Introduction
Understanding HIPAA shredding requirements is essential for healthcare organizations that seek to protect sensitive patient information. The potential for severe penalties associated with improper disposal practices underscores the importance of compliance. This article outlines the necessary methods and documentation to ensure adherence to these regulations, while also highlighting the significant risks that arise from neglecting these legal obligations.
How can healthcare facilities effectively navigate these requirements to safeguard patient privacy and maintain their operational integrity?
Clarify HIPAA Shredding Requirements and Legal Obligations
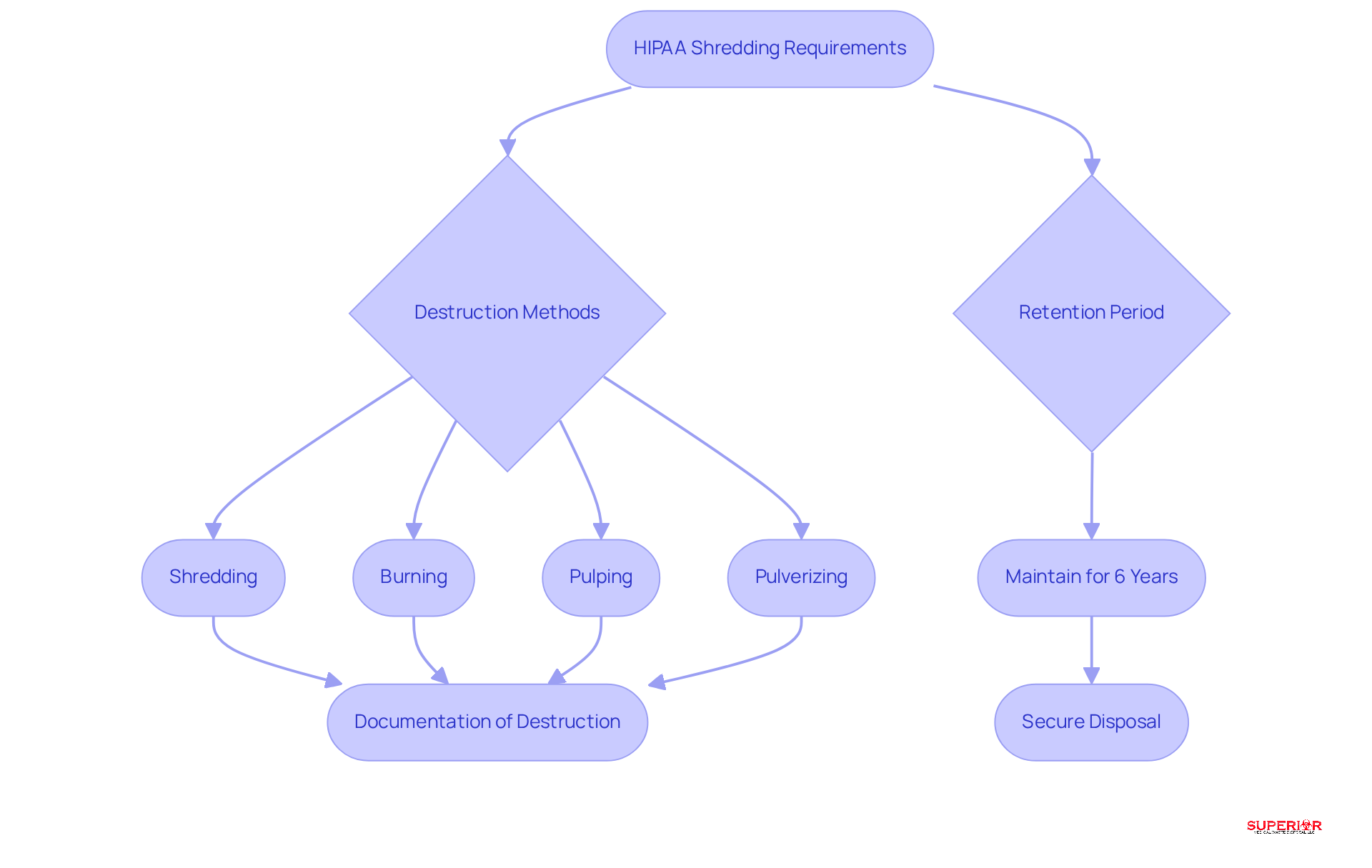
The Health Insurance Portability and Accountability Act (HIPAA) mandates that all covered entities comply with HIPAA shredding requirements to ensure the secure disposal of protected health information (PHI), which includes any documents containing identifiable patient information. Key requirements include the following:
-
Destruction Methods: HIPAA does not specify a particular destruction method; however, it requires that PHI be rendered unreadable, indecipherable, and otherwise unable to be reconstructed. Acceptable methods include shredding, burning, pulping, or pulverizing. Improper disposal of PHI can lead to significant penalties, as demonstrated by the New England Dermatology and Laser Center, which faced a $300,640 penalty for improper disposal practices.
-
Retention Period: Certain documents must be maintained for six years from the date of creation or the date when they were last in effect. After this period, secure disposal is necessary to meet HIPAA shredding requirements. Failure to adhere to these retention laws can result in hefty fines, with the average cost of a healthcare data breach reaching $10.93 million.
Organizations must maintain records of the destruction process, including the method used and the date of destruction, to demonstrate adherence to HIPAA shredding requirements during audits. This documentation is crucial, especially considering that 53% of healthcare data breaches are attributed to employee negligence. This statistic underscores the importance of proper training and adherence to disposal protocols.
Understanding these requirements is essential for healthcare facilities to avoid penalties and protect patient privacy. Regular adherence training and secure disposal practices not only fulfill legal obligations but also reinforce patient trust and organizational integrity.
Implement Secure Shredding Methods for PHI Disposal
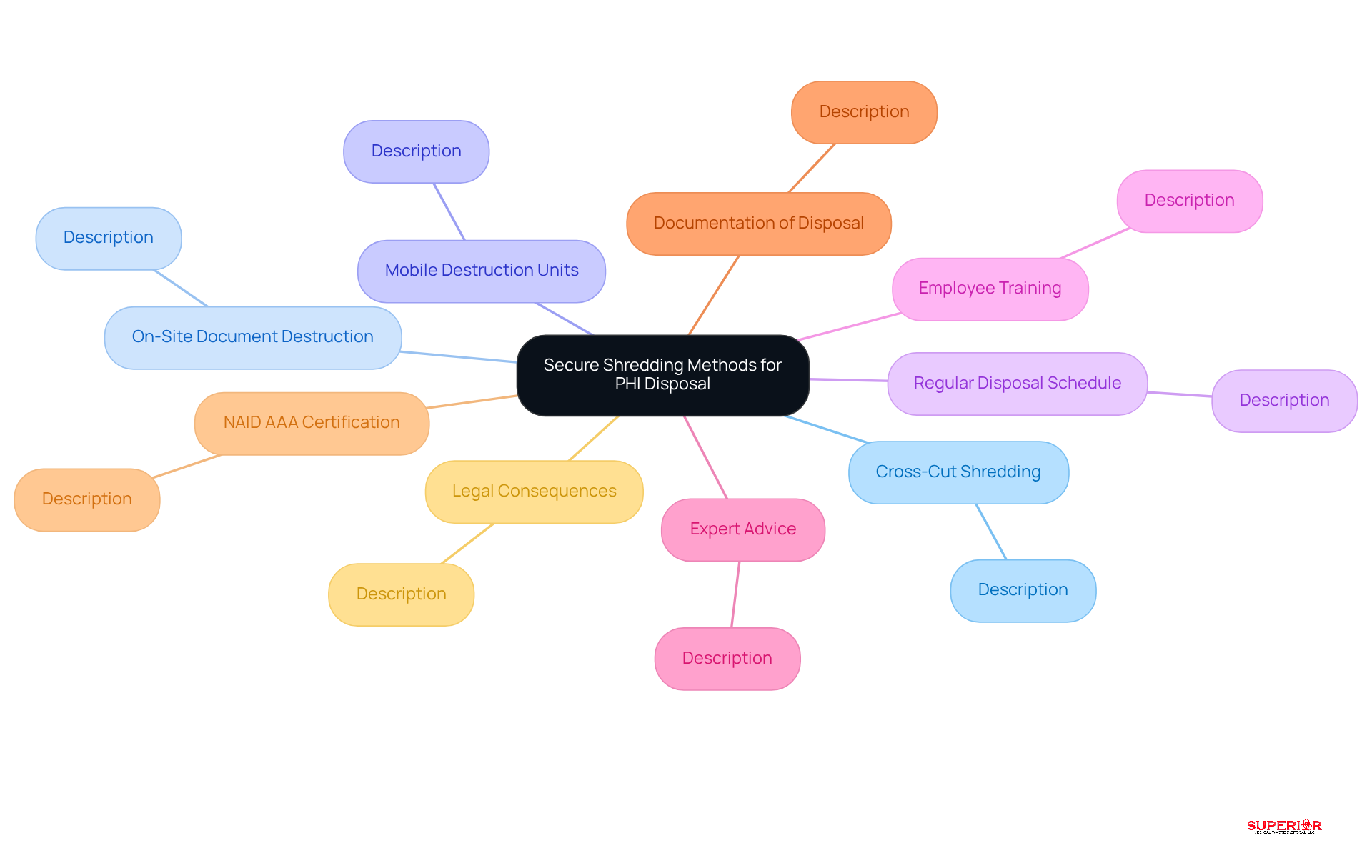
To ensure compliance with the HIPAA shredding requirements, healthcare facilities must adopt secure shredding methods that effectively protect sensitive information. The following approaches are recommended:
-
Cross-Cut Shredding: Utilize cross-cut shredders that reduce paper into particles as small as 1 mm x 5 mm. This method makes reconstruction nearly impossible and is essential for disposing of protected health information (PHI) in compliance with HIPAA shredding requirements.
-
On-Site Document Destruction Services: Engage professional disposal services, such as those provided by Superior Medical Waste Disposal, which offer on-site document destruction. This ensures that files are disposed of promptly and safely in your presence, enhancing accountability and compliance.
-
Mobile Destruction Units: Implement mobile destruction units that come directly to your facility, allowing for real-time disposal of materials. This not only boosts security but also provides peace of mind, knowing that sensitive information is handled on-site.
-
Regular Document Disposal Schedule: Establish a consistent document disposal routine to prevent the accumulation of PHI. Depending on your document volume, this could be weekly, monthly, or tailored to your specific needs, ensuring timely disposal and adherence to regulations.
-
Employee Training: Provide comprehensive training for staff on the importance of secure disposal and the specific methods implemented in your facility. This awareness is crucial for maintaining compliance and minimizing risks associated with improper disposal.
-
Seek Expert Advice: Consult with experts, such as those at Superior Medical Waste Disposal, for guidance on HIPAA regulations and disposal practices. This ensures that your facility complies with the latest HIPAA shredding requirements and follows best practices.
-
Documentation of Disposal: Maintain thorough documentation of the disposal process, including Certificates of Destruction, which serve as evidence of compliance during audits or investigations. This documentation is vital for accountability and regulatory adherence.
-
NAID AAA Certification: Ensure that your disposal provider is NAID AAA certified, signifying adherence to the highest standards for information destruction. This certification enhances the credibility of the techniques employed.
-
Legal Consequences of Improper Disposal: Be aware that improper disposal of PHI, including patient medical records and social security numbers, can lead to significant legal consequences, including fines that may reach up to $68,928 per incident. Understanding these risks underscores the importance of employing secure disposal methods.
By implementing these methods, healthcare organizations can significantly reduce the risk of data breaches, ensure compliance with regulations, and ultimately safeguard patient privacy while maintaining trust.
Document the Shredding Process for Compliance and Accountability
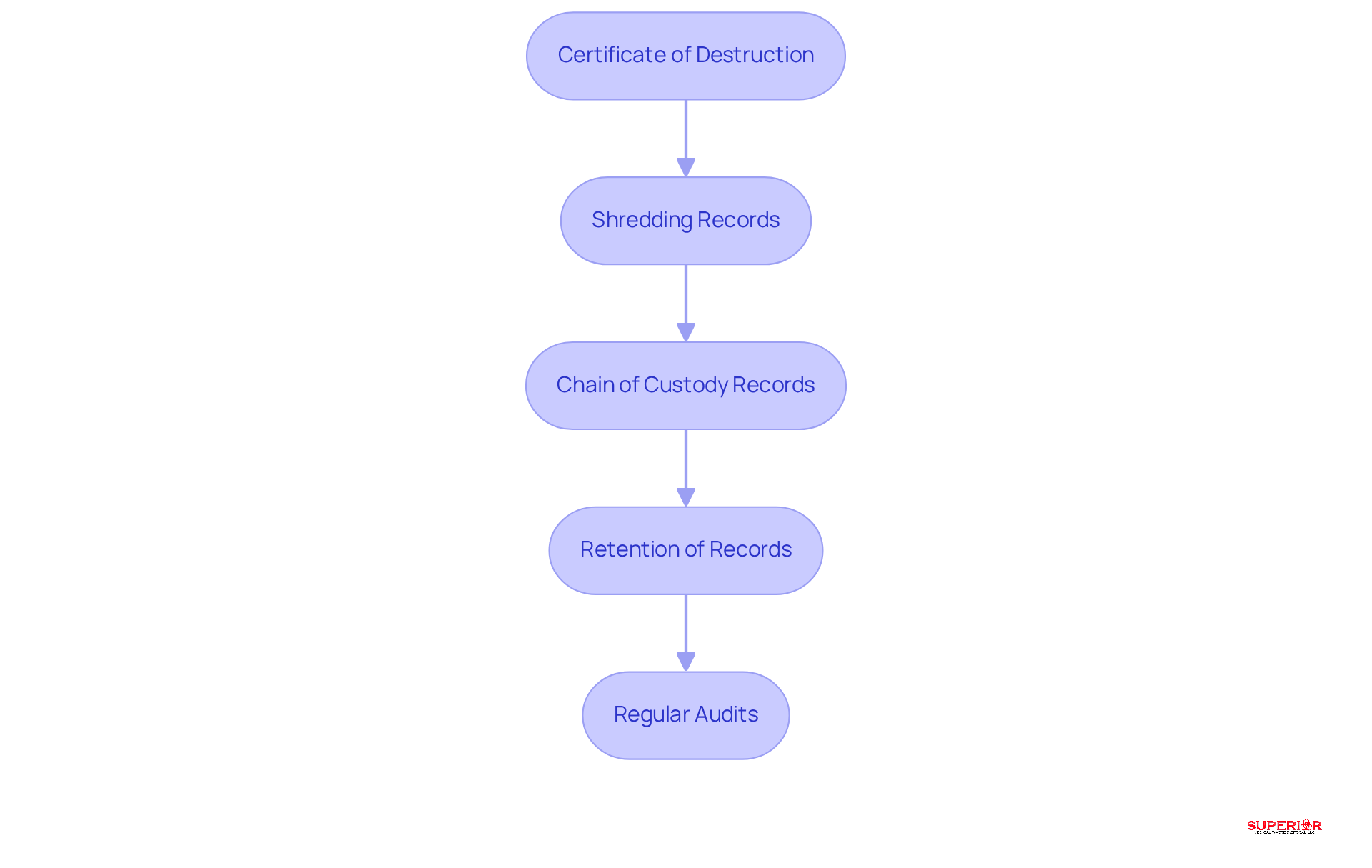
Accurate recording of the document disposal procedure is essential for compliance with privacy regulations. The following key components should be included:
-
Certificate of Destruction: Secure a Certificate of Destruction from your document disposal service provider. This document serves as proof that the files were destroyed in compliance with HIPAA shredding requirements, reinforcing your commitment to patient privacy.
-
Shredding Records: Maintain detailed records that specify the date of disposal, the types of materials destroyed, and the methods used. Regular updates to this log are vital for audit purposes and demonstrate compliance with established protocols.
-
Chain of Custody Records: Document the chain of custody for all protected health information (PHI). This includes tracking who handled the documents prior to disposal and recording the time and date of transfer to the destruction service, ensuring accountability throughout the process.
-
Retention of Records: Retain all documentation related to disposal for a minimum of six years, as mandated by HIPAA shredding requirements. This includes Certificates of Destruction and disposal logs, which are crucial for demonstrating compliance during audits.
-
Regular Audits: Conduct routine inspections of your disposal documentation to ensure compliance and identify areas for improvement. This proactive approach not only enhances security but also fosters a culture of accountability within your organization.
By meticulously documenting the destruction process, healthcare organizations can effectively protect patient information and reduce the risks associated with improper disposal, thereby reinforcing trust and compliance.
Choose HIPAA-Compliant Shredding Services and Equipment
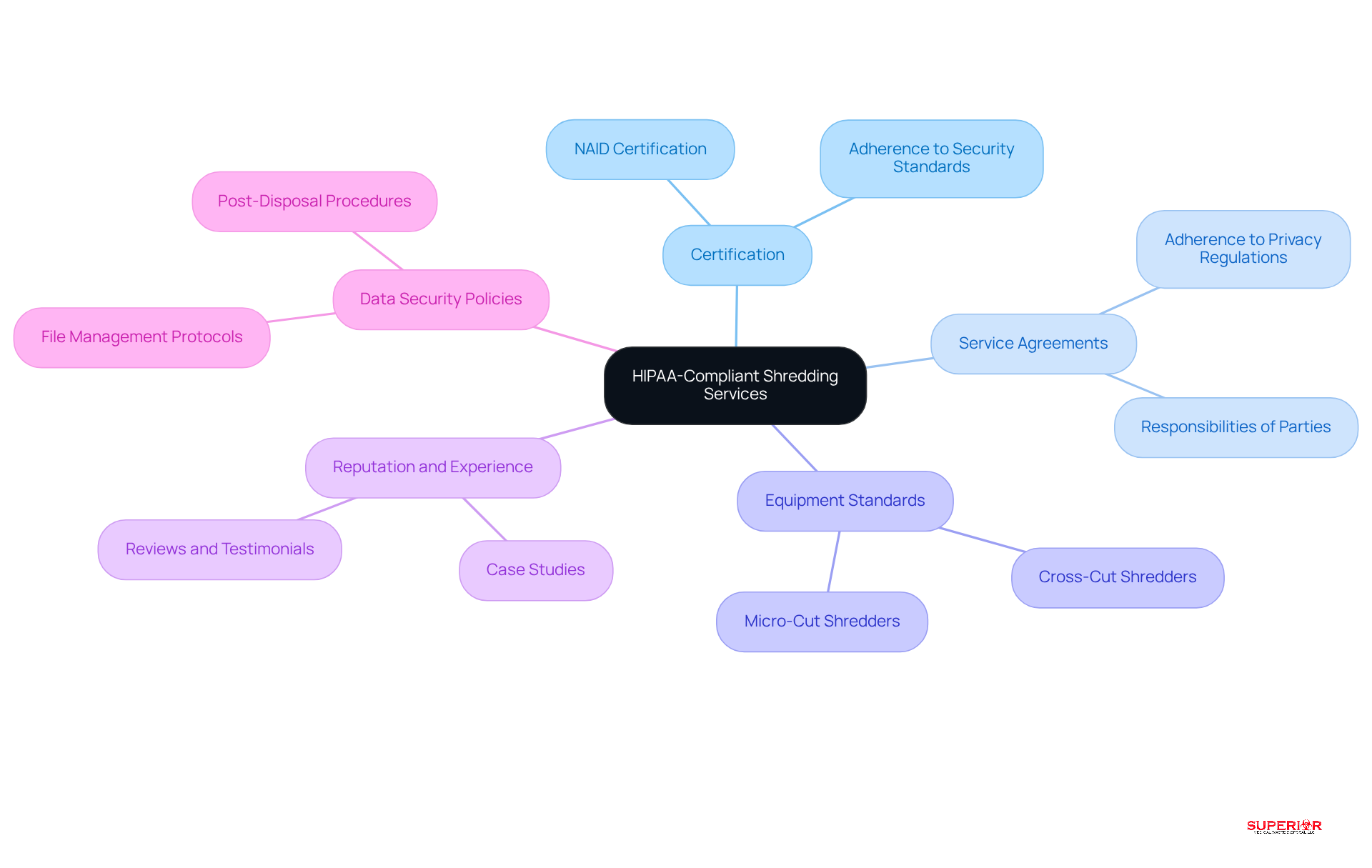
When selecting shredding services and equipment, healthcare organizations must prioritize several key factors to meet HIPAA shredding requirements.
-
Certification is paramount. Confirm that the shredding service provider holds NAID (National Association for Information Destruction) certification. This certification signifies adherence to rigorous security standards, essential for protecting sensitive information.
-
Next, consider Service Agreements. Ensure that these agreements explicitly state adherence to health information privacy regulations. They should clearly outline the responsibilities of both parties regarding the disposal of Protected Health Information (PHI).
-
Equipment Standards are also critical. Choose shredders that comply with or surpass HIPAA standards, such as cross-cut or micro-cut shredders, which effectively render papers unreadable and secure.
-
Additionally, investigate the Reputation and Experience of potential document destruction service providers. Look for reviews, testimonials, and case studies that highlight their expertise in securely handling PHI.
-
Finally, inquire about the Data Security Policies of the document disposal company. Understanding their protocols for managing files before and after disposal is vital to ensuring confidentiality throughout the process.
By meticulously selecting shredding services and equipment that comply with HIPAA shredding requirements, healthcare organizations can significantly bolster their data protection efforts and ensure adherence to legal requirements. NAID certification is particularly crucial, as it enhances operational efficiency and builds trust with clients and stakeholders, thereby mitigating legal risks associated with improper data handling.
Conclusion
Understanding and adhering to HIPAA shredding requirements is essential for healthcare organizations that seek to protect patient privacy and avoid significant penalties. The act mandates that all protected health information (PHI) must be disposed of in a way that renders it unreadable and irretrievable. By implementing secure shredding methods and maintaining thorough documentation of the disposal process, organizations can achieve compliance while reinforcing trust with their patients.
Key points highlighted in this article include:
- The importance of selecting appropriate shredding methods, such as cross-cut shredders and on-site destruction services, which significantly enhance security during the disposal process.
- The necessity of maintaining records, including Certificates of Destruction and detailed logs, underscores the accountability required for compliance audits.
- Regular employee training and consulting with experts further solidify an organization’s commitment to meeting HIPAA standards.
Ultimately, the stakes are high regarding the secure disposal of PHI. By prioritizing HIPAA-compliant shredding practices, healthcare facilities not only fulfill their legal obligations but also safeguard sensitive patient information from breaches. This proactive approach mitigates risks associated with non-compliance and fosters a culture of accountability and trust within the organization. Embracing these best practices is vital for any healthcare provider dedicated to upholding the highest standards of patient privacy and data security.
