Introduction
The management of surgical waste is a critical component of healthcare operations that demands immediate attention, posing significant risks to both staff and patients.
With stringent regulations and the potential for severe penalties looming, healthcare facilities must adopt best practices to ensure safe and compliant waste disposal.
Organizations must adopt comprehensive strategies to navigate the complexities of surgical waste management while fostering a culture of safety and compliance.
This article explores essential strategies and practices that safeguard health and enhance operational efficiency amidst stringent regulatory requirements.
Define Surgical Waste: Understanding Types and Regulations
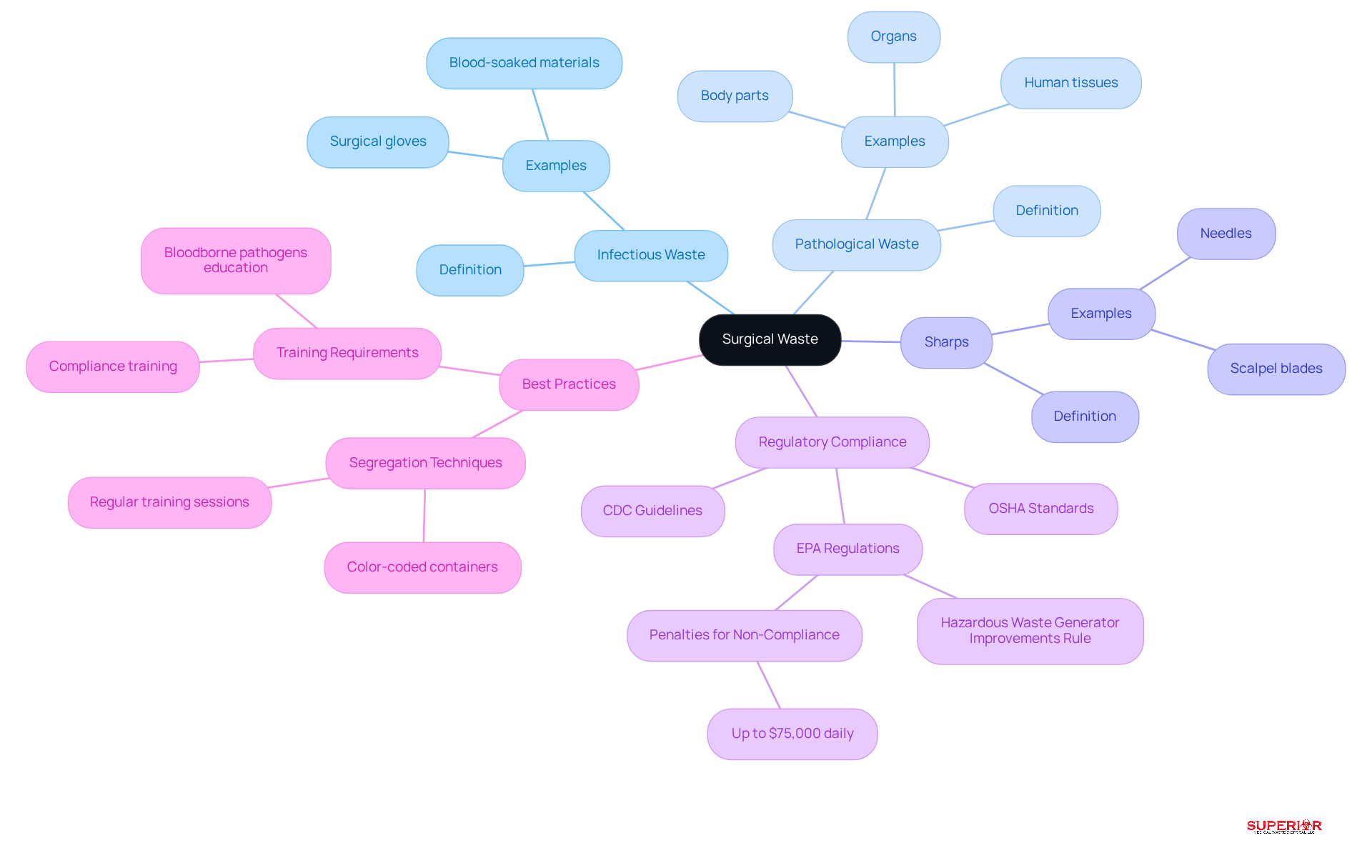
Surgical waste disposal includes a variety of materials generated during surgical procedures, necessitating precise categorization to ensure compliance with regulatory standards. This refuse includes sharps, pathological substances, and contaminated items. Accurate categorization is essential to comply with regulations set forth by organizations such as OSHA and the CDC. Common categories include:
- Infectious Waste: Waste that may contain pathogens, such as blood-soaked materials and surgical gloves.
- Pathological Waste: Human tissues, organs, and body parts removed during surgery.
- Sharps: Items that can puncture or cut skin, including needles and scalpel blades.
Recent statistics indicate that approximately 85% of surgical refuse falls into the categories of infectious, pathological, or sharps. This underscores the critical need for medical facilities to implement effective segregation practices. Failure to adhere to these regulations can lead to significant legal repercussions and jeopardize the safety of medical staff and patients. Facilities must remain vigilant regarding changing regulations, including the recent amendments to the Hazardous Generator Improvements Rule finalized by the EPA in December 2024, which emphasize reduction and tracking protocols. Furthermore, medical practitioners should be aware that fines for medical refuse non-compliance in 2026 can be severe, with federal EPA infractions carrying penalties of up to $75,000 daily. Medical personnel must receive thorough training on disposal management practices, including education on bloodborne pathogens, to minimize exposure risks and ensure compliance. Implementing best practices for refuse segregation, like utilizing color-coded containers and conducting regular training sessions, enables medical centers to uphold high standards in refuse management.
Comply with Regulations: Navigating Legal Requirements for Disposal
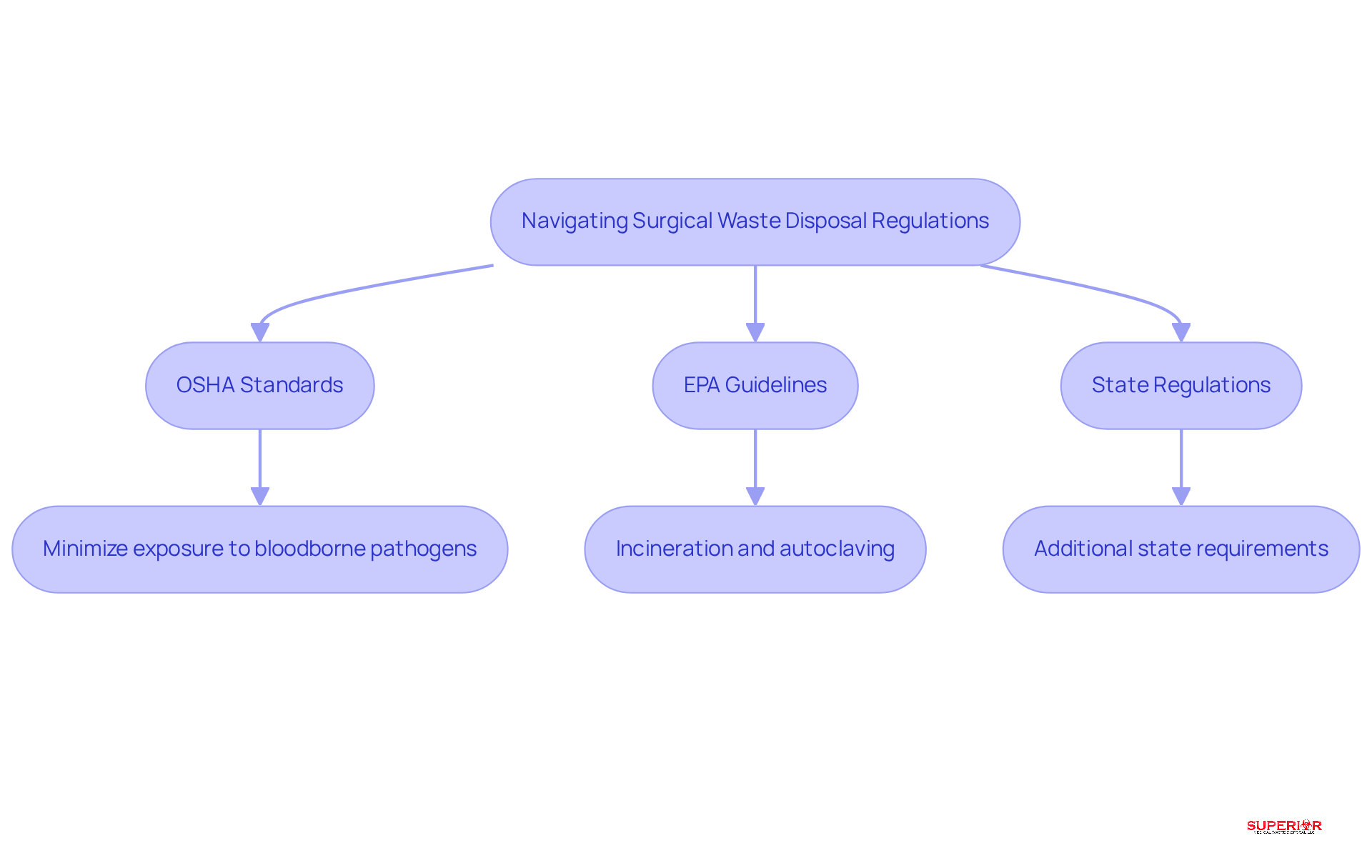
Healthcare facilities face significant challenges in navigating the intricate regulations surrounding surgical waste disposal. Key regulations include:
- OSHA Standards: These standards mandate that all medical waste be managed in a way that minimizes exposure to bloodborne pathogens, ensuring the safety of healthcare workers and patients alike.
- EPA Guidelines: The Environmental Protection Agency provides clear directives on the disposal of hazardous materials, recommending methods such as incineration and autoclaving to mitigate environmental impact and health risks, while also emphasizing the importance of protecting communities from PFAS exposure.
- State Regulations: Individual states may impose additional requirements that healthcare establishments must adhere to, reflecting local health and safety priorities.
Navigating these regulations can be challenging for healthcare facilities, often leading to compliance issues. Facilities need to conduct regular audits and stay informed about any changes in regulations, especially as numerous jurisdictions are anticipated to shift to required electronic reporting for refuse tracking by late 2026. Collaborating with certified surgical waste disposal companies, such as Superior Medical Waste Disposal, is essential for effective waste management. Our broad network of collaborations with prominent entities in the medical field boosts our knowledge and dedication to regulatory adherence and environmental sustainability. By implementing a robust regulatory management system, organizations can not only meet their legal obligations but also enhance their operational effectiveness and community trust.
Implement Segregation Practices: Safeguarding Against Contamination
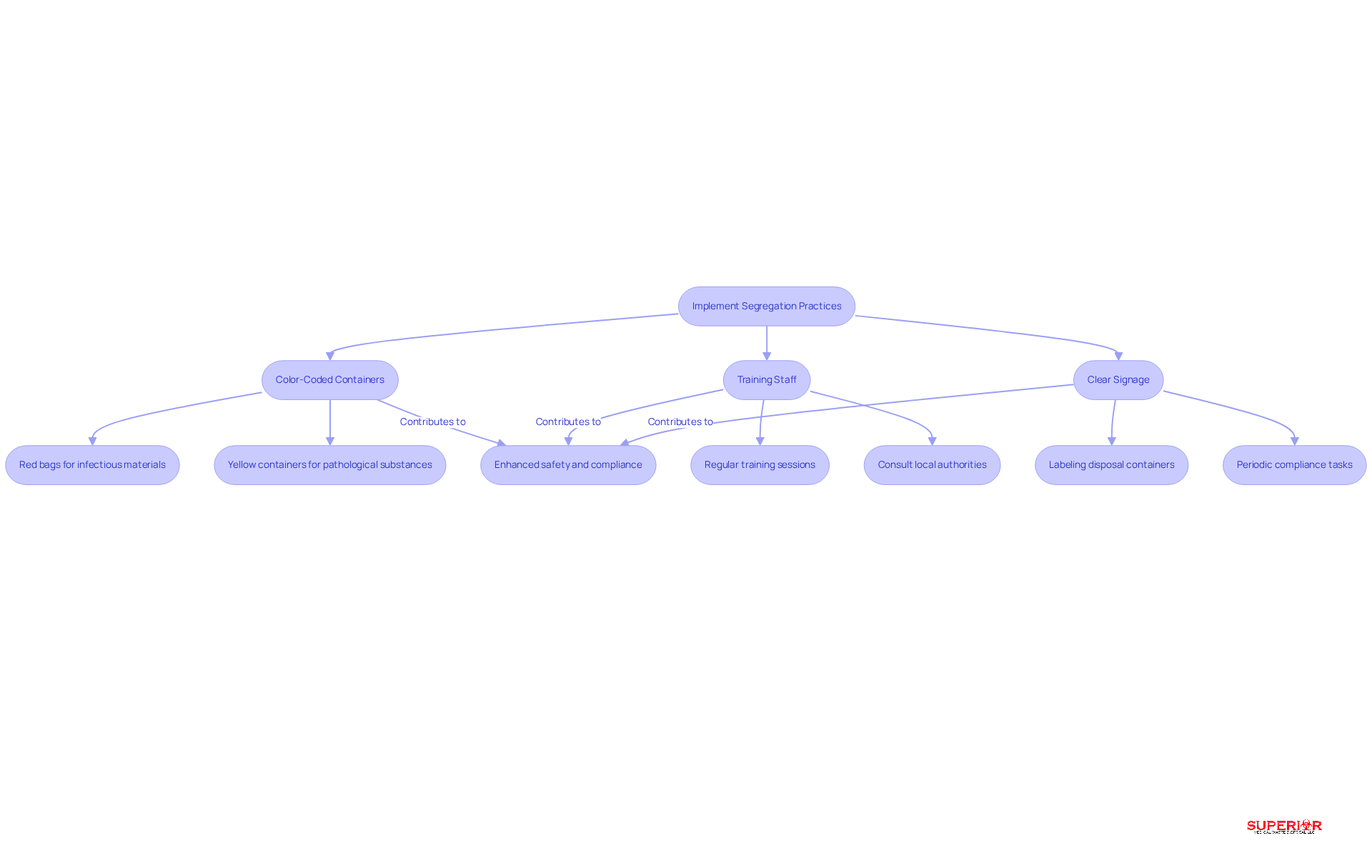
Effective segregation of refuse, particularly surgical waste disposal, is not just a regulatory requirement; it is a critical component of patient and staff safety in healthcare environments. To enhance compliance and safety, facilities should adopt the following best practices:
- Color-Coded Containers: Implement a system of distinct containers for various waste types. For example, red bags are assigned for infectious materials, while yellow containers are utilized for pathological substances. Color-coding serves as a clear visual cue, helping staff understand how to handle each type of waste, which reduces the chances of contamination and disposal errors. Red biohazard containers are especially significant, as they are utilized for regulated medical refuse, which includes items tainted with blood or potentially infectious materials.
- Training Staff: Without comprehensive training programs, personnel may struggle to comply with waste segregation requirements. Training employees on the importance of separating materials and the particular methods for disposing of various types can greatly enhance adherence rates. Regular training sessions ensure that employees are aware of the latest regulations and best practices, fostering a culture of safety and responsibility. With potential penalties reaching $75,000 per day for EPA violations, understanding compliance is more crucial than ever for healthcare facilities. Furthermore, it is essential to consult local environmental authorities concerning specific regulations and handling procedures for biohazard materials, as these can differ by state.
- Clear Signage: Ensure that disposal containers are clearly labeled with appropriate signage. This guidance assists staff in swiftly recognizing the appropriate disposal methods, emphasizing the significance of proper management protocols. When signage is clear and color-coded systems are in place, staff can quickly identify how to dispose of waste, reducing the likelihood of errors. Moreover, periodic compliance tasks, such as reviewing manifests and treatment records, are essential to ensure that disposal management practices align with regulatory requirements. At Superior Medical Waste Disposal, we utilize autoclaving and shredding processes to treat biohazard materials, reducing its volume by 70% before disposal, which exemplifies our commitment to efficient and compliant management.
Prioritizing refuse segregation not only minimizes contamination risks but also enhances surgical waste disposal, creating a safer environment for everyone involved. For example, a local Traverse City medical center applied these best practices and noted a 50% decrease in disposal errors within the first year. Furthermore, as the industry shifts to electronic refuse tracking (e-Manifest), staying informed about technological advancements will be essential for ensuring compliance.
Ensure Proper Packaging and Labeling: Enhancing Safety in Transport
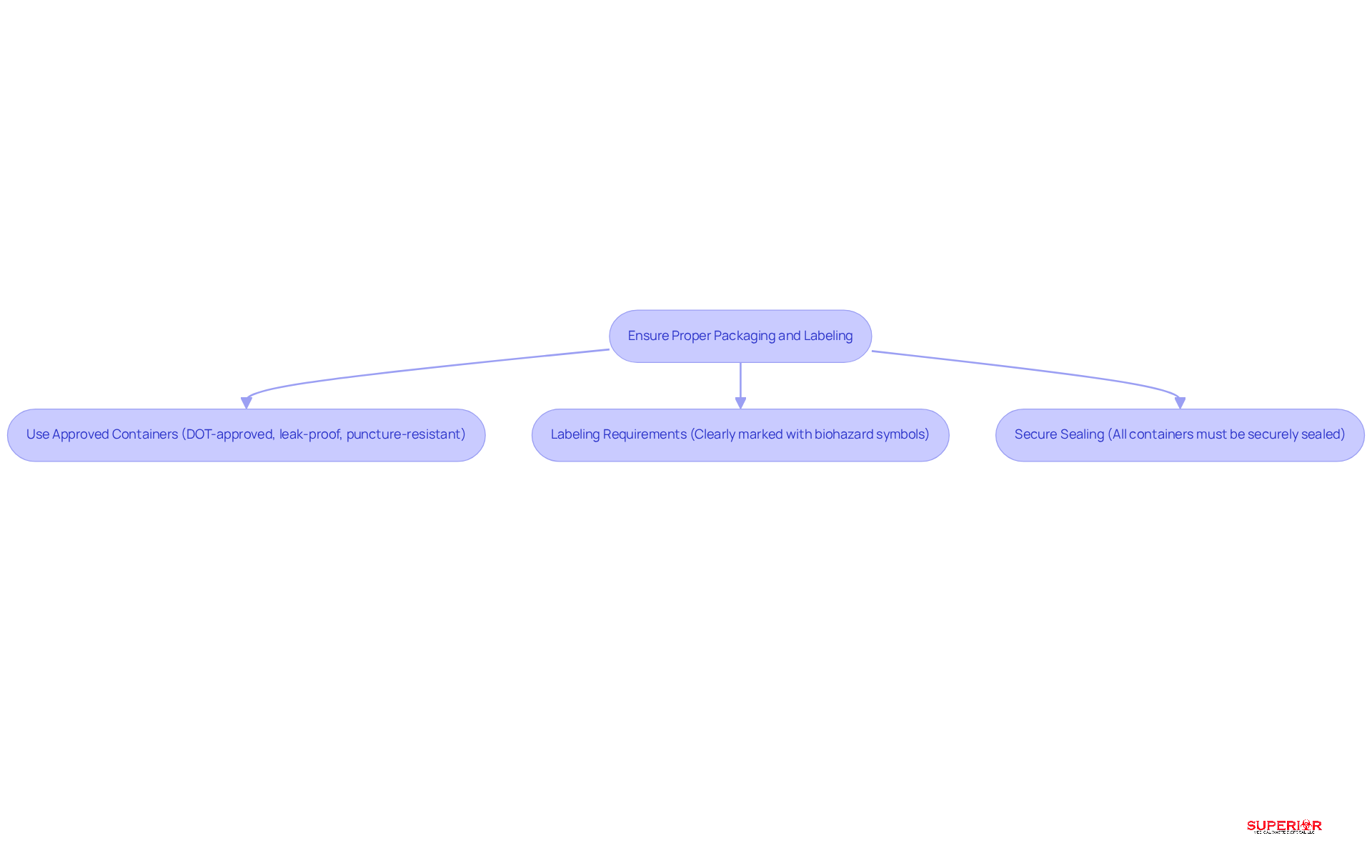
Improper surgical waste disposal poses significant risks to both healthcare workers and the environment. To ensure the safe transport of surgical waste, healthcare facilities must adhere to stringent packaging and labeling guidelines:
- Use Approved Containers: All surgical waste must be placed in DOT-approved containers that are both leak-proof and puncture-resistant. Using these containers is crucial for keeping transport safe and protecting the environment from contamination.
- Labeling Requirements: Each container must be clearly marked with the appropriate biohazard symbols and type of material. This labeling informs handlers of the contents, ensuring proper handling and adherence to safety protocols.
- Secure Sealing: It is crucial that all containers are securely sealed to prevent leaks during transport. Proper sealing not only protects staff but also safeguards the environment from potential dangers associated with medical refuse.
Adhering to these guidelines ensures compliance with regulations and protects both medical staff and the community from the risks of improper surgical waste disposal.
Train Staff Effectively: Building a Culture of Compliance and Safety
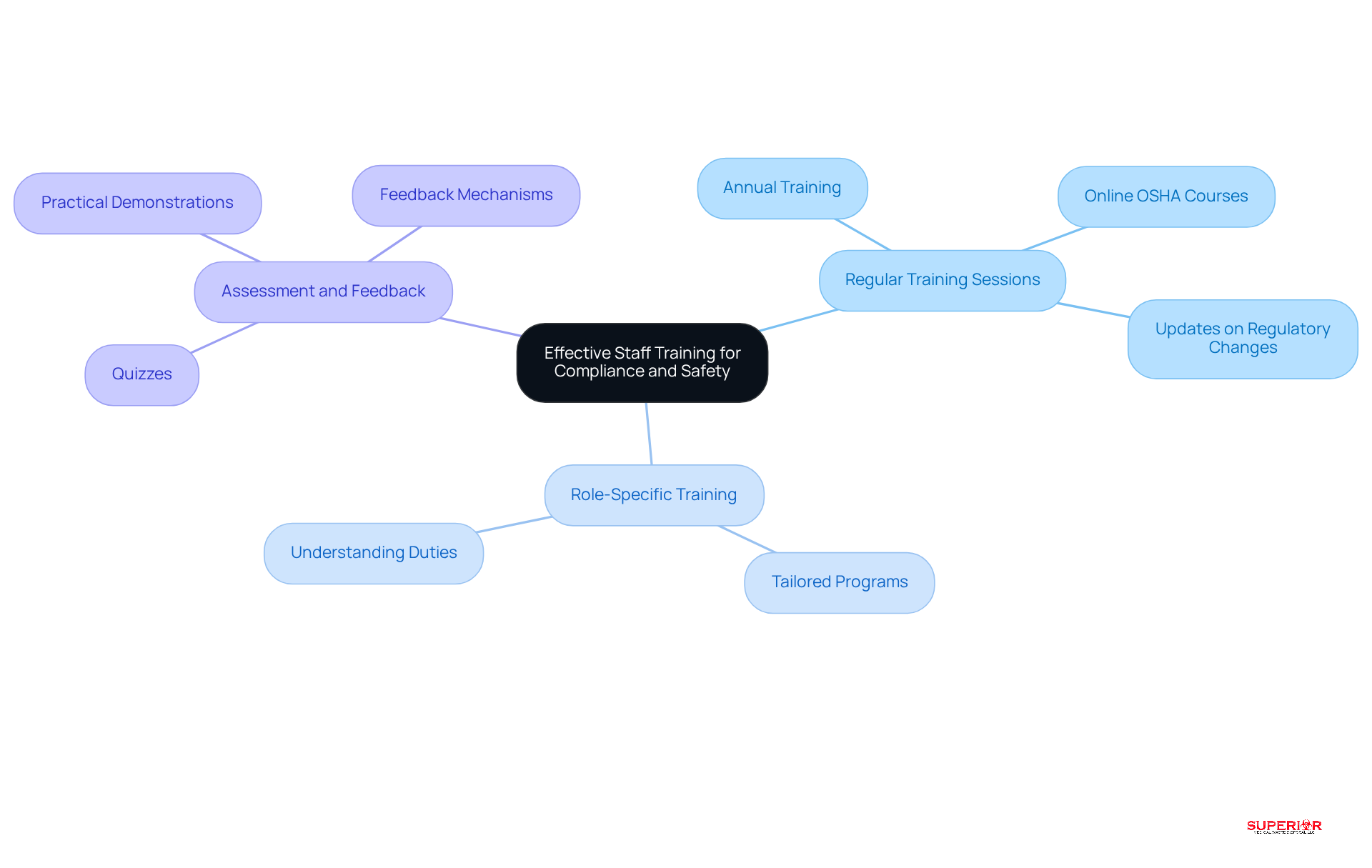
Effective management of surgical waste disposal hinges on comprehensive training within medical facilities. To optimize compliance and safety, the following strategies should be implemented:
- Regular Training Sessions: Conduct training sessions at least annually to ensure staff are informed about best practices and any regulatory changes. Ongoing education is essential. Medical disposal regulations change frequently, which requires updates to training resources and techniques. Superior Medical Waste Disposal offers comprehensive online OSHA training courses that cover essential topics such as HIPAA, BBP, and RMW, ensuring your team is well-prepared across various industries, including dental practices, physician’s offices, and more.
- Role-Specific Training: Tailor training programs to the specific roles of staff members. This guarantees that every person comprehends their duties concerning surgical waste disposal, which is essential for upholding regulations and minimizing hazards related to incorrect disposal.
- Assessment and Feedback: Regularly assess staff knowledge through quizzes or practical demonstrations. Providing feedback reinforces learning and helps identify knowledge gaps, allowing for targeted improvements in training effectiveness.
When you invest in comprehensive training programs, you’re fostering a culture of safety and adherence in your healthcare facility, which significantly reduces the risk of improper surgical waste disposal. Facilities that prioritize continuous improvement in their training programs often see enhanced compliance rates and a safer working environment. Ultimately, prioritizing training can transform compliance into a proactive culture of safety and responsibility.
Conclusion
Effective surgical waste disposal practices are essential for healthcare facilities, impacting both compliance and safety. By understanding surgical waste types and following strict disposal guidelines, facilities can reduce risks from improper management. Categorization, compliance, and training are critical for effective waste management, forming the backbone of a successful strategy.
Throughout this article, key strategies have been highlighted, including the necessity of proper segregation of waste, adherence to legal requirements, and the implementation of robust training programs. Utilizing color-coded containers, conducting regular staff training, and ensuring proper packaging and labeling of waste are essential steps in fostering a culture of safety and compliance. As healthcare regulations continue to evolve, staying informed and prepared is vital for minimizing legal repercussions and enhancing operational effectiveness.
In conclusion, the management of surgical waste is not merely a regulatory obligation but a critical aspect of healthcare that impacts community health and safety. When healthcare facilities prioritize effective waste disposal, they not only protect their staff but also earn the trust of their communities. Prioritizing surgical waste management not only fulfills regulatory requirements but also safeguards community health and enhances patient care.
Frequently Asked Questions
What is surgical waste?
Surgical waste includes various materials generated during surgical procedures, such as sharps, pathological substances, and contaminated items that require precise categorization for compliance with regulatory standards.
What are the main categories of surgical waste?
The main categories of surgical waste include: – Infectious Waste: Materials that may contain pathogens, like blood-soaked items and surgical gloves. – Pathological Waste: Human tissues, organs, and body parts removed during surgery. – Sharps: Items that can puncture or cut skin, including needles and scalpel blades.
What percentage of surgical waste falls into the main categories?
Approximately 85% of surgical waste falls into the categories of infectious, pathological, or sharps.
Why is accurate categorization of surgical waste important?
Accurate categorization is essential to comply with regulations from organizations like OSHA and the CDC, and failure to adhere can lead to legal repercussions and jeopardize the safety of medical staff and patients.
What recent changes have been made to regulations regarding surgical waste?
The Hazardous Generator Improvements Rule finalized by the EPA in December 2024 emphasizes reduction and tracking protocols for surgical waste management.
What penalties can healthcare facilities face for non-compliance with surgical waste regulations?
Fines for non-compliance can be severe, with federal EPA infractions potentially carrying penalties of up to $75,000 daily starting in 2026.
What training should medical personnel receive regarding surgical waste disposal?
Medical personnel should receive thorough training on disposal management practices, including education on bloodborne pathogens to minimize exposure risks and ensure compliance.
What best practices can medical centers implement for surgical waste management?
Best practices include utilizing color-coded containers for waste segregation and conducting regular training sessions for staff.
What are the key regulations healthcare facilities must follow for surgical waste disposal?
Key regulations include: – OSHA Standards: Mandating management of medical waste to minimize exposure to bloodborne pathogens. – EPA Guidelines: Providing directives on hazardous material disposal, recommending methods like incineration and autoclaving. – State Regulations: Additional requirements imposed by individual states reflecting local health and safety priorities.
How can healthcare facilities effectively navigate surgical waste regulations?
Facilities should conduct regular audits, stay informed about regulatory changes, and collaborate with certified surgical waste disposal companies for effective waste management.
List of Sources
- Define Surgical Waste: Understanding Types and Regulations
- Regulatory Updates in Medical Waste Management | ASMAI (https://asiwaste.com/medical-waste/regulatory-updates-in-medical-waste-management)
- Navigating Recent Regulations in Medical Waste Management: A Guide for Healthcare Providers – Onsite Waste (https://onsitewaste.com/navigating-recent-regulations-in-medical-waste-management-a-guide-for-healthcare-providers)
- 2026 Medical Waste Compliance Guide: 2025 Reg Changes & Beyond (https://sdmedwaste.com/post/healthcare-waste-regulations-compliance-guide)
- Medical Waste Disposal in 2026: Federal Foundations, State Authority, and Compliance Requirements (https://linkedin.com/pulse/medical-waste-disposal-2026-federal-foundations-state-authority-vim3c)
- Hospital Waste Disposal in 2026: Complete Compliance Guide for Healthcare Facilities (https://medprodisposal.com/hospital-waste-disposal-2026-compliance-guide)
- Comply with Regulations: Navigating Legal Requirements for Disposal
- Facts and Figures about Materials, Waste and Recycling | US EPA (https://epa.gov/facts-and-figures-about-materials-waste-and-recycling)
- 2026 Medical Waste Compliance Guide: 2025 Reg Changes & Beyond (https://sdmedwaste.com/post/healthcare-waste-regulations-compliance-guide)
- Medical Waste Disposal in 2026: Federal Foundations, State Authority, and Compliance Requirements (https://linkedin.com/pulse/medical-waste-disposal-2026-federal-foundations-state-authority-vim3c)
- EPA updates PFAS destruction and disposal guidance (https://wastetodaymagazine.com/news/epa-updates-pfas-destruction-and-disposal-guidance)
- Fact Sheet for the 2026 Interim Guidance on the Destruction and Disposal of PFAS | US EPA (https://epa.gov/pfas/fact-sheet-2026-interim-guidance-destruction-and-disposal-pfas)
- Implement Segregation Practices: Safeguarding Against Contamination
- Hospital Waste Disposal in 2026: Complete Compliance Guide for Healthcare Facilities (https://medprodisposal.com/hospital-waste-disposal-2026-compliance-guide)
- A Smarter Start to 2026: Simplifying Medical Waste Compliance in the New Year – Waste Medic (https://wastemedic.com/2026/01/07/a-smarter-start-to-2026-simplifying-medical-waste-compliance-in-the-new-year-2)
- What Biohazard Waste Container Colors Mean (And Why It Matters) (https://appliedinnovation.com/health-services/what-biohazard-waste-container-colors-mean-and-why-it-matters)
- 2026 Medical Waste Compliance Guide: 2025 Reg Changes & Beyond (https://sdmedwaste.com/post/healthcare-waste-regulations-compliance-guide)
- Ensure Proper Packaging and Labeling: Enhancing Safety in Transport
- Biohazard Waste Disposal Services: 2026 Federal and State Compliance Requirements (https://medprodisposal.com/biohazard-waste-disposal-2026-compliance-requirements)
- Hospital Waste Disposal in 2026: Complete Compliance Guide for Healthcare Facilities (https://medprodisposal.com/hospital-waste-disposal-2026-compliance-guide)
- 2026 Medical Waste Regulation Changes Every Healthcare Facility Needs to Know Before It’s Too Late (https://medprodisposal.com/2026-medical-waste-regulation-changes-guide)
- Medical Waste & Infectious Substances Transportation Medical Waste & Infectious Substances Transportation (https://highways.today/2025/09/19/medical-waste-transportation)
- Train Staff Effectively: Building a Culture of Compliance and Safety
- Essentials of Regulated Waste Disposal Training (https://stericycle.com/en-us/resource-center/blog/training-staff-about-regulated-medical-waste)
- Assessing Effectiveness of Medical Waste Training Programs | All Points (https://allpointsmedicalwaste.com/assessing-the-effectiveness-of-medical-waste-training-programs)
- How Often Should Employees Refresh Their Knowledge of the Biomedical Waste Operating Plan? | Daniels Health (https://danielshealth.com/knowledge-center/biomedical-waste-operating-plan-updates)
- Impact of training on waste management practices among healthcare workers – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12859272)
