Introduction
Effective management of infectious waste is essential in healthcare settings, where the risk of contamination and infection is significant. By recognizing the different types of infectious materials – ranging from sharps to biohazardous substances – medical facilities can adopt targeted strategies that not only meet stringent regulations but also improve safety for both staff and patients.
However, a pressing question arises: how can healthcare providers ensure that their waste management practices are both effective and compliant in a constantly changing regulatory environment? This article explores best practices that can transform infectious waste management from a challenging task into a streamlined and safe process.
Identify Types of Infectious Waste
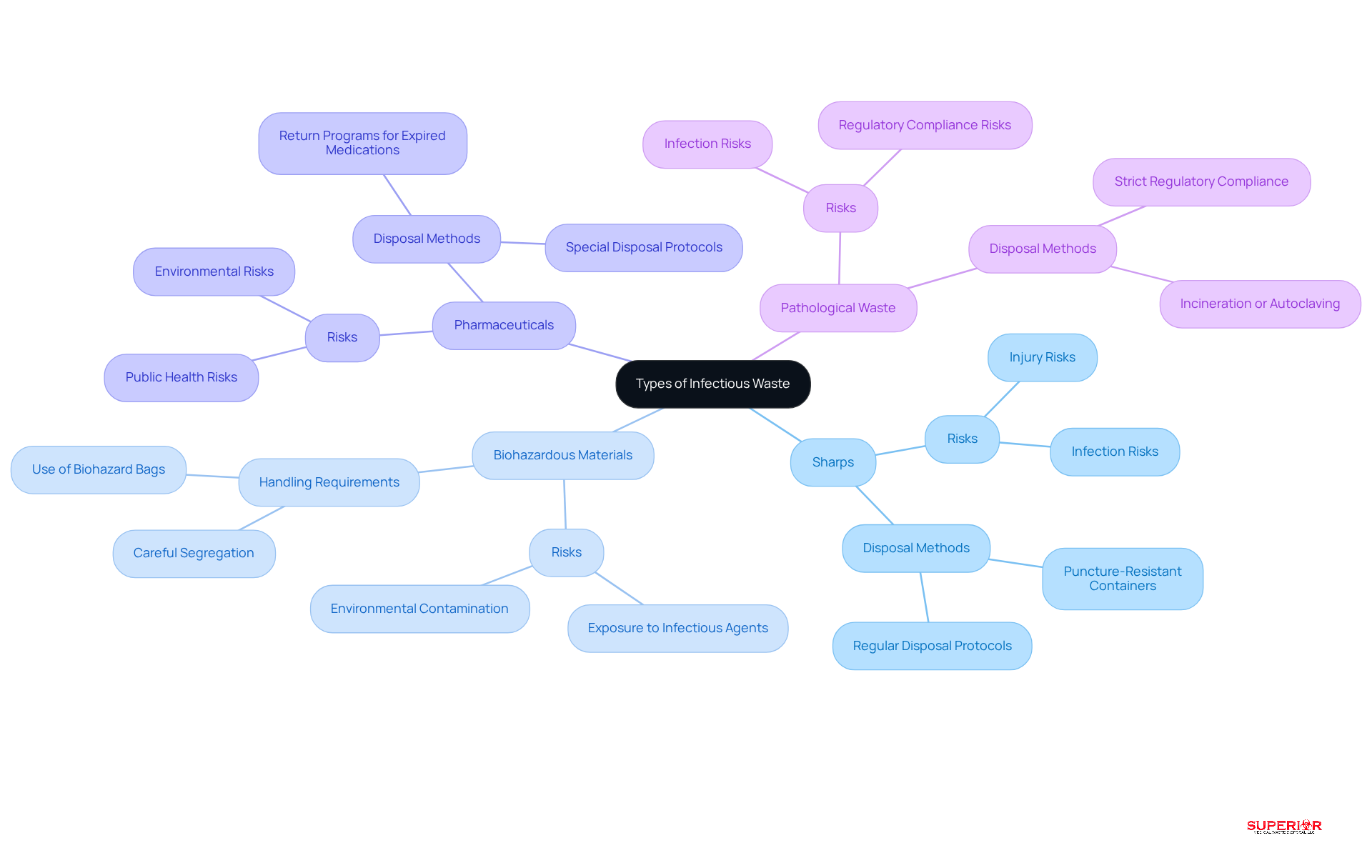
Efficient infectious waste management begins with accurately identifying the various types of infectious materials produced in medical settings. The primary categories include:
- Sharps: This category encompasses items like needles, scalpels, and broken glass, which can puncture skin and pose significant infection risks. While 15% of healthcare refuse is classified as , specific data on the percentage of sharps is not readily available. Nonetheless, it is crucial to recognize that sharps can lead to serious health hazards, including injuries caused by these materials.
- Biohazardous Materials: This includes waste contaminated with blood, bodily fluids, or other potentially infectious substances that necessitate careful handling to prevent exposure and environmental contamination.
- Pharmaceuticals: Expired or unused medications fall into this category and require special disposal methods to mitigate risks to public health and the environment.
- Pathological Waste: Human tissues, organs, and body parts must be disposed of in accordance with strict regulations to ensure safety and compliance.
Accurate classification of refuse enables medical facilities to implement targeted disposal methods as part of infectious waste management, significantly reducing the risk of contact with infectious agents. This strategy not only ensures compliance with local and federal regulations, including those set by the Ohio EPA, but also enhances overall safety within healthcare environments. Effective strategies for categorizing infectious materials include regular staff training on segregation practices and the use of clearly labeled containers to facilitate proper disposal. According to the CDC, medical refuse requires careful disposal and containment prior to collection and consolidation for treatment.
Ensure Regulatory Compliance and Safety Standards
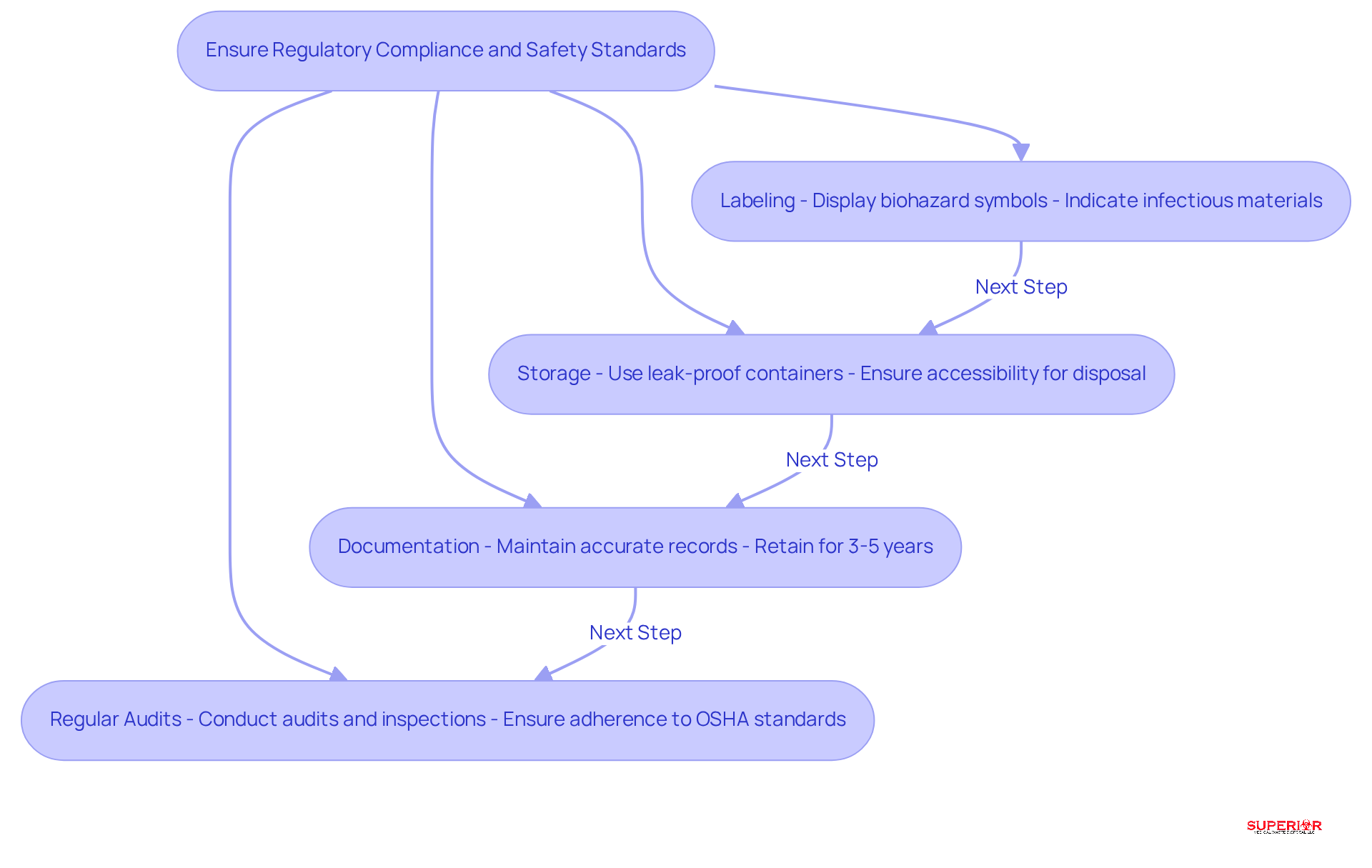
Healthcare facilities must comply with stringent regulations governing [infectious waste management](https://who.int/news-room/fact-sheets/detail/health-care-waste). Compliance is essential for safety and legal adherence, and it encompasses several critical measures:
- Labeling: Waste containers must prominently display biohazard symbols, clearly indicating the presence of infectious materials. This ensures that all personnel are aware of potential hazards, fostering a safer working environment.
- Storage: Waste should be stored in designated, leak-proof containers that are easily accessible for collection and disposal. This practice minimizes the and exposure, protecting both staff and patients.
- Documentation: Facilities are required to maintain accurate records of refuse disposal processes, including shipping manifests and treatment certificates. These records demonstrate compliance during audits. In Illinois, it is mandated that these records be retained for 3 to 5 years using IEPA-approved forms for medical waste documentation.
Regular audits and inspections are vital for ensuring adherence to OSHA standards and other relevant regulations. Facilities in Naperville, IL, that fail to follow these practices risk incurring significant penalties, with fines reaching up to $25,000 per day for non-compliance. Additionally, it is crucial to maintain training records for 3 years to avoid further fines. The rise in COVID-19 healthcare refuse has underscored the urgent need to enhance infectious waste management systems, highlighting the importance of implementing these best practices.
[Superior Medical Refuse Disposal](https://superiorwastedisposal.com) is equipped to assist medical facilities with all aspects of infectious waste management, including classification, storage, and transportation. By ensuring compliance with federal and local regulations, medical facilities can enhance safety, mitigate risks associated with improper refuse disposal, and maintain operational efficiency.
Implement Best Practices for Safe Disposal
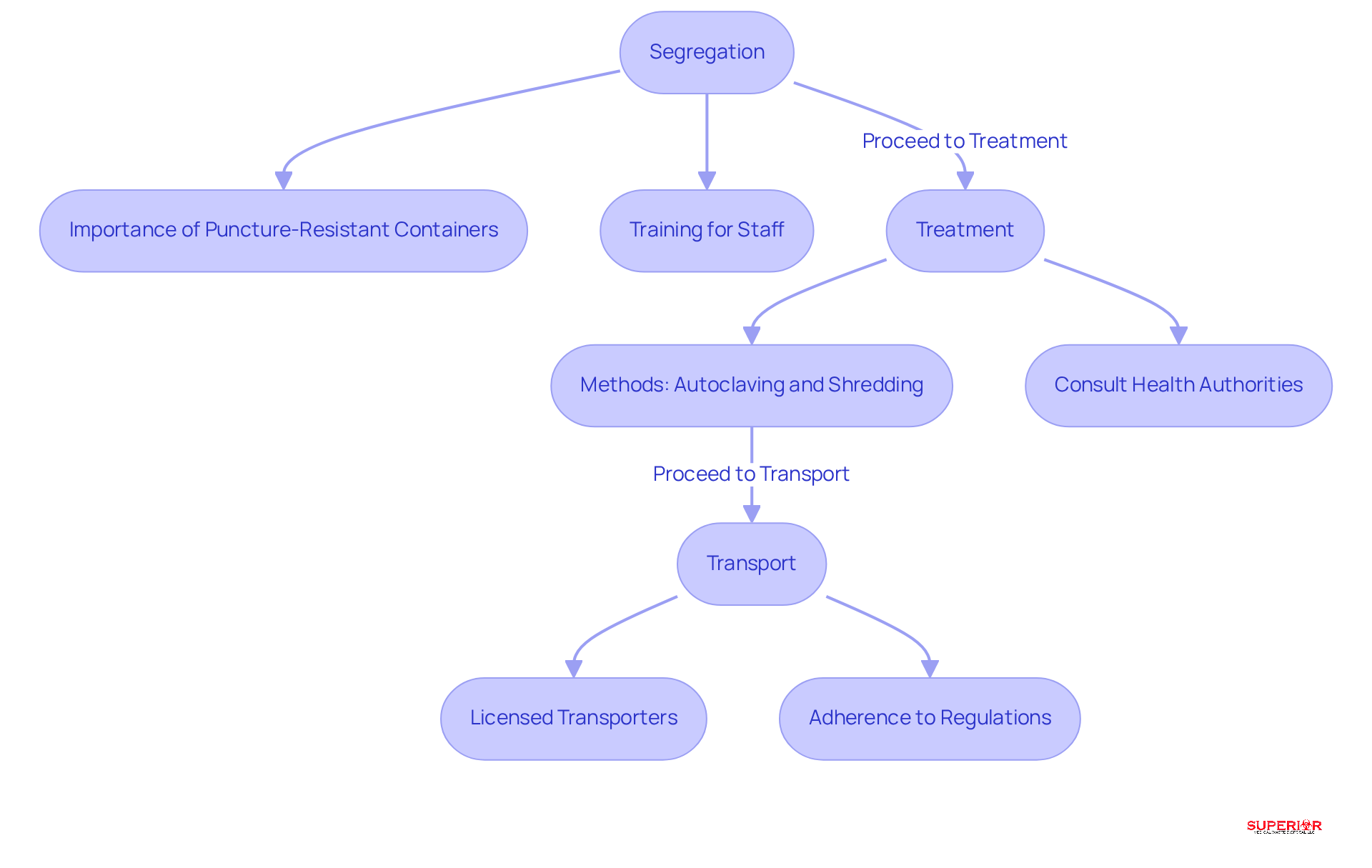
To ensure the safe disposal of infectious waste, healthcare facilities must implement several best practices:
- Segregation: Waste should be segregated at the point of generation to prevent cross-contamination. For example, sharps must be placed in puncture-resistant containers immediately after use, as improper handling can lead to injuries and infections. Effective segregation practices are essential; studies indicate that structured training can significantly improve compliance among staff.
- Treatment: Approved treatment methods, such as autoclaving or incineration, should be utilized to neutralize infectious materials prior to disposal. At Superior Medical Waste Disposal, our biohazard materials undergo autoclaving, which involves steam heating the materials at extreme temperatures to completely disinfect all potential biological threats. After treatment, the material is shredded to reduce its volume by 70% before being disposed of in a sanitary landfill. Facilities should stay informed about the latest directives from health authorities and consult local environmental agencies for specific regulations to enhance their treatment processes.
- Transport: Licensed transporters must be utilized to ensure that materials are handled and disposed of in accordance with regulatory standards. Involving experts who adhere to best practices in disposal management reduces the risk of exposure to hazardous materials during transport.
By adhering to these best practices, medical facilities can significantly mitigate the risks associated with infectious materials, thereby fostering a safer medical environment and ensuring compliance with evolving regulations.
Train Staff on Waste Management Protocols
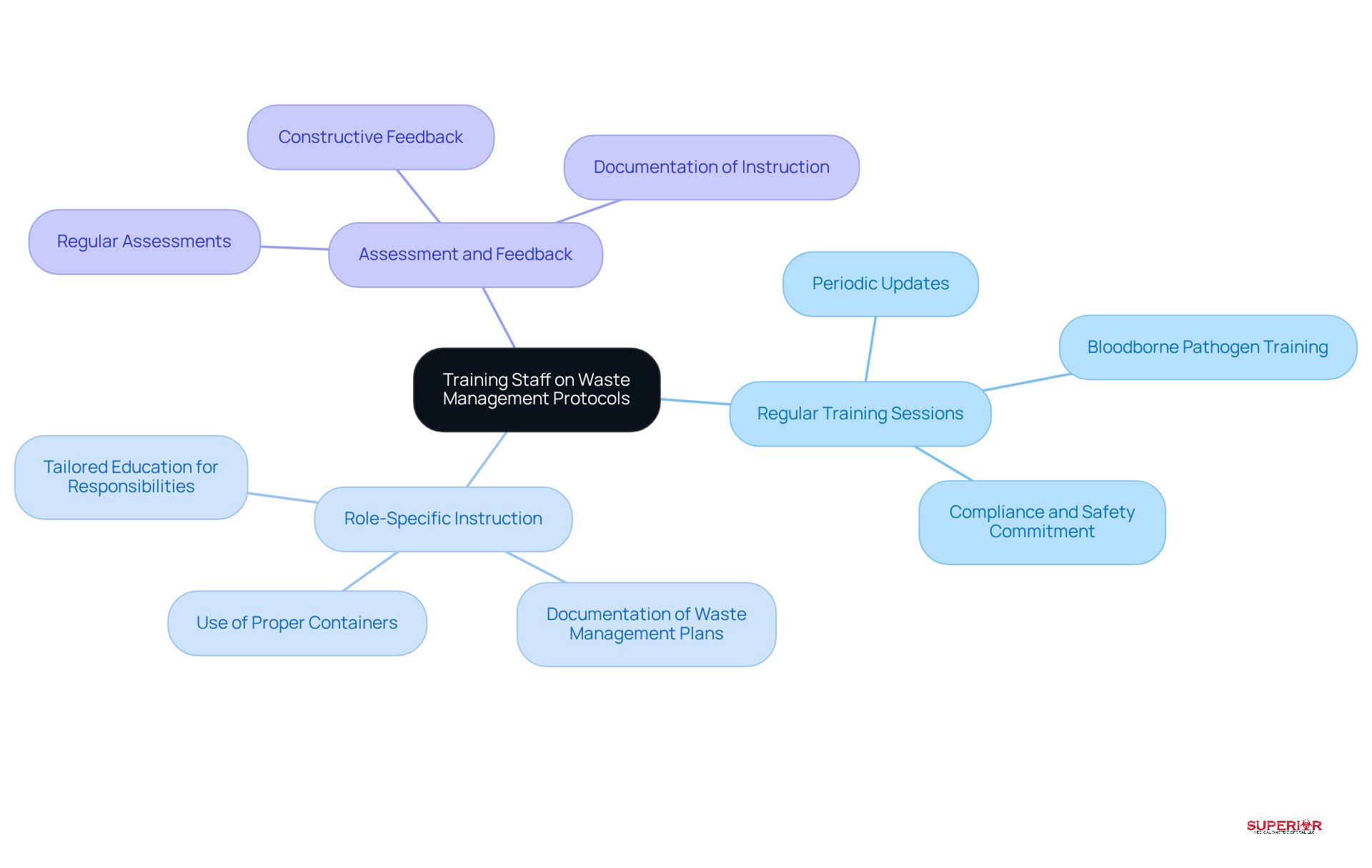
Efficient educational programs are crucial for equipping medical personnel with the necessary knowledge and skills for effective [infectious waste management](https://superiorwastedisposal.com). A successful training program comprises several key components:
- Regular Training Sessions: Periodic training sessions are vital for keeping staff updated on the latest regulations and best practices in waste management. In 2026, approximately 73% of healthcare facilities reported implementing regular management education, highlighting a growing commitment to compliance and safety. Additionally, training on bloodborne pathogens is essential for all employees handling such materials, ensuring they understand the associated risks and proper handling procedures.
- Role-Specific Instruction: Tailoring education to specific roles within the facility ensures that all employees grasp their responsibilities regarding refuse management and disposal. This approach not only enhances accountability but also boosts overall . Facilities must document their infectious waste management plans, detailing the types of waste generated and the methods for packaging, storage, treatment, and disposal for each waste type. For instance, using puncture-resistant containers for sharps and color-coded bags for different waste categories is essential.
- Assessment and Feedback: Implementing assessments to gauge staff understanding is critical. Providing constructive feedback reinforces learning and helps identify areas needing improvement. Industry leaders emphasize that effective development programs should include regular updates and practical demonstrations that bridge theoretical knowledge with real-world application. Furthermore, documentation of instruction must be maintained for a minimum of three years, as mandated by compliance regulations.
By investing in comprehensive education, medical facilities can cultivate a culture of safety and adherence, significantly reducing the risks associated with infectious waste management. Experts note that fostering an environment where staff are well-informed and engaged leads to improved waste management outcomes and enhances the overall sustainability of healthcare operations. Challenges such as high staff turnover and limited resources should also be taken into account when designing training programs.
Conclusion
Effective infectious waste management is essential for ensuring safety and compliance in healthcare settings. By adopting best practices that include accurate identification, adherence to regulations, and thorough staff training, medical facilities can significantly reduce the risks linked to infectious materials. This comprehensive approach not only safeguards healthcare workers and patients but also ensures that facilities operate within the legal frameworks set by health authorities.
Key strategies highlighted include the proper classification of waste types, such as:
- sharps
- biohazardous materials
- pharmaceuticals
- pathological waste
The article emphasizes the importance of regulatory compliance, outlining critical practices like:
- labeling
- storage
- documentation
These practices protect against legal repercussions and health hazards. Additionally, it underscores the necessity of staff training to equip personnel with the knowledge required to handle infectious waste safely and effectively.
In summary, the importance of robust infectious waste management cannot be overstated. As healthcare facilities navigate evolving regulations and the complexities of waste disposal, prioritizing these best practices will create a safer environment for all. Regular training and adherence to established protocols not only enhance operational efficiency but also contribute to the overall sustainability of healthcare operations. It is crucial for medical facilities to take proactive measures in refining their waste management strategies, ensuring that safety and compliance remain central to their efforts.
Frequently Asked Questions
What are the main types of infectious waste in medical settings?
The main types of infectious waste include sharps, biohazardous materials, pharmaceuticals, and pathological waste.
What items are classified as sharps?
Sharps include items such as needles, scalpels, and broken glass that can puncture skin and pose significant infection risks.
Why is it important to accurately classify infectious waste?
Accurate classification of infectious waste enables medical facilities to implement targeted disposal methods, reducing the risk of contact with infectious agents and ensuring compliance with regulations.
What are biohazardous materials?
Biohazardous materials are waste contaminated with blood, bodily fluids, or other potentially infectious substances that require careful handling to prevent exposure and environmental contamination.
How should expired or unused medications be disposed of?
Expired or unused medications, classified as pharmaceuticals, require special disposal methods to mitigate risks to public health and the environment.
What constitutes pathological waste?
Pathological waste includes human tissues, organs, and body parts that must be disposed of according to strict regulations to ensure safety and compliance.
What strategies can improve infectious waste management in healthcare facilities?
Effective strategies include regular staff training on segregation practices and the use of clearly labeled containers for proper disposal.
What regulations govern the disposal of medical refuse?
Medical refuse disposal is governed by local and federal regulations, including those set by the Ohio EPA, and requires careful containment prior to collection and treatment.
