Introduction
Effective healthcare waste management is not merely a regulatory requirement; it is a vital aspect of public health and environmental protection. The principle of cradle-to-grave responsibility underscores the duty of healthcare facilities to oversee waste from its creation to its final disposal, ensuring safety and compliance throughout each phase.
With increasing scrutiny and the threat of penalties for non-compliance, medical providers face the challenge of navigating the complexities of waste management while protecting their operations and community health.
This article delves into the essential practices and strategies that healthcare facilities must implement to effectively embrace cradle-to-grave responsibility in waste management, ultimately promoting a safer and more sustainable healthcare environment.
Define Cradle-to-Grave Responsibility in Healthcare Waste Management
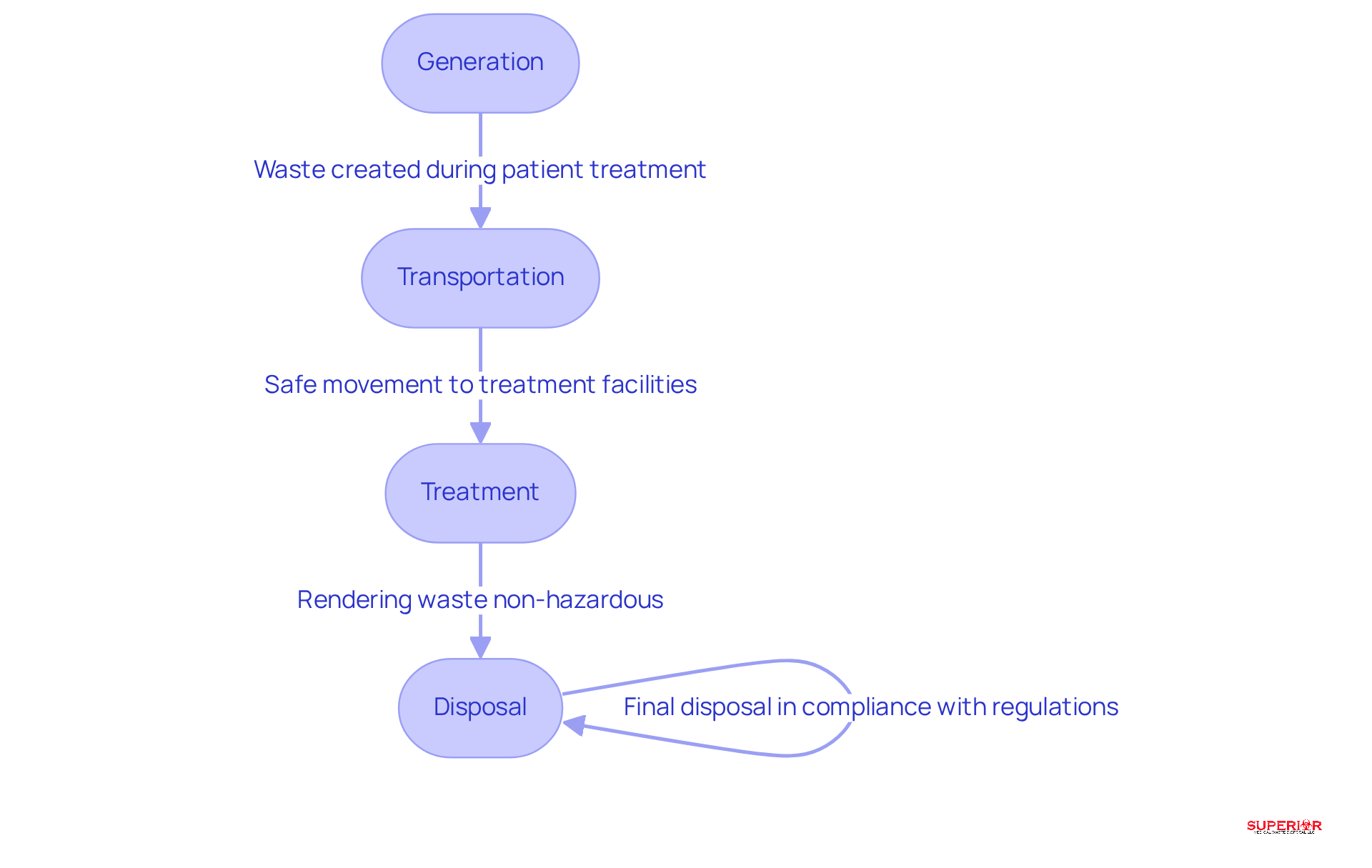
Cradle to grave responsibility in healthcare disposal management refers to the duty of healthcare facilities to manage their waste throughout its entire lifecycle. This responsibility encompasses several key components:
- Generation: Waste is created during patient treatment or medical procedures, marking the starting point of its lifecycle.
- Transportation: This involves the safe and compliant movement of waste to treatment facilities, ensuring proper handling during transit.
- Treatment: The processes employed to render waste non-hazardous or safe for disposal are crucial in mitigating potential risks associated with hazardous materials.
- Disposal: The final step involves discarding waste in accordance with established regulations, which is essential for maintaining environmental integrity and public health.
Understanding and implementing is vital for medical providers. It guarantees adherence to regulatory standards and plays a significant role in safeguarding public health and the environment from the negative impacts of improper disposal. For instance, medical establishments that efficiently manage their disposal lifecycle can significantly reduce the dangers linked to hazardous materials, such as contamination and legal liabilities.
Moreover, [collaborations with entities like Superior Medical Disposal](https://superiorwastedisposal.com) can enhance compliance and provide essential training for personnel on bloodborne pathogens and disposal practices. This proactive approach is crucial in fostering a safer and more sustainable medical environment. In 2026, penalties for medical waste non-compliance will vary by state, with federal EPA violations potentially incurring fines of up to $75,000 per day per violation. Additionally, the medical sector handles approximately 5.9 million tons of clinical waste each year, underscoring the extent of the issue and the necessity for efficient disposal practices. The Resource Conservation and Recovery Act (RCRA) regulates hazardous materials handling, emphasizing that the generator’s responsibility persists as long as the substance remains hazardous.
Outline the Stages of the Cradle-to-Grave Process
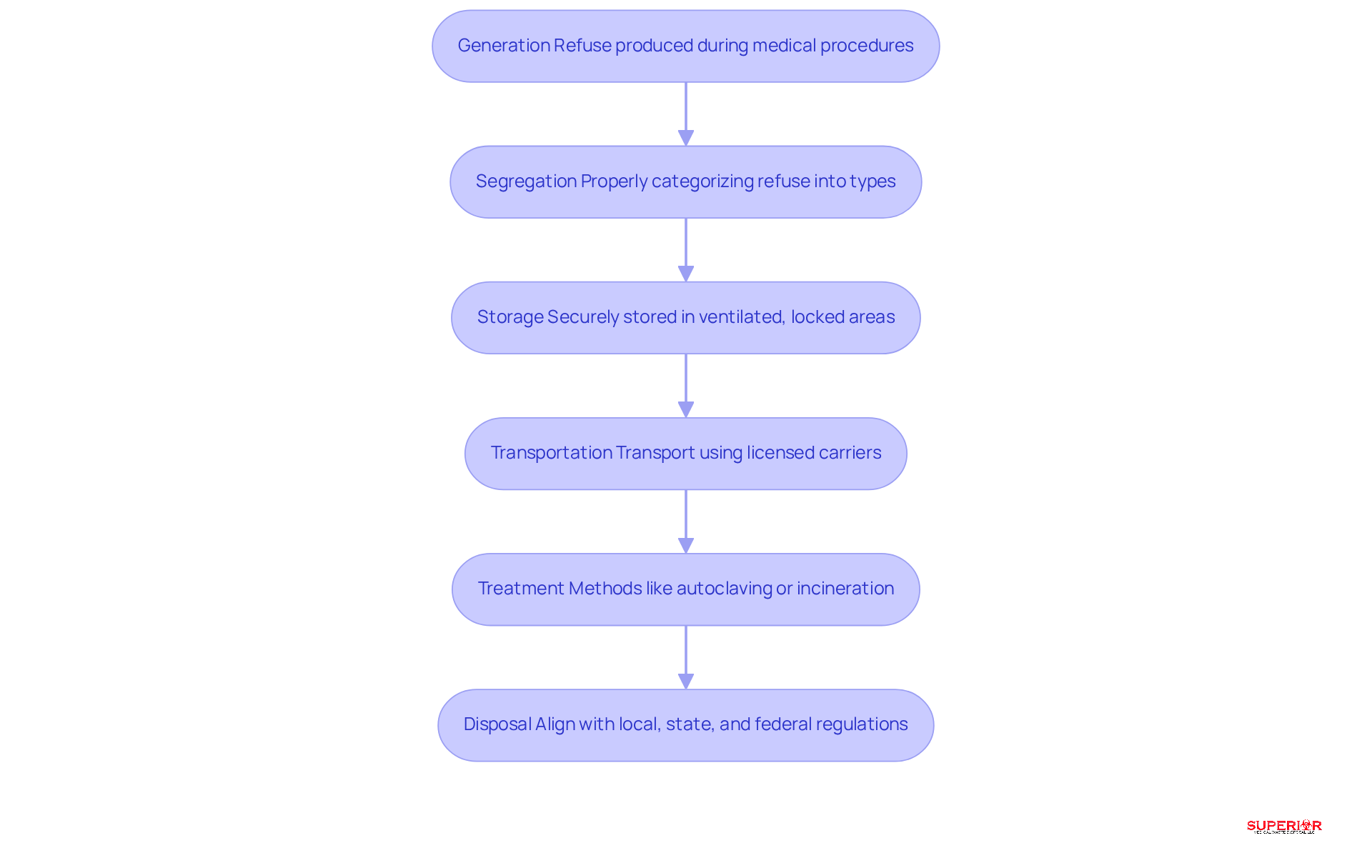
The cradle-to-grave process in healthcare waste management involves several critical stages that ensure safety and compliance:
- Generation: Refuse is produced during medical procedures, diagnostics, or treatments, with healthcare facilities generating significant volumes of refuse daily. For example, high-income nations produce an average of 0.5 kg of hazardous material per hospital bed per day.
- Segregation: Effective material separation is vital. Properly categorizing refuse into sharps, biohazardous, and non-hazardous materials minimizes contamination risks and enhances safety. Facilities should adopt standardized, puncture-resistant containers tailored to specific waste types to improve efficiency and adherence.
- Storage: Safe storage practices are essential. Waste must be securely stored in to prevent unauthorized access, with storage times varying by state regulations-some allowing up to 90 days. Clear labeling and adherence to local mandates are crucial for compliance.
- Transportation: Waste must be transported to treatment facilities using licensed carriers. This step is critical for maintaining safety and compliance, as improper transport can lead to significant regulatory penalties.
- Treatment: Treatment methods, such as autoclaving or incineration, are employed to neutralize hazardous materials. Facilities should ensure that their disposal partner utilizes locally mandated treatment methods to avoid liability.
- Disposal: Finally, the disposal of treated materials must align with local, state, and federal regulations. Maintaining precise documentation, including shipping manifests and certificates of destruction, is crucial for compliance and audit preparedness.
Every phase of this process reflects a cradle to grave responsibility that demands careful attention to detail to ensure adherence and reduce risks linked to improper disposal. By embedding these practices into daily operations, medical facilities can enhance safety, protect patient privacy, and support regulatory compliance.
Discuss Regulatory Compliance and Legal Implications
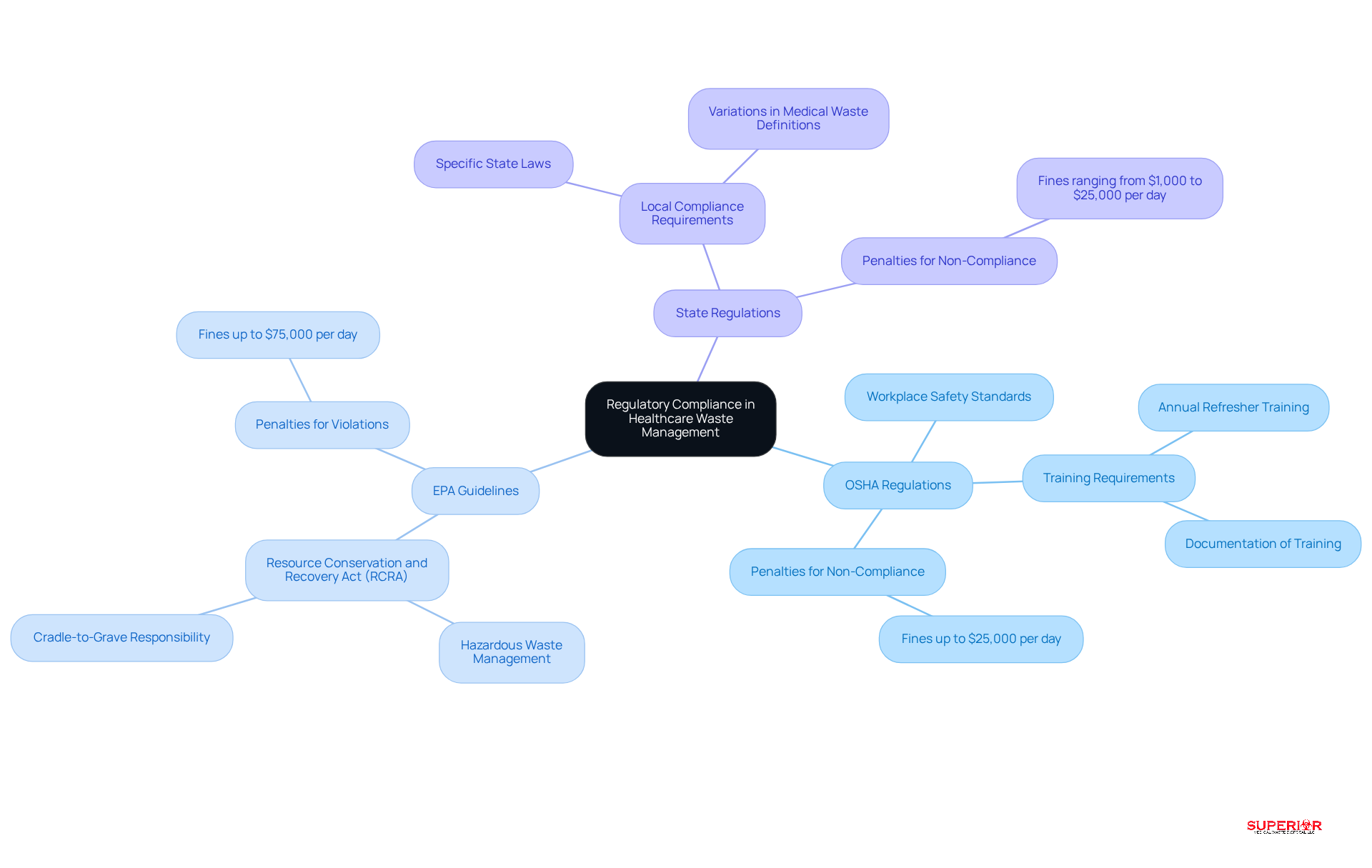
Regulatory compliance in healthcare waste management is essential, requiring adherence to various laws and guidelines:
- OSHA Regulations: These regulations ensure workplace safety and health standards are upheld during waste handling, protecting staff from potential hazards associated with medical waste.
- EPA Guidelines: Compliance with the Resource Conservation and Recovery Act (RCRA) is vital for the proper handling of hazardous materials, which involves strict protocols for disposal and treatment.
- State Regulations: Many states impose specific laws that may exceed federal requirements, necessitating a thorough understanding of local regulations to avoid penalties.
Prominent healthcare establishments in Flint, such as Hurley, McLaren, and Ascension, significantly contribute to the medical refuse produced in the region, underscoring the need for effective disposal solutions. Non-compliance with these regulations can lead to severe repercussions, including fines that can reach up to $75,000 per day for federal violations and state penalties ranging from $1,000 to $25,000 per day for improper storage, labeling, or disposal. For example, a Missouri podiatry clinic faced proposed penalties exceeding $93,000 due to multiple OSHA violations related to documentation failures. Additionally, a hospital in Western Pennsylvania was penalized $451,000 for improperly discarding untreated medical materials in a landfill, highlighting the legal consequences of negligence in disposal management.
Healthcare facilities must prioritize maintaining thorough documentation and regular training for staff to ensure adherence to these regulations. This includes understanding the importance of , accurate labeling, and the use of compliant containers. Regular training sessions not only help mitigate risks but also serve as crucial evidence during inspections, as fines for non-compliance with training documentation can reach up to $25,000 per day. By fostering a culture of compliance, medical facilities can protect their reputation and ensure the safety of their staff and patients.
Create Customized Waste Management Plans for Healthcare Facilities
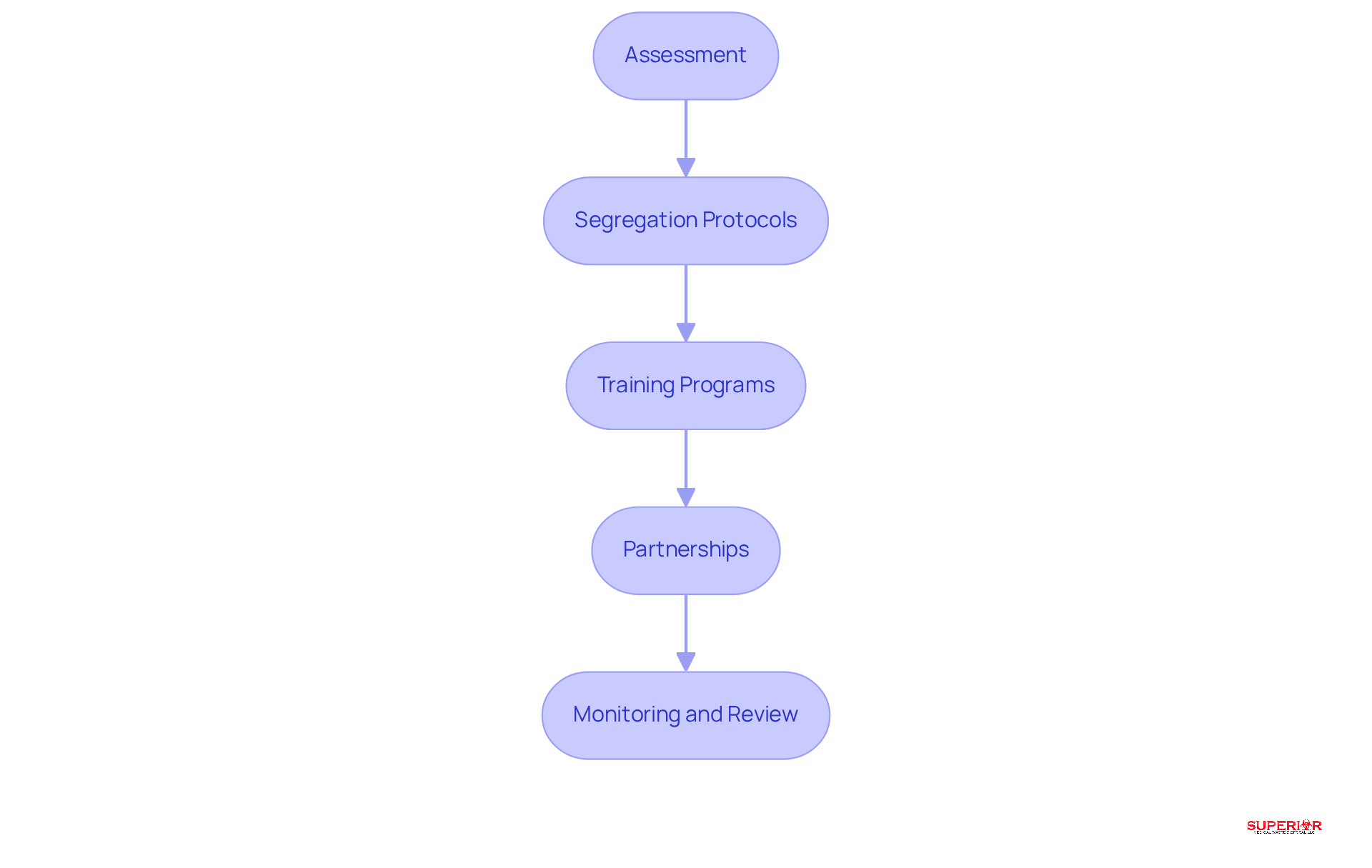
To develop an effective customized waste management plan, healthcare facilities should follow these essential steps:
- Assessment: Conduct a thorough evaluation of the types and volumes of refuse generated to identify specific needs and challenges.
- Segregation Protocols: Establish clear guidelines for material segregation to minimize contamination risks and ensure compliance with regulatory standards. Proper segregation is essential, as the World Health Organization estimates that 15% of healthcare refuse is hazardous or biohazardous, necessitating careful handling.
- Training Programs: Implement on proper refuse handling and disposal procedures. Enhanced training and protocols, as recommended by the Centers for Disease Control and Prevention, are vital for ensuring safe practices.
- Partnerships: Collaborate with licensed disposal firms to guarantee safe transportation and treatment of refuse. Engaging with experienced partners can streamline processes and enhance accountability.
- Monitoring and Review: Regularly assess and revise the disposal strategy to adjust to alterations in regulations or facility operations. Ongoing monitoring aids in upholding standards and enhances operational efficiency.
By tailoring waste management plans to the unique needs of each facility, healthcare providers can significantly enhance compliance, safety, and overall operational efficiency, ultimately contributing to better patient care and environmental sustainability.
Conclusion
Effective healthcare waste management relies on the principle of cradle-to-grave responsibility, which encompasses the entire lifecycle of waste generated within medical facilities. This comprehensive approach ensures that waste is managed from its creation to its final disposal, highlighting the importance of safety, regulatory compliance, and environmental protection.
The article explored critical components of the cradle-to-grave process, including:
- Waste generation
- Segregation
- Storage
- Transportation
- Treatment
- Disposal
Each stage plays a pivotal role in minimizing risks associated with hazardous materials and maintaining adherence to regulations set forth by entities like OSHA and the EPA. Furthermore, the discussion emphasized the necessity of customized waste management plans tailored to the specific needs of healthcare facilities, enabling them to enhance compliance and operational efficiency.
As healthcare providers navigate the complexities of waste management, the insights shared serve as a vital reminder of their responsibility in safeguarding public health and the environment. By prioritizing thorough training, regulatory adherence, and effective waste management strategies, medical facilities can mitigate potential liabilities and contribute to a more sustainable future. Embracing cradle-to-grave responsibility is not merely a regulatory requirement; it represents a commitment to excellence in patient care and environmental stewardship.
Frequently Asked Questions
What does cradle-to-grave responsibility in healthcare waste management entail?
Cradle-to-grave responsibility refers to the duty of healthcare facilities to manage their waste throughout its entire lifecycle, including generation, transportation, treatment, and disposal.
What are the key components of cradle-to-grave responsibility?
The key components include: – Generation: Waste created during patient treatment or medical procedures. – Transportation: Safe and compliant movement of waste to treatment facilities. – Treatment: Processes to render waste non-hazardous or safe for disposal. – Disposal: Discarding waste according to established regulations.
Why is understanding cradle-to-grave responsibility important for medical providers?
It ensures adherence to regulatory standards and helps safeguard public health and the environment from the risks associated with improper waste disposal.
What are the potential consequences of improper waste disposal in healthcare?
Improper disposal can lead to contamination, legal liabilities, and negative impacts on public health and the environment.
How can collaborations with disposal entities benefit healthcare facilities?
Collaborations can enhance compliance and provide essential training for personnel on bloodborne pathogens and proper disposal practices, fostering a safer medical environment.
What are the penalties for medical waste non-compliance expected in 2026?
Penalties will vary by state, with federal EPA violations potentially incurring fines of up to $75,000 per day per violation.
How much clinical waste does the medical sector handle annually?
The medical sector handles approximately 5.9 million tons of clinical waste each year.
What does the Resource Conservation and Recovery Act (RCRA) regulate?
The RCRA regulates the handling of hazardous materials, emphasizing that the generator’s responsibility continues as long as the substance remains hazardous.
