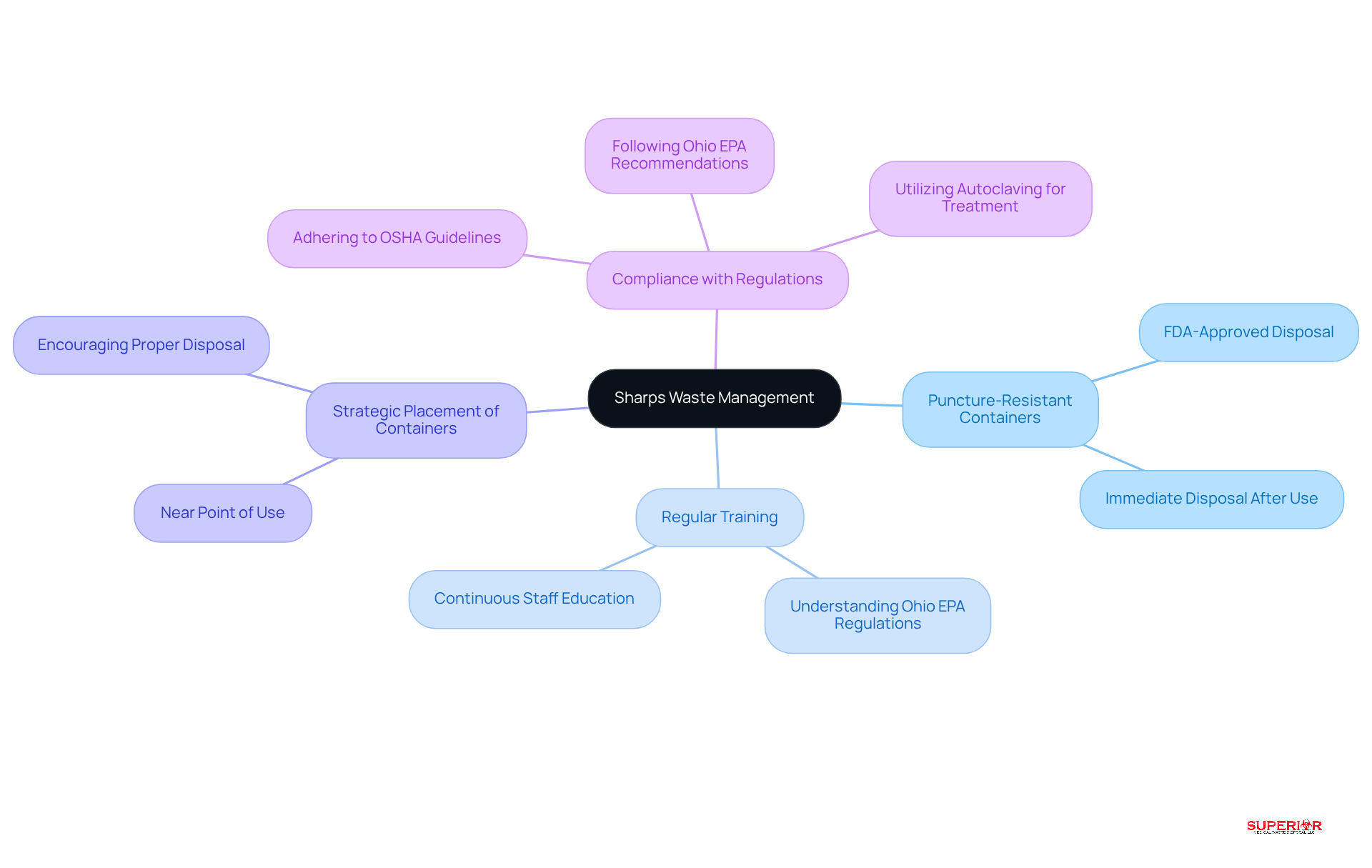
Sharps materials, such as needles, blades, and other sharp objects, pose significant risks of injury and infection transmission. Effective management strategies are essential to ensure safety in healthcare settings.
- Use of Puncture-Resistant Containers: It is crucial to dispose of sharps in FDA-approved, puncture-resistant containers immediately after use. This practice minimizes the risk of accidental injuries and ensures safe handling.
- Regular Training: Continuous training for staff on the handling and disposal of sharps is vital. This training should include an understanding of regarding medical refuse management, which helps to minimize risks associated with sharps.
- Strategic Placement of Containers: Positioning sharps containers near the point of use encourages proper disposal and significantly reduces the risk of needlestick injuries. Accessibility is key to promoting safe practices.
- Compliance with Regulations: Adhering to OSHA guidelines for sharps management and following Ohio EPA recommendations for the treatment of medical refuse is essential for ensuring safety and legal compliance. At [Superior Medical Waste Treatment](https://superiorwastedisposal.com), we employ autoclaving as a preferred method for treating sharps materials, effectively disinfecting them and preparing them for safe elimination.
Biohazardous Materials: Identification and Safe Disposal Practices
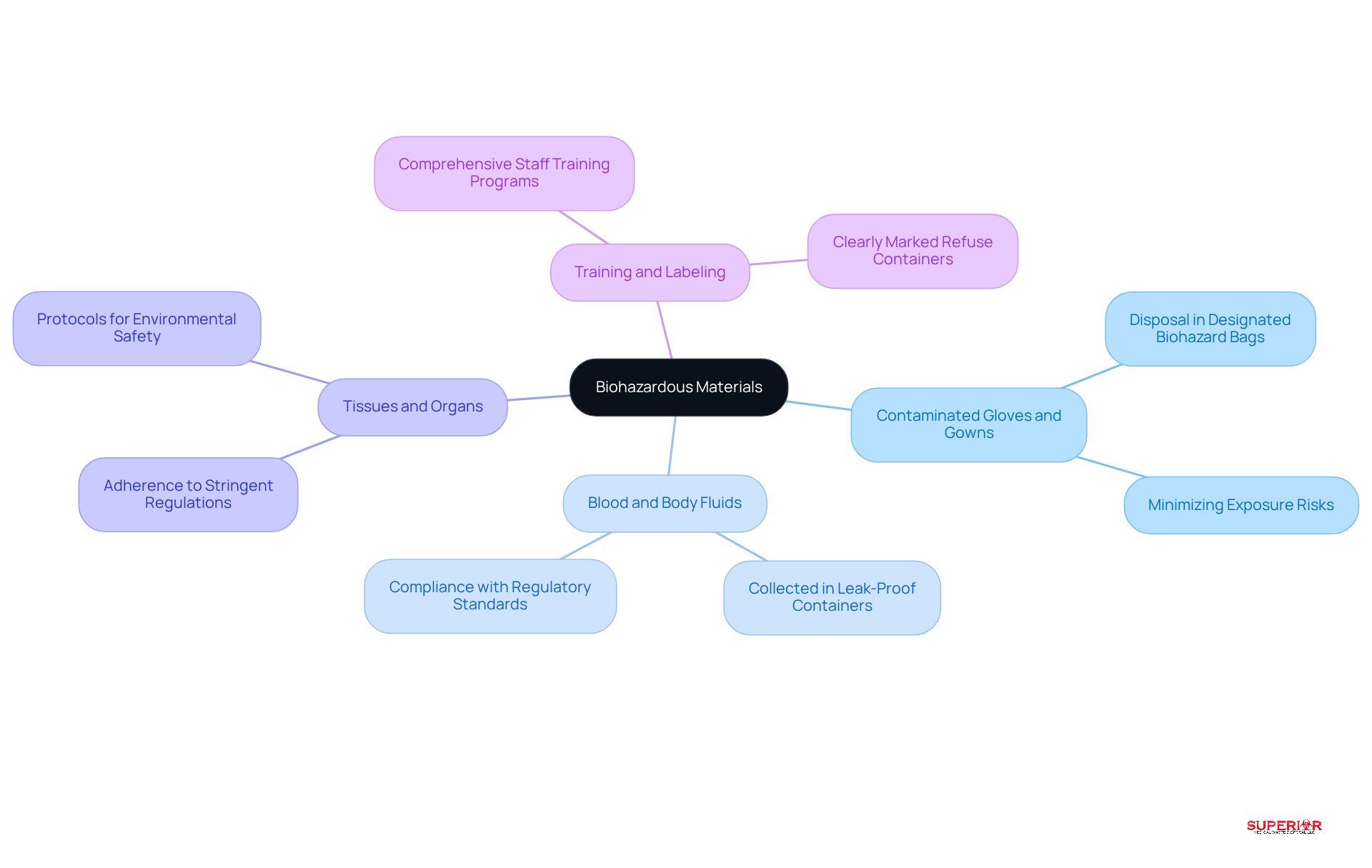
Biohazardous materials encompass any refuse that poses a risk of infection, necessitating careful handling and removal. Key examples include:
- Contaminated Gloves and Gowns: These items must be disposed of in designated biohazard bags to minimize exposure risks. Proper disposal practices are crucial; improper handling can lead to contamination and health hazards.
- Blood and body fluids are critical medical waste examples that should be collected and disposed of in leak-proof containers specifically labeled as biohazardous. This practice ensures safety and complies with .
- The disposal of tissues and organs, as medical waste examples, must adhere to stringent regulations to prevent environmental contamination and public health risks. Facilities should implement protocols that align with local and federal guidelines.
- Training and Labeling: Comprehensive training programs for staff on identifying biohazardous materials are vital. Clearly marked refuse containers aid in upholding regulations and enhance safety within the premises.
In 2026, medical centers are expected to emphasize biohazard training programs, with a significant proportion of organizations adopting these initiatives to enhance safety and compliance. Infection control specialists assert that effective management of biohazardous materials is crucial in reducing healthcare-associated infections (HAIs), which correlate strongly with healthcare hazardous substances (HHCW) generation. By implementing effective methods for handling contaminated materials, such as gloves and gowns, establishments can significantly reduce dangers linked to improper handling.
Pharmaceutical Waste: Best Practices for Safe Disposal
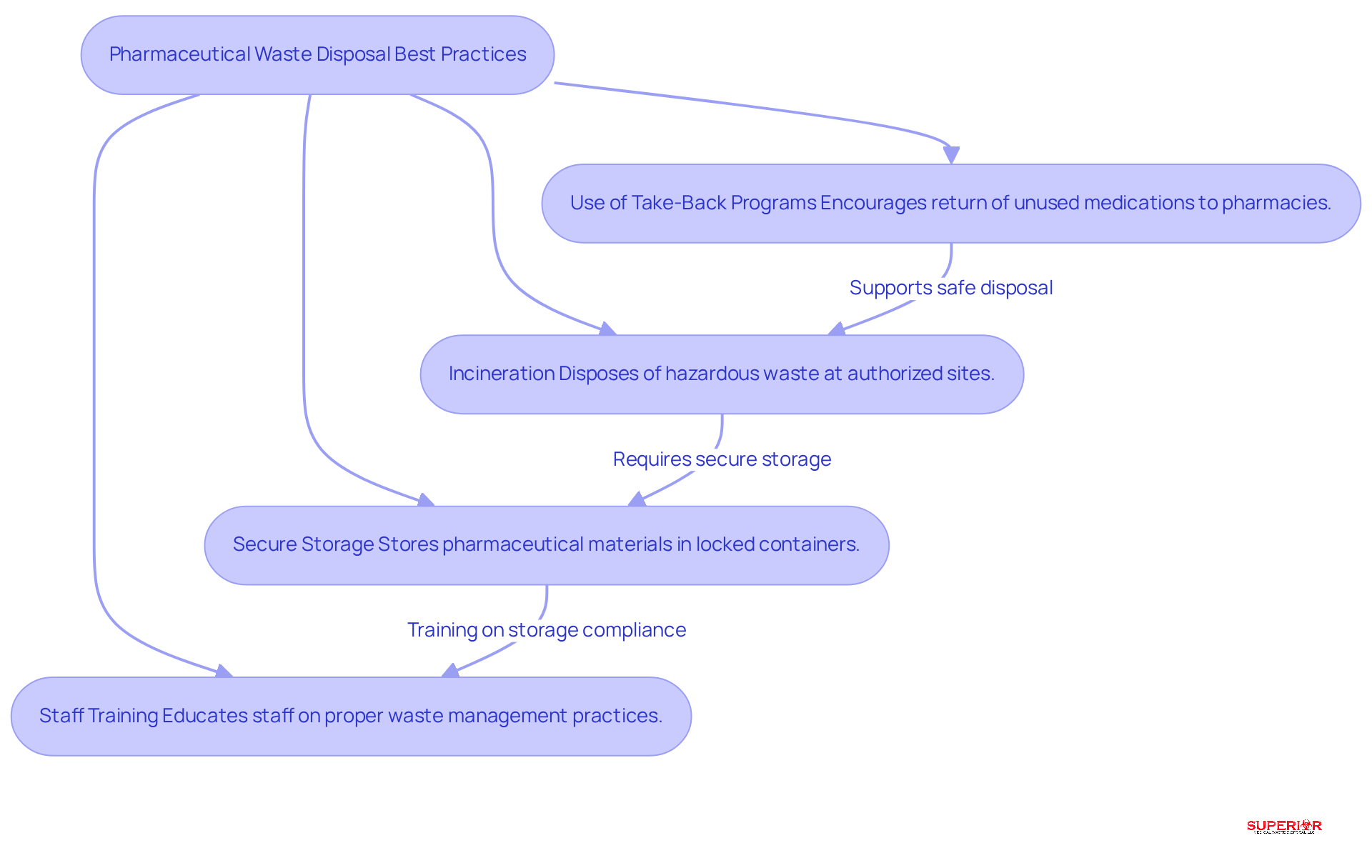
Pharmaceutical waste, which encompasses expired or unused medications, presents significant environmental risks if not disposed of properly. To address these concerns, healthcare facilities in Traverse City should implement best practices for safe disposal:
- Use of Take-Back Programs: These programs are crucial for encouraging patients to return unused medications to pharmacies or designated take-back locations. They facilitate safe disposal and help mitigate the risk of drug misuse, particularly among vulnerable populations such as seniors, who often retain leftover medications. Recent studies reveal that nearly 130 Americans die from opioid overdoses daily, highlighting the urgent need for effective medication take-back initiatives.
- Incineration: Hazardous pharmaceutical waste should be disposed of through incineration at authorized sites. This method effectively eliminates harmful substances and prevents environmental contamination. Superior Medical Waste Disposal collaborates with licensed facilities to ensure compliance with local regulations, including those specific to Traverse City.
- Secure Storage: Until disposal, pharmaceutical materials must be stored in locked containers to prevent unauthorized access. This practice is essential for maintaining compliance with regulations and ensuring safety within healthcare settings. In Michigan, facilities have up to 90 days to store biohazard materials, underscoring the importance of secure storage practices.
- Staff Training: Regular training for staff on the importance of proper pharmaceutical waste management and the associated regulations is vital. Training and fosters a culture of safety and responsibility. Effective communication strategies can significantly improve participation in drug collection programs.
A case study examining practices at a major University Hospital illustrates the growing awareness of trace amounts of discarded pharmaceuticals in waterways and the necessity for effective management to prevent environmental contamination. By adopting these optimal methods and utilizing resources like Superior Medical Waste Disposal’s services, including sharps disposal and document shredding, medical institutions can significantly reduce the environmental impact of pharmaceutical waste and contribute to public health safety.
Hazardous Waste: Types and Compliance Guidelines
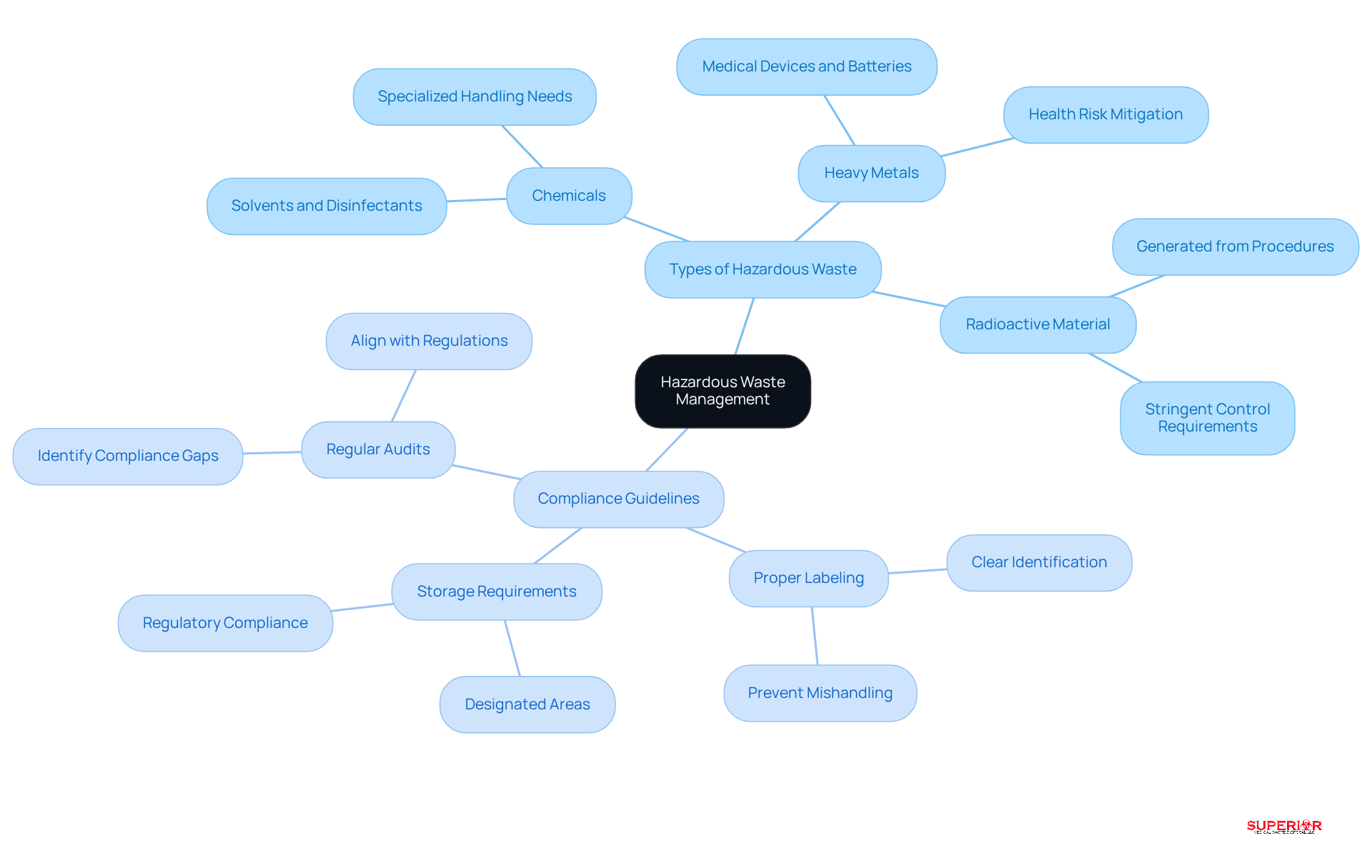
Hazardous materials include substances that are toxic, flammable, or reactive, presenting significant risks if not managed properly. In healthcare facilities, key categories of hazardous waste encompass:
- Chemicals: This category includes solvents, disinfectants, and other substances that necessitate specialized handling to prevent exposure and environmental contamination.
- Heavy Metals: Found in certain medical devices and batteries, these substances require careful handling to mitigate health risks.
- Radioactive Material: Generated from diagnostic and treatment procedures, this type of material demands stringent controls to ensure safety.
Compliance guidelines for hazardous waste management are crucial for maintaining safety and adhering to regulations:
- Proper Labeling: All hazardous waste must be clearly labeled to prevent mishandling and ensure accurate identification during disposal.
- Storage Requirements: Hazardous materials should be stored in designated areas that comply with regulatory standards, including impermeable floors and restricted access to minimize risks.
- Regular Audits: Conducting audits is essential for identifying compliance gaps and ensuring that hazardous material management practices align with current regulations.
As we approach 2026, medical establishments must prepare for evolving compliance expectations, particularly as states implement stricter regulations regarding hazardous materials. Effective compliance strategies involve maintaining thorough records of disposal management practices, conducting internal audits every three months, and ensuring that all personnel receive appropriate training on hazardous material handling. By adopting these strategies, healthcare facilities can effectively mitigate risks associated with hazardous materials while enhancing their operational efficiency.
Anatomical Waste: Handling and Disposal Requirements
Anatomical byproducts, which include human tissues, organs, and body parts, require stringent handling and disposal protocols to mitigate health risks and ensure compliance with regulations. Key practices for managing anatomical waste include the following:
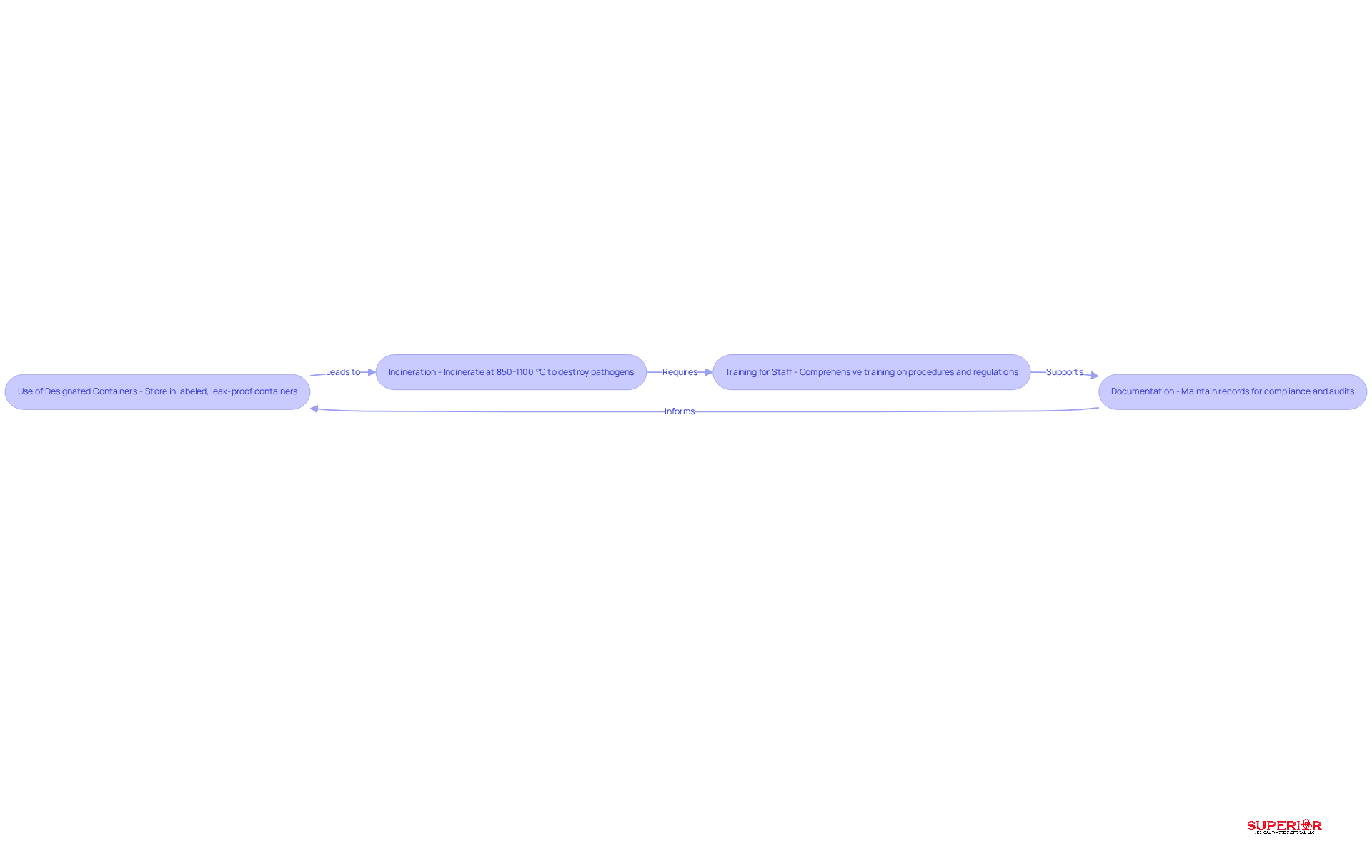
- Use of Designated Containers: It is essential to store anatomical waste in clearly labeled, leak-proof containers. This practice prevents leaks and contamination, safeguarding both personnel and the environment.
- Incineration: The majority of anatomical material must be incinerated at [high temperatures ranging from 850 to 1100 °C](https://pmc.ncbi.nlm.nih.gov/articles/PMC9858835). This process ensures the complete destruction of pathogens and adherence to international emission standards. Additionally, incineration effectively reduces the volume of refuse and minimizes environmental impact.
- Training for Staff: Comprehensive training for all personnel involved in handling anatomical materials is vital. This training by ensuring that staff are well-versed in proper procedures and regulatory requirements.
- Documentation: Maintaining precise records of anatomical refuse management is crucial for regulatory compliance and audit preparedness. Facilities should ensure that manifests and treatment certificates are easily accessible and consistently updated.
Pathological Waste: Identification and Safe Management
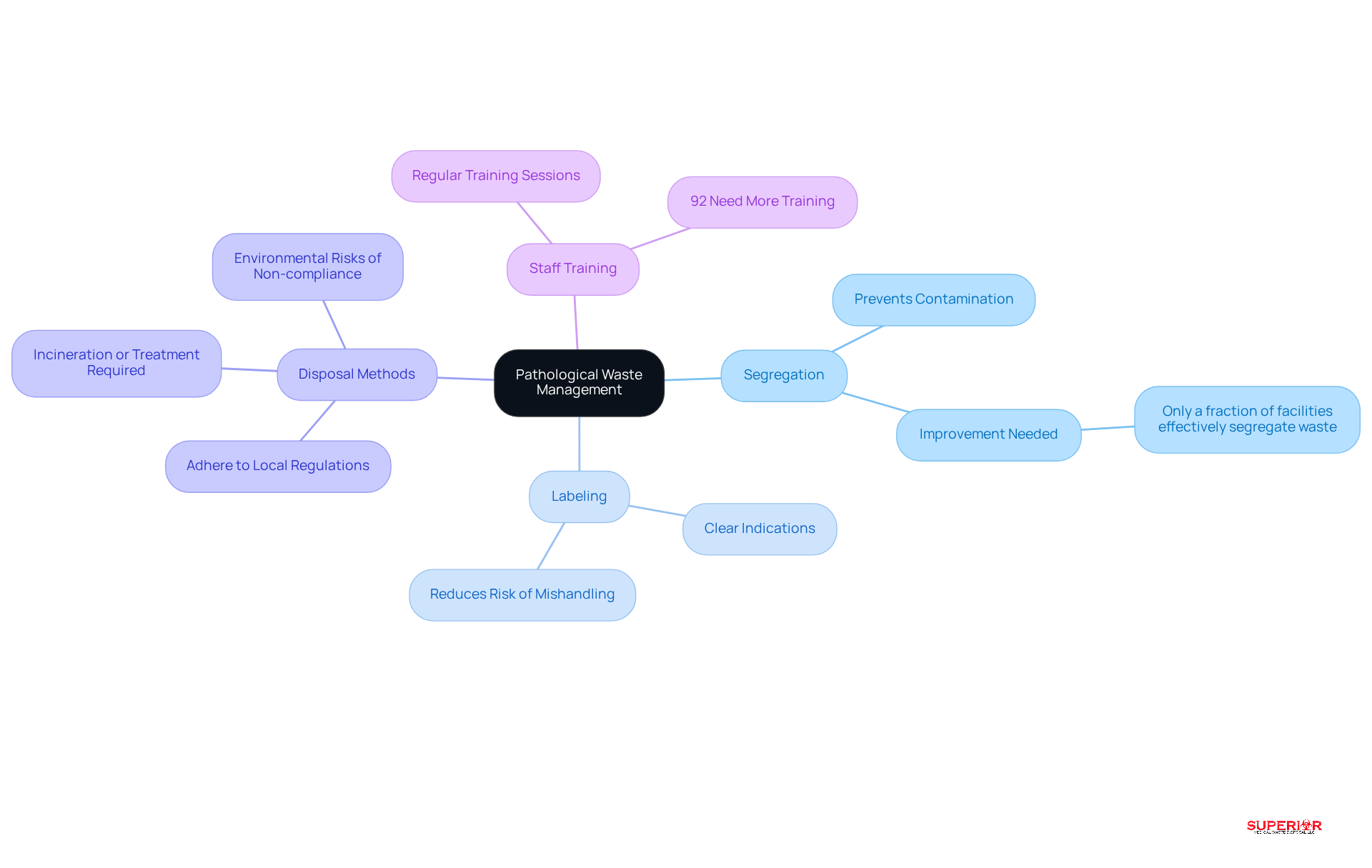
Pathological material includes identifiable human tissues, organs, and fluids, which require stringent management practices to ensure safety and compliance. Effective management is crucial for minimizing risks associated with this type of waste.
- Segregation is essential; keeping pathological waste separate from other waste types prevents contamination and ensures proper disposal. Research indicates that only a fraction of healthcare facilities effectively segregate this waste, highlighting the need for improved practices.
- Labeling is another critical aspect. Clear labels indicating that the material is pathological assist in proper management and disposal, thereby reducing the risk of mishandling.
- Disposal methods must adhere to local regulations, with incineration or treatment being necessary for pathological materials. Non-compliance poses significant environmental and health risks, as improper disposal can contaminate soil and water supplies.
- Staff training is vital. Regular training sessions on the identification and handling of pathological materials are necessary. Studies show that 92% of medical professionals feel they require additional training to ensure safe working environments, underscoring the importance of in waste management.
Established segregation methods in various medical environments demonstrate that with appropriate protocols and training, organizations can significantly reduce the dangers associated with pathological waste. As the medical landscape evolves, particularly with the rise of home care services, the need for effective disposal management strategies becomes increasingly critical. Ongoing education and a commitment to best practices will ensure that healthcare facilities manage pathological materials safely and responsibly.
Chemical Waste: Types and Disposal Protocols
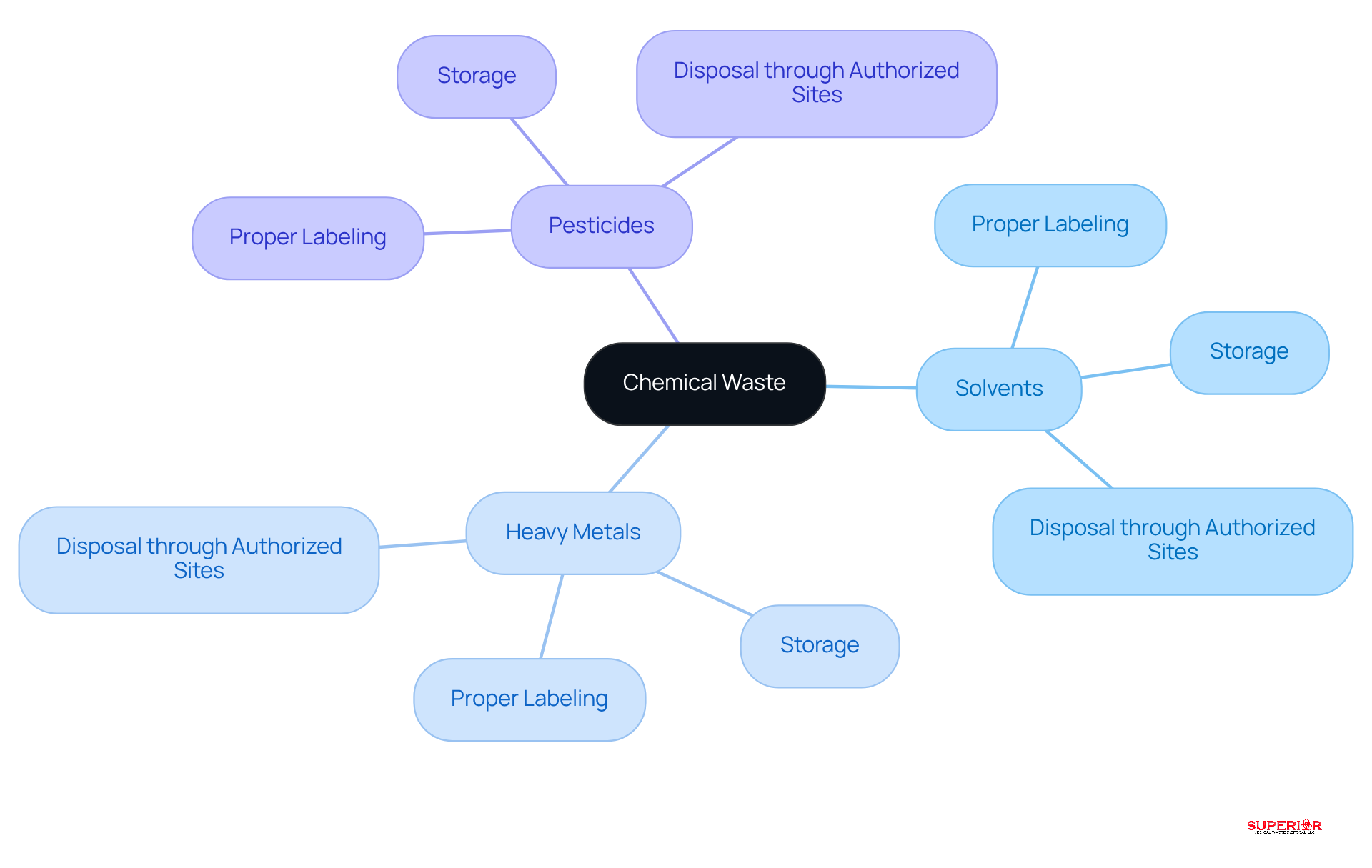
Chemical waste encompasses substances that pose hazards to health or the environment. The primary types include:
- Solvents: Commonly utilized in laboratory settings, these require specific disposal methods to mitigate risks.
- Heavy Metals: Often found in batteries and certain medical devices, these materials necessitate careful handling due to their toxicity.
- Pesticides: Employed in healthcare facilities for pest control, these substances must be managed according to strict regulations.
Disposal protocols for chemical waste are critical and include:
- Proper Labeling: It is essential that all chemical waste is clearly labeled with its contents and associated hazards to ensure safe handling.
- Storage: Chemicals should be stored in designated areas that comply with safety standards. According to Ohio EPA regulations, all hazardous materials, including chemical substances, must be stored in a manner that prevents them from becoming a food source or breeding ground for animals or insects. Furthermore, storage areas must be clearly marked with appropriate warning signs to alert personnel.
- Disposal through Authorized Sites: Chemical refuse must be discarded through licensed hazardous material disposal sites. In Ohio, healthcare facilities are required to adhere to local regulations, which may involve maintaining a certificate of registration and ensuring that refuse is removed every 90 days or less.
Medical Waste Segregation: Importance and Best Practices
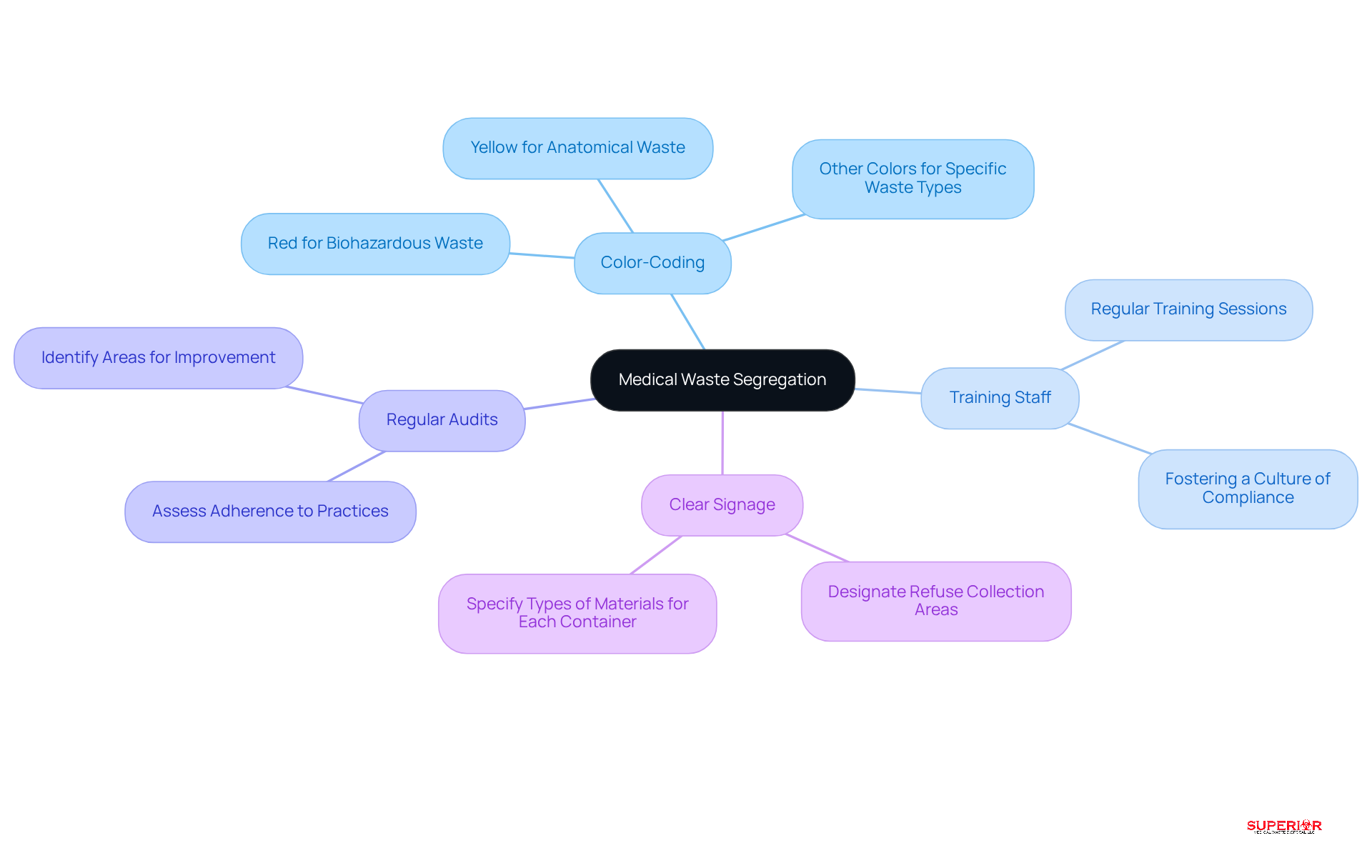
Proper segregation of medical materials is essential for ensuring safety and regulatory compliance. The key best practices include:
- Color-Coding: Implementing a color-coded system for waste containers-red for biohazardous waste, yellow for anatomical waste, and other colors for specific waste types-facilitates quick identification and minimizes the risk of contamination.
- Training Staff: Regular training sessions are crucial for educating staff on the significance of waste segregation and the specific requirements for each waste category. This ongoing education fosters a within the establishment.
- Regular Audits: Routine audits should be performed to assess adherence to segregation practices. These evaluations help identify areas needing improvement and ensure that the facility remains compliant with evolving regulations.
- Clear Signage: Utilizing clear and informative signage to designate refuse collection areas and specify the types of materials for each container reduces confusion and reinforces proper waste management practices.
Recent research indicates that approximately 70% of medical centers have adopted color-coded disposal systems, significantly enhancing their refuse management. Compliance officers emphasize that proper segregation not only mitigates risks but also reduces disposal costs associated with mixed refuse loads. By prioritizing these best practices, medical establishments can improve their operational efficiency while ensuring adherence to state and federal regulations.
Superior Medical Waste Disposal: Comprehensive Solutions for Healthcare Facilities
[Superior Medical Waste Disposal](https://superiorwastedisposal.com) provides a comprehensive range of services designed to meet the diverse needs of medical facilities, ensuring compliance and safety in waste management. The key offerings include:
- Regulated Medical Waste Disposal: This service ensures the safe and compliant disposal of various types of medical waste, which is essential for protecting public health and adhering to strict regulations.
- Sharps Collection and Management: The efficient collection and handling of sharps, such as needles and blades, significantly mitigate the risk of needlestick injuries and infections among healthcare professionals.
- Pharmaceutical Disposal: Secure disposal of pharmaceutical materials is critical for safeguarding public health and the environment, especially in light of the ongoing opioid crisis.
- [Customized Waste Management Plans](https://factmr.com/report/4804/medical-waste-management-market): Tailored solutions are developed to address the specific needs of each facility, ensuring compliance with local and federal regulations while enhancing operational efficiency.
The importance of customized waste management strategies cannot be overstated; they not only improve compliance but also increase satisfaction among medical system administrators. Research indicates that 90% of consumers believe effective medical waste management is vital for delivering optimal patient care, underscoring the essential role these services play in healthcare settings. By prioritizing safety and regulatory compliance, Superior Medical Waste Disposal establishes itself as a reliable partner for healthcare facilities throughout Michigan, Ohio, and Indiana.
Training and Education: Essential for Effective Medical Waste Management
Ongoing training and education are essential for effective medical refuse management. Key components include:
- Regular Training Sessions: Consistent training sessions for all staff on waste management protocols and compliance requirements are crucial. Research indicates that regular training significantly improves adherence to waste management practices among medical staff.
- Online Training Resources: Utilizing online platforms for OSHA training ensures that staff remain updated on the latest regulations. By 2026, many healthcare facilities are adopting digital training solutions to enhance accessibility and engagement, allowing staff to complete modules at their convenience.
- Assessment and Feedback: Regular assessments of staff knowledge, coupled with constructive feedback, are vital for improving compliance and safety practices. Studies show that ongoing evaluation reinforces learning and helps identify areas needing additional focus.
- Documentation: Maintaining thorough records of training sessions and participant attendance is necessary to demonstrate compliance with regulatory requirements. This documentation not only supports accountability but also aids in .
Conclusion
In conclusion, effective management of medical waste is essential for ensuring safety and compliance within healthcare facilities. This article has outlined ten critical examples of medical waste, highlighting the necessity of proper handling, disposal, and training. Categories such as sharps, biohazardous materials, pharmaceuticals, and hazardous waste each demand specific management strategies to mitigate risks and protect public health.
Key points emphasize the importance of using designated containers for sharps, adhering to regulations for biohazardous waste, and implementing best practices for pharmaceutical disposal. Furthermore, the significance of staff training and compliance with evolving regulations cannot be overstated. Facilities that prioritize these practices not only enhance safety but also contribute to environmental protection and public health.
Given the increasing complexities surrounding medical waste management, healthcare facilities must commit to continuous education and adherence to best practices. As regulations evolve, staying informed and implementing comprehensive waste management systems will be vital for ensuring compliance and safeguarding both personnel and the community. By fostering a culture of responsibility and safety, healthcare providers can effectively manage medical waste and mitigate associated risks.
Frequently Asked Questions
What are sharps waste, and why is it a concern?
Sharps waste includes materials such as needles, blades, and other sharp objects that pose significant risks of injury and infection transmission, making effective management essential in healthcare settings.
How should sharps be disposed of properly?
Sharps should be disposed of in FDA-approved, puncture-resistant containers immediately after use to minimize the risk of accidental injuries and ensure safe handling.
Why is regular training important for staff handling sharps?
Continuous training for staff on the handling and disposal of sharps is vital to minimize risks and ensure compliance with Ohio EPA regulations regarding medical refuse management.
What is the significance of strategically placing sharps containers?
Positioning sharps containers near the point of use encourages proper disposal and significantly reduces the risk of needlestick injuries, promoting safe practices.
What regulations must be followed for sharps management?
Compliance with OSHA guidelines for sharps management and Ohio EPA recommendations for the treatment of medical refuse is essential for ensuring safety and legal compliance.
What are biohazardous materials, and how should they be disposed of?
Biohazardous materials include refuse that poses a risk of infection, such as contaminated gloves, gowns, blood, body fluids, and tissues. They must be disposed of in designated biohazard bags or leak-proof containers labeled as biohazardous.
What training is necessary for handling biohazardous materials?
Comprehensive training programs for staff on identifying biohazardous materials and proper disposal practices are vital to enhance safety and compliance within healthcare facilities.
Why is pharmaceutical waste disposal important?
Pharmaceutical waste, including expired or unused medications, presents significant environmental risks if not disposed of properly, necessitating best practices for safe disposal.
What are some best practices for disposing of pharmaceutical waste?
Best practices include using take-back programs, incineration at authorized sites, secure storage in locked containers, and regular staff training on proper pharmaceutical waste management.
How do take-back programs help with pharmaceutical waste?
Take-back programs encourage patients to return unused medications to pharmacies or designated locations, facilitating safe disposal and reducing the risk of drug misuse.
What is the role of incineration in pharmaceutical waste disposal?
Incineration at authorized sites effectively eliminates hazardous pharmaceutical waste and prevents environmental contamination.
How long can biohazard materials be stored in Michigan before disposal?
In Michigan, facilities have up to 90 days to store biohazard materials, underscoring the importance of secure storage practices.
