Introduction
In an era where data breaches pose significant risks to healthcare organizations, the necessity of adhering to HIPAA regulations is paramount. For administrators of healthcare facilities, implementing best practices transcends mere compliance; it is crucial for safeguarding patient trust and protecting sensitive information. This article delves into ten essential HIPAA best practices that can markedly strengthen a facility’s security posture.
However, what are the consequences when these measures are neglected? Grasping the critical nature of these practices is vital for navigating the intricate landscape of healthcare compliance and defending against the continuously evolving threats to patient data.
Conduct Comprehensive Risk Analysis
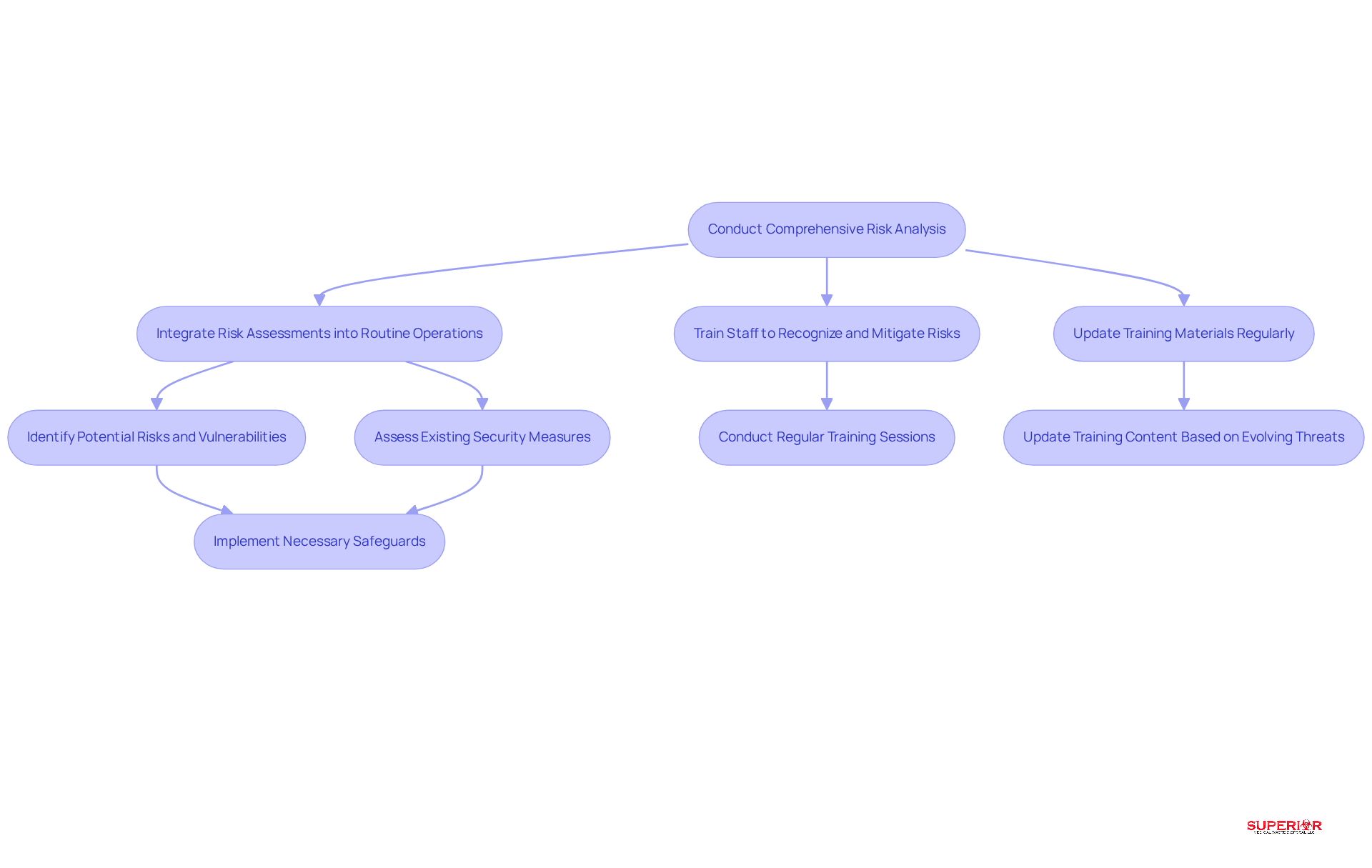
A comprehensive risk analysis is crucial for healthcare facilities and is considered one of the essential practices for protecting electronic protected health information (ePHI). This process entails identifying potential risks and vulnerabilities that could jeopardize the confidentiality, integrity, and availability of ePHI. Regular risk evaluations are vital; statistics indicate that only 57% of medical organizations review their access controls annually, highlighting a significant opportunity for improvement. By assessing existing security measures, administrators can identify weaknesses and bolster their organization’s overall security posture.
To effectively conduct a risk analysis, medical facilities should leverage tools and frameworks that align with recommendations by the Department of Health and Human Services (HHS). These resources offer structured guidance for pinpointing vulnerabilities and implementing necessary safeguards. Effective strategies that align with best practices include:
- Integrating technology solutions
- Ensuring that all staff are trained to recognize and mitigate risks
- Updating policies to reflect evolving threats
By adopting a proactive approach to risk management, medical organizations can not only achieve compliance but also cultivate a culture of security that protects sensitive patient data.
Implement Technical Safeguards
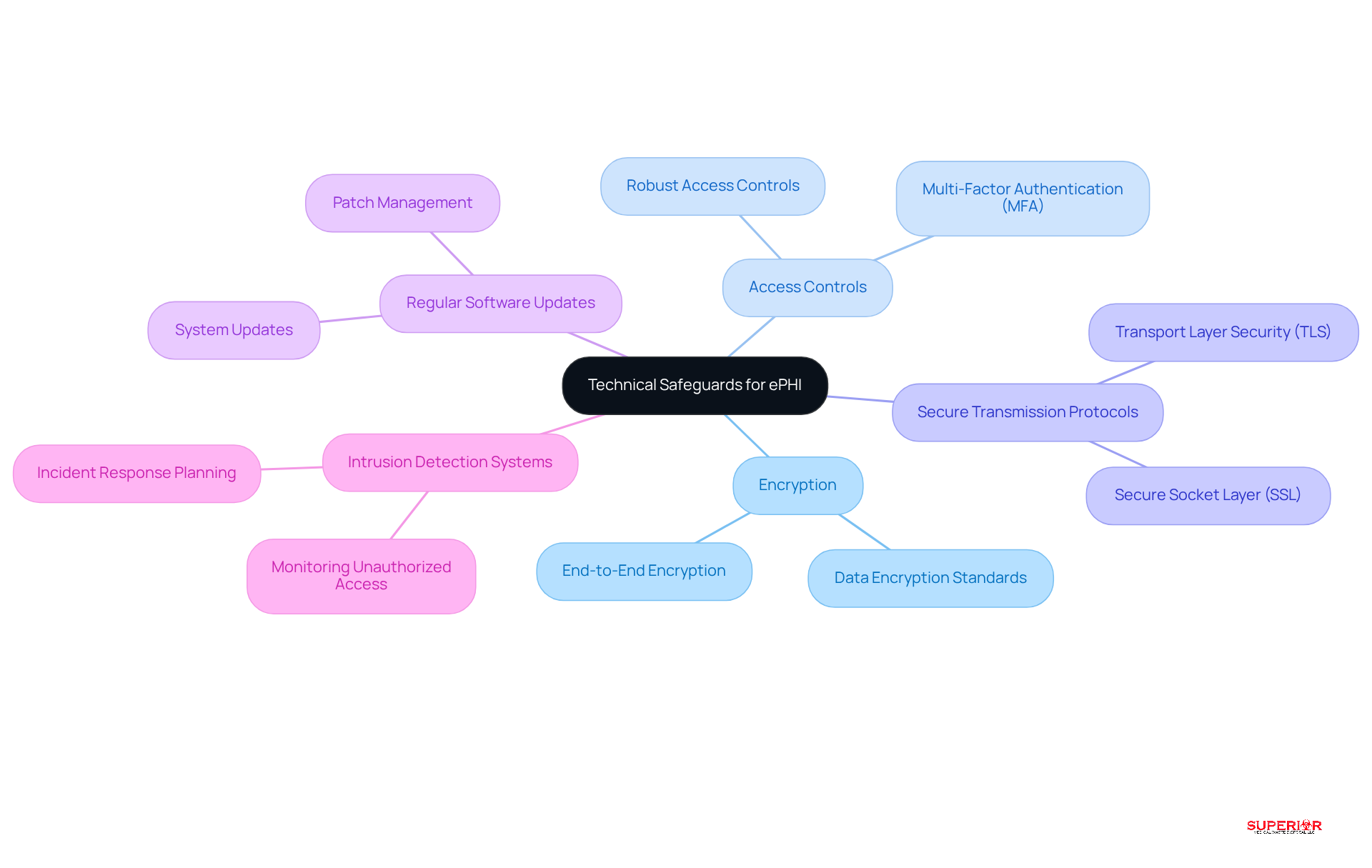
Technical safeguards are essential for protecting electronic protected health information (ePHI). The key components include:
- Encryption
Implementing multi-factor authentication (MFA) across all systems that access ePHI is crucial; it ensures that only authorized personnel can access sensitive information. Recent trends show that medical organizations are taking steps to bolster their security posture. Notably, 92% of medical institutions reported experiencing at least one cyberattack in the past year, highlighting the urgent need for enhanced protective measures.
Regular software and system updates are vital for mitigating vulnerabilities, while employing intrusion detection systems can effectively monitor unauthorized access attempts. In 2024, medical organizations faced an average of 40 cyber incidents, underscoring the necessity of maintaining a proactive security strategy. By prioritizing these safeguards, organizations can ensure adherence to compliance standards.
Train Employees on HIPAA Regulations
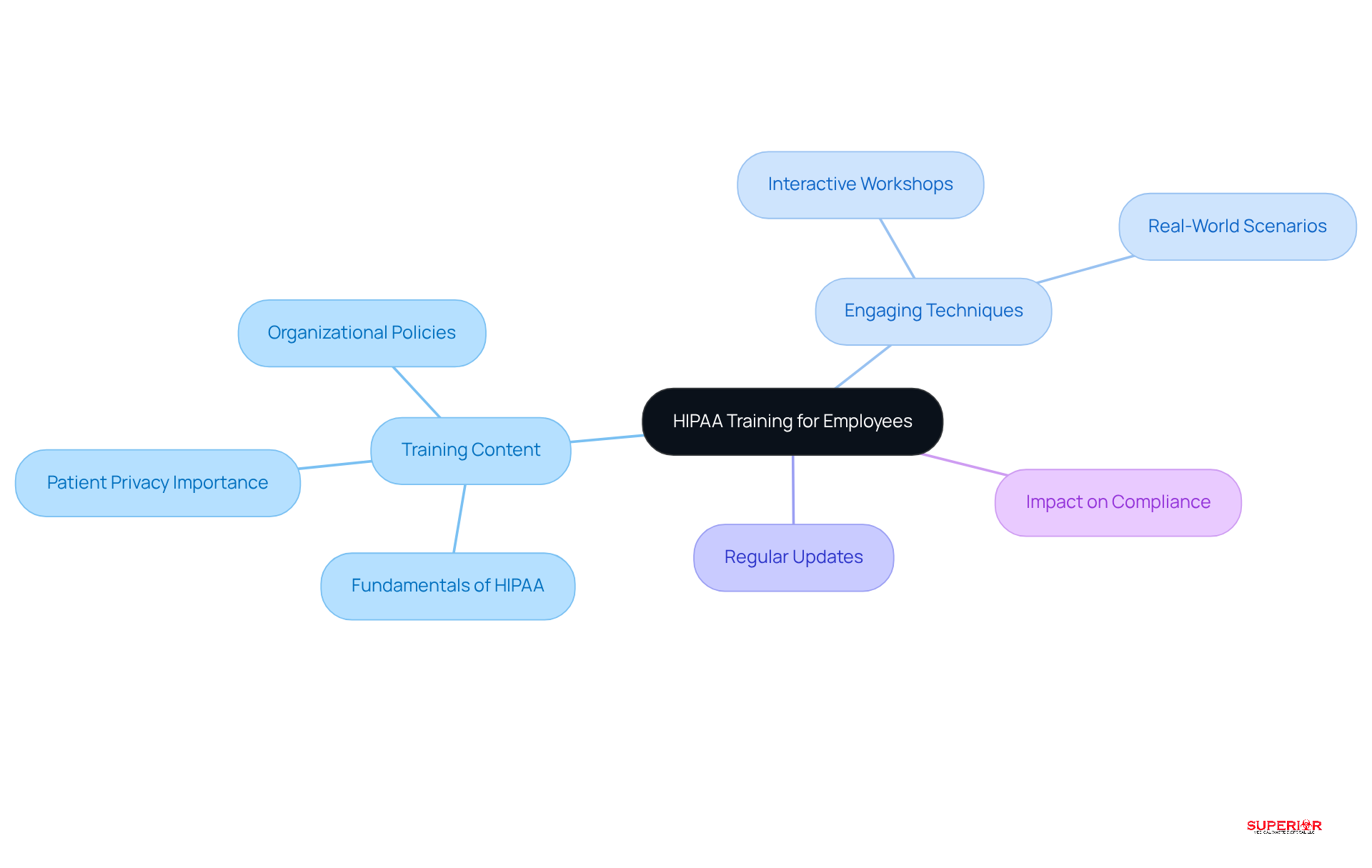
Regular training sessions on HIPAA regulations are crucial for all employees who handle protected health information (PHI). These sessions should cover the fundamentals of HIPAA, the policies, and the procedures of the organization. Engaging training techniques, such as interactive workshops and real-world scenarios, can significantly enhance staff engagement and knowledge retention.
Moreover, it is vital to update training materials to reflect any changes in regulations. This ensures that employees remain informed and compliant. Research indicates that a significant percentage of healthcare staff educated on HIPAA compliance leads to more effective practices, ultimately fostering a culture of adherence within the facility.
Develop and Enforce Compliance Policies
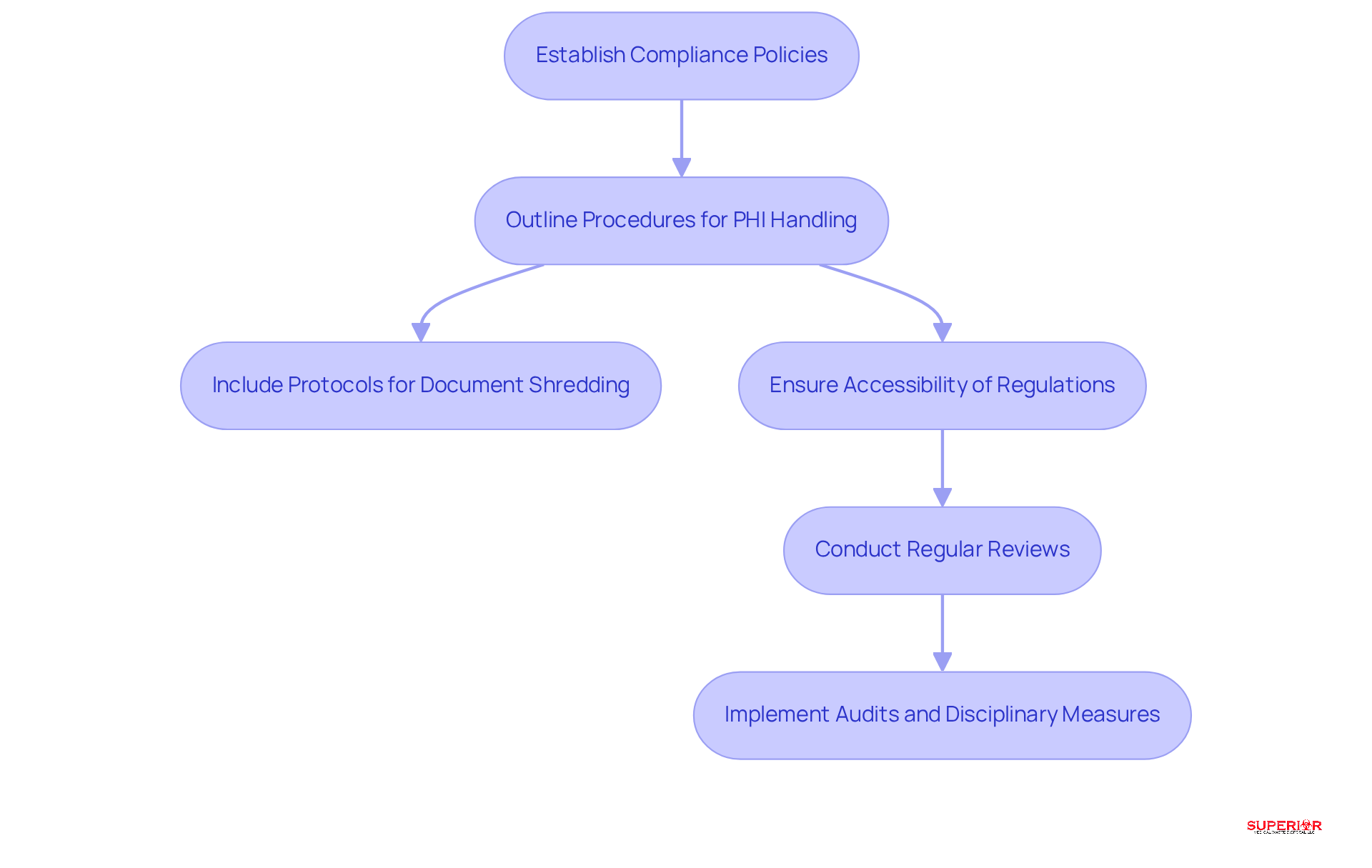
Healthcare facilities must establish comprehensive compliance policies that adhere to regulations, clearly outlining procedures for handling protected health information (PHI), reporting breaches, and ensuring data security. These policies should include specific protocols for risk management, also known as compliance training, monitoring, and enforcement, as safeguarding sensitive health data is essential. Information that must be shredded includes:
- Patient medical records
- Social security numbers
- Other identifiable health information such as birth dates
- Geographic identifiers
- Medical record numbers
Ensuring that regulations are easily accessible to all employees is crucial, along with regular reviews to confirm they remain current and effective. Enforcing adherence to compliance policies is vital; audits should be conducted, and disciplinary measures for non-adherence must be implemented to foster a culture of accountability and responsibility. Notably, around 37% of healthcare organizations perceive themselves as highly or extremely vulnerable to cyber threats in the upcoming 12 months, underscoring the need for strong security measures.
Moreover, making regulations accessible can significantly improve understanding and adherence among staff, ultimately enhancing compliance and decreasing the risk of costly breaches. As Rick Stevenson, a former Manager of Advisory Services, stated, “95% of regulatory staff have established or are establishing a culture of adherence to share the responsibility across their organization.”
Monitor and Audit Compliance Regularly
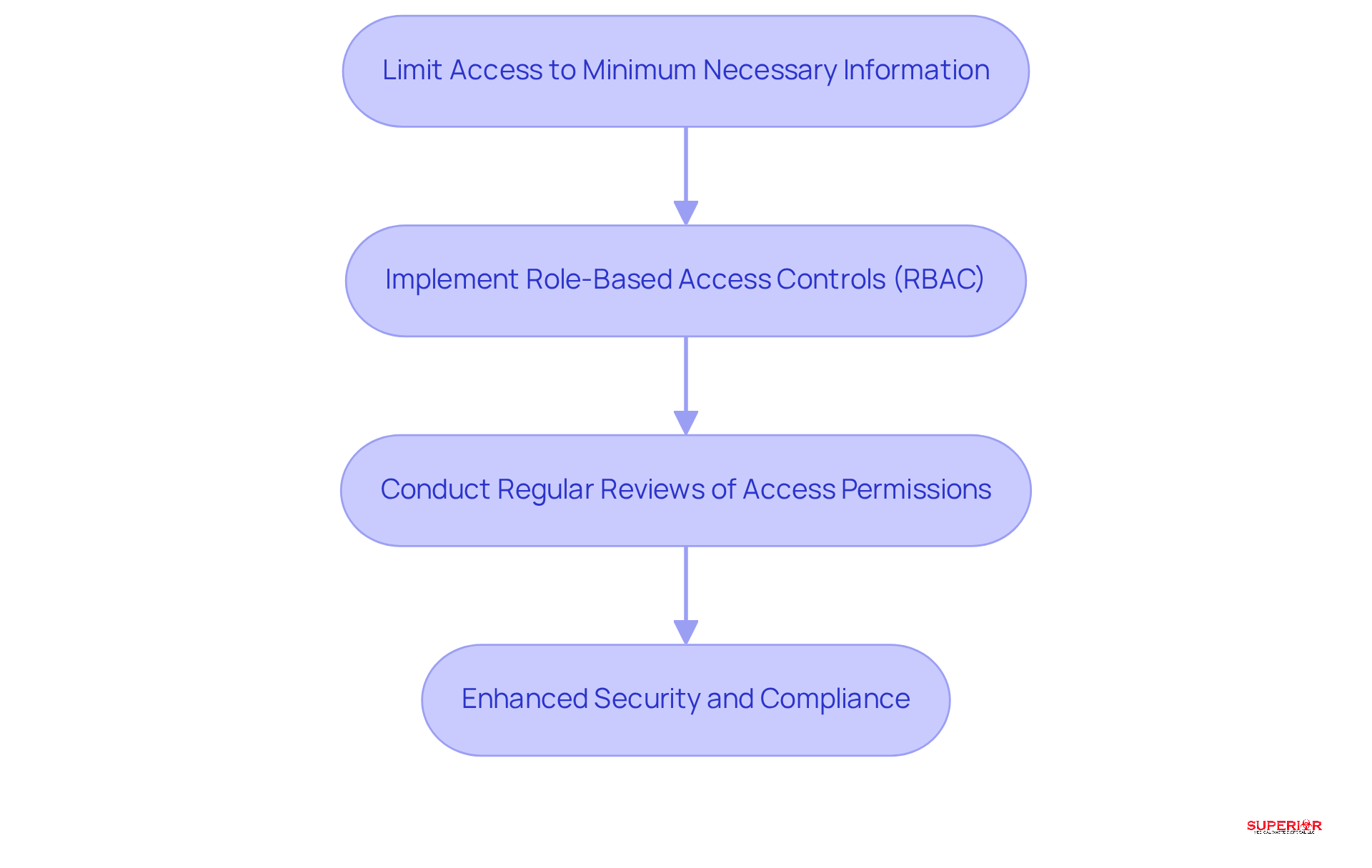
Regular monitoring and auditing of compliance processes are essential for identifying potential weaknesses in compliance. Establishing a timetable for audits allows for a thorough evaluation of adherence to policies and procedures, particularly regarding HIPAA regulations. Utilizing these audits enables necessary adjustments and improvements to be made.
In addition to internal audits, consider engaging external consultants for an objective assessment of your adherence status. This external perspective can provide valuable insights into compliance efforts.
It is crucial to recognize that paper shredding – also known as secure shredding or secured destruction – plays a vital role in protecting sensitive information, including patient medical records and personally identifiable information. Ensuring that all documents containing such data are securely shredded is a fundamental aspect of compliance and data protection.
Implement Physical Safeguards
Implementing robust physical safeguards is essential for protecting electronic Protected Health Information (ePHI) from unauthorized access. Notably, 75% of medical facilities prioritize physical security measures, which encompass access controls, surveillance systems, and alarms. For example, many facilities have adopted layered access controls enforced by badges, PINs, or biometrics to restrict entry to sensitive areas. Furthermore, areas where ePHI is stored must be accessible only to authorized personnel, ensuring that sensitive information remains secure.
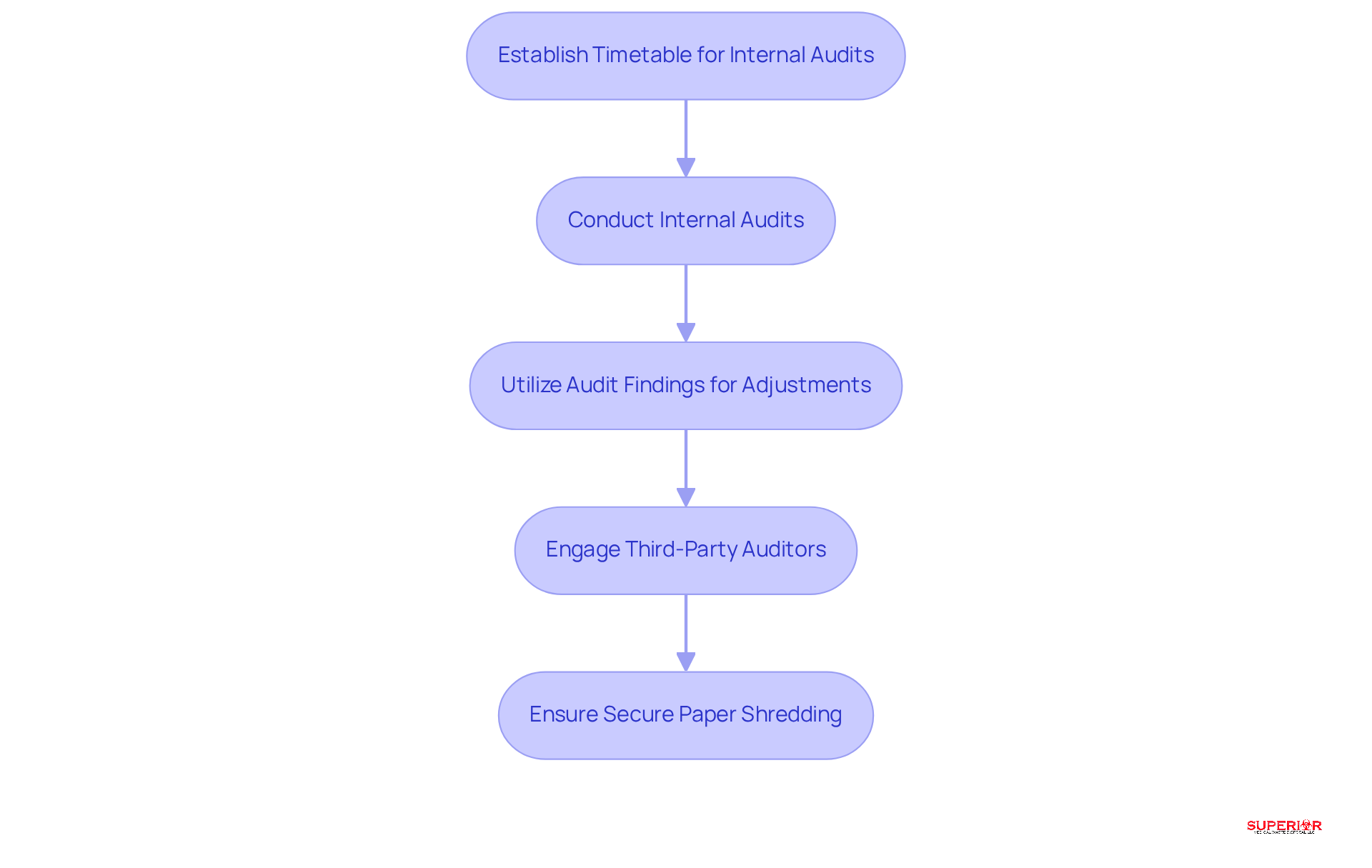
The HIPAA best practices for securing healthcare facilities involve:
- Establishing clear policies for the handling of ePHI.
- Utilizing secure document destruction services, such as those provided by shredding companies, which focuses on on-site shredding. Their procedure involves utilizing gray and white locking consoles to collect documents until they are shredded on-site, ensuring confidentiality.
- Employing data-wiping methods for hard drives to render details unrecoverable.
- Regular audits of access lists and prompt revocation of access for personnel changes to maintain security integrity.
- Training staff and conducting routine drills to significantly enhance compliance with HIPAA best practices and safeguard against potential breaches.
Limit Access to Minimum Necessary Information
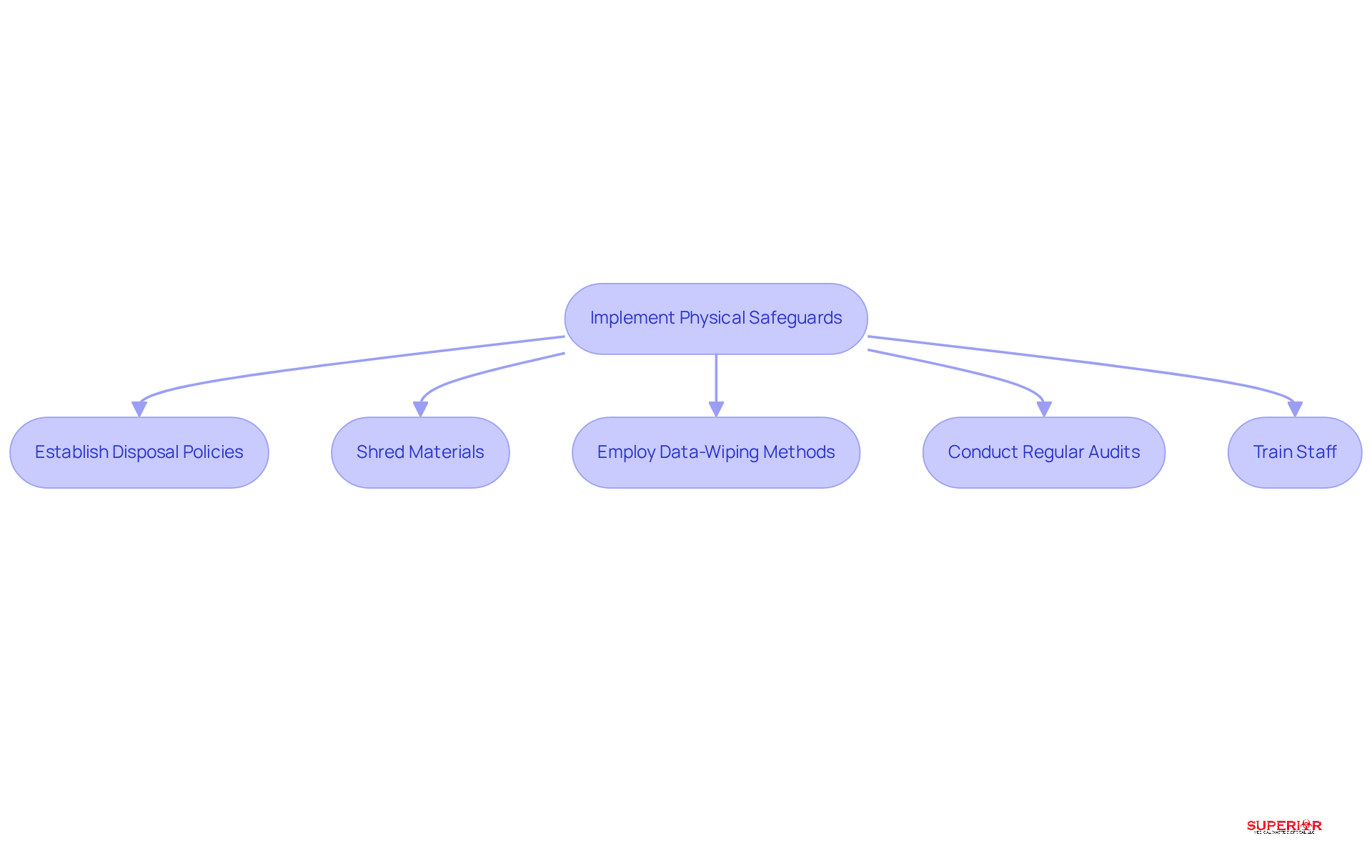
To comply with the regulations, healthcare facilities must restrict access to protected health information (PHI) to individuals whose job functions require it. Implementing role-based access control (RBAC) is essential for ensuring that employees can access only the information pertinent to their roles. This approach not only enhances security but also adheres to compliance standards.
Regular reviews of access permissions are crucial. Organizations should conduct these assessments at least quarterly to ensure that access remains appropriate and to adjust permissions as necessary. Studies indicate that medical facilities employing RBAC have experienced fewer data breaches, with many reporting improved accountability and a reduction in unauthorized access.
As of 2024, approximately 70% of healthcare organizations have adopted RBAC, reflecting its growing importance in safeguarding patient information. Given that medical breaches represented 32% of all documented U.S. data breaches from 2015 to 2022, and considering that the typical expense of a data breach is anticipated to reach $7.42 million in 2025, adopting RBAC not only adheres to regulations but also serves as a cost-reducing strategy.
Utilize Secure Document Destruction Services
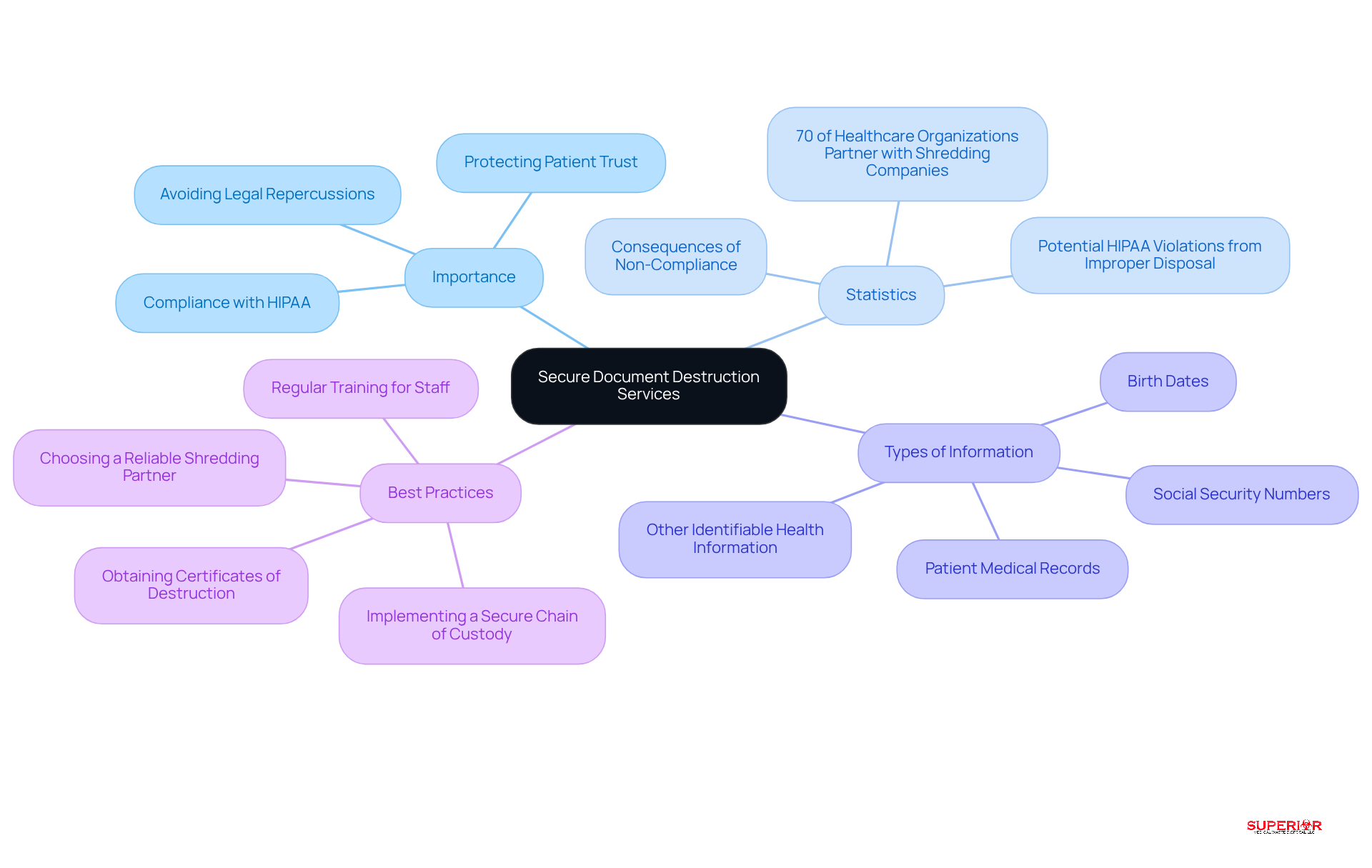
Reliable record elimination services are essential for medical establishments to ensure the proper disposal of confidential data. Approximately 70% of healthcare organizations partner with shredding companies to follow best practices. Terms such as secure information destruction, and compliance underscore the importance of protecting sensitive health information. When choosing a shredding partner, it is crucial to select those that provide a certificate of destruction, which serves as proof of compliance and can safeguard against potential audits.
Secure processes for physical materials are vital, as improper practices, like discarding items in the trash, can lead to violations of HIPAA regulations. Information that must be shredded includes:
- Patient medical records
- Social security numbers
- Birth dates
- Other identifiable health information
Furthermore, it is important to ensure that electronic records are securely wiped before disposal to prevent unauthorized access.
To bolster your facility’s compliance efforts, consider implementing regular training on the significance of HIPAA regulations. By adhering to best practices, medical facilities can foster a culture of accountability and professionalism, reinforcing their commitment to patient privacy and regulations while also protecting patient trust and the organization’s reputation.
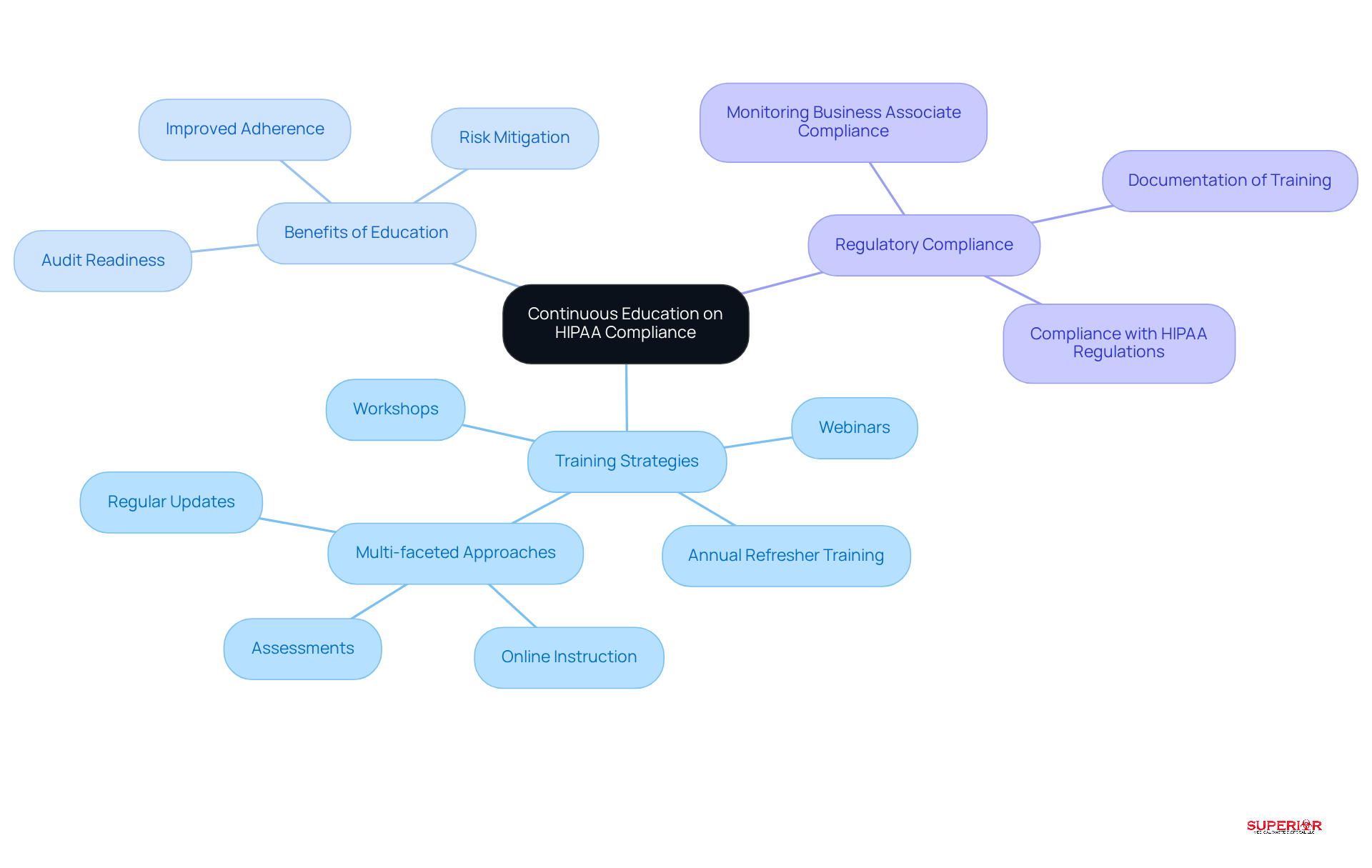
Ensure Continuous Education on HIPAA Compliance
Ongoing education on HIPAA compliance is crucial for keeping staff informed and engaged. A robust training program includes refresher courses; currently, over 90% of organizations provide training to staff handling protected health information (PHI). Encouraging participation in workshops, webinars, and conferences can significantly enhance staff knowledge and skills.
For instance, medical institutions that implement a blended learning approach – combining online instruction with assessments and frequent updates – have seen improved adherence and readiness for audits. This proactive approach not only strengthens understanding of HIPAA requirements but also helps to mitigate risks associated with data breaches and regulatory violations. Regular training is vital, as inadequate training is often cited in enforcement actions by the Department of Health and Human Services. By prioritizing continuous education, medical organizations can foster a culture of compliance among their workforce.
Moreover, integrating secure document destruction into your compliance strategy is essential. Whether on-site or off-site, these services ensure the proper disposal of sensitive data, effectively complying with HIPAA regulations and safeguarding patient privacy.
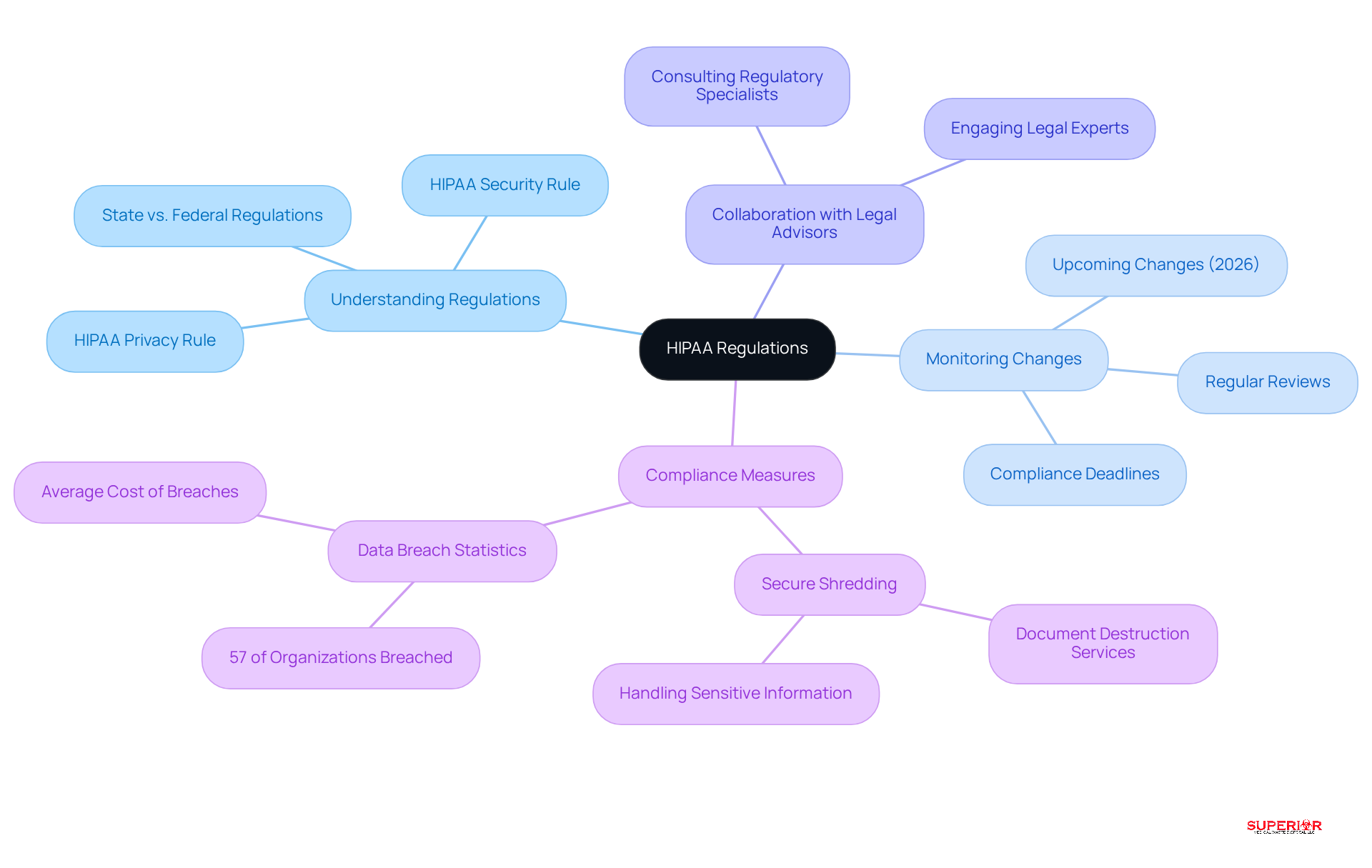
Understand State and Federal HIPAA Regulations
Healthcare facility administrators must have a thorough understanding of both state and federal regulations. This responsibility includes actively monitoring any changes or updates to the law, as the landscape of medical regulations is constantly evolving. Regular reviews of state-specific regulations are crucial, as these may impose stricter requirements than federal standards.
For instance, over 57% of healthcare organizations reported experiencing multiple data breaches in 2021. This statistic underscores the critical need for robust regulatory measures. Furthermore, in January 2026 new regulations make it essential for administrators to remain informed.
Collaboration with legal advisors or regulatory specialists is vital to ensure that your facility adheres to all relevant guidelines. This adherence not only protects patients but also minimizes the risk of legal penalties. A key aspect of compliance is the safeguarding of sensitive information, such as patient medical records, Social Security numbers, and other personally identifiable information.
Utilizing secure document destruction services, often referred to as shredding services, is essential for safeguarding patient privacy and ensuring compliance with HIPAA regulations.
Conclusion
In conclusion, implementing HIPAA best practices is crucial for healthcare facility administrators to safeguard patient information effectively. By prioritizing comprehensive risk analysis, technical safeguards, employee training, and robust compliance policies, facilities can significantly improve their adherence to HIPAA regulations. Continuous education and regular audits further solidify the foundation of a secure healthcare environment, fostering a culture of accountability and trust.
Key strategies include:
- Conducting thorough risk assessments
- Implementing multi-factor authentication
- Engaging in regular staff training
These are critical components for achieving compliance. Moreover, the significance of secure document destruction and a thorough understanding of both state and federal regulations cannot be overstated, as these elements are vital in protecting sensitive health information.
As healthcare regulations continue to evolve, it is imperative for administrators to remain vigilant and proactive in their compliance efforts. By adopting these best practices and cultivating a culture of security awareness, healthcare facilities can not only protect patient data but also enhance their reputation and operational integrity. Embracing these strategies will ensure compliance with current HIPAA standards and prepare organizations for future challenges in healthcare data security.
Frequently Asked Questions
Why is conducting a comprehensive risk analysis important for HIPAA compliance?
A comprehensive risk analysis is crucial for HIPAA compliance as it helps identify potential risks and vulnerabilities that could jeopardize the confidentiality, integrity, and availability of electronic protected health information (ePHI).
What percentage of medical organizations review their access controls annually?
Statistics indicate that only 57% of medical organizations review their access controls annually.
What tools should medical facilities use to conduct a HIPAA risk assessment?
Medical facilities should leverage tools and frameworks that align with HIPAA best practices recommended by the Department of Health and Human Services (HHS) to effectively conduct a HIPAA risk assessment.
What are some effective strategies for risk management in healthcare organizations?
Effective strategies include integrating risk assessments into routine operations, training all staff to recognize and mitigate risks, and regularly updating training materials to reflect evolving threats.
What are technical safeguards and why are they important?
Technical safeguards are essential for protecting ePHI and include encryption, robust access controls, and secure transmission protocols. They are important for ensuring that only authorized personnel can access sensitive information.
How can multi-factor authentication (MFA) enhance security in healthcare organizations?
Implementing multi-factor authentication (MFA) ensures that only authorized personnel can access systems that contain ePHI, thereby bolstering the security posture of medical organizations.
What recent trends highlight the need for enhanced protective measures in healthcare?
Recent trends indicate that 92% of medical institutions reported experiencing at least one cyberattack in the past year, underscoring the urgent need for enhanced protective measures.
What role do regular software and system updates play in cybersecurity?
Regular software and system updates are vital for mitigating vulnerabilities and ensuring that healthcare facilities maintain a proactive security strategy against cyber threats.
Why is training employees on HIPAA regulations essential?
Regular training sessions on HIPAA best practices are crucial for all employees handling protected health information (PHI) to ensure they understand the importance of patient privacy and comply with regulations.
How can training techniques be improved for better engagement?
Engaging training techniques, such as interactive workshops and real-world scenarios, can significantly enhance staff engagement and knowledge retention regarding HIPAA best practices.
List of Sources
- Conduct Comprehensive Risk Analysis
- HIPAA Training Requirements for 2026: Complete Compliance Guide (https://thehipaaetool.com/the-hipaa-e-tool-the-complete-guide-to-hipaa-training-requirements-for-2026)
- Healthcare Data Breach Statistics (https://hipaajournal.com/healthcare-data-breach-statistics)
- 2024 HIPAA Trends and Statistics (https://securitymetrics.com/blog/2024-hipaa-trends)
- hipaavault.com (https://hipaavault.com/resources/2026-hipaa-changes)
- OCR’s Latest HIPAA Guidance: Strategic Measures to Protect Your Systems and Data (https://bakerdonelson.com/ocrs-latest-hipaa-guidance-strategic-measures-to-protect-your-systems-and-data)
- Implement Technical Safeguards
- Healthcare Data Breach Statistics (https://hipaajournal.com/healthcare-data-breach-statistics)
- 38 Must-Know Healthcare Cybersecurity Stats (https://varonis.com/blog/healthcare-cybersecurity-statistics)
- Healthcare Cybersecurity Statistics 2024 (https://ispartnersllc.com/blog/healthcare-cybersecurity-statistics)
- Healthcare Data Breach Statistics: HIPAA Violation Cases and Preventive Measures in 2025 (https://sprinto.com/blog/healthcare-data-breach-statistics)
- 51 HIPAA Statistics Every Healthcare Entity Needs to Know in 2026 | UpGuard (https://upguard.com/blog/hipaa-statistics)
- Train Employees on HIPAA Regulations
- HIPAA Training for Healthcare Workers: What’s Required and Why It Matters – Clinical Gate HIPAA Training for Healthcare Workers in 2026 (https://clinicalgate.com/hipaa-training-for-healthcare-workers-whats-required-and-why-it-matters)
- More than half of employees don’t understand HIPAA rules | Medical Economics (https://medicaleconomics.com/view/more-than-half-of-employees-don-t-understand-hipaa-rules)
- HIPAA Training for Employees – Updated for 2026 (https://hipaajournal.com/hipaa-training-for-employees)
- hipaajournal.com (https://hipaajournal.com/hipaa-training-for-healthcare-workers)
- hipaajournal.com (https://hipaajournal.com/hipaa-training-requirements)
- Develop and Enforce Compliance Policies
- 51 HIPAA Statistics Every Healthcare Entity Needs to Know in 2026 | UpGuard (https://upguard.com/blog/hipaa-statistics)
- 115 Compliance Statistics You Need To Know in 2023 – Drata (https://drata.com/blog/compliance-statistics)
- Healthcare Compliance Trends & Statistics (https://ispartnersllc.com/blog/healthcare-compliance-trends)
- Healthcare Compliance News (https://hipaajournal.com/category/healthcare-compliance)
- Monitor and Audit Compliance Regularly
- 115 Compliance Statistics You Need To Know in 2023 – Drata (https://drata.com/blog/compliance-statistics)
- Healthcare Compliance Trends & Statistics (https://ispartnersllc.com/blog/healthcare-compliance-trends)
- Respond Effectively to Healthcare Audits and Investigations | University of Miami School of Law (https://news.miami.edu/law/stories/2026/01/respond-effectively-to-healthcare-audits-and-investigations.html)
- HIPAA Statistics (https://compliancy-group.com/hipaa-statistics)
- 130+ Compliance Statistics & Trends to Know for 2026 (https://secureframe.com/blog/compliance-statistics)
- Implement Physical Safeguards
- Healthcare Data Breach Statistics (https://hipaajournal.com/healthcare-data-breach-statistics)
- scoop.market.us (https://scoop.market.us/physical-security-statistics)
- HIPAA Physical Safeguards for PHI: Requirements, Examples, and Best Practices (https://accountablehq.com/post/hipaa-physical-safeguards-for-phi-requirements-examples-and-best-practices)
- 38 Must-Know Healthcare Cybersecurity Stats (https://varonis.com/blog/healthcare-cybersecurity-statistics)
- 51 HIPAA Statistics Every Healthcare Entity Needs to Know in 2026 | UpGuard (https://upguard.com/blog/hipaa-statistics)
- Limit Access to Minimum Necessary Information
- Healthcare Data Breach Statistics (https://hipaajournal.com/healthcare-data-breach-statistics)
- Healthcare Data Breach Statistics: HIPAA Violation Cases and Preventive Measures in 2025 (https://sprinto.com/blog/healthcare-data-breach-statistics)
- How Role-Based Controls Protect Patient Data | Censinet, Inc. (https://censinet.com/perspectives/how-role-based-controls-protect-patient-data)
- ROLE-BASED ACCESS CONTROL (RBAC) IMPLEMENTATION FOR SOC 2 & HIPAA (https://certpro.com/role-based-access-control)
- Best Practices for HIPAA Privacy Officers Managing EMR Access, Audits, and Breaches (https://accountablehq.com/post/best-practices-for-hipaa-privacy-officers-managing-emr-access-audits-and-breaches)
- Utilize Secure Document Destruction Services
- appliedinnovation.com (https://appliedinnovation.com/shredding-services/how-to-avoid-a-hipaa-violation-with-secure-document-shredding)
- Document Shredding in the Healthcare Industry (https://danielshealth.com/knowledge-center/document-shredding-healthcare-industry)
- HIPAA-Compliant Healthcare Shredding Services | Shred-it USA (https://shredit.com/en-us/who-we-serve/healthcare)
- The Heartbeat Of Confidentiality: Why Document Shredding Is Vital In Healthcare – The Shred Truck (https://theshredtruck.com/news/the-heartbeat-of-confidentiality-why-document-shredding-is-vital-in-healthcare)
- Why a Secure Shredding Service Is Critical to Healthcare Compliance (https://shredit.com/en-us/resource-center/info-sheets/why-a-secure-shredding-service-is-critical-to-healthcare-complia)
- Ensure Continuous Education on HIPAA Compliance
- 2024 HIPAA Trends and Statistics (https://securitymetrics.com/blog/2024-hipaa-trends)
- HIPAA (https://ama-assn.org/practice-management/hipaa)
- Survey Finds Over 90% of Organizations Now Provide Annual HIPAA Refresher Training (https://hipaajournal.com/over-90-of-organizations-now-provide-annual-hipaa-refresher-training)
- HIPAA Training Trends (https://securitymetrics.com/learn/hipaa-training-trends)
- Looking for HIPAA Compliance Quotes? (https://compliancy-group.com/hipaa-compliance-quotes)
- Understand State and Federal HIPAA Regulations
- HIPAA Updates and HIPAA Changes in 2026 (https://hipaajournal.com/hipaa-updates-hipaa-changes)
- Understanding HIPAA healthcare statistics (https://hipaatimes.com/understanding-hipaa-healthcare-statistics)
- Looking for HIPAA Compliance Quotes? (https://compliancy-group.com/hipaa-compliance-quotes)
- HIPAA Enforcement Statistics | CMS (https://cms.gov/priorities/key-initiatives/burden-reduction/administrative-simplification/enforcement/hipaa-statistics)
- Navigating State vs. HIPAA Regulations: Overriding Inconsistencies Explained (https://accountablehq.com/post/navigating-state-vs-hipaa-regulations-overriding-inconsistencies-explained)
